How Can Clinicians Limit the Risk of Peri-implantitis?
Chandur P.K. Wadhwani, BDS, MSD
Abstract: When using dental implants as a treatment modality for tooth replacement, the integration of peri-implant soft tissue is an extremely important consideration. Numerous systemic risk factors for peri-implant disease are known to be associated with peri-implant soft tissues. The soft-tissue connection provides a barrier seal directly to the implant or implant abutment and plays a critical role in limiting peri-implant disease. Therefore, clinicicans must take great care in managing the soft tissue. This article discusses three key stages of soft-tissue connection that should be considered when providing dental implant therapy: the healing stage, where cellular adhesion and proliferation are attained; the restorative phase, during which protection is provided to the mature soft-tissue site; and maintenance, a phase where the soft tissue offers revealing information about the health of the implant.
Although dental implant treatment is beneficial for tooth replacement for many patients, peri-implant disease is a prevalent challenge for clinicians and remains a potential complication. Conducting a holistic evaluation in which soft-tissue/implant interactions are considered may help enable clinicians make proper decisions and limit the risks from peri-implant disease.
Osseointegration is synonymous with dental implantology. For example, implant surgical planning primarily relates to bone structure profiles attained through radiographic imaging, and treatment outcomes are commonly related to bone levels. Even various educational academies are dedicated to osseointegration. Clearly, bone is vitally important in stabilizing, securing, and supporting the implant body and restoration.
With regard to longevity, one area that may often be overlooked is peri-implant soft-tissue integration. These tissues, both connective and epithelial, are vital to providing the seal that develops around and directly attaches to a dental implant. This soft-tissue barrier compartment is often referred to as the implant biologic width.1 This biological element is important to recognize since dentistry is one of the few disciplines in medicine in which practitioners purposely perforate the body's external barrier and leave an implanted medical device exposed. Not only does the device connection site become a potential portal to the body, but it exists in an extremely hostile environment, namely the oral cavity. Additionally, the implant site is constantly challenged by microbes, thermal changes, and extreme forces of mastication.
Risk Factors
An interesting observation is that the known risk factors related to peri-implant disease do not appear to be impacted by conditions that weaken or compromise alveolar bone, but rather are associated with conditions or diseases that affect primarily host soft tissues. Examples of systemic bone conditions that are not considered to present contraindications to dental implant placement or affect implant outcome include osteoporosis,2 osteomalacia (x-linked hypophosphatemia),3 osteogenesis imperfecta,4 Paget's disease,5 and antiresoptive therapy such as oral bisphosphonate use.6
Conversely, a number of known systemic risk factors for peri-implant disease are associated with peri-implant soft tissues. Two such factors are previous periodontal disease and poor oral hygiene.Associated microbes have been shown to affect the mucosal epithelial barrier. For example, Porphyromonas gingivalis can subvert host responses by inactivating immune cells and molecules and further activating host processes that lead to epithelial tissue destruction.7,8 Other factors include diabetes and smoking, which have both been shown to have reduced mucosal microcirculation.9,10 Rheumatoid arthritis is another risk factor;a greater degree of soft-tissue inflammation with increased bone resorption around implants is found, particularly in concomitant connective tissue disease.11Lastly, residual excess cementmaterials have been shown to affect gingival fibroblast growth.12
Three Phases of Soft-Tissue Connection
Recognizing that the soft-tissue connection provides a barrier seal to the implant or implant abutment and plays a crucial role in the progression of peri-implant disease, it is prudent to treat the soft tissue with great respect. Three distinct stages of soft-tissue connection may be considered: (1) healing, where the goals are cellular adhesion and proliferation; (2) restorative, where the mature soft-tissue site needs to be protected during restoration; and (3) maintenance, during which the soft tissue provides intimate information about the health of the implant.
Soft-Tissue Healing: Nurturing Through Planning and Surgical Stages
Healing of the soft tissue is a prerequisite to implant planning. The goal in this phase is to ensure that the soft tissue is of adequate thickness to shroud underlying bone and maintain esthetics.13 The tissue site should be generally healthy, so as to eliminate or, at minimum, reduce risk factors for future implant disease or failure. Examples of ways to nurture healing would be to improve oral hygiene with periodontal debridement as a preparatory procedure to lower the microbial load and, where appropriate, promote smoking cessation.14
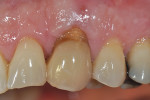
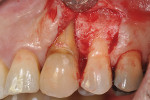
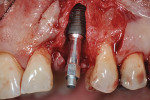
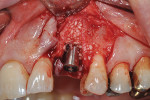
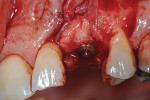
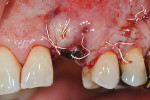
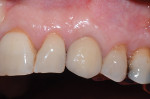
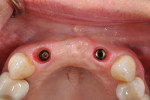
Surgical implant planning should be used to evaluate the quality and quantity of both hard and soft tissues, and, if necessary, a proactive approach should be taken by implementing soft- and/or hard-tissue augmentation procedures. Efforts made during this stage to ensure that the site is properly prepared may improve long-term results (Figure 1 through Figure 7).
Componentry used for implant placement should be clean and uncontaminated; implants should maintain their ideal surface characteristics and free surface energy.15 Reuse of implant components, including healing abutments and cover screws, is discouraged, as studies have reported an inability to clean these components to a degree comparable to new healing abutments (Figure 8 and Figure 9).16,17 Biologically, any contamination will affect cell adhesion and growth.15 Moreover, surface modifications that occur as a result of steam autoclaving have been shown to have a negative effect on gingival fibroblast attachment and spreading.18
The clinician should consider the materials used when fabricating either a custom-contoured healing abutment or a provisional restoration against which the soft tissues will come into contact during healing. Resin composite, compomers, and glass-ionomers have been shown to be cytotoxic to gingival fibroblasts.19 All componentry should be new and free from contamination when used in the wound site. Resins placed during flap surgery have also been shown to induce negative effects resulting in bone resorption.20 If the provisional restoration is cement-retained, the cement must be well controlled, with consideration given to material type, volume used, application technique, and seating forces.21,22 Cement within the healing tissue can cause a foreign-body reaction, which has been strongly implicated in causing peri-implant disease.23
Restorative: The Mature Implant Sulcus
The soft tissues are affected by repeated removal and reattachment of implant components. Therefore, doing so should be kept to a minimum because it could result in unwanted loss in implant-supporting tissues.15 The healed soft-tissue site that forms the sulcus around the implant differs in multiple ways from that which is found around a natural tooth.23 Natural tooth sulcular tissue is more robust and less permeable and has a greater ability to repair due to good blood supply derived from the periodontal ligament and adjacent tissues. As described by Atherton, the tooth sulcus is well supported by underlying connective tissue containing Sharpey's fiber attachments that are inserted into the cementum of the tooth and the parakeratinized and keratinized epithelial tissue, providing a somewhat impervious barrier.24
In contrast, the sulcus surrounding an implant is weaker, with a hemidesmosomal attachment that is easily traumatized and torn by forces, such as when retraction cord is placed.23 This soft tissue also has a poor blood supply with limited repair capability, which is derived primarily from the underlying periosteum and adjacent tissues. The sulcus around an implant is mucosal (Figure 10). It has no keratinization and great permeability, allowing intrusion of foreign materials such as cement. Residual excess cement can have other negative effects, including allergic response and corrosion of titanium and its alloys, and it can act as a nidus for pathogenic microbial contamination.25
Although the avoidance of cement may reduce the likelihood of peri-implant disease, the use of screw retention also has issues that need to be considered. Screw-loosening events can result in inflammatory peri-implant mucositis due to movement of the abutment. In extreme cases wear of the implant can occur, shedding titanium particles into the surrounding tissues.26 Screw loosening in single implant crowns represents the primary complication reported, with an incidence rate of approximately 10%.27 This can be attributed mainly to poor control and lack of understanding of how an implant screw works, use of inappropriate tightening procedures and/or torque wrenches that are out of calibration,28,29 and physiological changes that occur in the natural dentition that dynamically alter the occlusion.30,31 Such alterations may result in increased forces being placed on the implant restoration in a different direction from which it was originally designed.
Implant components for the final restoration should be as biocompatible as possible. Obviously, they should be clean on delivery. Ideally, abutments should be sterilized by gamma radiation. They should not be autoclaved, as autoclaving is known to alter the surface of materials such as titanium and zirconia and reduce the adhesion of gingival fibroblasts.32 Disinfection of custom abutments can be achieved by using high-pressure steam.33 Cleaners such as sodium hypochlorite damage titanium and have been shown to induce corrosion and alter surface roughness significantly.33
Component fit is another factor that may increase the likelihood of complications and the potential for peri-implant disease. In most cases component fit has been shown to be optimum when original manufacturer components are used.34 Component fit is known to have an impact on both the microgap and micromovement at the implant-abutment interface.35
Implant componentry and restoration must allow for access to cleaning, by both the patient and dental team. Poor oral hygiene is a major factor in promoting peri-implant disease.
Maintenance: Soft Tissues as an Indicator of Implant Health
Lastly, the soft tissues may provide a signal that alerts the clinician to the development of a disease process. Bleeding on probing is considered a useful test with a high positive predictive value for disease. The American Academy of Periodontology adopted this test in its 2018 classification system.36
If the sulcus is probed correctly and bleeding occurs at two out of three recall occasions, the site is deemed to be diseased.37 At a minimum, peri-mucositis is occurring, and treatment must be started. Treatment may involve simply improving oral hygiene. If bone loss is noted and considered to be beyond physiological, then more advanced treatments may be required.
While seemingly a simple test, bleeding on probing must be performed correctly with the proper amount of pressure.38 If too much force is used with an inappropriate probe, bleeding of a non-diseased site will likely produce a false positive. Conversely, if too little force is applied or an inappropriate probe used, the opposite, a false negative, will occur.
One way to determine whether the correct pressure is being used is to regularly perform calibration. This can be done with the use of a weigh scale that measures in grams and by knowing the dimension of the probing instrument (Figure 11 through Figure 14). The goal is to use a target pressure of 119 Ncm2, which is calculated by knowing the probe tip diameter and recognizing that 1 N equals 102 g in weight.38,39
Conclusion
To minimize problems associated with peri-implant disease and maximize long-term outcomes, clinicians need to have knowledge of the medical, environmental, sterilization, and componentry considerations involved in implant placement, as well as the phases of hard- and soft-tissue healing and maturation. Understanding and respecting biological concepts related to the soft-tissue attachment at an implant site can reduce the risk of future problems, such as peri-implant disease.
About the Author
Chandur P.K. Wadhwani, BDS, MSD
Affiliate Assistant Professor, Restorative Department, University of Washington School of Dentistry, Seattle, Washington; Adjunct Assistant Professor, Advanced Education Program in Prosthodontics, Loma Linda University School of Dentistry, Loma Linda, California; Affiliate Associate Professor, Graduate Periodontics, Oregon Health & Science University School of Dentistry, Portland, Oregon; Private Practice, Bellevue, Washington
References
1. Judgar R, Giro G, Zenobio E, et al. Biological width around one- and two-piece implants retrieved from human jaws. Biomed Res Int. 2014;
2014:850120.
2. Wagner F, Schuder K, Hof M, et al. Does osteoporosis influence the marginal peri-implant bone level in female patients? A cross-sectional study in a matched collective. Clin Implant Dent Relat Res. 2017;19
(4):616-623.
3. Friberg B. Brånemark system implants and rare disorders: a report of six cases. Int J Periodontics Restorative Dent. 2013;33(2):139-148.
4. Prabhu N, Duckmanton N, Stevenson AR, Cameron A. The placement of osseointegrated dental implants in a patient with type IV B osteogenesis imperfecta: a 9-year follow-up. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007;103(3):349-354.
5. Torres J, Tamimi F, Garcia I, et al. Dental implants in a patient with Paget disease under bisphosphonate treatment: a case report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;107(3):387-392.
6. Stavropoulos A, Bertl K, Pietschmann P, et al. The effect of antiresorptive drugs on implant therapy: systematic review and meta-analysis. Clin Oral Implants Res. 2018;29(suppl 18):54-92.
7. Andrian E, Grenier D, Rouabhia M. Porphyromonas gingivalis-epithelial cell interactions in periodontitis. J Dent Res. 2006;85(5):392-403.
8. Abdulkareem AA, Shelton RM, Landini G, et al. Potential role of periodontal pathogens in compromising epithelial barrier function by inducing epithelial-mesenchymal transition. J Periodontal Res. 2018;53(4):565-574.
9. Scardina G, Citarrella R, Messina P. Diabetic microagiopathy of oral mucosa depends on disease duration and therapy. Med Sci Monit. 2017;
23:5613-5619.
10. Scardina GA, Messina P. Morphologic changes in the microcirculation induced by chronic smoking habit: a videocapillaroscopic study on the human gingival mucosa. Am J Dent. 2005;18(4):301-304.
11. Krennmair G, Seemann R, Piehslinger E. Dental implants in patients with rheumatoid arthritis: clinical outcome and peri-implant findings. J Clin Periodontol. 2010;37(10):928-936.
12. Rodriguez LC, Saba JN, Chung KH, et al. In vitro effects of dental cements on hard and soft tissues associated with dental implants. J Prosthet Dent. 2017;118(1):31-35.
13. Puisys A, Linkevicius T. The influence of mucosal tissue thickening on crestal bone stability around bone-level implants. A prospective controlled clinical trial. Clin Oral Implants Res. 2015;26(2):123-129.
14. Davis JM, Ramseier CA, Mattheos N, et al. Education of tobacco use prevention and cessation for dental professionals-a paradigm shift. Int Dent J. 2010;60(1):60-72.
15. Rompen E, Domken O, Degidi M, et al. The effect of material characteristics, of surface topography and of implant components and connections on soft tissue integration: a literature review. Clin Oral Implants Res. 2006;17(suppl 2):55-67.
16. Bidra AS, Kejriwal S, Bhuse K. Should healing abutments and cover screws for dental implants be reused? A systematic review. J Prosthodont. 2020;29(1):42-48.
17. Wadhwani C, Schonnenbaum TR, Audia F, Chung KH. In-vitro study of the contamination remaining on used healing abutments after cleaning and sterilizing in dental practice. Clin Implant Dent Relat Res. 2016;18(6):1069-1074.
18. Vezeau PJ, Keller JC, Wightman JP. Reuse of healing abutments: an in vitro model of plasma cleaning and common sterilization techniques. Implant Dent. 2000;9(3):236-246.
19. Celik N, Binnetoglu D, Ozakar Ilday N, et al. The cytotoxic and oxidative effects of restorative materials in cultured human gingival fibroblasts. Drug Chem Toxicol. 2019;1-6. doi: 10.1080/01480545.2019.1620265.
20. Santamaria MP, Suaid FF, Carvalho MD, et al. Healing patterns after subgingival placement of a resin-modified glass-ionomer restoration: a histometric study in dogs. Int J Periodontics Restorative Dent. 2013;33(5):679-687.
21. Wadhwani CP, Schwedhelm ER. The role of cements in dental implant success, Part I. Dent Today. 2013;32(4):74-78.
22. Wadhwani CP, Chung KH. The role of cements in dental implant success, Part 2. Dent Today. 2013;32(6):46,48-51.
23. Wadhwani C, ed. Cementation in Dental Implantology: An Evidence-Based Guide. Springer-Verlag Berlin Heidelberg; 2015.
24. Atherton JD. The gingival response to orthodontic tooth movement. Am J Orthod. 1970;58(2):179-186.
25. Raval NC, Wadhwani CP, Jain S, Darveau RP. The interaction of implant luting cements and oral bacteria linked to peri-implant disease: an in vitro analysis of planktonic and biofilm growth-a preliminary study. Clin Implant Dent Relat Res. 2015;17(6):1029-1035.
26. Taylor TD, Klotz MW, Lawton RA. Titanium tattooing associated with zirconia implant abutments: a clinical report of two cases. Int J Oral Maxillofac Implants. 2014;29(4):958-960.
27. Goodacre BJ, Goodacre SE, Goodacre CJ. Prosthetic complications with implant prostheses (2001-2017). Eur J Oral Implantol. 2018;11 suppl 1:S27-S36.
28. Wadhwani CPK, O'Brien RT, Rosen PS, Chung KH. A technique to validate the accuracy of a beam-type mechanical torque limiting device. J Prosthet Dent. 2020;S0022-3913(20)30025-1.
29. ISO 6789-2:2017. Assembly tools for screws and nuts - hand torque tools - Part 2: requirements for calibration and determination of measurement uncertainty. 2017. Geneva, Switzerland: International Organization for Standardization; https://www.iso.org/standard/62550.html. Accessed May 22, 2020.
30. Varthis S, Tarnow DP, Randi A. Interproximal open contacts between implant restorations and adjacent teeth. Prevalence - causes - possible solutions. J Prosthodont. 2019;28(2):e806-e810.
31. Daftary F, Mahallati R, Bahat O, Sullivan RM. Lifelong craniofacial growth and the implications for osseointegrated implants. Int J Oral Maxillofac Implants. 2013;28(1):163-169.
32. Mehl C, Kern M, Zimmermann A, et al. Impact of cleaning procedures on adhesion of living cells to three abutment materials. Int J Oral Maxillofac Implants. 2017;32(5):976-984.
33. Homayouni A, Bahador A, Moharrami M, et al. Effect of 5 popular disinfection methods on microflora of laboratory: customized implant abutments. Implant Dent. 2019;28(5):437-446.
34. Hurson S. Use of authentic, integrated dental implant components vital to predictability and successful long-term clinical outcomes. Compend Contin Educ Dent. 2016;37(7):450-455.
35. Liu Y, Wang J. Influences of microgap and micromotion of implant-abutment interface on marginal bone loss around implant neck. Arch Oral Biol. 2017;83:153-160.
36. Caton JG, Armitage G, Berglundh T, et al. A new classification scheme for periodontal and peri-implant diseases and conditions - introduction and key changes from the 1999 classification. J Periodontol. 2018;89
(suppl 1):S1-S8.
37. Luterbacher S, Mayfield L, Brägger U, Lang NP. Diagnostic characteristics of clinical and microbiological tests for monitoring periodontal and peri-implant mucosal tissue conditions during supportive periodontal therapy (SPT). Clin Oral Implants Res. 2000;11(6):521-529.
38. Cha J, Wadhwani C, Wang M, et al. Instrument selection and application used to probe dental implants. Int J Oral Maxillofac Implants. 2019;34(1):115-123.
39. Gerber JA, Tan WC, Balmer TE, et al. Bleeding on probing and pocket probing depth in relation to probing pressure and mucosal health around oral implants. Clin Oral Implants Res. 2009;20(1):75-78.