A Clinical Guide for Treatment of Dental Cervical Lesions Through a Restorative, Surgical, or Combination Approach: A Proposed Evidence-Based Algorithm
Neel B. Bhatavadekar, BDS, MS, MPH; Amit S. Gharpure, BDS, MSD; and Ricardo Kern, BDS, DClinDent, MSc
ABSTRACT
The incidence of dental cervical carious and noncarious lesions is common, and often these are treated with a restorative material without due attention paid to the amount of exposed cementum/enamel, level of interproximal bone, and final desired esthetic result. This article is intended to provide clinicians an evidence-based clinical decision tree for treating such lesions through a restorative, surgical, or combination approach such that the optimum functional and cosmetic result is achieved.
With a steady increase in the geriatric population occurring, there has been a growing interest in the management of cervical lesions, both carious and noncarious.1 Such lesions are important components for long-term oral health. Cervical lesions pose several concerns, such as poor esthetic appearance, dentin hypersensitivity, and bacterial plaque accumulation due to the anatomy of the defect making oral hygiene challenging. Several factors are considered to play a role in the etiology of these lesions,2 and there is consensus that these lesions are due to multifactorial conditions.2,3 In addition to being a source of tooth sensitivity and plaque retention, these lesions may inhibit structural integrity and pulp vitality and can pose challenges for successful restoration.2,3
The management of such lesions relies heavily on an accurate diagnosis based on several restorative and periodontal factors identified by evaluating a patient's medical and dental history and providing a thorough clinical evaluation. Although several guidelines have been proposed for the management of noncarious cervical lesions,4,5 to the best of the authors' knowledge previously published studies do not include a comprehensive surgical and restorative evidence-based decision tree for both carious and noncarious lesions. The restorative, surgical, or combination (RSC) approach differs from previous decision trees in that it provides an evidence-based treatment algorithm to sequence and manage both carious cervical lesions (CCLs) and noncarious cervical lesions (NCCLs). Thus, the objective of this article is to provide a comprehensive guide using a restorative, surgical, or combination approach for the diagnosis and management of both carious and noncarious cervical lesions.
Classification of Cervical Lesions Based on Etiology
The first step for successful therapy is early identification of the etiological agents. This can be done by evaluating the patient's medical and dental history and through a comprehensive clinical examination in which erosion, abrasion, and abfraction are checked.
Erosion: Erosion represents tooth surface loss caused by chemical action, and this can be endogenous (due to gastroesophageal acid reflux) or exogenous (caused by intake of citrus fruits, carbonated soft drinks, and other highly acidic fruits).2 The diagnosis of early form of erosion is difficult since it has few signs and symptoms. Therefore, clinical appearance is the most important feature for diagnosing this condition. Typical presentation involves a smooth, silky glazed, sometimes dull enamel with the absence of perikymata and intact enamel along the gingival margin.6
Abrasion: Abrasion is the result of friction between a tooth and an exogenous agent.7 These lesions often occur due to overzealous toothbrushing, improper use of dental floss and/or toothpicks, and detrimental oral habits. They usually appear as painless cavities with polished surfaces but may also present with pain. The enamel resists differently than dentin, eroding following the path made by the toothbrush, causing a characteristic V-shaped lesion.7 Occasionally, masticatory abrasion may occur on the facial and lingual aspects of teeth, when coarse food (eg, granolas, nuts, bran cereal) is forced against these surfaces by the tongue, lips, and cheeks during mastication.
Abfraction: Abfraction is thought to take place when excessive cyclic, nonaxial tooth loading leads to cusp flexure and stress concentration in the vulnerable cervical region of teeth. Such stress is then believed to directly or indirectly contribute to the loss of cervical tooth substance.8 However, involvement of abfraction lesions has long been controversial when it comes to treatment of cervical lesions. There is only a small amount of experimental evidence for abfraction, and most literature is predominantly from finite element analysis studies.9
Frequently, more than two mechanisms may be involved in the etiology of tooth surface lesions (both CCLs and NCCLs). Therefore, clinicians need to be aware of the multifactorial etiology of cervical lesions so they may be able to appropriately treatment plan for the patient.
Treatment Options
Treatment options for cervical lesions are summarized as follows:
Manage etiology: The first step in treatment of cervical lesions is to manage the etiology. Erosion lesions caused by endogenous etiology such as gastroesophageal acid reflux would need medical management. For erosive lesions caused by an exogenous source, diet modification and oral hygiene instruction is recommended. Lesions caused by abrasion require modification of brushing technique and oral hygiene instruction. Occlusal adjustment may help in abfraction lesions, but their association is highly controversial.9 CCLs need plaque control, diet modification, and oral hygiene instruction for prevention and to stop further progression.
Restorations: Several different materials have been used and studied for restoration of cervical lesions ranging from glass-ionomer cements and composites to resin-modified glass-ionomer cements.10 There is insufficient evidence to recommend any specific material for routine use in the restoration of cervical lesions. There seems to be higher success for bonding to enamel than to dentin and cementum.10 Thus, restorative treatment appears to be more effective in lesions that are limited to anatomic crowns involving mainly enamel and coronal dentin.
Autogenous connective tissue grafts: Autogenous connective tissue grafts (CTGs) from the palate have been successfully used to gain root coverage for gingival recession.11,12 Several different techniques for harvest and donor site incisions have been proposed and compared.13-16 All the techniques have provided predictable long-term results for root coverage and have demonstrated an increase in keratinized tissue width and soft-tissue volume.17,18 Several explanations have been proposed for the benefits of using a CTG with a coronally advanced flap for treatment of cervical lesions.4,19,20 The presence of the CTG beneath the flap may prevent flap collapse inside the dead space created by the anatomy of cervical lesions, provide adequate flap support, and, in turn, enhance stability.4,19,20 Further, the addition of a CTG may increase keratinized tissue width and soft-tissue volume.17,18 Thus, CTGs provide a good treatment option for treating cervical lesions with root surface involvement (cementum and/or dentin).
Combination approach: In cervical lesions that involve both the anatomic crown and root (enamel, cementum, and/or dentin), a combination approach of restoration and CTG is necessary.4 Frequently, restorative procedures are adopted as the only treatment. There are several technical issues in restoring such areas, such as difficulty in access and field isolation, the variable microstructural characteristics of enamel and dentin, unsuitability as a substrate for adhesion,21 and biomechanical stress concentration.22 The anatomic arrangement of the hard and soft tissues at this location may make it difficult to obtain a perfect marginal seal and may affect the long‐term success for cervical restorations. Further, the placement of subgingival restorations results in marginal bleeding, attachment loss, and gingival recession23 caused by an increasing amount of bacterial biofilm and changes in its composition. A combination approach with a restoration and CTG has been shown in previously published randomized controlled trials to have greater results than restorations alone.24,25 Therefore, cervical lesions with root and crown involvement would benefit from a combination of restorative and periodontal surgical management.
Treatment Algorithm for a Restorative, Surgical, or Combination (RSC) Approach
1. Management of Etiology
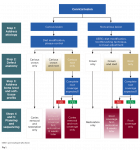
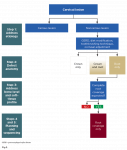
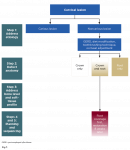
The first step in sequencing in the RSC algorithm is to manage the etiology (Figure 1). This can be done through medical consultation, diet modification, oral hygiene instruction, modification of toothbrushing technique, and occlusal adjustment as needed. Once a plan for management of etiologic agents has been discussed, replacement of hard and soft tissues may be attempted.
2. Identification of the Defect Anatomy
The next step involves identifying the extent of the lesion (Figure 1). This can be done by locating the cementoenamel junction (CEJ) of the tooth. In cases where the CEJ is not clinically discernable, an estimation based on knowledge of anatomic measurements of teeth may be used. Once the CEJ is identified, the lesion is categorized into "crown only," "root only," and "combination defect." The crown-only cervical lesion is limited to anatomic crowns, involves enamel and/or coronal dentin of the tooth, and is located coronal to the CEJ. The root-only cervical lesion involves cementum and/or radicular dentin and is located apical to the CEJ. The combination defect extends across the CEJ involving both the crown and exposed root and affecting enamel, cementum, and/or dentin. For carious teeth, the anticipated defect dimension after caries removal must be used to classify the sites as crown-only, root-only, or combination.
3. Assessment of Bone Level and Soft-Tissue Profile
In this step an evaluation is made of the clinical examination of the soft tissue, radiographic bone level, and prediction of the amount of root coverage expected (Figure 1). The soft-tissue evaluation includes assessment of gingival phenotype, amount of keratinized tissue width, and depth of vestibule. Sites with thick phenotype and more that 2 mm of keratinized tissue width have shown to have better health indicators, esthetics, and patient comfort.26 Conversely, for sites with thin phenotype and inadequate keratinized tissue width, phenotype enhancement through soft-tissue grafting may be considered to improve periodontal stability, especially in cases of restorations.26 Thus soft-tissue evaluation is important to determine if grafting is necessary. For prediction of root coverage, absence of interdental bone loss with complete papillae fill is a good indicator for obtaining complete root coverage in root-only cervical defects.27-29 Conversely, if there is interdental bone and papillae loss, the predictability for complete root coverage is reduced.27-29 Thus, identifying the interdental bone level and papillae fill is important in estimating the level of root coverage to be gained with a CTG.
4. Treatment Plan Selection
Once the assessment of the extent of the cervical lesion and evaluation of soft-tissue anatomy and predictability of root coverage is complete, a suitable treatment plan is selected (Figure 1). Crown-only cervical lesions that involve enamel and/or coronal dentin may be treated with restorative therapy only. A soft-tissue graft may be indicated at such sites first, if the site has a thin phenotype, inadequate keratinized tissue width, and shallow vestibule to achieve a more predictable outcome in the long-term. For lesions limited to the root surface (cementum and/or root dentin), which are commonly associated with gingival recession, only mucogingival surgical procedures may be indicated, provided there is no loss of interdental bone and predictability for complete root coverage is high. However, in cases where there is loss of interdental bone, complete root coverage is not possible.27-29 Such defects are treated as a combined crown and root defect and would need restorative and surgical treatment. When the cervical lesions include both crown and root there is loss of enamel, cementum, and/or dentin. The ideal treatment of such a lesion should involve a combined restorative and surgical approach.
5. Sequencing of Combined Restorative and Surgical Treatment
For lesions needing both restorative and surgical correction, a surgical approach should be attempted first, and the restoration may be completed after complete healing has occurred (Figure 1). The objective of the surgery is to position the gingival margin as close to the CEJ as possible. There has been some debate about whether restorative procedures should be done before surgical procedures for NCCLs.4 However, surgical outcomes are dependent on multiple factors and more difficult to predict than restorative outcomes. By performing surgery first, the final result becomes more predictable because the restoration can be adjusted to treat the coronal portion of the lesion and parts of the radicular portion that did not achieve coverage. If the restoration is attempted first and the surgical outcome does not achieve the desired root coverage, the restoration might have to be redone. Further, the use of a CTG increases the soft-tissue thickness and the zone of keratinized tissue. Such a thick gingival phenotype is more favorable to resist inadvertent trauma potentially caused by placement of rubber dam clamps, use of high-speed burs along the margins during tooth preparation and polishing of the restoration, and packing retraction cords during restorative treatment. Conversely, restorative therapy before mucogingival surgery may offer advantages such as better access and visibility and greater control over the emergence profile,4 but the risks outweigh the benefits.
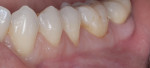
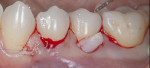
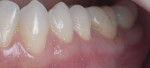
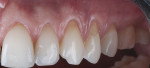
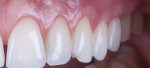
The RSC algorithm used in the management of two different cases of cervical lesions is depicted in Figure 2 through Figure 8.
Conclusion
A thorough medical and dental history and clinical examination are necessary to identify the etiology of dental cervical lesions. Furthermore, assessment of the extent of the lesion (enamel, cement, and/or dentin) and soft-tissue anatomy play an integral role in determining the treatment plan for such lesions. Additionally, a combined cervical lesion involving both the coronal and radicular portions can be best addressed with a combination therapy of connective tissue graft first, followed by a restoration. Thus, the RSC approach provides a useful tool in management of both carious and noncarious cervical lesions.
ABOUT THE AUTHOR
Neel B. Bhatavadekar, BDS, MS, MPH
Adjunct Faculty, University of North Carolina at Chapel Hill, North Carolina; Private Practice, Clarus Dental Specialties, Pune, India; Diplomate, American Board of Periodontology
Amit S. Gharpure, BDS, MSD
Affiliate Instructor, Periodontics, University of Washington School of Dentistry, Seattle, Washington; Diplomate, American Board of Periodontology; Fellow, Royal College of Dentists©
Ricardo Kern,BDS, DClinDent, MSc
Private Practice, Curitiba, Brazil
REFERENCES
1. Shay K. The evolving impact of aging America on dental practice. J Contemp Dent Pract. 2004;5(4):101-110.
2. Grippo JO, Simring M, Schreiner S. Attrition, abrasion, corrosion and abfraction revisited: a new perspective on tooth surface lesions. J Am Dent Assoc. 2004;135(8):1109-1118.
3. Steele JG, Sheiham A, Marcenes W, et al. Clinical and behavioural risk indicators for root caries in older people. Gerodontology. 2001;18(2):95-101.
4. Zucchelli G, Gori G, Mele M, et al. Non-carious cervical lesions associated with gingival recessions: a decision-making process. J Periodontol. 2011;82(12):1713-1724.
5. Femiano F, Grassia V, Femiano R, et al. Decision-making process as guide to the management of non-carious cervical lesions with and without painful symptomatology. J Biol Regul Homeost Agents. 2019;33(4):1013-1018.
6. Lussi A, Hellwig E, Ganss C, Jaeggi T. Buonocore memorial lecture: Dental erosion. Oper Dent. 2009;34(3):251-262.
7. Dzakovich JJ, Oslak RR. In vitro reproduction of noncarious cervical lesions. J Prosthet Dent. 2008;100(1):1-10.
8. Bartlett DW, Shah P. A critical review of non-carious cervical (wear) lesions and the role of abfraction, erosion, and abrasion. J Dent Res. 2006;85(4):306-312.
9. Michael JA, Townsend GC, Greenwood LF, Kaidonis JA. Abfraction: separating fact from fiction. Aust Dent J. 2009;54(1):2-8.
10. Hayes M, Brady P, Burke FM, Allen PF. Failure rates of class V restorations in the management of root caries in adults - a systematic review. Gerodontology. 2016;33(3):299-307.
11. Chambrone L, Ortega MAS, Sukekava F, et al. Root coverage procedures for treating single and multiple recession-type defects: an updated Cochrane systematic review. J Periodontol. 2019;90(12):1399-1422.
12. Langer B, Langer L. Subepithelial connective tissue graft technique for root coverage. J Periodontol. 1985;56(12):715-720.
13. Allen AL. Use of the supraperiosteal envelope in soft tissue grafting for root coverage. I. Rationale and technique. Int J Periodontics Restorative Dent. 1994;14(3):216-227.
14. Zucchelli G, Mele M, Mazzotti C, et al. Coronally advanced flap with and without vertical releasing incisions for the treatment of multiple gingival recessions: a comparative controlled randomized clinical trial. J Periodontol. 2009;80(7):1083-1094.
15. Bhatavadekar NB, Gharpure AS, Chambrone L. Long-term outcomes of coronally advanced tunnel flap (CATF) and the envelope flap (mCAF) plus subepithelial connective tissue graft (SCTG) in the treatment of multiple recession-type defects: a 6-year retrospective analysis. Int J Periodontics Restorative Dent. 2019;39(5):623-630.
16. Bhatavadekar NB, Gharpure AS. Controlled palatal harvest technique for harvesting a palatal subepithelial connective tissue graft. Compend Contin Educ Dent. 2018;39(2):e9-e12.
17. Chambrone L, Pini Prato GP. Clinical insights about the evolution of root coverage procedures: the flap, the graft, and the surgery. J Periodontol. 2019;90(1):9-15.
18. Pini Prato GP, Franceschi D, Cortellini P, Chambrone L. Long-term evaluation (20 years) of the outcomes of subepithelial connective tissue graft plus coronally advanced flap in the treatment of maxillary single recession-type defects. J Periodontol. 2018;89(11):1290-1299.
19. Santamaria MP, Ambrosano GM, Casati MZ, et al. Connective tissue graft plus resin-modified glass ionomer restoration for the treatment of gingival recession associated with non-carious cervical lesion: a randomized-controlled clinical trial. J Clin Periodontol. 2009;36(9):791-798.
20. Mele M, Zucchelli G, Montevecchi M, Checchi L. Bilaminar technique in the treatment of a deep cervical abrasion defect. Int J Periodontics Restorative Dent. 2008;28(1):63-71.
21. Tay FR, Pashley DH. Resin bonding to cervical sclerotic dentin: a review. J Dent. 2004;32(3):173-196.
22. Lee WC, Eakle WS. Stress-induced cervical lesions: review of advances in the past 10 years. J Prosthet Dent. 1996;75(5):487-494.
23. Schätzle M, Land NP, Anerud A, et al. The influence of margins of restorations of the periodontal tissues over 26 years. J Clin Periodontol. 2001;28(1):57-64.
24. Cairo F, Cortellini P, Nieri M, et al. Coronally advanced flap and composite restoration of the enamel with or without connective tissue graft for the treatment of single maxillary gingival recession with non-carious cervical lesion. A randomized controlled clinical trial. J Clin Periodontol. 2020;47(3):362-371.
25. Santamaria MP, Silveira CA, Mathias IF, et al. Treatment of single maxillary gingival recession associated with non-carious cervical lesion: randomized clinical trial comparing connective tissue graft alone to graft plus partial restoration. J Clin Periodontol. 2018;45(8):968-976.
26. Kao RT, Curtis DA, Kim DM, et al. American Academy of Periodontology best evidence consensus statement on modifying periodontal phenotype in preparation for orthodontic and restorative treatment. J Periodontol. 2020;91(3):289-298.
27. Miller PD Jr. A classification of marginal tissue recession. Int J Periodontics Restorative Dent. 1985;5(2):8-13.
28. Zucchelli G, Testori T, De Sanctis M. Clinical and anatomical factors limiting treatment outcomes of gingival recession: a new method to predetermine the line of root coverage. J Periodontol. 2006;77(4):714-721.
29. Cairo F, Nieri M, Cincinelli S, et al. The interproximal clinical attachment level to classify gingival recessions and predict root coverage outcomes: an explorative and reliability study. J Clin Periodontol. 2011;38(7):661-666.