Correcting Occlusal Dysfunction While Addressing Patient’s Esthetic Concerns
Jennifer Graas, BMSc, DDS
Abstract: This case illustrates a method of addressing a patient's esthetic and functional concerns using additive restorative dentistry to avoid increasing biomechanical risk. Use of a Kois deprogrammer aided in the functional diagnosis and treatment to equilibrate the new additive restorations. At presentation, the patient was unhappy with the appearance of her smile, as she had bulbous, triangular-shaped crowns, a midline discrepancy due to a missing lateral incisor, and mismatched shades of porcelain-fused-to-metal crowns. Also, her bite was uncomfortable, as she found it difficult to find a repeatable bite position. Before addressing the patient's esthetic concerns, it was necessary to first evaluate her functional, periodontal, biomechanical, and dentofacial risk factors. After arriving at the functional diagnosis, and prior to preparing the patient's teeth, the clinician was able to allow the patient to preview her new smile with an intraoral mock-up. The treatment both satisfied the patient's esthetic expectations and addressed her functional concerns.
A middle-aged female patient presented with concerns about the esthetics of her smile and the feel of her bite. Due to her high periodontal risk, the patient was not a candidate for orthodontic treatment. To avoid increasing biomechanical risk to the teeth with removal of significant tooth structure, the patient's vertical dimension of occlusion (VDO) would be increased to address the esthetic and functional concerns.
This case also demonstrates how clinicians can camouflage a missing lateral incisor and midline discrepancy without orthodontic treatment. By increasing the patient's anterior tooth length, moving line angles inward, and closing the incisal embrasures, a more balanced and harmonious smile was able to be achieved.
Clinical Case Overview
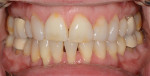
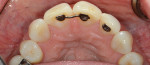
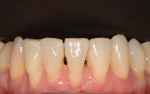
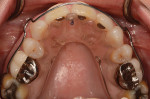
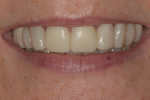
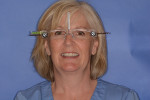
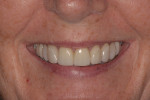
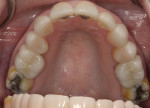
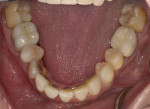
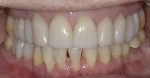
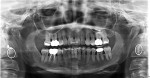
The 50-year-old woman presented with a chief concern of the appearance of her smile. She was unhappy with the size, shape, and shade of many teeth (Figure 1 and Figure 2), and she needed to shift her jaw and squeeze to make her posterior teeth contact. The patient had received orthodontic treatment in her late teens when teeth Nos. 5, 7, 12, and 28 had been extracted for lack of space, resulting in a significant midline shift to the right (Figure 3). The treatment goal was to provide the patient with a balanced occlusion while improving the esthetics of her smile. Due to her high periodontal risk, further orthodontic treatment was not an option. The patient's functional and esthetic concerns would have to be managed with restorative treatment, with care taken to avoid increasing her biomechanical risk.
Medical and Dental History
The medical history was unremarkable and revealed no significant concerns that would affect her dental treatment. The patient had seasonal allergies and took vitamins B6, B12, B complex, and D, and magnesium supplements. She was determined to be American Society of Anesthesiologists (ASA) I classification.
As for her dental history, the patient reported cold sensitivity during hygiene appointments, especially around her mandibular anterior teeth. Teeth Nos. 5, 7, 12, and 28 had been extracted during orthodontic treatment more than 30 years prior. She was aware of increased periodontal risk, noting that her older sister and parents all had dentures. She had previously seen a periodontist and was told her mandibular anterior teeth were a concern with significant recession. She also reported that when biting her teeth together, she primarily contacted her anterior and premolar teeth, and had to shift and squeeze her jaw to enable her molars to contact fully. She wore an occlusal guard every night, which helped her jaw feel more relaxed.
Diagnosis, Risk Assessment, and Prognosis
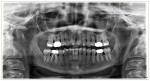
Periodontal: All maxillary anterior teeth, premolars, and second molars and mandibular second molars (teeth Nos. 2, 4, 6, 8 through 11, 13, 15, 18, and 31) had 2 mm to 3 mm generalized horizontal bone loss and 3 mm to 4 mm of clinical attachment loss (Figure 4). No bleeding on probing or mobility was noted, which had not changed in 5 years. The aforementioned teeth were classified as stage II, grade B.1
The maxillary first molars and all other mandibular teeth (teeth Nos. 3, 14, and 19 through 30) had 4 mm generalized horizontal bone loss that had progressed in the past 5 years and 5 mm clinical attachment loss. All first molars had class II furcation involvement. Tooth No. 29 had apical root resorption and a 1:1 crown-to-root ratio. These teeth were classified as stage III, grade B. The periodontal risk was determined to be high based on the most severe areas of disease. Without treatment, the patient's periodontal prognosis was poor.
Risk: High
Prognosis: Poor
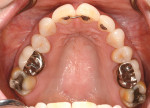
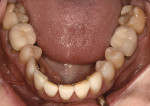
Biomechanical:While all of the patient's first and second molars had been previously restored, all other teeth were intact and unrestored with a good prognosis. She had low caries risk. Teeth Nos. 6, 8, 9, 11, 14, 19 through 21, 23 through 26, and 30 all had less than 1 mm of abrasion. All first molars (teeth Nos. 3, 14, 19, and 30) had porcelain-fused-to-metal (PFM) crowns that were more than 20 years old. Tooth No. 30 had acceptable endodontic treatment. Occlusal composites with marginal staining were present on the mandibular second molars (teeth Nos. 18 and 31), and both of these teeth had isthmus widths of less than one-third the intercuspal width. Her maxillary second molars (teeth Nos. 2 and 15) had occlusal amalgam restorations with craze lines on both mesial marginal ridges and isthmus widths of one-half the intercuspal width. These two teeth had fair prognoses without treatment (Figure 5 and Figure 6).
Risk: Moderate
Prognosis: Fair
Functional: The examination revealed a normal range of motion, no joint sounds, no head and neck discomfort, and no tenderness to muscle palpation. Load and immobilization tests were negative. The patient's cephalometric tracing was also unremarkable, as all values were within the normal range. Minimal (<1 mm) attrition was noted on teeth Nos. 6, 10, 23 through 25, and 27). Moderate (1 mm to 2 mm) attrition was noted on teeth Nos. 9 and 26 (Figure 7 and Figure 8), and tooth No. 8 displayed fremitus. The patient's dental history pointed toward a diagnosis of constricted chewing pattern and dysfunction, as she had described feeling like she primarily contacted her anterior and premolar teeth and had to shift and squeeze her jaw to enable her molars to contact fully. However, upon deprogramming and mounting the models, the point of initial contact was found to be at teeth Nos. 2 and 31. The patient also confirmed that these were the only teeth that contacted when she removed the deprogrammer in the morning. In addition, her mandible did not move forward with deprogramming, as the initial contact was not on an anterior tooth. Therefore, the diagnosis was confirmed to be occlusal dysfunction.2
Risk: Moderate
Prognosis: Fair
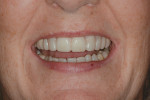
Dentofacial:The patient was mainly concerned about the esthetics of all visible maxillary teeth (teeth Nos. 3 through 14). She felt self-conscious about the appearance of her dentition and desired a more feminine and age-appropriate smile. She wanted to address the color of her teeth and the triangular shape of her central incisors and make her teeth appear narrower and less "bulbous." As a result of the missing/extracted tooth No. 7, her midline was positioned to the right and axially inclined. She had a diastema between teeth Nos. 9 and 10, which had been previously closed with composite. She had normal lip dynamics (4.5 mm to 6 mm) and displayed the full length of her anterior teeth to the free gingival margins in the Duchenne smile. Her prognosis was determined to be poor due to the amount of gingival display (Figure 1 and Figure 2). Teeth Nos. 20 through 29 had a fair prognosis, as they had minimal display when the patient smiled; however, these teeth were visible in the Duchenne smile.
Risk: Moderate
Prognosis: Poor
Treatment Goals
Three treatment goals were identified. The first was to treat the dysfunction by creating a precise posterior occlusion with bilateral equal simultaneous contacts; this would also minimize the friction on her anterior teeth. The second goal was to improve the esthetics of the patient's smile and camouflage the missing lateral incisor. All restorative treatment would be performed additively to minimize the patient's biomechanical risk. Finally, to avoid further periodontal disease progression, the patient would need more frequent periodontal maintenance care.
Treatment Plan
A trial equilibration was performed on the deprogrammed mounted models. Significant reduction of posterior teeth would have been required to achieve bilateral equal simultaneous contact. Therefore, to treat the occlusal dysfunction, the VDO needed to be increased. Furthermore, lengthening the patient's anterior teeth (Nos. 6, 8 through 10, 25, and 26) was desired, which would not have been possible without opening the VDO. Because of the patient's high periodontal risk, orthodontics was ruled out, and therefore her VDO would need to be raised restoratively.
A Kois deprogrammer (Kois Center, koiscenter.com) was used to find a repeatable reference position3 to perform an additive occlusal equilibration4 and to later equilibrate the new additive posterior restorations (Figure 9). Anterior teeth adhesive restorations were also planned additively wherever possible. The patient was given a "preview" of her new smile with a preoperative intraoral mock-up (Figure 10) and in the temporary phase (Figure 11) to ensure she was satisfied prior to fabrication of the final restorations. A periodontal maintenance interval of 3 months was recommended to control further loss of attachment. Periodontal treatment consisting of scaling and root planing, chemotherapeutics, and connective tissue grafting were planned to reduce the risk of disease progression.
Treatment Phases
Phase 1: Deprogram, Wax-up, Mock-up, and Try-in
The patient wore the Kois deprogrammer for 4 weeks, and three separate bite records were taken to confirm that the mandible did not move forward and that muscle engrams were disrupted. The diagnosis of occlusal dysfunction was confirmed.2 This also determined the reference condylar position. A Kois dentofacial analyzer (Panadent, panadent.com) was used to determine natural head posture and ensure the maxillary model was mounted level with the horizon on the Panadent articulator (Figure 12).5,6 A diagnostic wax-up was then performed after visually determining that the maxillary and mandibular incisal edges (Nos. 6, 8 through 10, 25, and 26) should be lengthened by 1 mm and the canines coupled. Equal bilateral simultaneous centric contacts were established for the posterior teeth, improving the patient's ability to find a repeatable, maximum intercuspation (MIP) position.
During production of the wax-up, care was taken to add as much contour as possible to the buccal surfaces of the anterior teeth and premolars to minimize the reduction required for the veneer preparations and keep the preparations 100% within enamel.4 The fuller buccal corridors also provided a more balanced smile. A polyvinyl siloxane (PVS) matrix of the maxillary wax-up was made and placed over the patient's teeth. This was done to allow the patient to see the proposed esthetic changes in her mouth as well as to confirm that the facebow record was accurate and level with the horizon.
Phase 2: Increase Vertical Dimension of Occlusion
Based on the wax-up, an injection mold technique was used to add composite to the premolars and lower anterior teeth (Nos. 4, 13, 24 through 26, and 29). The PFM crowns on teeth Nos. 3, 14, and 30 were removed, the margins were refined, the final PVS impressions were taken, and bis-acryl provisionals were made using a PVS matrix of the wax-up at the new VDO.
The new restorations and temporary crowns were then equilibrated for equal bilateral simultaneous contact at the new VDO using the Kois deprogrammer. A small amount of composite was bonded to the platform, ensuring a single flat point of contact with the opposing lower anterior tooth, then gradually reducing the platform and adjusting the new restorations to achieve equal bilateral simultaneous contact. The maxillary anterior teeth were then prepared, impressed, and temporized for porcelain veneers (Figure 13). The patient was extremely pleased with her smile after this visit. Zirconia was selected for the posterior crowns (teeth Nos. 3, 14, and 30), and lithium-disilicate (e.max®, Ivoclar Vivadent, ivoclarvivadent.com) for the anterior porcelain veneers. The final restorations were delivered, and the patient's occlusion was refined using the Kois deprogrammer (Figure 14 through Figure 18). The patient was completely satisfied with her occlusion, and her bite was very comfortable. A new occlusal guard was provided.
Phase 3: Periodontal Treatment and Maintenance
The patient committed to a 3-month periodontal maintenance interval. She also began to use a treatment rinse (CariFree® CTx4 Treatment Rinse, CariFree, carifree.com) and a water flosser at home to reduce inflammation as much as possible. She was referred to a periodontist for connective tissue grafting of teeth Nos. 23 through 26.
Discussion
In this case both the patient and practitioner were very satisfied with the functional and esthetic results. All treatment was done additively and within enamel in order to maintain the patient's biomechanical risk. All indirect and direct restorations were made to cover exposed dentin at the cervical margins, thereby reducing environmental risk. Several remaining existing restorations were left for future treatment, as needed. The patient's functional risk was decreased and her occlusion was comfortable. The fremitus on tooth No. 8 resolved, and the risk of future attrition was minimal. The patient's periodontal risk remains unchanged due to inherent/host factors.
The treatment successfully camouflaged the patient's missing lateral incisor and midline discrepancy, giving her a pleasing appearance by altering the line angles and closing the incisal embrasures. Her dentofacial risk remains unchanged due to her moderate lip dynamics; however, her prognosis has improved to good because her esthetic concerns were addressed.
Conclusion
With the aid of the Kois deprogrammer, additive restorative dentistry was achieved to provide the patient proper occlusal function to support excellent esthetics and biomechanical results. Utilizing a systematic diagnosis, detailed treatment plan, and carefully designed wax-up, the clinician was able to allow the patient to realize her esthetic goals without increasing biomechanical risk. Additionally, the patient's periodontal, dentofacial, and functional prognoses were improved and she attained a smile with which she was highly pleased without unnecessary tooth reduction.
Acknowledgment
The author thanks Star Dental Technologies, Inc., Calgary, Alberta, Canada, for laboratory support; Bonnie Ferrell, DDS, and Jack Courtney, DDS, for their guidance and mentorship; Betsy Bakeman, DDS, for her incredible diagnostic wax-up course; and John Kois, DMD, MSD, for all of his support.
About the Author
Jennifer Graas, BMSc, DDS
Mentor, Kois Center, Seattle, Washington; Private Practice, Calgary, Alberta, Canada
References
1. Tonetti MS, Greenwell H, Kornman KS. Staging and grading of periodontitis: framework and proposal of a new classification and case definition. J Periodontol. 2018;89 suppl 1:S159-S172.
2. Kois JC. Functional Occlusion: Science Driven Management Manual. Seattle, WA: Kois Center; January 2011:79.
3. Beshar MJ. Systematic treatment using a direct deprogrammer to resolve long-standing problems in a phobic patient. Compend Contin Educ Dent. 2015;36(6):418-425.
4. Swanson K, Hermanides L. Biomechanics and function: altering paradigms to treat a patient's esthetic disability conservatively. Compend Contin Educ Dent. 2020;41(5):284-289.
5. Misch CE. Guidelines for maxillary incisal edge position - a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.
6. Arnett GW, Gunson MJ. Facial analysis: the key to successful dental treatment planning. J Cosmetic Dentistry. 2005;21(3):20-33.