Reconstructing Peri-implant and Papillary Soft Tissue in the Esthetic Area Using Interdental Tissue, a Tuberosity Connective Tissue Graft, and a Tunneling Approach: A Case Report
Ye Shi, DDS, MS; Inés Fernández Guallart, DDS; Mashal Alrajhi, BDS, MPH; Sang-Choon Cho, DDS; and Stuart J. Froum, DDS
Abstract: Long-term survival of dental implants in both fully and partially edentulous patients has been proven successful, as reported in the literature. However, maintenance of soft-tissue quality and volume is often difficult due to the multiple surgeries involved in implant placement and the physiological resorption of bone after tooth extraction. Soft-tissue augmentation is frequently necessary to improve soft-tissue contour and can be done simultaneously with implant or abutment placement or following the final insertion of the implant-supported prostheses. The purpose of this case report is to demonstrate a surgical procedure used to augment a peri-implant buccal soft-tissue defect using interdental palatal tissue from a pocket reduction procedure in combination with a distal wedge graft from the tuberosity as connective tissue utilizing a tunneling approach in the esthetic area. The implant restorations in the reported case were delivered 1 year prior to the soft-tissue reconstruction.
Long-term survival of dental implants in both fully and partially edentulous patients has been extensively demonstrated in the literature. 1-3 Nevertheless, as the use of implant-supported restorations has increased there has been a concomitant rise in esthetic and functional demands. To measure esthetic outcomes, the pink esthetic score proposed by Fürhauser in 2005 used seven parameters to evaluate soft-tissue esthetics. Among these were the papilla, soft-tissue margin level, and buccal contour, as well as the soft-tissue morphology around the implant.4 Maintaining soft-tissue quality and volume, however, is often difficult due to the multiple surgeries involved in implant placement and the physiological resorption of bone after tooth extraction.5 Tissue augmentation is often necessary to improve soft-tissue contour. Such procedures can be performed either prior to or in conjunction with any necessary hard-tissue augmentation, during the time of implant placement, at the time of abutment insertion, or following placement of the final implant-supported restoration. The latter can be the most challenging scenario because it requires additional surgery to augment tissues that have already undergone healing.
Various surgical techniques and materials have been described to augment peri-implant soft tissues.6 These include autografts (ie, subepithelial connective tissue grafts [SECTGs]), allogenic grafts, xenografts, and guided bone regeneration procedures. Many clinicians consider autogenous grafts to be the gold standard for soft-tissue augmentation.7 The SECTG harvested from the palate is a well-documented procedure.8 Although this type of graft reportedly undergoes significant initial shrinkage or contraction, it ultimately remains stable over time with good esthetic results.9 The harvesting procedure of a SECTG from the palatal area, however, is technique sensitive and can be unpleasant for patients during healing, and oftentimes the graft is limited in size due to the palatal morphology.10 In contrast, soft-tissue grafts from the tuberosity have been shown to be dimensionally stable for the first few months, then progressively tend to become hyperplastic and can result in an unesthetic white tissue patch appearance.9
Despite the aforementioned drawbacks, the maxillary tuberosity can be used as an alternative graft donor site, allowing surgeons to collect thicker grafts, and when used in combination with other oral care interventions (such as pocket reduction) this type of graft can provide a unique shape (recreating a papillary triangular shape) while reducing patient postoperative discomfort compared to using a palatal donor site. In previous reports, maxillary tuberosity grafts were used to treat teeth recession in root coverage procedures, but to date no articles have been published on the use of this unique donor site to treat an inter-implant soft-tissue deficiency.11-13
The purpose of this case report is to demonstrate the step-by-step surgical procedures used to augment a peri-implant soft-tissue defect using interdental soft tissue from a pocket reduction procedure in conjunction with the tuberosity as connective tissue donor sites utilizing a tunneling approach in an esthetic area.
Case Report
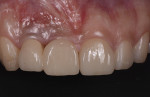
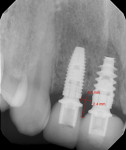
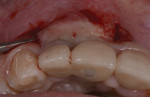
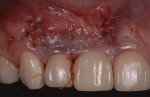
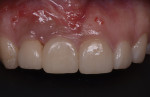
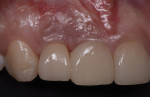
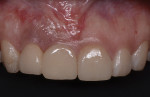
In 2016, a 28-year-old female patient presented to the Ashman Department of Periodontology and Implant Dentistry at New York University College of Dentistry with the chief complaint of grayish color of the gingiva around implant crowns Nos. 7 and 8 and a shadow between the two implant crowns (Figure 1). One year prior to this visit, the patient had the two implants placed and restored with splinted screw-retained zirconia crowns in a private dental office. A radiograph was taken showing 2.4 mm distance between the two implants and 4.5 mm distance between the inter-implant crestal bone to the contact point of the restorations (Figure 2).The patient was healthy, a nonsmoker, and had an unremarkable medical history. A soft-tissue graft thus was planned to augment the buccal contour and papilla around the implants.
Soft-Tissue Grafting Procedure
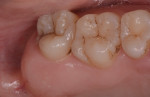
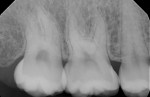
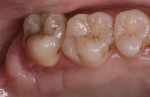
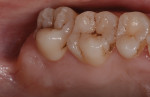
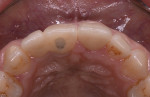
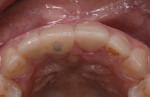
The tuberosity area, including the right first and second molars in the maxillary arch (teeth Nos. 3 and 2, respectively), was evaluated as a potential donor site for a connective tissue graft. The third molar (tooth No. 1) was absent, thereby presenting a large area for tissue harvesting (Figure 3). Probing depths of 5 mm and 6 mm were measured on the distal aspect of tooth No. 2 and the palatal aspects of teeth Nos. 2 and 3. Periapical radiographs revealed no periodontal bone loss, periapical lesions, or subgingival calculus, which confirmed the deep pockets were pseudo pockets (Figure 4). The goal of the surgical procedure was to reduce the periodontal pockets in teeth Nos. 2 and 3 while harvesting interdental and tuberosity tissue and use the connective tissue as a soft-tissue graft around implants Nos. 7 and 8. All surgical procedures were performed at the same visit.
Pocket Reduction and Connective Tissue Graft Harvesting
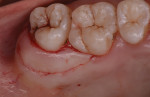
Pocket reduction at distal and palatal sites of teeth Nos. 2 and 3 was achieved using a distal wedge incision followed by a modified apically positioned Widman flap. The surgical procedure was performed as follows: A wedge incision was performed starting at the distal of tooth No. 2 and continued as an internal bevel incision on the palatal of teeth Nos. 2 and 3 (Figure 5). A mucoperiosteal flap was then elevated to the level of the alveolar crest. Crevicular incisions were made around the cervical areas of the involved teeth. After the flap was reflected, a third interdental incision was made.
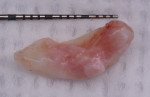
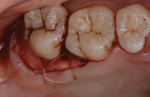
The tuberosity tissue and palatal tissue around teeth Nos. 2 and 3 were excised in one piece (5 mm x 15 mm). No infrabony defect or negative architecture was present at the No. 2 distal and Nos. 2 and 3 palatal sites; therefore, osseous reduction was not performed in this case. The root surfaces were examined and debrided. The palatal flap was repositioned, and the area was sutured with resorbable chromic gut 5-0 suture (Henry Schein Dental, henryschein.com). The harvested tissue was removed, and the epithelium was separated with a #15C blade and removed, leaving the connective tissue for grafting (Figure 6 and Figure 7). Resorbable collagen tape was inserted at the donor site and sutured with resorbable chromic gut 5-0 suture to achieve hemostasis (Figure 8).
Recipient Site Preparation
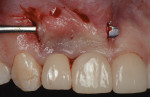
Two vertical incisions were made at the distal of implant No. 7 and mesial of implant No. 8. The vertical incisions were extended apically to the vestibule and coronally beyond the mucogingival junction. Subsequently, the two incisions were connected by elevating a full-thickness mucoperiosteal flap using a vertical incision subperiosteal tunnel approach (VISTA) periosteal elevator (Hu-Friedy, hufriedygroup.com). Remaining collagen bundles on the inner surface of the flap were carefully excised using curettes until passive, tension-free mobilization of the flap was achieved (Figure 9 and Figure 10).
Graft Insertion
The SECTG harvested from the tuberosity area was contoured to the measured length and width of the recipient site. Resorbable vicryl 4-0 sutures (Henry Schein Dental) were used to engage the two edges of the graft, and the graft was pulled laterally by the two sutures toward each of the vertical incisions and stabilized at the distal and mesial ends of the tunnel (Figure 11). Another suture was inserted at the center of the graft and, with the splinted crown No. 7 and No. 8 being used as an anchor, served to coronally position and stabilize the graft (Figure 12). The vertical incisions were sutured with resorbable chromic gut 5-0 sutures.
Postsurgical Protocol
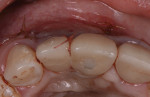
The patient was prescribed antibiotics (500 mg amoxicillin, three times a day) for 7 days and was instructed to rinse with a 0.2% chlorhexidine solution, two times a day for 1 minute for 2 weeks. The patient was instructed to avoid brushing in the operated area until suture removal at 2 weeks. All sutures that were not resorbed were removed at the 2-week postoperative visit. The patient was recalled for follow-up at 1 week, 2 weeks, 1 month, 3 months, and 1 year; at each visit the teeth were scaled and root planed and polished, and her oral hygiene was reviewed (Figure 13 through Figure 19). (To compare pretreatment vs 1-year post-treatment photographs, see Figure 1 vs Figure 17 [frontal views] and Figure 18 vs Figure 19 [occlusal views].)
Discussion
The patient's chief complaint was the soft-tissue appearance around implant restorations, particularly the mucosal discoloration and flattened papilla between two implant crowns in the esthetic zone. With implant survival and success rates being relatively high, the esthetic outcome has become a main focus of interest for both patients and clinicians, especially in anterior areas. An optimal esthetic outcome of an implant restoration should be in harmony with the adjacent dentition. For decades, Albrektsson's criteria of success was widely used for evaluating implant outcome; it considered only the survival of the implant with absence of mechanical and biological complications.14 However, current advances in contemporary oral implantology, coupled with patients' high treatment expectations, underscore the need for a more comprehensive definition of success than just implant and bone stability. A systematic review by Papaspyridakos et al listed the most frequently used parameters for assessing implant success in the literature and separated them into four groups: implant level, peri-implant soft tissue, prosthesis, and patient's subjective evaluation.15 It added to the classic definition of implant success by Albrektsson.14 In a clinical situation like the one described in this case report, it is evident that implant survival without considering other parameters is not sufficient to satisfy the current criteria for a successful outcome of a case and that the patient's satisfaction and the esthetics of the final results are extremely important. These factors are often related to the appearance of the peri-implant soft tissue.
The deficient papilla between implant restorations leading to a compromised esthetic outcome has been a common dilemma. In the anterior region, where the creation of papillae requires that a vertical component be added to any soft-tissue enhancement of a flat profile, a modified surgical protocol becomes necessary. Over the years, various techniques have been proposed to address this issue, such as injecting a hyaluronic gel, sculpting soft tissue with provisional crowns, using guided tissue regeneration, and soft-tissue grafting.16-18
Soft-tissue grafts differ in their characteristics depending on the donor site. When harvested from the tuberosity, significantly thicker graft may be obtained compared to one taken from the hard palate.9 The literature suggests that an SECTG harvested from the palate undergoes significant initial shrinkage but remains stable after the initial changes. In marked contrast, a soft-tissue graft from the tuberosity area remains stable for the first few months and tends to progressively increase in size with time. The reason for these differences is that tissue from the tuberosity area is denser and thicker, having more collagen fibers and less fat and glandular tissue compared to palatal tissue.19,20 Another benefit of a tuberosity graft is that it allows for pocket reduction to be achieved. In the present case, the initial pseudo pockets of 5 mm to 6 mm at distal No. 2 and palatal Nos. 2 and 3 sites were successfully reduced after harvesting a palatal graft from the tuberosity. Access to the tuberosity donor site, however, can be difficult in patients with limited mouth opening. Moreover, the presence of a third molar reduces the volume and thickness of available tissue. These factors must be considered when contemplating harvesting a soft-tissue graft from the tuberosity.
In the reported case, the tuberosity graft harvesting was extended to the interdental palatal papillary area between the two distal teeth in the maxillary arch, thus creating a graft with a "V" shape that could readily fit and correct the inter-implant papillary soft tissue in the esthetic area (Figure 6 and Figure 7). This approach was previously reported on by Hirsch et al in cases in which they removed excessive tissue in a pocket reduction procedure and used it to cover root recessions in esthetic areas.13 The use of this less commonly utilized donor site to correct inter-implant defects, however, was never previously reported on in the literature. The rationale for using it is the combination of the highly fibrotic nature of tissue from the tuberosity along with the accessibility and advantageous shape of the interdental coronal palatal tissue.
The graft placement and stabilization by using a tunnel approach provides sufficient access to the defect area with the advantages of preservation of the cervical soft-tissue integrity and blood supply. Because the crestal area is not accessed, there is less chance of wound dehiscence, graft necrosis, or postsurgical recession. In fact, when compared to a conventional approach of reflecting a full-thickness mucoperiosteal flap, this less invasive procedure has been reported to be a more cost-effective and time-efficient option with similar success and fewer complications.21 It is also advantageous compared to a full-thickness mucoperiosteal flap in preserving the blood supply to the grafted area.
The final outcome of the papilla between the two implant restorations in this case was still slightly deficient compared to the contralateral side with natural teeth. Another critical determinate factor is the distance between the crestal bone to the contact point. According to Tarnow et al's clinical study, when this distance was 5 mm or less, the papilla completely filled this space almost 100% of the time. When the distance was 6 mm, the interdental space filled about 55% of the time. The percentage of complete papilla fill decreased as distance increased.22 In addition, an average of 5 mm papilla height can be expected between two natural teeth. However, in the case of two adjacent implants, only 2 mm, 3 mm, or 4 mm of soft-tissue height (average 3.4 mm) can be expected from the inter-implant crest of bone to the contact point.23 In the present case, there was minor bone loss of the inter-implant crestal bone as shown in the radiograph, resulting in the distance of 4.5 mm between crestal bone and contact point (Figure 2). If the contact point was made more coronal, complete papilla fill might not have been achieved.
In addition, the absence of marginal and crestal bone loss around the implant platform is a critical factor in stabilizing the papilla. The 1.2 mm to 1.5 mm horizontal bone loss of non-platform-switching implants has been reported.24 If these implants are placed less than 3 mm apart, there is an increased risk of loss of inter-implant bone peak due to the circumferential crestal bone loss for both implants. Although another clinical study demonstrated reduced marginal bone loss with platform-switching implants, it still reported that only 64% of interdental bone peak can be preserved if the distance between two implants is less than 3 mm.25 Therefore, it is still recommended to maintain a minimum of 3 mm inter-implant distance, especially in the anterior esthetic zone, to prevent inter-implant crestal bone loss. In the present case, the distance between the two implants was 2.4 mm, which might be the etiologic factor for the inter-implant crestal bone loss, resulting in deficient inter-implant papilla.
Conclusion
The subepithelial connective tissue graft obtained from the combination of interdental palatal tissue from a pocket reduction surgery and distal wedge-shaped tissue from the tuberosity area was shown in this case to provide a predictable and esthetic outcome when augmenting an inter-implant site in terms of buccal contour gain and papilla, after being recontoured and repositioned in the previously described fashion. The hyperplastic nature of the tuberosity graft allows it to become thicker and denser over time, maintaining and improving its esthetic outcome even years after the surgery. More research and comparative studies are necessary to verify the technique and results of the present case report. Prospective clinical studies and additional case reports with objective esthetic evaluation scores should be considered for the future studies.
About the Authors
Ye Shi, DDS, MS
Clinical Assistant Professor, New York University International Implant Program, Ashman Department of Periodontology and Implant Dentistry, NYU College of Dentistry, New York, New York
Inés Fernández Guallart, DDS
Former Resident, New York University International Implant Program, Ashman Department of Periodontology and Implant Dentistry, NYU College of Dentistry,
New York, New York
Mashal Alrajhi, BDS, MPH
Former Resident, New York University International Implant Program, Resident, NYU Master of Public Health, Ashman Department of Periodontology and Implant Dentistry, NYU College of Dentistry, New York, New York
Sang-Choon Cho, DDS
Director, New York University International Implant Program, Ashman Department of Periodontology and Implant Dentistry, NYU College of Dentistry, New York,
New York
Stuart J. Froum, DDS
Adjunct Clinical Professor and Director of Clinical Research, Ashman Department
of Periodontology and Implant Dentistry, NYU College of Dentistry, New York,
New York
References
1. Creugers NH, Kreulen CM, Snoek PA, de Kanter RJ. A systematic review of single-tooth restorations supported by implants. J Dent. 2000;28(4):209-217.
2. Buser D, Sennerby L, De Bruyn H. Modern implant dentistry based on osseointegration: 50 years of progress, current trends and open questions. Periodontol 2000. 2017;73(1):7-21.
3. Brånemark PI, Svensson B, van Steenberghe D. Ten-year survival rates of fixed prostheses on four or six implants ad modum Brånemark in full edentulism. Clin Oral Implants Res. 1995;6(4):227-231.
4. Fürhauser R, Florescu D, Benesch T, et al. Evaluation of soft tissue around single-tooth implant crowns: the pink esthetic score. Clin Oral Implants Res. 2005;16(6):639-644.
5. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent. 2003;23(4):313-323.
6. Thoma DS, Buranawat B, Hämmerle CH, et al. Efficacy of soft tissue augmentation around dental implants and in partially edentulous areas: a systematic review. J Clin Periodontol. 2014;41 suppl 15:S77-S91.
7. Thoma DS, Benić GI, Zwahlen M, et al. A systematic review assessing soft tissue augmentation techniques. Clin Oral Implants Res. 2009;20 suppl 4:146-165.
8. Langer B, Calagna L. The subepithelial connective tissue graft. J Prosthet Dent. 1980;44(4):363-367.
9. Studer SP, Allen EP, Rees TC, Kouba A. The thickness of masticatory mucosa in the human hard palate and tuberosity as potential donor sites for ridge augmentation procedures. J Periodontol. 1997;68(2):145-151.
10. Song JE, Um YJ, Kim CS, et al. Thickness of posterior palatal masticatory mucosa: the use of computerized tomography. J Periodontol. 2008;79(3):406-412.
11. Jung UW, Um YJ, Choi SH. Histologic observation of soft tissue acquired from maxillary tuberosity area for root coverage. J Periodontol. 2008;79(5):934-940.
12. Dellavia C, Ricci G, Pettinari L, et al. Human palatal and tuberosity mucosa as donor sites for ridge augmentation. Int J Periodontics Restorative Dent. 2014;34(2):179-186.
13. Hirsch A, Attal U, Chai E, et al. Root coverage and pocket reduction as combined surgical procedures. J Periodontol. 2001;72(11):1572-1579.
14. Albrektsson T, Zarb G, Worthington P, Eriksson AR. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986;1(1):11-25.
15. Papaspyridakos P, Chen CJ, Singh M, et al. Success criteria in implant dentistry: a systematic review. J Dent Res. 2012;91(3):242-248.
16. Salama H, Salama M, Garber D, Adar P. Developing optimal peri-implant papillae within the esthetic zone: guided soft tissue augmentation. J Esthet Dent. 1995;7(3):125-129.
17. Becker W, Gabitov I, Stepanov M, et al. Minimally invasive treatment for papillae deficiencies in the esthetic zone: a pilot study. Clin Implant Dent Relat Res. 2010;12(1):1-8.
18. Wittneben JG, Buser D, Belser UC, Brägger U. Peri-implant soft tissue conditioning with provisional restorations in the esthetic zone: the dynamic compression technique. Int J Periodontics Restorative Dent. 2013;33(4):447-455.
19. Roccuzzo M,Gaudioso L,Bunino M,Dalmasso P.Surgical treatment of buccal soft tissue recessions around single implants: 1-year results from a prospective pilot study. Clin Oral Implants Res. 2014;25(6):641-646.
20. Zuhr O, Bäumer D, Hürzeler M. The addition of soft tissue replacement grafts in plastic periodontal and implant surgery: critical elements in design and execution. J Clin Periodontol. 2014;41 suppl 15:S123-S142.
21. Zadeh HH. Minimally invasive treatment of maxillary anterior gingival recession defects by vestibular incision subperiosteal tunnel access and platelet-derived growth factor BB. Int J Periodontics Restorative Dent. 2011;31(6):653-660.
22. Tarnow DP, Magner AW, Fletcher P. The effect of the distance from the contact point to the crest of bone on the presence or absence of the interproximal dental papilla. J Periodontol. 1992;63(12):995-996.
23. Tarnow D, Elian N, Fletcher P, et al. Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. J Periodontol. 2003;74(12):1785-1788.
24. Hermann JS, Cochran DL, Nummikoski PV, Buser D. Crestal bone changes around titanium implants. A radiographic evaluation of unloaded nonsubmerged and submerged implants in the canine mandible. J Periodontol. 1997;68(11):1117-1130.
25. Rodríguez-Ciurana X, Vela-Nebot X, Segalà-Torres M, et al. The effect of interimplant distance on the height of the interimplant bone crest when using platform-switched implants. Int J Periodontics Restorative Dent. 2009;29(2):141-151.