Repair of Lingual Gingival Fenestrations Through the Use of a Subepithelial Connective Tissue Graft
Joshua Shayefar, DMD; Elena Sanz-Miralles, DDS, MSc, MS, PhD; Robert N. Eskow, DMD, MScD; and Gary Greenstein, DDS, MS
Abstract: A gingival fenestration is a localized perforation of keratinized gingival tissue that may result in underlying bone resorption and root exposure. This case report describes treatment of mandibular lingual gingival fenestrations caused by traumatic forces from an ill-fitting removable partial denture that rested on a thin periodontal phenotype. A subepithelial connective tissue graft was used to correct these fenestrations. At the 2-year follow-up, the gingival tissues presented in a state of health.
Fenestrations and dehiscences are two commonly encountered alveolar defects. An alveolar dehiscence is defined as a lack of facial or palatal/lingual alveolar bone,1 while an alveolar fenestration is a circumscribed defect of the bony plate that does not involve the coronal alveolar bone margin.2 Gingival fenestrations are less common and are seen clinically as a localized window devoid of gingiva, and they may cause bone necrosis and eventual root exposure.3
The development of a gingival fenestration can be attributed to a variety of factors, including absence or diminished thickness of alveolar bone, malposition of teeth, non-anatomical contours of root apices, orthodontic tooth movement, nodular subgingival calculus, occlusal and traumatic forces, and endodontic pathosis.4 Gingival fenestrations are often found in maxillary or mandibular anterior regions, particularly on the facial aspect of teeth.5
This case report documents the diagnosis and treatment of lingual gingival fenestrations. The authors' hypothesis is that the gingival fenestrations were the result of trauma caused by the patient's mandibular removable partial denture (RPD). Other risk factors that may have contributed to the development of these lesions were the patient's poor plaque control, a thin periodontal phenotype, and the absence of prosthodontic aftercare. This case report is unique because of the location of the gingival fenestrations and the proposed treatment. To the authors' knowledge, this is the first report that suggests the use of a subepithelial connective tissue graft (SCTG)6 to correct lingual gingival fenestrations.
Clinical Presentation
A 79-year-old woman presented to Columbia University College of Dental Medicine in November 2016. Her chief complaint was "pain near my bottom front teeth, and my denture doesn't fit well." The patient's medical history included high blood pressure, high cholesterol, and a pacemaker that was placed in 2010. She was taking amlodipine and atorvastatin to treat the aforementioned conditions.
At the initial periodontal consultation at the Postgraduate Periodontics Clinic, the patient presented with a complete maxillary denture and a Kennedy class 1 mandibular RPD. She stated that she had worn both dentures for more than 20 years and that her dentures had never been adjusted or relined. Clinical examination revealed poor oral hygiene, with notable supra- and subgingival plaque and calculus deposits. The marginal gingiva around all teeth was highly inflamed and produced bleeding on probing (BOP).
Teeth present in the patient's mouth were unrestored teeth Nos. 22 and 27 and a fixed porcelain-fused-to-metal bridge from Nos. 23 through 26 (with pontics at sites Nos. 24 and 25). Probing depths were 6 mm at the mesio-, mid-, and distolingual locations of teeth Nos. 22 and 23, with approximately 40% interproximal bone loss. All teeth demonstrated no more than grade 1 mobility.
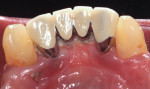
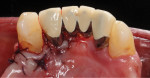
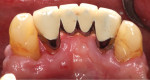
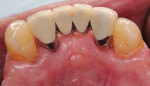
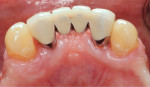
A gingival fenestration 4 mm apical to the lingual gingival margin of tooth No. 22 was present, with its apical border at the mucogingival junction (MGJ). Its dimensions were 2.5 mm x 3 mm. A second gingival fenestration was detected 2 mm apical to the lingual gingival margin of tooth No. 23; it measured 1.5 mm x 1.5 mm (Figure 1 and Figure 2). These gingival fenestrations resulted in the root surfaces of teeth Nos. 22 and 23 being exposed and covered with plaque and calculus. A diagnosis of stage III grade B periodontitis was made.7
Initial therapy consisting of scaling and root planing (SRP) with ultrasonics and hand instrumentation was completed. The patient returned in 5 weeks for a re-evaluation, at which time dramatic improvement in oral hygiene and BOP was noted. However, reductions in probing depths were minimal, the size of the gingival fenestrations remained unchanged, and there was still inflammation and sensitivity in the area.
The treatment plan at this point included the use of a SCTG with the primary objective being to eliminate the gingival fenestrations at sites Nos. 22 and 23 and increase the soft-tissue thickness of the mandibular anterior lingual surfaces. Informed patient consent was obtained and the treatment plan signed.
Therapy
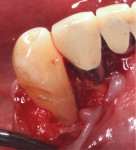
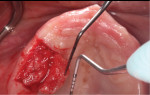
Infiltration anesthesia with two carpules of 2% lidocaine with 1:100,000 epinephrine was administered to the mandibular anterior lingual gingiva and the maxillary right alveolar ridge. A mid-crestal incision distal to tooth No. 22 and sulcular incisions from the distal of tooth No. 22 to the mesial of pontic site No. 24 were made with a 15C blade (Figure 3). A full-thickness mucoperiosteal flap was elevated on the lingual surface past the level of the MGJ (Figure 4). Plaque and calculus were removed from only the affected areas to avoid disrupting the attached connective tissue fibers and to facilitate healing by periodontal repair.8
The patient's edentulous maxillary right alveolar ridge and palate at the premolar sites was selected as the donor site. This site was chosen so as to avoid complications in relation to the neurovascular bundle of the greater palatine. A mid-crestal incision 15 mm in length was made with a 15C blade, followed by mesial and distal vertical releasing incisions. A subepithelial connective tissue graft 2 mm in thickness was harvested from the crest of the edentulous ridge and palate (Figure 5). (Note: The denture would be relined 2 weeks after surgery to ensure proper fit and comfort.)
The SCTG was then split into two pieces to treat the two separate gingival fenestrations (Figure 6). The grafts were placed individually over the exposed root surfaces at sites Nos. 22 and 23, and positioned in the center of each gingival fenestration. The SCTGs were stabilized and fixed in place using 5-0 chromic gut sutures. Then 4-0 vicryl sutures (Ethicon, ethicon.com) were used to secure the lingual flap over the grafts. Flap advancement was not performed and the grafts were left exposed in the fenestrated areas (Figure 7).
The patient was instructed to not wear her mandibular RPD until a new one was fabricated (approximately 4 months later) and to not brush the area for 2 weeks. The use of chlorhexidine 0.12% mouthrinse twice per day for 10 days was prescribed, and ibuprofen 600 mg was recommended as needed for pain. At the 2-week postoperative appointment, the recipient and donor sites both were healing satisfactorily. At the 1-month follow-up, tissues continued to heal well and remaining sutures were removed (Figure 8). Complete healing was noted 6 weeks after the surgical procedure.
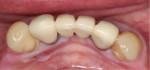
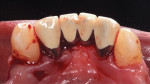
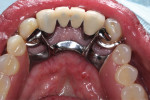
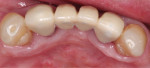
After 4 months, a new mandibular RPD was fabricated with consideration given to its prosthetic design (Figure 9). The design was aimed at aiding oral hygiene maintenance and improving stability of the prosthesis. The 1-year (Figure 10), 18-month, and 2-year (Figure 11 through Figure 13) examinations all continued to show complete repair of the gingival fenestrations, with a notable increase in the thickness of the mandibular anterior lingual gingiva. The patient reported no pain and was content with her new prosthesis. No relapse of the fenestration defects was observed.
Discussion
This case report describes the clinical management of gingival fenestrations on the mandibular anterior lingual gingiva. The most likely etiology for these fenestrations was trauma from the patient's ill-fitting RPD, which caused pressure spots on the gingiva. This probably compressed the underlying gingival tissues and blood vessels, thereby compromising the local blood supply.9 Also, Carlsson et al showed that lingual plate major connectors of RPDs have the propensity to press against the mucous membrane of lingual alveolar ridges during chronic denture use and ultimately cause gingival depressions.10 Additionally, inflammation caused by the patient's periodontal status and low level of oral hygiene may have contributed as well.
The main therapeutic objectives of the treatment were to correct the gingival fenestrations and increase the thickness of the lingual gingival tissue. To complete these objectives, initial therapy consisting of SRP was performed in an attempt to close the gingival fenestrations using nonsurgical treatment. At 5 weeks, the gingival fenestrations remained unchanged. This result was anticipated since gingival fenestrations leave roots vulnerable to plaque accumulation and calculus formation, thus making soft-tissue coverage of the exposed roots improbable.11 Therefore, a treatment plan that included the use of a SCTG was devised to correct the soft-tissue fenestrations through surgical methods.
After healing, the restorative team fabricated a new mandibular RPD with some notable differences compared to the patient's previous partial denture. The major connector of the RPD was changed from a chromium-cobalt lingual plate to a metal lingual bar. This modification was designed to help decrease plaque accumulation on the lingual surfaces and improve the patient's oral hygiene.12 The lingual bar allowed the major connector to be farther from the gingival margin, thereby reducing food impaction and marginal inflammation.13
Additionally, the cingulum rest seats on the canines were prepared 1 mm to 2 mm greater in depth than the previous denture to create a more stable prosthesis that would withstand the forces of mastication14 and further prevent future RPD settling.15 Overall, a prosthesis was fabricated that was adapted closely to the underlying soft tissues with the goal of minimizing any potential destructive forces to the periodontium.
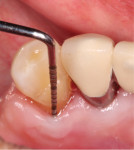
At the 2-year postoperative follow-up, the patient had continued to perform good oral hygiene and maintain minimal levels of gingival inflammation. There were no sites that bled upon probing, and all probing depths around the teeth supporting the RPD were 3 mm or less (Figure 12). The authors attribute this improvement in periodontal condition to the patient's improved oral hygiene and compliance to the proposed 3-month maintenance interval.
An appreciable increase in the thickness and width of keratinized gingiva of the mandibular anterior lingual gingiva at sites Nos. 22 and 23 was noted upon clinical examination (Figure 13). Thicker gingival tissue and increased width of keratinized gingiva are advantageous because this may help prevent possible soft-tissue defects.16 There was also an increased thickness of keratinized tissue at sites Nos. 26 and 27, although these teeth did not receive any type of soft-tissue augmentation. It is surmised that the improved design and increased relief of the RPD allowed this area to thicken without surgical intervention.9
Although no surgical treatment was performed at the sites of the contralateral teeth (Nos. 26 and 27), the authors postulate that the combination of surgical/nonsurgical treatment, along with an improved design of the RPD, was needed to resolve the fenestrations at sites Nos. 22 and 23, as their presence precluded the patient from being able to perform effective oral hygiene. Another consideration in favor of the surgical/nonsurgical approach was that the clinicians needed validation in the prognosis of the teeth as well as a dimensionally stable surface before proceeding with a new RPD.
Conclusion
This case report demonstrates the use of a SCTG as a viable treatment option in the restoration of gingival fenestrations in the mandibular anterior lingual region. The case underscores the significance of partial denture design in relation to gingival health and the importance of compliance to a strict maintenance protocol with proper oral hygiene techniques and debridement at the appropriate interval.
About the Authors
Joshua Shayefar, DMD
Private Practice specializing in Periodontics and Implant Dentistry, Los Angeles, California
Elena Sanz-Miralles, DDS, MSc, MS, PhD
Assistant Professor in Dental Medicine, Division of Periodontics, Section of Oral, Diagnostic and Rehabilitation Sciences, Columbia University College of Dental Medicine, New York, New York
Robert N. Eskow, DMD, MScD
Clinical Professor, Division of Periodontics, Section of Oral, Diagnostic and Rehabilitation Sciences, Columbia University College of Dental Medicine, New York, New York; Private Practice specializing in Periodontics, Implant Dentistry, and Oral Medicine, Livingston, New Jersey
Gary Greenstein, DDS, MS
Clinical Professor, Division of Periodontics, Section of Oral, Diagnostic and Rehabilitation Sciences, Columbia University College of Dental Medicine, New York, New York; Private Practice specializing in Surgical Implantology and Periodontics, Freehold, New Jersey
References
1. Elliot JR, Bowers GM. Alveolar dehiscence and fenestration. Periodontics. 1963;1:245-248.
2. Edel A. Alveolar bone fenestrations and dehiscences in dry Bedouin jaws. J Clin Periodontol.1981;8(6):491-499.
3. Lane JJ. Gingival fenestration. J Clin Periodontol. 1977;48(4):225-227.
4. Chen G, Fang CT, Tong C. The management of mucosal fenestration: a report of two cases. Int Endod J. 2009;42(2):156-164.
5. Rawlinson A. Treatment of a labial fenestration of a lower incisor tooth apex. Br Dent J. 1984;156(12):448-449.
6. Langer B, Langer L. Subepithelial connective tissue graft technique for root coverage. J Periodontol. 1985;56(12):715-720.
7. Caton JG, Armitage G, Berglundh T, et al. A new classification scheme for periodontal and peri-implant diseases and conditions - introduction and key changes from the 1999 classification. J Periodontol. 2018;89(suppl 1):S1-S8.
8. Schüpbach P, Gaberthüel T, Lutz F, Guggenheim B. Periodontal repair or regeneration: structures of different types of new attachment. J Periodontal Res. 1993;28(4):281-293.
9. Bissada NF, Ibrahim SI, Barsoum WM. Gingival response to various types of removable partial dentures. J Periodontol. 1974;45(9):651-659.
10. Carlsson GE, Hedegard B, Koivumaa KK. Studies in partial dental prosthesis, III. A longitudinal study of mandibular partial dentures with double extension saddles. Acta Odontol Scand. 1962;20:95-119.
11. Sawes WL, Barnes IE. The surgical treatment of fenestrated buccal roots of an upper molar: a case report. Int Endod J. 1983;16(2):82-86.
12. Addy M, Bates JF. Plaque accumulation following the wearing of dif-fe-rent types of removable partial dentures. J Oral Rehabil. 1979;6(2):111-117.
13. Owall B. Design of removable partial dentures and dental technician education. Sven Tandlak Tidskr. 1974;67(1):21-32.
14. Carr AB, Brown DT. Rests and rest seats. In: Carr AB, Brown DT, eds. McCracken's Removable Partial Prosthodontics. 12th ed. St. Louis, MO: Mosby; 2011:56-66.
15. Dello Russo NM. Gingival autografts as an adjunct to removable partial dentures. J Am Dent Assoc. 1982;104(2):179-181.
16. Edel A. Clinical evaluation of free connective tissue grafts used to increase the width of keratinised gingiva. 1974. Periodontal Clin Investig. 1998;20(1):12-20.