The Future of Dentistry
Christopher M. Balaban, DMD, MSc; Wardah Inam, PhD, SM; Ryan Kennedy, MBA, MMP; Robert A. Faiella, DMD, MMSc
This year Compendium will be publishing a six-part series focused on how artificial intelligence (AI) is transforming the dental industry. This series will touch on all aspects of dentistry and bring together insights from experts in private practice, dental service organizations, insurance, academia, public health, and distribution under the auspices of Overjet, a leading provider of AI in dentistry. Through this collection of informative and engaging articles, readers will learn where AI is having an impact today and how it will define the future of dentistry.
Artificial intelligence is already transforming transportation, advertising, e-commerce, finance, media, and healthcare. We interact with AI every day, whether through a television show recommendation by Netflix, photo tagging by Facebook, a predictive search by Google, voice recognition by Amazon, or tracking of health vitals by Apple Watch. In dentistry, new innovations in AI and deep learning are rapidly emerging to augment the capabilities of dental professionals and improve dental care for patients.
A subfield of AI, deep learning takes its inspiration from the human brain. Similar to how the brain has billions of neurons that learn and are connected together in networks to give us our cognitive abilities, deep learning models have millions of connected nodes (called neural networks), which learn from examples to give machine intelligence. By learning from millions of data points, the models produce accurate and repeatable outputs. For example, by analyzing a large sample of x-rays, the computer model learns what a tooth looks like and can predict teeth numbers with clinician-level accuracy on novel images. Additionally, machine learning models for bone levels measured from the cementoenamel junction to the crest of bone offer extreme accuracy.
In this month's edition (see adjacent page), the series will cover how AI is transforming dental practices and how it can be used to improve patient quality of care and experience. In future months, the series will review the role of AI in the following topics:
• AI-driven growth of dental practices
• AI enhancing the payer-provider relationship
• Virtual dental care powered by AI: making dental appointments more accessible and convenient
• AI enabling medical-dental integration for better overall health
• Beyond digital dentistry: AI transforming the digital workflows
Artificial intelligence builds upon the digital tools dentistry has already adopted. It has the potential to revolutionize patient care while assisting practitioners in improving oral health.
AI Transforming Dental Practices: Enhancing Quality of Care and the Patient Experience
Dentists have adopted numerous technologies to help their patients maintain and improve oral health throughout their lifetimes. Digital tools such as practice management software, digital radiographs, and oral photographs are commonplace in practices. These tools aid dentists in applying scientific principles, clinical acumen, and technical expertise to prevent, diagnose, and care for patients with oral disease or injury. The result of such digitization is an abundance of data that can be analyzed using artificial intelligence (AI) throughout the patient care journey.
In this journey, the dentist reviews data to stratify patient risk and consider potential diagnoses. These steps are followed by communicating diagnostic data, discussing treatment options, and then receiving acceptance from the patient. A treatment plan may be initiated, and then finally, the dentist monitors the longitudinal outcome of treatment.1
AI builds upon the digital tools the dental profession has already adopted. It promises to transform the patient journey outlined above and support the quest of the dental community to improve oral health. In this review, we will detail how AI is used today in the clinic to improve patient care and experience. Discussion will include the diagnostic capabilities of AI, how AI can be used to support treatment planning and patient communication, and the benefits of AI quantification.
Supporting Diagnosis with AI
Dentists analyze a significant amount of data in a short period of time to diagnose disease and create a personalized treatment plan for each patient. Deployed effectively, AI can support the practitioner to improve diagnostic quality, consistency, and speed.2 To see how, it is helpful to review a variety of capabilities of dental AI today.
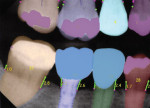
In radiographs, computer vision models can replicate the intuitive pattern recognition performed by dentists reviewing a radiograph for dental anatomy, past treatments, and dental pathology.3 For example, in dental anatomy, models can identify tooth numbers,4 enamel, bone level, pulp, cementoenamel junction (CEJ), and dentinoenamel junction (DEJ) (Figure 1). For past treatments, models can detect and outline crowns, implants, and endodontic obturations. And for dental pathologies, models accurately identify primary and secondary caries and periapical radiolucencies.5 The output of dental AI analysis is thorough and consistent and can be stored in digital notation, readable by humans and other software algorithms alike. This data can then be used to auto-populate a hard-tissue chart with the diagnostic codes and treatment plan, freeing up time for office personnel, reducing the chance for missed findings, and maintaining consistent documentation.
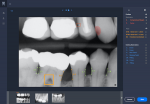
Beyond radiographs, AI can also be useful in gathering data from disparate software systems and various forms of media. For example, natural language processing models can review patient data in the electronic medical or dental records to identify risk factors such as severity of diabetes, frequency of smoking, brushing habits, and current medications.6,7 From the practice management software, probing depths from periodontal charts and past treatments can be accessed. After data is automatically gathered from across practice systems, algorithms can surface the most relevant information for review by the clinician, saving time and supporting quality decision making (Figure 2).
Along with gathering relevant information, AI can automatically evaluate data against quantified and clinically relevant standards for confirmation by clinicians. For instance, radiographic bone levels for specific teeth in excess of 3 mm from CEJ to crest of bone and the presence of root surface calculus can support a diagnosis of periodontitis.8 These results are generated in real-time as data is captured by diagnostic tools and globally for all patients in the practice to raise the level of clinical cognition. Additionally, AI algorithms can incorporate comorbidities and self-reported patient risk indicators to stratify patients with a specific diagnosis into high-, intermediate-, and low-risk groups for dental disease development.9 This stratification can inform the aggressiveness of treatment and should prove to be a powerful predictor of treatment success. Clinicians have an opportunity for meaningful time savings with individual patients and actionable clinical trends that can inform training and discussion with office staff.
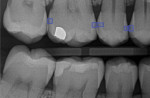
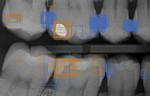
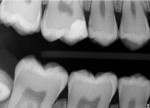
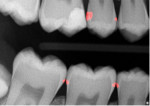
AI is also likely to emerge as a powerful training partner for dentists to support quality. In one academic study, dentists were shown to have an inter-observer agreement of only 58% when reviewing the same intraoral radiographs for measuring marginal bone height.10 In typical clinical routines, dentists may not realize other dentists would look at the same radiograph or diagnostic information differently than them (Figure 3). Also, on a busy day, a less noticeable finding could be overlooked. In this way, AI can serve as a complementary feedback tool for both new and even experienced dentists. For example, a caries detection model could be run with every radiograph (Figure 4). Today, the best chess players in the world train against AI chess models.11 They do so not to replace themselves as chess players but to reach new levels of excellence in play. Dentists now have this same opportunity. As dental AI for diagnostic support becomes more prolific, the industry may follow patterns seen in other healthcare fields where the combination of experienced practitioners and AI together produce the best measured results compared to either alone.12
AI models are trained using input from dentists and have seen millions of data points to identify clinical findings with high sensitivity and specificity. However, just as feedback for practitioners is important, so too is feedback for AI models. In-clinic AI software can allow feedback and detection adjustments by practitioners to train future AI models so that the next iteration of a model can predict accurately and robustly across varied inputs. Dentists can then utilize the recommendation of these AI models and their clinical judgment to provide the final diagnosis.
Improving Patient Treatment Workflow
Today, AI models also inform the workflow of the practice to support office efficiency and patient experience. Before patients arrive, AI flags those whose clinical records lack critical baseline data or have untreated disease. During a dental consultation, AI models prioritize the most relevant annotated radiographs and predicted clinical findings. For the first time, dentists can have real-time, quantitative estimates of disease progression; for instance, the relation and percentage of caries toward or through the DEJ over time. This detail can be used to inform treatment versus maintenance and set practice protocols, informed by clinical research. On the administrative side, AI models inform office personnel where notes and data in the patient file are inconsistent with coding; an example of this might be when a full-mouth x-ray was acquired for the patient file, but insurance was only billed for a bitewing radiograph.
All of this workflow, however, ultimately culminates in a decision point by the patient to accept treatment. Here too, AI can be of service.
Improving Case Acceptance through AI Visualization
Case acceptance has traditionally been based on the trust relationship between the patient and provider.13,14 With AI, the ability for patients to visualize, recognize, and understand objective indications for treatment-with interpretation by the clinician-allows patients more control in making the right decision for their conditions. Instead of saying, "you have bone loss here," the practitioner can explain, "near this orange line, you have probing depths in excess of 4mm and radiographic bone levels of 4.3mm and evidence supports treatment once levels progress beyond 3 mm" (Figure 2). The precision and computer visualization support the clinical judgment of the dentist, and intuitive color coding draws the attention of the patient to the most relevant points of concern.
Longitudinal Tracking of Treatment Outcomes
Even with the best explanation by the practitioner and support from AI visualizations, the patient may still choose to defer treatment. In this case, quantified, longitudinal tracking becomes important to identify and monitor disease progression.15 Dentists will no longer need to rely only on their own visual assessment of progression. AI can provide quantitative measures such as millimeters of bone loss over time and percentage of caries progression toward the DEJ, along with visualizations of the progression. These data points support the call to escalate the urgency of care and provide an appropriate record of patient compliance. The ability to quantify the extent of caries and its progression or stability over time will give greater confidence to the clinician regarding the recommended treatment approach.
Once treatment occurs, the opportunity exists for longitudinal quality tracking for individual patients and by practitioner outcomes. Measurements can be taken over time to help the dentist monitor marginal integrity of both crowns and restorations, outcomes of bone regeneration procedures, or bone loss adjacent to an implant (Figure 5).
In addition to providing care, dentists assume responsibility for the management of the practice, including oversight of quality control among the providers to maintain standards of care and regulatory compliance.16 AI models configured to practice goals and clinical best practices can continuously monitor patient data over time to highlight opportunities for improvements such as potentially missed treatments, incorrect documentation, disrupted treatment workflow, and compliance with office protocols.
The Rising Era of AI in Dental Care Delivery
The digitization of the dental practice and advances in machine learning have combined to unlock practical uses of AI to improve the patient experience and care today. The profession has new AI tools to support diagnosis, treatment planning, patient acceptance, longitudinal tracking, and administration. Deployed well, AI tools hold the promise to improve quality, speed, and trust across the patient care journey.
Regardless of the advances in dental AI technology, adoption will still be key for patients to experience the benefits. What may quicken the pace of dental AI adoption is that the technology does not require new hardware, significant financial investment, or extensive training. The best AI technology installs seamlessly as software, uses existing data generated by the practice, and presents findings in an intuitive and actionable manner.
The ultimate utility of AI to the profession is still tied to the larger dental ecosystem, including dental support organizations, payers, academia, and dental vendors. Upcoming articles in this series will examine current and future uses of AI in different dental contexts. The technology is likely to impact the relationship between providers and payers, expand approaches to clinical research, and unlock new business models. Anchoring this change is the fundamental mission of dentists to prevent, diagnose, and care for patients. Dental artificial intelligence now shares this mission as well.
References
1. Douglass GD. Making a comprehensive diagnosis in a comprehensive care curriculum. J Dent Educ. 2002;66(3):414-420.
2. Murdoch TB, Detsky AS. The inevitable application of big data to health care. JAMA. 2013;309(13):1351-1352.
3. Tandon D, Rajawat J. Present and future of artificial intelligence in dentistry. J Oral Biol Craniofac Res. 2020;10(4):391-396.
4. Chen H, Zhang K, Lyu P, et al. A deep learning approach to automatic teeth detection and numbering based on object detection in dental periapical films. Sci Rep. 2019;9(1):3840.
5. Pretty IA, Maupomé G. A closer look at diagnosis in clinical dental practice: Part 3. Effectiveness of radiographic diagnostic procedures. J Can Dent Assoc. 2004;70(6):388-394.
6. D'Avolio LW, Nguyen TM, Goryachev S, Fiore LD. Automated concept-level information extraction to reduce the need for custom software and rules development. J Am Med Inform Assoc. 2011;18(5):607-613.
7. Zeng Z, Deng Y, Li X, et al. Natural language processing for EHR-based computational phenotyping. IEEE/ACM Trans Comput Biol Bioinform. 2019;16(1):139-153.
8. Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontol. 1961;32(3):261-267.
9. Giannobile WV, Braun TM, Caplis AK, et al. Patient stratification for preventive care in dentistry. J Dent Res. 2013;92(8):694-701.
10. Molander B, Ahlqwist M, Gröndahl HG, Hollender L. Agreement between panoramic and intraoral radiography in the assessment of marginal bone height. Dentomaxillofac Radiol. 1991;20(3):155-160.
11. Siegel R. 20 years later, humans still no match for computers on the chessboard. National Public Radio website. October 24, 2016. https://www.npr.org/sections/alltechconsidered/2016/10/24/499162905/20-years-later-humans-still-no-match-for-computers-on-the-chessboard. Accessed December 7, 2020.
12. Patel BN, Rosenberg L, Willcox G, et al. Human-machine partnership with artificial intelligence for chest radiograph diagnosis. NPJ Digit Med. 2019;2:111. doi: 10.1038/s41746-019-0189-7.
13. Brookes-Howell L, Wood F, Verheij T, et al. Trust, openness and continuity of care influence acceptance of antibiotics for children with respiratory tract infections: a four country qualitative study. Fam Pract. 2014;31(1):102-110.
14. Dyer TA, Owens J, Robinson PG. The acceptability of care delegation in skill-mix: the salience of trust. Health Policy. 2014;117(2):170-178.
15. Layton DM, Clarke M. Quality of reporting of dental survival analyses. J Oral Rehabil. 2014;41(12):928-940.
16. Nadaud MJ. Key performance indicators for dental practices: management by statistics. Dental Economics website. March 1, 2019. https://www.dentaleconomics.com/practice/article/16386298/key-performance-indicators-for-dental-practices-management-by-statistics. Accessed December 7, 2020.
About the Authors
Christopher M. Balaban, DMD, MSc
Clinical Director, Overjet, Inc.; Clinical Faculty, Boston University Goldman School of Dental Medicine, Boston, Massachusetts; Private Practice, Boston, Massachusetts
Wardah Inam, PhD, SM
Chief Executive Officer,
Overjet, Inc.
Ryan Kennedy, MBA, MPP
Chief of Staff,
Overjet, Inc.
Robert A. Faiella, DMD, MMSc, MBA
Chief Dental Officer, Overjet, Inc.; Diplomate, American Board of Periodontology; Private Practice,
Osterville, MA