Lasso Guided Bone Regeneration Technique for the Management of Implant Fenestration Defects
Bruna T. Neiva, DDS, MS; Gisele F. Neiva, DDS, MS; and Rodrigo Neiva, DDS, MS
Abstract: Implant placement in the anterior maxilla provides many unique challenges to the clinician, including esthetics and potential alveolar bone anatomic variations. The depth of the implant osteotomy is a key consideration to avoid a fenestration defect, which could necessitate subsequent treatment. Treatment options for such defects include bone augmentation with or without implantoplasty. Bone augmentation for the correction of dehiscence or fenestration defects on restored dental implants can be difficult due to the grafted site being close to the margin of the flap, thereby favoring premature bone graft and/or barrier membrane exposure. This article describes the management of an implant fenestration defect using lasso guided bone regeneration, a contemporary technique for bone augmentation and alveolar reconstruction designed to maximize predictability and tissue quality by combining fast-absorbing bone replacement materials with long-lasting barrier membranes and stabilization with internal periosteal sutures.
Compared with other areas of the dentition, implant-supported rehabilitation in the anterior maxilla typically presents significant and additional challenges due to greater esthetic demand to recreate a natural replacement for missing anterior teeth.1,2 Esthetic implant-supported replacement of teeth in the maxillary anterior region is dependent on multiple factors, such as ideal hard- and soft-tissue contours and adequate mesiodistal, buccolingual, and crestal positions of the dental implant for natural contours and emergence profile of the final restorative treatment.3-6 Surgical guides can be used to facilitate precise placement of the dental implant. However, surgical guides can mask alveolar bone anatomic variations that may be more easily detected when surgical guides are not used.7-12 Hence, the surgeon may not be able to detect when an implant osteotomy comes into proximity with or perforates a bony plate, thus creating or contributing to the development of a fenestration defect that may be become symptomatic or require implant removal.
The aim of this article is to illustrate the management of an implant fenestration defect with a contemporary guided bone regeneration (GBR) technique used for alveolar ridge augmentation.
Case Presentation
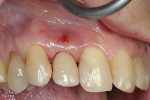
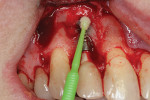
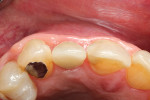
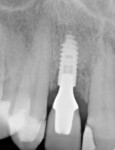
A 45-year-old female patient presented with a sinus tract on the buccal aspect of the No. 7 implant (Figure 1). The patient reported significant discomfort upon palpation and occasional drainage in this area. No mobility was detected. Probing examinations revealed probing depths within normal limits and no bleeding on probing. A periapical radiograph confirmed adequate bone levels and no signs of pathology. Palpation on the buccal aspect of the implant stimulated drainage through the sinus tract, and the threads of the dental implant could be felt, suggesting existence of a buccal fenestration or dehiscence defect.
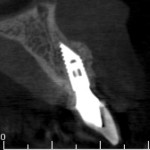
CBCT images confirmed that the apical aspect of the dental implant was completely exposed, protruding from the osseous envelope. A review of the patient's chart showed that the implant had been in function for 31 months and that it was placed using a computer-generated guide. Treatment options were discussed with the patient, including implant removal and/or bone augmentation. The patient was fully satisfied with the existing restoration and strongly desired to save the implant. As a result, the patient was scheduled for bone augmentation and possible reshaping of the dental implant to maximize regenerative treatment outcomes.
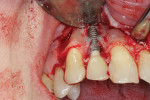
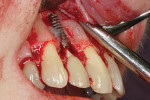
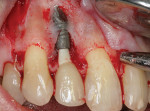
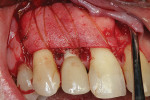
Following local anesthesia via infiltration of 2% xylocaine with 1:100,000 epinephrine, a sulcular incision was made on the buccal aspect only of Nos. 6 through 9, protecting interdental papillae, and a vertical releasing incision was placed on the mesial aspect of tooth No. 5 for adequate surgical access. Full-thickness mucoperiosteal flap elevation exposed the fenestration defect and incipient dehiscence defect (Figure 2). After complete defect degranulation was achieved, implantoplasty was performed to remove the part of the implant that was protruding from the osseous envelope (Figure 3 and Figure 4). Additional implant decontamination was achieved with topical application of citric acid and irrigation with sterile saline (Figure 5).
Bone augmentation was performed following the principles of lasso GBR to maximize wound stability during early healing, thus leading to more predictable volumetric bone gain and tissue quality.13 Lasso GBR utilizes fast-absorbing bone scaffolds in combination with long-lasting barrier membranes for optimal graft material retention and periosteal-stabilizing sutures to secure the bone graft/membrane complex against the defect.13
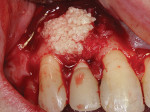
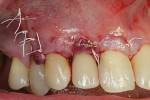
The defect in this case was grafted with a 0.5 cc layer of a cancellous bone allograft (Puros® Cancellous, Zimmer Biomet, zimmerbiomet.com), which was covered with a 0.5 cc layer of a cortical bone allograft (Puros® Cortical, Zimmer Biomet) (Figure 6). An allogenic dermal matrix was used as a long-lasting barrier membrane (Puros® Dermis, Zimmer Biomet) (Figure 7). Stabilizing lasso sutures were completed with absorbable 4-0 chromic-gut suture (Ethicon, ethicon.com). The buccal flap was advanced, repositioned, and stabilized with non-absorbable 4-0 polytetrafluoroethylene (PTFE) sutures (Organogenesis, organogenesis.com) (Figure 8). The patient was prescribed 500 mg amoxicillin every 8 hours for 7 days and a Medrol® dose-pack. The patient was instructed to take 500 mg acetaminophen, as needed, for additional pain control.
At a regular postoperative appointment 2 weeks after bone augmentation, adequate wound healing was evident and the patient reported minimal to no discomfort. The PTFE sutures were removed. The patient returned 3 months later and no evidence of recurring sinus tract was found. Clinical examination showed stable peri-implant soft tissues. The patient continued to be seen for regular maintenance visits every 3 months.
Results of the case at 2 years post-treatment are shown in Figure 9 through Figure 11. A CBCT obtained at that time demonstrated the re-establishment of adequate alveolar bone coverage of the dental implant and stability of the regenerative outcome (Figure 10). At the time of this writing, the implant remains in function for more than 4 years after implantoplasty and bone augmentation.
Lasso GBR Technique
To summarize the technique, it begins with full-thickness mucoperiosteal flap elevation. Flap release is done using a single periosteal incision. A periosteal anchor is created to accommodate stabilizing sutures. A layered approach to bone grafting is utilized, and membrane adaptation and stabilization is done with lasso sutures. Finally, passive wound closure is performed.
Discussion
Implant dentistry started decades ago as a treatment alternative to provide a fixed replacement option or improved retention for lower dentures and rapidly evolved into a preferred method of care for tooth replacement.14 Patient expectations also evolved with the maturation of implant dentistry, as the treatment modality progressed from a fixed solution, to removable prosthetics, to meeting high esthetic demands provided by implant-supported prostheses that imitate natural tooth function and appearance.15-20 A key condition for achieving ideal functional and esthetic outcomes in implant dentistry is optimal implant position. Guided implant surgery associated with 3D planning allows for unmatched accuracy and precision. However, complications of guided implant surgery have been reported,21-23 one of which is the inability to detect anatomic variations that are not always captured during treatment planning, like perforation of buccal or lingual plates.
The anterior maxilla offers significant challenges due to the undercut of the premaxilla. To achieve ideal prosthetic buccolingual implant angulation, anatomic position is often compromised. This is further exacerbated when screw-retained restorations are planned, because in order to provide palatal screw access, implants need to be placed with more palatal angulation, consequently forcing the apical part of the implant in a buccal direction. Hence, clinicians must pay close attention to the depth of the osteotomy and, if necessary, choose shorter implants to avoid these complications. A fenestration defect may not interfere with osseointegration, may go unnoticed and remain asymptomatic for years, and may never cause a problem for some patients.24-28 However, other patients may experience a sore spot where the bone fenestration is located. This soreness is caused by the soft tissues rubbing or being forced against the sharp threads of the implant. This soft-tissue irritation is likely to expose the apex or threads of the implant, creating a sinus tract. Diagnosis can be confirmed with 3D imaging. Ideally, these types of defects should be treated before a sinus tract is established. Treatment options include bone augmentation with or without implantoplasty. The need to alter the shape of the implant is related to the degree of protrusion of the implant in relation to the osseous envelope and adjacent teeth. A significant degree of apical protrusion will interfere with bone formation. More severe cases may require implant removal and retreatment.29-31
Bone augmentation for the correction of dehiscence or fenestration defects on restored dental implants can be difficult since the grafted site is close to the margin of the flap, favoring premature bone graft and barrier membrane exposure, and affecting wound stability. Lasso GBR is a contemporary technique of bone augmentation and alveolar reconstruction that is designed to maximize predictability and tissue quality by combining fast-absorbing bone replacement materials with long-lasting barrier membranes and stabilization with internal periosteal sutures.13 Traditional methods of bone augmentation are based on opposite concepts: long-lasting bovine-derived bone substitutes in combination with fast-absorbing barrier membranes. These traditional approaches and materials for bone augmentation limit overall bone quality because the bone replacement material acts as permanent bone filler, taking up space and limiting bone remodeling and function.32-34 Conversely, human-derived bone substitutes provide mineral content and density similar to native bone, resulting in more rapid turnover and superior tissue quality.35-37
Barrier membrane coverage is critical for the success of fast turnover bone replacement materials. Long-lasting absorbable membranes provide barrier function for at least 4 months, preventing encapsulation of the fast-absorbing bone replacement by the mucoperiosteal flap.38,39 Despite the superior and prolonged barrier function provided by these membranes, they offer less wound stability during the first few weeks of wound healing due to micromotion of the barrier membrane under the mucoperiosteal flap. Hence, membrane stabilization is required for predictable outcomes. Membrane stabilization methods include the use of titanium pins and micro screws, which need to be removed after bone formation.40 Failure to remove these titanium fixating devices may lead to future complications. Lasso GBR, on the other hand, provides ideal membrane stabilization during the first few weeks following bone augmentation, the most critical stage of wound healing, utilizing internal absorbable sutures that do not require a second surgical intervention, as is the case for removal of fixation devices. This makes lasso GBR a preferred method for the management of fenestration and dehiscence defects.
Conclusion
Clinicians must be cognizant of the potential difficulties of implant placement in the anterior maxilla, even when using guided implant surgery. Placement of shorter implants (<10 mm) may prevent apical implant fenestration. When a fenestration defect is identified, bone augmentation with or without implantoplasty should be performed, preferably before a sinus tract is formed. Preventive treatment may preclude the need for implant removal and retreatment. Taking into account the unique challenges associated with bone augmentation, lasso GBR offers significant advantages over conventional augmentation methods, including treatment predictability, stability, and long-term results.
Disclosure
Dr. Rodrigo Neiva has lectured for and received honoraria from Zimmer Biomet. Drs. Bruna and Gisele Neiva have conducted research for Zimmer Biomet.
About the Authors
Bruna T. Neiva, DDS, MS
Academic Director, Neiva Institute, Curitiba, Paraná, Brazil
Gisele F. Neiva, DDS, MS
Clinical Professor and Graduate Program Director, Department of Cariology, Restorative Sciences and Endodontics, University of Michigan School of Dentistry, Ann Arbor, Michigan
Rodrigo Neiva, DDS, MS
Chairman and Clinical Professor, Department of Periodontics, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania
References
1. Paul SJ, Jovanovic SA. Anterior implant-supported reconstructions: a prosthetic challenge. Pract Periodontics Aesthet Dent. 1999;11(5):585-590.
2. Jovanovic SA, Paul SJ, Nishimura RD. Anterior implant-supported reconstructions: a surgical challenge. Pract Periodontics Aesthet Dent. 1999;11(5):551-558.
3. Esposito M, Cardaropoli D, Gobbato L, et al. The role of dental implant abutment design on the aesthetic outcome: preliminary 3-month post-loading results from a multicentre split-mouth randomised controlled trial comparing two different abutment designs. Eur J Oral Implantol. 2018;11(1):77-87.
4. Bonde MJ, Stokholm R, Schou S, Isidor F. Patient satisfaction and aesthetic outcome of implant-supported single-tooth replacements performed by dental students: a retrospective evaluation 8 to 12 years after treatment. Eur J Oral Implantol. 2013;6(4):387-395.
5. Visser A, Raghoebar GM, Meijer HJ, et al. Care and aftercare related to implant-retained dental crowns in the maxillary aesthetic region: a 5-year prospective randomized clinical trial. Clin Implant Dent Relat Res. 2011;13(2):157-167.
6. Gehrke P, Degidi M, Lulay-Saad Z, Dhom G. Reproducibility of the implant crown aesthetic index-rating aesthetics of single-implant crowns and adjacent soft tissues with regard to observer dental specialization. Clin Implant Dent Relat Res. 2009;11(3):201-213.
7. Ku JK, Lee J, Lee HJ, et al. Accuracy of dental implant placement with computer-guided surgery: a retrospective cohort study. BMC Oral Health. 2022;22(1):8.
8. Yogui FC, Verri FR, de Luna Gomes JM, et al. Comparison between computer-guided and freehand dental implant placement surgery: a systematic review and meta-analysis. Int J Oral Maxillofac Surg. 2021;50(2):242-250.
9. Laverty DP, Buglass J, Patel A. Flapless dental implant surgery and use of cone beam computer tomography guided surgery. Br Dent J. 2018;224(8):601-611.
10. Choi W, Nguyen BC, Doan A, et al. Freehand versus guided surgery: factors influencing accuracy of dental implant placement. Implant Dent. 2017;26(4):500-509.
11. Cebrian-Carretero JL, Guinales-Diaz de Cevallos J, Sobrino JA, et al. Predictable dental rehabilitation in maxillomandibular reconstruction with free flaps. The role of implant guided surgery. Med Oral Patol Oral Cir Bucal. 2014;19(6):e605-e611.
12. Nocini PF, Castellani R, Zanotti G, et al. The use of computer-guided flapless dental implant surgery (NobelGuide) and immediate function to support a fixed full-arch prosthesis in fresh-frozen homologous patients with bone grafts. J Craniofac Surg. 2013;24(6):e551-e558.
13. Neiva R, Duarte W, Tanello B, Silva F. LASSO GBR - rationale, technique, and long-term results. Clin Oral Implants Res. 2018;29(suppl 17):447.
14. Adell R, Lekholm U, Rockler B, Branemark PI. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10(6):387-416.
15. Jung RE, Heitz-Mayfield L, Schwarz F, Groups of the 2nd Osteology Foundation Consensus Meeting. Evidence-based knowledge on the aesthetics and maintenance of peri-implant soft tissues: Osteology Foundation Consensus Report Part 3 - aesthetics of peri-implant soft tissues. Clin Oral Implants Res. 2018;29(suppl 15):14-17.
16. Giannobile WV, Jung RE, Schwarz F, Groups of the 2nd Osteology Foundation Consensus Meeting. Evidence-based knowledge on the aesthetics and maintenance of peri-implant soft tissues: Osteology Foundation Consensus Report Part 1 - effects of soft tissue augmentation procedures on the maintenance of peri-implant soft tissue health. Clin Oral Implants Res. 2018;29(suppl 15):7-10.
17. Schwarz F, Giannobile WV, Jung RE, Groups of the 2nd Osteology Foundation Consensus Meeting. Evidence-based knowledge on the aesthetics and maintenance of peri-implant soft tissues: Osteology Foundation Consensus Report Part 2 - effects of hard tissue augmentation procedures on the maintenance of peri-implant tissues. Clin Oral Implants Res. 2018;29(suppl 15):11-13.
18. Karateew ED. MAC and ZAC: clinical protocols for predictable implant aesthetics. Dent Today. 2014;33(9):90-94.
19. Kois JC, Kan JY. Predictable peri-implant gingival aesthetics: surgical and prosthodontic rationales. Pract Proced Aesthet Dent. 2001;13(9):691-698.
20. Tarnow DP, Eskow RN, Zamzok J. Aesthetics and implant dentistry. Periodontol 2000. 1996;11:85-94.
21. Migliorati M, Amorfini L, Signori A, et al. Internal bone temperature change during guided surgery preparations for dental implants: an in vitro study. Int J Oral Maxillofac Implants. 2013;28(6):1464-1469.
22. Landazuri-Del Barrio RA, Cosyn J, De Paula WN, et al. A prospective study on implants installed with flapless-guided surgery using the all-on-four concept in the mandible. Clin Oral Implants Res. 2013;24(4):428-433.
23. Malo P, de Araujo Nobre M, Lopes A. The use of computer-guided flapless implant surgery and four implants placed in immediate function to support a fixed denture: preliminary results after a mean follow-up period of thirteen months. J Prosthet Dent. 2007;97(6 suppl):S26-S34.
24. Lin CY, Pan WL, Wang HL. Facial fenestration and dehiscence defects associated with immediate implant placement without flap elevation in anterior maxillary ridge: a preliminary cone beam computed tomography study. Int J Oral Maxillofac Implants. 2018;33(5):1112-1118.
25. Kher U, Tunkiwala A, Umrigar Z. Management of fenestration defects during flapless immediate implant placement in the esthetic zone. Int J Periodontics Restorative Dent. 2015;35(6):e90-e96.
26. Kukreja BJ, Gupta U, Dodwad V, Kukreja P. Periosteal fenestration vestibuloplasty procedure for sulcus deepening in a hemimandibulectomy patient following implant therapy. J Indian Soc Periodontol. 2014;18(4):508-511.
27. Chan HL, Garaicoa-Pazmino C, Suarez F, et al. Incidence of implant buccal plate fenestration in the esthetic zone: a cone beam computed tomography study. Int J Oral Maxillofac Implants. 2014;29(1):171-177.
28. Steigmann M, Wang HL. Esthetic buccal flap for correction of buccal fenestration defects during flapless immediate implant surgery. J Periodontol. 2006;77(3):517-522.
29. Bianchini MA, Galarraga-Vinueza ME, Bedoya KA, et al. Implantoplasty enhancing peri-implant bone stability over a 3-year follow-up: a case series. Int J Periodontics Restorative Dent. 2020;40(1):e1-e8.
30. Sahrmann P, Luso S, Mueller C, et al. Titanium implant characteristics after implantoplasty: an in vitro study on two different kinds of instrumentation. Int J Oral Maxillofac Implants. 2019;34(6):1299-1305.
31. Stavropoulos A, Bertl K, Eren S, Gotfredsen K. Mechanical and biological complications after implantoplasty - a systematic review. Clin Oral Implants Res. 2019;30(9):833-848.
32. Bartee BK. Extraction site reconstruction for alveolar ridge preservation. Part 2: membrane-assisted surgical technique. J Oral Implantol. 2001;27(4):194-197.
33. Valentini P, Bosshardt DD. 20-year follow-up in maxillary sinus floor elevation using bovine-derived bone mineral: a case report with histologic and histomorphometric evaluation. Int J Oral Maxillofac Implants. 2018;33(6):1345-1350.
34. Rodriguez AE, Nowzari H. The long-term risks and complications of bovine-derived xenografts: a case series. J Indian Soc Periodontol. 2019;23(5):487-492.
35. Becker W, Clokie C, Sennerby L, et al. Histologic findings after implantation and evaluation of different grafting materials and titanium micro screws into extraction sockets: case reports. J Periodontol. 1998;69(4):414-421.
36. Demetter RS, Calahan BG, Mealey BL. Histologic evaluation of wound healing after ridge preservation with cortical, cancellous, and combined cortico-cancellous freeze-dried bone allograft: a randomized controlled clinical trial. J Periodontol. 2017;88(9):860-868.
37. Iorio-Siciliano V, Blasi A, Nicolo M, et al. Clinical outcomes of socket preservation using bovine-derived xenograft collagen and collagen membrane post-tooth extraction: a 6-month randomized controlled clinical trial. Int J Periodontics Restorative Dent. 2017;37(5):e290-e296.
38. Aimetti M, Manavella V, Corano L, et al. Three-dimensional analysis of bone remodeling following ridge augmentation of compromised extraction sockets in periodontitis patients: a randomized controlled study. Clin Oral Implants Res. 2018;29(2):202-214.
39. Parodi R, Santarelli G, Carusi G. Application of slow-resorbing collagen membrane to periodontal and peri-implant guided tissue regeneration. Int J Periodontics Restorative Dent. 1996;16(2):174-185.
40. Lifshey FM, Kang BB. A simple method of barrier membrane fixation for large sinus membrane tears. J Oral Maxillofac Surg. 2009;67(9):1937-1940.