Comprehensive, Phased Restoration of Worn Dentition Utilizing Digital Analysis and Diagnostic Protocols
Christine Hansen, DDS
Abstract: In this case of a comprehensive dental restoration, a predictable course of treatment is demonstrated in which dental risk was stabilized and definitive treatment was provided in a phased approach to accommodate financial limitations of the patient. Utilizing digital photographic analysis, facial reference glasses, and intraoral scanning, the clinician implemented a treatment plan that was aimed at minimizing and managing the patient's biomechanical and functional risks and resolving his concerns about past failing dental work and an unattractive smile. The phased rehabilitation plan included opening of the vertical dimension of occlusion to accommodate restorative space, appropriate incisal edge position, and function.
Comprehensive dental rehabilitation is a complex undertaking that can be challenging for both the clinician and the patient. For the clinician, planning and executing treatment requires systematic data collection and predictable, evidence-based methods for managing care and future oral health risk factors. For the patient, emotional and financial hurdles often must be overcome.
This case exhibits a predictable course of treatment for a patient with emotional and financial challenges that both satisfied the desires of the patient and addressed the issues that the clinician deemed essential. Digital photographic analysis was employed using facial reference glasses (Kois Facial Reference Glasses, Kois Center, koiscenter.com) and scans of the patient's dentition. A phased treatment plan was utilized to stabilize dental risk and provide definitive treatment over several years, allowing care to be more affordable for the patient.
Clinical Case Overview
Patient History and Chief Concerns
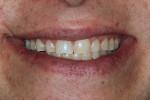
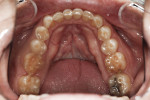
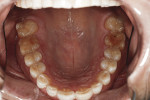
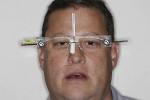
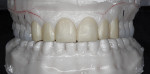
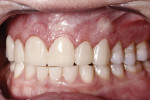
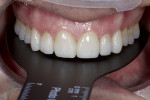
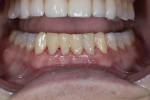
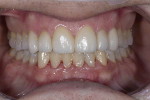
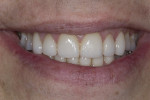
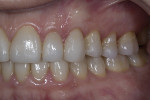
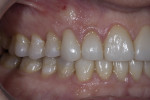
A 47-year-old man presented in November 2018 with chief concerns of worn, chipped teeth and failing composite restorations (Figure 1 through Figure 3). He expressed frustration and anxiety over previous restorations that had continued to chip and required multiple repairs. He was despondent and apprehensive about how to move forward with a successful, affordable plan of treatment that would allow him to smile with confidence. The patient, who is a public school teacher, expressed concern about limited finances, so a phased treatment plan would be used to provide definitive treatment over several years, making care more affordable.
Medical History
The patient reported a history of obstructive sleep apnea, gastroesophageal reflux disease (GERD), and generalized anxiety disorder. He had been using continuous positive airway pressure (CPAP) successfully, and as a result his GERD improved. His anxiety was managed with Prozac (fluoxetine), a selective serotonin reuptake inhibitor (SSRI) medication, which is known to increase the potential for parafunctional habits as well as xerostomia1 and can increase caries and dental corrosion risk.
Dental History
The patient rated his fear of dental treatment as 5 of 10 on the visual analog scale and expressed great frustration that previous dentistry had failed, including broken fillings, areas of sensitivity, and teeth that were too short. He considered his prior dental experiences to be unsuccessful and the dentist judgmental, which further diminished his motivation and confidence. Dental examination revealed many areas of erosion, attrition, and fractured enamel that contributed to his failing dental health.
Diagnosis, Risk Assessment, and Prognosis
Periodontal: The periodontal assessment revealed generalized horizontal attachment loss of approximately 2 mm in both the maxillary and mandibular arches with no probing depths exceeding 4 mm. Localized mild gingivitis was present at teeth Nos. 3 through 7 with bleeding on probing. Both of the patient's biological parents had periodontal disease, he reported. The periodontal diagnosis was American Academy of Periodontology (AAP) stage II, grade B.
Risk: Low
Prognosis: Good
Biomechanical:No active caries was present; however, examination revealed significant generalized erosion and attrition. Severe erosion with attrition greater than 2 mm on teeth Nos. 13, 14, 19, 28, and 30 was noted. Moderate erosion with attrition of 1 mm to 2 mm was noted on all other teeth.
Risk: High
Prognosis: Poor
Functional:The patient had a normal range of motion with maximum opening of 55 mm. No joint noises or muscle tenderness were noted, and immobilization and loading tests were normal. Attrition was present on every tooth. There was no history of neurologic disorders; however, the patient reported grinding his teeth at night and had been wearing a nightguard. At the time of his first visit, he was wearing an over-the-counter soft nightguard during sleep. His history of taking SSRI medications for his anxiety disorder may have been contributory to his parafunctional habits.2,3 The deprogrammed bite showed his first point of posterior contact at tooth No. 3, which helped confirm a combined diagnosis of occlusal dysfunction with some contributory level of parafunction.
Risk: Moderate
Prognosis: Poor to hopeless
Dentofacial:The patient deemed his teeth to be too short when he smiled. Average adult male maxillary central incisor tooth length is around 10 mm.4 Measurements revealed deficient central incisor facial length of 8.6 mm. Evaluating his smile in repose, the right canine was hidden by his lip by 2 mm. The canines may be successfully referenced in this way to determine a desirable show of dentition in repose and while smiling.5 Lip mobility was in the normal range of 6 mm to 10 mm at the right central incisor. When smiling fully (Duchenne smile) the patient showed gingival contours readily on most of his maxillary anterior teeth.
Risk: High
Prognosis: Poor
Treatment Plan
The intention of the treatment plan was to minimize and manage the patient's biomechanical and functional risks and resolve his concerns with regard to failing dentistry and an unsightly smile. He was presented with a comprehensive, phased rehabilitation plan that included opening of the vertical dimension of occlusion to accommodate restorative space, appropriate incisal edge position, and function.
Phase 1: Digital Records and Analysis
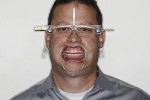
The clinician utilized digital planning in the diagnostic portion of the case and collected photographs with the patient wearing facial reference glasses for digital facebow mounting and fabrication of a milled Kois deprogrammer (Kois Center) (Figure 4 through Figure 7). An intraoral scanner (iTero®Element, Align Technology, Inc, itero.com) was utilized for imaging the maxillary and mandibular arches. All records were then sent to the laboratory, which milled a Kois deprogrammer to assist with occlusal diagnosis.
The Kois deprogrammer was delivered, and the patient wore it for 6 weeks. After deprogramming, the patient was able to produce a repeatable reference position on the deprogrammer platform. Occlusal centric relation records were taken with vinyl polysiloxane material (Take 1™ Advanced™, Kerr, kerrdental.com).
The incisal edge position of the maxillary anterior teeth was determined using the visual position of the maxillary canine in repose.5 From the repose photograph with facial reference glasses (Figure 7), which showed the maxillary canine at -2 mm from the lip in repose, it was determined that the addition of 2 mm to the incisal edge of tooth No. 6 would provide an appropriate reference tooth for an esthetic smile. Using the digital facebow model mounted on the articulator (Panadent, panadent.com), the platform was then dropped 2 mm to complete the diagnostic wax-up of maxillary teeth Nos. 3 through 14 (Figure 8).
Next, the mandibular incisal position was determined by utilizing the facial reference glasses photographs, lip dynamics, and average tooth length range data. The decision was made to add 2 mm to the incisal edges of the mandibular teeth (Nos. 22 through 27).
Phase 2: Restoration of the Maxillary Arch
After the Kois deprogrammer was used to find a repeatable position and esthetics were verified, the maxillary arch was restored. Laboratory-processed composite onlays (Radica®, Dentsply Sirona, dentsplysirona.com) were cemented onto teeth Nos. 3 through 5 and 12 through 14 after air-abrasion, selective-etch, and bond techniques were performed, with a composite (Kerr SonicFill™ 3, Kerr) used as the luting agent. Sealing the severely eroded and worn posterior teeth with strong transitional restorations would mitigate the long-term biocorrosion (erosion and attrition) of tooth structure and improve the biomechanical prognosis.6,7 After cementation of the composite onlays, the posterior occlusion was equilibrated using the Kois deprogrammer. Adjustments were made on the mandibular teeth to preserve the idealized maxillary posterior teeth. The clinician was then able to move forward with definitive treatment of the anterior teeth.
Teeth Nos. 6 through 11 were prepared as follows: approximately 0.3 mm reduction in the gingival region, a smooth transition to 0.6 mm in the mid-facial area, and 2 mm incisal reduction. These teeth were then temporized with a provisional material (Luxatemp®, DMG America, dmg-america.com) and tack-bonded in place (Figure 9). After digital scanning and laboratory fabrication of the anterior veneers (IPS e.max®, Ivoclar Vivadent, ivoclarvivadent.com) the patient returned for cementation of the veneers with a translucent cement (Calibra™, Dentsply Sirona) (Figure 10). The maxillary posterior composite onlays were then separated and polished.
After the Kois deprogrammer was used to equilibrate the maxillary teeth, the deprogrammer platform required rebuilding. This was completed chairside by adding composite to the platform, then occlusal records were taken and the mandibular dentition was scanned for fabrication of the mandibular arch posterior teeth composite onlays. The patient continued using the Kois deprogrammer except during chewing until the following week when the mandibular arch was treated.
Phase 3: Restoration of the Mandibular Arch
Cementation of laboratory-processed composite onlays (Radica) on teeth Nos. 19 through 21 and 28 through 30 was completed using air-abrasion, selective-etch, and bond techniques and SonicFill 3 composite. The occlusal equilibration of the mandibular indirect composite onlays was completed utilizing the retrofitted Kois deprogrammer. Anterior teeth Nos. 22 through 27 were then prepared using appropriate reduction guidelines for adhesive restorations. The preparations of the lower anteriors and the mandibular arch were scanned and sent to the laboratory. Teeth Nos. 22 through 27 were temporized with Luxatemp and tack-bonded in place (Figure 11 and Figure 12).
Three weeks later the e.max veneers were cemented with translucent cement (Calibra). The mandibular posterior composite onlays were then separated and polished.
Final photographs of the comprehensive restoration are shown in Figure 13 through Figure 16. The treatment was completed in March 2020.
Because of the patient's positive history of reported sleep bruxism and expected ongoing use of SSRI medications for anxiety, the clinician chose to finalize the case with a laboratory-fabricated acrylic occlusal guard to protect the newly restored teeth from any parafunctional stresses during sleep. Digital records were taken with the scanner (iTero Element) for fabrication of the occlusal guard.
Conclusion
The clinician was able to achieve stable functional occlusion and improved esthetics while decreasing functional and biomechanical risk factors. The patient, who was very pleased with the results, continues as an active patient in the practice and is seen for routine recare visits. The long-term plan is to transition the posterior teeth to lithium-disilicate (e.max) restorations over the next several years.
Using Kois protocols and devices for obtaining records, analysis, and risk assessment simplified a complex case and helped ensure what is expected to be a long-lasting outcome. The use of a Kois deprogrammer was beneficial for determining a repeatable reference position for centric relation and simplified the management of occlusion when seating multiple restorations. Implementation of a phased treatment plan allows a worn dentition to be restored in a manner that can accommodate financial concerns and may lead to increased treatment acceptance.
Acknowledgment
The author thanks Claudio Bucceri, CDT, of Swiss Dental; Matt Falkenstein, DDS; and Susan Sheets, DDS.
About the Author
Christine Hansen, DDS
Mentor, Kois Center, Seattle, Washington; Diplomate, American Academy of Dental Sleep Medicine; Private Practice, Palo Alto, California
References
1. Ferguson JM. SSRI antidepressant medications: adverse effects and tolerability. Prim Care Companion J Clin Psychiatry. 2001;3(1):22-27.
2. Garrett AR, Hawley JS. SSRI-associated bruxism: a systematic review of published case reports. Neurol Clin Pract. 2018;8(2):135-141.
3. Milanlioglu A. Paroxetine-induced severe sleep bruxism successfully treated with buspirone. Clinics (Sao Paulo). 2012;67(2):191-192.
4. Sterrett JD, Oliver T, Robinson F, et al. Width/length ratios of normal clinical crowns of maxillary anterior dentition in man. J Clin Periodontol. 1999;26(3):153-157.
5. Misch CE. Guidelines for maxillary incisal edge position-a pilot study: the key is the canine. J Prosthodont. 2008;17(2):130-134.
6. Heying JJ. Flexural Strength of Interim Fixed Prosthesis Materials After Simulated Function [master's thesis]. Iowa City, IA: University of Iowa;2009. http://ir.uiowa.edu/etd/377. Accessed July 9, 2021.
7. Oliva GS. Mechanical Properties of Provisional Restorative Materials[master's thesis]. Indianapolis, IN: Indiana University School of Dentistry; 2010. http://hdl.handle.net/1805/2320. Accessed July 9, 2021.