Correction of an Anteriorly Constricted/Deep Bite Through Orthodontics and Restorative Enhancements: A 3-Year Case Study
Fred H. Peck, DDS
Abstract: A constricted chewing pattern can result in abnormal anterior wear, open interproximal contacts, diastemas, or temporomandibular disorder symptoms, which when combined with a deep bite often limits esthetic restorative options and requires orthodontic correction. This article discusses the case of a female patient with a constricted chewing pattern, severely worn mandibular teeth, and wide spaces on the maxilla closed with unesthetic crowns. The case report provides the step-by-step details necessary to transform a dentition with existing dental treatment and an unfavorable occlusion into one with a stable occlusion with a restored, beautiful smile.
A constricted chewing pattern (CCP) often may be misdiagnosed as bruxism and treated with a nightguard. However, the destructive forces of this condition occur primarily during normal daily activities with teeth in contact, such as chewing and swallowing.1 If CCP is left untreated, the patient may experience cracked and worn teeth with eventual vertical dimension collapse, which can be difficult to correct.
Clinical Case Overview
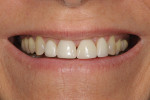
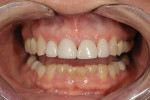
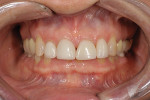
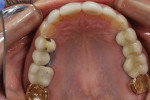
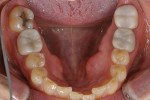
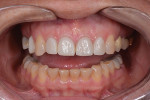
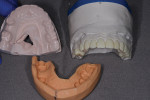
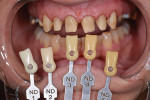
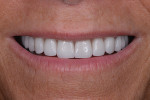
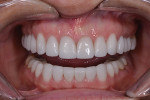
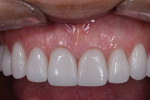
The patient, a 62-year-old woman, sought treatment to enhance her smile (Figure 1 and Figure 2). She was unhappy with her crowded mandibular anterior teeth, uneven tooth coloration, and wide maxillary anterior crowns, which flared facially (Figure 3). Many questionable and failing restorations were present. She reported constant clenching and had been prescribed a nightguard. She expressed interest in all options to improve her smile and function. A comprehensive examination was completed and clinical photographs were taken (Figure 4 through Figure 6).
Medical and Dental History
Pertinent medical history included mitral valve prolapse and gastric reflux. The patient's gastric reflux was evaluated by her physician and eliminated through diet and medication changes. She was American Society of Anesthesiologists (ASA) II classification.
With regard to the patient's dental history, she reported thermal sensitivity and chipped and broken teeth, with food catching between her teeth. She noted inadequate saliva but no new decay in the past 3 years. Teeth Nos. 4 and 13 were lost when they fractured several years earlier. Over the past 5 years, she noticed her teeth becoming thinner, spaces developing between the teeth, and clenching. She disliked the appearance of her teeth, including the maxillary right posterior bridge, and was self-conscious about her smile.
Diagnosis, Risk Assessment, and Prognosis
Periodontal: Periodontal examination revealed isolated 4 mm and 5 mm pockets, with bleeding on probing, and inadequate interproximal oral hygiene. Teeth Nos. 8 and 9 exhibited class II mobility, teeth Nos. 2, 4, 5 through 7, and 10 through 12 had class I mobility. She had no bone loss and was, therefore, diagnosed as American Academy of Periodontology (AAP) stage II, grade B.
Risk: Moderate
Prognosis: Fair
Biomechanical: Clinical examination revealed many extensively restored teeth, cracked veneers on teeth Nos. 7 through 10, and crowns with open and carious margins. The crown on tooth No. 12 was cracked and had thermal sensitivity. Many restorations had been previously repaired or replaced.
Risk: High
Prognosis: Poor
Functional: The patient had a 6 mm vertical overbite with attrition on the maxillary lingual and mandibular facial surfaces. Her occlusion was uncomfortable, cracks were noted in her anterior restorations, and she reported having to pull her jaw back and squeeze to get her posterior teeth to touch. Temporomandibular joint (TMJ)/Doppler examination revealed moderate crepitus due to the distalization of the patient's condyles.2 These findings were consistent with a diagnosis of CCP. Her masseter and temporalis muscles were hypertrophied; however, joint loading test caused no pain.
Risk: Moderate
Prognosis: Good
Dentofacial: The patient presented with improperly sized teeth, uneven gingival symmetry, and crowding. The maxillary gingiva showed when she smiled, and teeth Nos. 8 and 9 needed a more favorable height-to-width ratio. Her desire was to have an attractive white smile that was uniform in color and shape, but she was unable to be specific in her details and sought the clinician's advice.
Risk: Moderate
Prognosis: Fair
Treatment Goals
The treatment goals were to eliminate the gingival inflammation through hygiene treatment and improved home care, eliminate the CCP, restore teeth Nos. 7 through 10 for proper size as well as restore teeth Nos. 2 through 5, 11 through 15, and 20 through 29, and correct the gingival levels.3 The ultimate objective was to provide the patient a comfortable and stable occlusion with an esthetic smile.
Treatment Plan
Periodontal treatment would be completed first. Prior to orthodontic treatment, a diagnostic wax-up would be created. Provisional restorations would be placed on the maxillary arch, fabricated to facilitate correct orthodontic spacing of the teeth. The pontic replacing tooth No. 4 would be removed prior to orthodontics to allow for improved positioning of the adjacent teeth, which were too close together to accommodate an implant crown. Placement of an implant in the area of No. 4 was part of the initial treatment plan and proper spacing would be established during orthodontic treatment. The implant would be placed after orthodontic treatment. The orthodontic treatment would intrude teeth Nos. 8 and 9 and create ideal gingival margin positions. Teeth Nos. 23 through 26 would also be intruded to allow for final restorations with adequate tooth structure for support.4
The maxillary arch restorations would be completed first, proper centric relation (CR) would be determined, and then the mandibular restorations would be completed. The patient desired to keep the existing crowns on Nos. 18, 19, and 30, which were clinically acceptable. An orthodontic retainer would later be fabricated to keep the teeth stable and protect the occlusion.
Treatment Phases
Phase 1: Periodontal Treatment
The patient received routine scaling and oral hygiene instruction. Oral hygiene was improved, and pockets were eliminated prior to proceeding with orthodontic treatment. She was placed on a 4-month recall.
Phase 2: Diagnostic Wax-up, Provisionalization,
and Orthodontics
Photographs were taken and casts made. With the lips in repose the maxillary right cuspid was 1 mm apical to the upper lip. Tooth No. 6 had approximately 1 mm of incisal wear and, thus, was positioned well dentofacially for the maxillary incisaledge.5 For orthodontic planning purposes, placement of the maxillary anterior teeth would be guided by idealization of the gingival contours relative to the position of tooth No. 6. The maxillary incisor gingival margins would be intruded 2 mm to match the gingival margins of the cuspids. The lateral incisor gingival margins would be positioned approximately 0.5 mm coronal to incisors and cuspids. The mandibular anterior teeth had lost approximately 2 mm of incisal length and had supraerupted. They would be intruded to allow the planned restorations to be properly positioned while preserving natural tooth structure.
Crowns on Nos. 7 through 10 and the No. 4 pontic were removed. A polyvinyl siloxane (PVS) impression was taken to fabricate long-term polymethyl methacrylate (PMMA) single-unit provisional crowns. Caries was found under the crown on tooth No. 3 and removed, and Nos. 3 and 7 through 10 were temporized with bisphenol A-glycidyl methacrylate (bis-GMA) temporary restorations and luted with a temporary luting cement (UltraTemp™, Ultradent, ultradent.com). After the PMMA provisional restorations were fabricated, the bis-GMA provisionals were removed and the PMMA restorations were cemented with a self-adhesive resin cement (RelyX™ Unicem 2, 3M Oral Care, 3m.com).
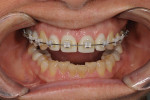
Orthodontic treatment was initiated with wire and brackets. During the 24-month orthodontic treatment time, regular progress checks verified that the tooth movement was consistent with the planned outcomes of incisal edge position, gingival level location, prescribed intrusion, buccal corridor expansion, and desired overbite and overjet (Figure 7 and Figure 8).
Phase 3: Post-orthodontic Treatment Planning
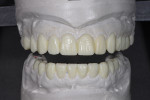
After orthodontic completion, maximum intercuspation(MIP) coincident with CR was verified utilizing a chairside deprogrammer bonded to the lingual surfaces of teeth Nos. 8 and 9. New photographs and models were taken and mounted in MIP on a Panadent articulator utilizing a Kois dentofacial analyzer (Kois Center, koiscenter.com) and then sent to the laboratory for a diagnostic wax-up (Figure 9 and Figure 10).6 The clinician determined from the diagnostic wax-up that to maintain a 4 mm preparation height for ideal retention and minimize tooth reduction, the vertical dimension needed to be opened 1 mm, which would allow up to 2 mm to 3 mm of additional space in the anterior region.7 This change was added to the wax-up. A try-in of the proposed restorative treatment was done with bis-GMA resin in a putty matrix (MirrorImage™, Cosmedent, cosmedent.com) (Figure 10). The patient accepted the proposed esthetic outcome.
Phase 4: Definitive Maxillary Restorations
The provisional restorationson teeth Nos 3 through 7 and 10 through 14 were removed and those teeth prepared. In order to stabilize the occlusal records, the existing crowns on teeth Nos. 2 and 15 were left intact and would be completed after cementation of the definitive restorations on teeth Nos 3 and 5 through 14. A composite deprogrammer stop was placed on the lingual of the provisional crowns Nos. 8 and 9, and the patient was reclined 45 degrees and instructed to repeatedly close lightly. CR was confirmed when only one point of contact was present on the deprogrammer, at an increased vertical dimension with no contacts on Nos. 2 and 15, and a bite registration was taken at the increased vertical dimension. Provisional crowns on teeth Nos. 8 and 9 were then removed, and the maxillary crown preparations were finalized, retraction cords were placed, and a PVS impression was taken. Shades were determined using the IPS Natural Die Material Shade Guide (Ivoclar Vivadent, ivoclarvivadent.com) (Figure 11). Temporary crowns were fabricated with MirrorImage shade B1 using the putty matrix. Layered IPS e.max® porcelain (Ivoclar Vivadent) was chosen for teeth Nos. 4 through 13 to maximize esthetics, and monolithic e.max was used on the molars for additional strength.
When the patient returned for cementation, the teeth were anesthetized, retraction cords were placed, and the teeth were sandblasted with 27-micron aluminum oxide. The crowns were tried in and approved by the clinician and the patient for interproximal contacts, occlusion, and esthetics. All intaglio surfaces of the crowns were etched, silanated, and then cemented (RelyX Unicem 2). The occlusion was verified and adjusted with 8-micron articulating paper (TrollFoil, TrollDentalUSA, trolldentalusa.com). Lateral excursions were checked, and marks on inclined planes were removed as detected with red occlusal articulating film (AccuFilm®, Parkell, parkell.com). The patient then sat upright and chewed on 200-micron paper to verify proper occlusion with no interferences in the envelope of function. She was then dismissed and scheduled for e.max crowns on teeth Nos. 2 and 15 and the implant abutment and crown on the new implant in the area of No. 4. The abutment for the implant (NobelReplace® Conical Connection, NP 3.5 mm, Nobel Biocare, nobelbiocare.com) was fabricated with zirconia. Occlusion was again verified and adjusted as needed.
Phase 5: Definitive Mandibular Restorations
The patient returned to the office for preparation of teeth Nos. 20 through 29. The teeth were prepared in the same manner described for the maxillary arch. PVS impressions of both arches were taken. A CR bite was taken along with a new Kois dentofacial analyzer recording. Provisional restorations were fabricated from a putty matrix created from the diagnostic wax-up. Monolithic e.max was selected for increased strength.
At the insertion appointment, the same protocols described for the maxillary crowns were followed. The occlusion was adjusted, all interferences were removed in lateral excursions, and the patient was again seated upright to remove any lingual streaks to ensure there was no remaining CCP. She returned to the orthodontist for fabrication of final retainers to maintain the achieved occlusion and esthetic outcome (Figure 12 through Figure 15).
Discussion
Evaluation of a patient's dental issues requires the use of a systematic approach to diagnose and treat underlying conditions to ensure a predictable, successful outcome. In the present case, the patient was willing to complete the treatment as presented; no shortcuts were taken, and she followed post-insertion treatment recommendations. Three years after completion, no complications have been noted and the esthetics remain excellent.
Conclusion
When she presented, the patient was unhappy with the appearance of her smile. After a complete diagnosis, periodontal issues were detected along with a CCP, unattractive crowns, and uneven gingival levels. Tooth positions dictated that restorative changes alone could not fully address her concerns. Orthodontics would be required to move teeth to a more favorable position and correct her CCP. The treatment plan was implemented, and provisional crowns were placed prior to orthodontics. A diagnostic wax-up was completed, an implant was placed, the upper arch was restored with an increased vertical dimension, and most of the lower arch was restored. The CCP was eliminated, gingival levels were aligned, and the results were predictable, enabling the patient to have a beautiful and functional smile. An additional benefit was that the hypertrophied masseter and temporalis muscles that were present prior to treatment returned to their normal size, giving her face a thinner, more appealing appearance.
Acknowledgment
Acknowledging that this case was a team effort, the author thanks Dwight Rickert, CDT, for his exceptional artistic ceramic skills in all aspects of the laboratory phases of the treatment, and Kent Morris, DMD, for the excellent orthodontic results.
Disclosure
The author lectures on behalf of Cosmedent and Clinician's Choice but did not receive any compensation or material support related to this patient's treatment or this article.
About the Author
Fred H. Peck, DDS
Private Practice, Cincinnati, Ohio; Accredited Fellow, American Academy of Cosmetic Dentistry; Fellow, International College of Dentists
References
1. Dawson PE. Functional occlusion: from TMJ to smile design. J Indian Prosthodont Soc. 2007;7(1):49.
2. Rebibo M, Darmouni L, Jouvin J, Orthlieb JD. Vertical dimension of occlusion: the keys to decision. J Stomat Occ Med. 2009;2(3):147-159.
3. Chu SJ, Tan JHP, Stappert CFJ, Tarnow DP. Gingival zenith positions and levels of the maxillary anterior dentition. J Esthet Restor Dent. 2009;21(2):113-120.
4. Fitzgerald MW. Overcoming esthetic, functional, and biomechanical challenges with assistance from orthodontic intrusion. Compend Contin Educ Dent. 2019;40(4):246-250.
5. Misch CE. Guidelines for maxillary incisal edge position-a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.
6. Simon H, Magne P. Clinically based diagnostic wax-up for optimal esthetics: the diagnostic mock-up. J Calif Dent Assoc. 2008;36(5):355-362.
7. Kois JC, Phillips KM. Occlusal vertical dimension: alteration concerns. Compend Contin Educ Dent. 1997;18(12):1169-1174.