A Multidisciplinary Approach to Conservatively Treat a Worn Dentition
John Scalas, DDS
Abstract: This case report demonstrates how a patient whose initial complaint involving "chipped and broken front teeth" was provided improved function, esthetics, and prognosis through a multidisciplinary treatment approach. In this example of timely, conservative, and judicious use of several disciplines of dentistry, orthodontic treatment was employed to increase the amount of restorative space available for restoring the patient's maxillary anterior teeth, periodontal therapy was utilized to address gingival inflammation, and conservative restorative dentistry featuring enamel-bonded porcelain veneers was used to restore tooth length and improve the patient's smile.
Many clinicians have patients who come into their practice desiring a more youthful smile. Often, these patients have teeth that have prematurely worn down, are shorter than some of their other teeth, and may have uneven edges, and the patient would like these teeth lengthened and straightened. Before deciding on a course of treatment, however, it is important for the clinician to diagnose why the teeth have worn down prematurely, which will also help lead to a predictable treatment plan.
In the following case, the clinician had to determine whether the patient's excessive wear was due to a friction chewing pattern, constricted chewing pattern, dysfunction, or parafunction. The findings led to a conservative treatment plan.
Clinical Case Overview
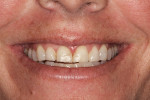
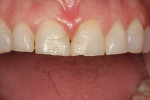
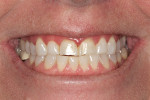
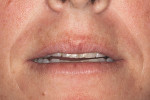
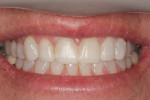
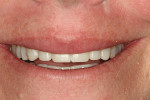
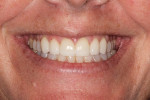
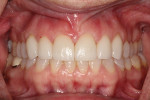
A 35-year-old woman, who had been a patient at the treating clinician's practice since childhood, expressed interest in improving the appearance of her front teeth, which displayed a considerable amount of wear and some chipping (Figure 1 through Figure 3). Her medical history was American Society of Anesthesiologists (ASA) II due to her history of hypertension, which was successfully treated with Diovan®. Otherwise, her health history was noncontributory.
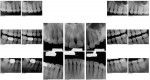
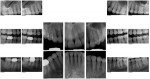
The patient's dental history revealed some restorative care and missing third molars, which were removed during her teens (Figure 4). She also had a history of previous orthodontic care during childhood. Her main concern was the unsightly look of the chipped, short, and uneven edges of teeth Nos. 6 through 11.
The patient noted that her teeth had gotten shorter over the past 5 years, and that she could no longer locate a repeatable bite position. She also reported that her gums had recently become progressively redder and more inflamed (Figure 5).
Diagnosis, Risk Assessment, and Prognosis
Periodontal: Clinical and radiographic examination revealed bleeding on probing in all four quadrants, probing depths of 2 mm to 4 mm, and bone heights generally 3 mm from the cementoenamel junction. There was no appreciable mobility. Generalized horizontal attachment loss of 1 mm to 2 mm was noted along with moderate gingival inflammation on teeth Nos. 6 through 11. She was, therefore, classified as American Academy of Periodontology (AAP) stage II, grade B. The patient had generally maintained a consistent 6-month recall interval since childhood, but in recent months the demands of family and work had interfered with both her recall and homecare regimen.
Risk: Moderate
Prognosis: Fair
Biomechanical: Teeth Nos. 6 through 11 and 22 through 27 had moderate attrition. The patient's mandibular first molars had been restored with full-coverage restorations, resulting in an increased risk for future root canal treatment.1 The mandibular second molars had occlusal composite restorations. Teeth Nos. 8 and 9 had facial abrasions of unknown etiology. No active caries were noted.
Risk: Moderate
Prognosis: Fair
Functional: The patient reported having "more than one bite" on the dental history. She was also aware that her teeth had become shorter in the past 5 years. She reported no temporomandibular joint disorder symptoms, and clinical evaluation revealed no pain, soreness, or joint sounds. Load and immobility tests were within normal limits, and maximal opening was 54 mm with no deviations. Muscle palpations were negative as well. The occlusal diagnosis was occlusal dysfunction.
Risk: Moderate
Prognosis: Fair
Dentofacial: The patient presented with high lip dynamics, normal scallop form, and horizontal symmetry. In repose, her maxillary right canine extended 1 mm below the lip ("plus 1"), while the incisal edge of the left canine was even with resting lip, or "cuspid zero" (Figure 6).2 Her lip moved up 11 mm when changing from repose to a Duchenne smile, resulting in a diagnosis of upper lip hypermobility.3
Risk: High
Prognosis: Hopeless
Treatment Plan
The clinician presented a comprehensive treatment plan that he considered ideal for the patient. It included periodontal therapy, orthodontic treatment, and restorative care, and the patient agreed to the plan.
Periodontal therapy was recommended to address the patient's gingival inflammation, which had increased during her absence from dental care. There were two primary goals for orthodontics. First, to address the functional problem-occlusal dysfunction-treatment was orthodontically driven to create equal-pressure, bilateral, simultaneous contacts on all posterior teeth. Occlusal dysfunction often presents with multiple areas of wear, including on anterior and posterior teeth, and is often accompanied by avoidance patterns and oral habits, such as chewing on pencils or nail biting. This may be differentiated from true parafunction, which typically presents with flattened wear on all teeth and is mediated by the central nervous system. Occlusal dysfunction is further differentiated from a constricted chewing pattern, which often involves wear on maxillary lingual and mandibular facial anterior tooth surfaces and the patient reporting the feeling of having their jaw "pushed back."4,5 The second main goal of the orthodontic treatment was movement of the anterior teeth, which was driven by the restorative needs for adequate space to re-establish natural shape and contour to teeth Nos. 6 through 11. The restorative treatment would utilize conservative, enamel-bonded porcelain veneers to restore the loss of tooth length and improve the patient's smile.
Treatment Phases
Periodontal
The patient underwent four appointments of scaling and root planing with local anesthetic, followed by one visit of fine scaling and polishing. At 6 weeks, a re-evaluation of her periodontal health was performed. Her bleeding and inflammation had greatly improved, and 4 mm pocket depths had decreased to 3 mm. The clinician determined that a 3-month periodontal maintenance interval would be best initially to confirm that her homecare was adequate to maintain her improved periodontal health. The long-term goal was to return to a 6-month recare interval.
Orthodontics
Through orthodontics, the clinician was able to address the patient's complaint of having "more than one bite" by improving her cusp/fossa relationship. The orthodontist was also able to create room for her future veneers by proclining teeth Nos. 7 through 10 five degrees (based on the maxillary central incisor to sella-nasion [SN] angle) and intruding teeth Nos. 22 through 27 1.5 mm, as established with a wax-up and tooth mock-up at repose and "cuspid zero."
Post-Orthodontics
The occlusion was equilibrated, both after orthodontic therapy and after delivery of the veneers, to ensure that a stable and nondestructive functional position was achieved.6,7 Equal-pressure, bilateral, simultaneous contacts were achieved on all posterior teeth with very light cuspid contact and no contact on incisors in maximum intercuspation. Further, with the patient reclined 45 degrees, equal, bilateral posterior contacts were confirmed using 200-micron blue articulating paper (Bausch, bauschpaper.com), followed by the use of 8-micron foil (TrollFoil™, TrollDental, trolldental.com). Finally, the patient was seated upright to confirm, with the use of 200-micron paper, that no chewing envelope interferences were present. No marks were evident on teeth Nos. 7 through 10, nor were there any heavy streak marks on teeth Nos. 6 and 11.
Restorative
After 6 months of orthodontic retention to lower the incidence of immediate relapse, an intraoral mock-up was fabricated by the lab technician. Teeth Nos. 6 through 11 were waxed to their ideal length and contour, and a putty matrix was fabricated. The clinician filled the matrix with a bis-acrylic self-cure provisional material (Structur, VOCO America, voco.com) and placed it over the teeth. After 1 minute and 45 seconds, the material had cured, and the putty matrix was removed (Figure 7 and Figure 8). The bis-acrylic material was left on the teeth, and appropriate depth cuts were made through the material. This technique allows for maximum tooth structure preservation. Because the orthodontic treatment had increased the anterior interdental space, only 0.5 mm of additional incisal reduction was necessary to create an adequate 2 mm incisal reduction. The clinician achieved this minimal reduction using a Brasseler® 330 bur (Brasseler USA, brasselerusa.com), and a Brasseler® KS1 bur was used for the rest of the teeth preparation, which was entirely in enamel. This approach reduced biomechanical risk as less tooth structure was removed than if full-coverage, cohesive restorations had been used.
After impressions were taken, the teeth were provisionalized using the aforementioned bis-acrylic self-cure provisional material and spot-bonded with flowable composite, followed by a 20-second light cure. The patient returned 2 weeks later for the final placement.
Cementation Procedure
After try-in of the six veneer restorations (IPS e.max®, Ivoclar Vivadent, ivoclarvivadent.com) and confirmation of esthetics and proper fit, the veneers were cleaned using 37% phosphoric acid. The phosphoric acid was gently scrubbed on the internal surface of each veneer for 60 seconds, then the veneers were placed in an ultrasonic bath filled with deionized water for 5 minutes. The veneers were then dried, and silane was placed on them for 60 seconds and allowed to air-dry. The teeth were etched with phosphoric acid for 20 seconds, rinsed, and a thin layer of a universal bonding agent (All-Bond Universal®, BISCO, bisco.com) was placed. The bonding agent was thinned with an air syringe and cured for 20 seconds.
Translucent veneer cement (RelyX™ Veneer Cement, 3M Oral Care, 3m.com) was used as the luting agent, and the veneers were seated two at a time, starting with the central incisors, followed by the lateral incisors, then, finally, the cuspids. Each restoration was tacked in placed with a 3-second light-cure, and excess cement was removed with a posterior scaler. The final cure was accomplished by light-curing for an additional 20 seconds per tooth.
The post-treatment results are shown in Figure 9 through Figure 12.
Discussion
The patient was enthusiastic to move forward with treatment to address her multiple dental issues and, after periodontal, orthodontic, and restorative care, was thrilled with the results. The total treatment time was 14 months. With continued periodontal recall, the patient's periodontal risk remains moderate, and her prognosis has improved.
Biomechanically, the patient's risk was unchanged as the completed treatment involved enamel-borne, adhesively placed lithium-disilicate veneers. The prognosis remains moderate.
Functionally, the patient's risk was decreased from moderate to low, because her function is now stable and acceptable. This was achieved through orthodontic therapy, carefully controlling and equilibrating her occlusion, and correctly planning and delivering the veneer restorations. The patient's dentofacial risk remained unchanged as no treatment (eg, botulinum toxin injection or lip lengthening) was provided to address the amount of gingival display due to her high lip line. The patient expressed no concern either pre- or postoperatively about her gingival or tooth display when smiling. Her prognosis improved because the treatment resulted in a more harmonious tooth and gingival appearance.
The clinician decided against splint fabrication post treatment, as the patient's new occlusion was stable and very comfortable.
Conclusion
This case report demonstrates how a clinician can conservatively treat a worn dentition. Clinicians are often faced with this same challenge, and through judicious treatment planning, risk assessment, and the use of a multidisciplinary approach the desired esthetic outcome can be achieved while restoring a minimal number of teeth.
Acknowledgment
The author thanks Susan A. Sheets, DDS, Kois Center Editor-in-Chief, for her help in writing this article.
About the Author
John Scalas, DDS
Private Practice, Cypress, California
References
1. Jackson CR, Skidmore AE, Rice RT. Pulpal evaluation of teeth restored with fixed prostheses. J Prosthet Dent. 1992;67(3):323-325.
2. Misch CE. Guidelines for maxillary edge position - a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.
3. Robbins JW. Differential diagnosis and treatment of excess gingival display. Pract PeriodonticsAesthet Dent. 1999;11(2):265-272.
4. Lavigne G, Kato T. Usual and unusual orofacial motor activities associated with tooth wear. Int J Prosthodont. 2005;18(4):291-292.
5. The glossary of prosthodontic terms: ninth edition. J Prosthetic Dent. 2017;117(5S):e1-e105.
6. Kois J, Hartrick N. Functional occlusion: science-driven management. J Cosmetic Dent. 2007;23(3):54-57.
7. Dawson PE. Centric relation. Its effect on occluso-muscle harmony. DentClinNorthAm. 1979;23(2):169-180.