Preventing Porcelain Fractures During Endodontic Treatment
Kenneth P. Goldstein, DMD; Ronald E. Goldstein, DDS; Brandon Englert; Nathaniel C. Lawson, DMD, PhD; and Thomas J. Lucas, DMD, PhD
Abstract: Attempting endodontic access through ceramic or veneering porcelain can be wrought with challenges. Clinicians must take every precaution to assist patients who are in pain without causing harm through chipping or fracturing the restoration. This article discusses strategies clinicians can consider when facing the task of achieving endodontic access through an all-ceramic crown.
Most dentists have experienced a scene similar to this one: It's late on a Friday afternoon, and the last patient of the day, who is in pain, needs a root canal through a brand new ceramic crown. Part of the dental creed is to do no harm. It is a dentist's duty to help patients who are in pain without causing them any harm or distress. This harm has many different facets. From an endodontic standpoint, the thought of drilling through an all-ceramic crown can lead to apprehension and uncertainty regarding chipping or fracturing the ceramic or veneering porcelain during the access preparation, which can lead to esthetic or functional failures.
Open Communication
At this point, if possible, it may be helpful to call the referring dentist to find out what type of ceramic system (zirconia vs lithium disilicate; monolithic vs layered) was used for the crown. Alternatively, a radiograph may aid in determining the crown material. (Zirconia has a radiopacity similar to metal, whereas lithium disilicate and porcelain have a radiopacity similar to tooth structure.)
Once the pulpal diagnosis is made and the patient is aware of the need for endodontic treatment, an informed consent should be signed by the patient, dated, and the signing witnessed. Part of the language of the consent form must include a possible risk of fracturing or chipping the ceramic crown while the endodontic access is performed. The patient must understand that if the ceramic or veneering porcelain chips or fractures, the result may be an esthetic or functional failure and a new crown may be needed. However, the restorative dentist may be able to repair the crown. Having this conversation with the patient and documenting it in the patient's record along with the signed consent with proper language can mitigate the "blame game" and possibly dismiss any charges of negligence.
Access Challenges
Endodontic access through layered restorations presents a challenge because there is a relatively thin layer of veneering porcelain that must be accessed first, and this veneering porcelain is weaker than the core material. Both the clinician and patient must realize that porcelain is a brittle, glass-based material, and drilling through it can create microfractures that can weaken the structure of the restoration and lead to future failures. Haselton et al examined endodontic access through 30 layered all-ceramic crowns.1 The study found that both diamond and tungsten carbide burs caused edge chipping, microcracks, and fractures at equal rates. The study also noted that just drilling on the porcelain to create the endodontic access could weaken the porcelain bond, which can cause chipping or fractures. Furthermore, the vibration of the bur on the porcelain could also disturb the cement bond of the crown, thus potentially causing microcracks.
Another interesting component of porcelain fractures in relation to endodontic treatment is the damage that rubber dam clamps can cause, such as cracks and pits in the cervical porcelain, which could also lead to the porcelain debonding from the core.2 In a study by Wood et al, 24 layered alumina and 24 layered zirconia crowns exhibited edge chipping around the access openings. Four zirconia crowns even showed radial crack formation of the porcelain around the access openings. The authors concluded that endodontic access through layered all-ceramic crowns resulted in significant altered structural integrity of the porcelain causing loss of bond between the veneering porcelain and core.3
Proper Bur Selection
Along with preventing delamination of the layering porcelain, choosing the right type of access bur can also minimize the frequency of microfractures in porcelain. Unfortunately, porcelain has a relatively low fracture toughness, which can be defined as "a measurement of the material's resistance to brittle fracture when a crack or flaw is present." Over time, weakened porcelain can fail due to "constant cyclic fatigue by crack propagation."4 According to Sutherland et al, the use of diamond burs with copious amounts of water is recommended during endodontic access to minimize chipping and fracture of the porcelain.5
So, what type of diamond bur should clinicians be using to make access through porcelain? In a study by Stokes and Tidmarsh, a coarse diamond eliminated vibration or "chatter," which can be bothersome to patients, but the cutting efficiency relates to grit size and bur shape. The study concluded that the extra-coarse dome-ended cylinder diamond bur was able to cut smoothly and prevent microfractures of the five access preparations made.6 However, an in vitro study by Rues et al in which the fracture resistance of layered zirconia crowns was measured using diamond-coated burs of grit sizes 46 µm, 107 µm, and 151 µm concluded that the use of the larger-grit size burs caused increased fracturing of the layered zirconia crowns and even caused deep scores in the veneered layer, which could result in crack propagation.7 Therefore, using a smaller-grit size diamond bur when preparing the access through porcelain should minimize the potential for fractures.
Zirconia and Lithium Disilicate
Accessing through monolithic zirconia and lithium-disilicate restorations presents a different challenge, as these materials are harder to cut through than porcelain. In a study by Qeblawi et al, a smaller-grit size diamond bur, such as 126 µm, used for endodontic access preparations did not alter the failure load of lithium-disilicate restorations. However, use of larger-grit diamond burs reduced the failure load of bonded restorations, which could result in cracks or fractures.8 In a systematic review by Gorman et al, the authors reported the effects of microcracks at the access cavity, repair protocols, ceramic type, crown fabrication method, luting agent, and grit size of the diamond bur on the strength of monolithic ceramic crowns. A "best practice" protocol for improving the fracture resistance of endodontically accessed all-ceramic crowns could not be identified.9
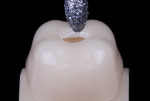
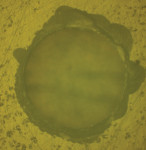
A recent ongoing study by Lucas et al compared a ceramic removal diamond bur (150 µm to 200 um) to a fine diamond bur for endodontic access.10 In the study, a 2.5 mm access hole was placed in the center of 1 mm thick bonded lithium disilicate and 0.8 mm cemented zirconia crowns (Figure 1). The access holes were examined with transillumination and no radial cracks were noted (Figure 2). Surprisingly, the fine diamond bur caused more edge chipping around the endodontic access hole (Figure 3 and Figure 4). After testing in compression (Figure 5), it was determined that accessing the crowns with a fine diamond led to a lower crown fracture strength in lithium-disilicate crowns and similar fracture strength with zirconia crowns. Additionally, the ceramic removal diamond bur was more efficient in cutting through both zirconia and lithium disilicate.
Outside Factors
No matter how careful the endodontist is in accessing through a porcelain crown, fractures can happen that may be beyond the clinician's control. According to Winter, using a diamond bur at too high of a revolutions per minute (RPM) speed can cause excessive trauma, vibration, and heat, which can lead to microcracks. These cracks can propagate and cause chipping of the porcelain leading to a restoration failure. Another condition that is beyond the clinician's control is strictly technical. If the ceramic restoration is thinner than the manufacturer's recommendation, cracking, chipping, or fractures can occur while accessing through the porcelain.11
Conclusion
In summary, consent should be obtained from the patient. If the crown is veneered with porcelain, a fine diamond bur may likely be used for access. For a monolithic-disilicate or zirconia crown, a coarse ceramic removal diamond bur should be considered. Additional study on this topic is recommended.
Disclosure
This project was supported by an Alpha Omega Foundation Grant as well as a donation from Brasseler.
About the Authors
Kenneth P. Goldstein, DMD
Private Practice in Endodontics, Atlanta, Georgia; Fellow, Academy of General Dentistry
Ronald E. Goldstein, DDS
Clinical Professor, Department of Restorative Sciences, Dental College of Georgia at Augusta University, Augusta, Georgia
Brandon Englert
First-Year Dental Student, Division of Biomaterials, School of Dentistry, University of Alabama at Birmingham, Birmingham, Alabama
Nathaniel C. Lawson, DMD, PhD
Associate Professor, Division of Biomaterials, School of Dentistry, University of Alabama at Birmingham, Birmingham, Alabama
Thomas J. Lucas, DMD, PhD
Endodontic Resident, School of Dentistry, University of Alabama at Birmingham, Birmingham, Alabama
References
1. Haselton DR, Lloyd PM, Johnson WT. A comparison of the effects of two burs on endodontic access in all-ceramic high lucite crowns. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2000;89(4):486-492.
2. Madison S, Jordan RD, Krell KV. The effects of rubber dam retainers on porcelain fused-to-metal restorations. J Endod. 1986;12(5):183-186.
3. Wood KC, Berzins DW, Luo Q, et al. Resistance to fracture of two all-ceramic crown materials following endodontic access. J Prosthet Dent. 2006;95(1):33-41.
4. Helvey GA, Lowe E, Rego N, Williams B. Roundtable: As material science advances, what common "myths" exist regarding porcelain dental restorations? Compend Contin Educ Dent. 2019;40(5):268-270.
5. Sutherland JK, Teplitsky PE, Moulding MB. Endodontic access of all-ceramic crowns. J Prosthet Dent. 1989;61(2):146-149.
6. Stokes AN, Tidmarsh BG. A comparison of diamond and tungsten carbide burs for preparing endodontic access cavities through crowns. J Endod. 1988;14(11):550-553.
7. Rues S, Schwindling FS, Meyer A, et al. Fracture resistance of zirconia-based all-ceramic crowns after bur adjustment. Eur J Oral Sci. 2017;125(4):310-313.
8. Qeblawi D, Hill T, Chlosta K. The effect of endodontic access preparation on the failure load of lithium disilicate glass-ceramic restorations. J Prosthet Dent. 2011;106(5):328-336.
9. Gorman CM, Ray NJ, Burke FM. The effect of endodontic access on all-ceramic crowns: a systematic review of the in vitro studies. J Dent. 2016;53:22-29.
10. Lucas TJ, Lawson NC, Englert B, et al. Fracture strength of zirconia and lithium disilicate restorations following endodontic access. J Esthet Restor Dent. 2021. doi: 10.1111/jerd.12829.
11. Winter R. Ceramic restorations: why do they break? Spear website. October 2, 2014. https://www.speareducation.com/spear-review/2014/10/ceramic-restorations-break-bob-winter#:~:text=The%20two%20most%20common%20reasons,heat%2C%20which%20cause%20the%20microflaws. Accessed March 2, 2022.