Observed Healing of an Immediately Placed Implant in a Molar Site Without Bone Replacement Graft or Primary Closure
Noam Saltzburg, DDS; and Philip Kang, DDS
Abstract: The aim of this case report is to present a clinical example of successful osseointegration of an implant placed immediately following extraction of a mandibular left first molar (tooth No. 19) with a horizontal gap of more than 2 mm and implant threads exposed within the socket, with healing by secondary intention without flap closure, bone grafting, or barrier membrane placement. The healing was photographed every day for the first week to provide photodocumentation of early healing and then was subsequently photographed weekly for the first month and monthly for the first 6 months. The outcome showed that osseointegration of an implant placed immediately in a posterior extraction site is possible without having to graft the gap around the implant.
When a tooth is extracted, multiple processes are initiated that ultimately lead to healing of the extraction site. Initially, blood fills the socket and a clot is formed. This clot plugs severed vessels and stops the bleeding.1 Within a few days, large numbers of inflammatory cells, including polymorphonuclear cells (PMNs) and macrophages, migrate to the wound to clean the site and form granulation tissue. The granulation tissue is then replaced by provisional connective tissue matrix or osteoid tissue that is rich in collagen fibers and cells. The osteoid tissue fills the socket by 3 to 4 weeks and subsequently is penetrated by blood vessels and osteoblasts. Woven bone formation is completed around 3 months and is further mineralized to form denser lamellar bone at around 4 months.1
According to a systematic review by Tan et al, the mean horizontal ridge dimensional reduction following tooth extraction was 3.79 mm in the first 6 months, and mean vertical dimensional reduction was 1.24 mm at 6 months.2 Their study included cases in which a flap was elevated to extract the tooth. Other studies demonstrate that when no flap is raised, there is less horizontal and vertical bone loss.3,4
Factors to Consider
When deliberating immediate implant placement in a molar site, several factors should be considered:
Immediate implants-Implants that are placed immediately into fresh extraction sockets offer the benefit of saving time and patient visits. It is worth noting that immediate implant placement in fresh extraction sites yields similar survival rates to implants placed in healed ridges.5
Molar site classification-Smith and Tarnow presented a classification of molar sites for immediate implant placement.6 Type A socket has an adequate septal bone to circumferentially contain the coronal portion of the implant within the bone. Type B socket has septal bone to stabilize the implant but does not fully contain it. Type C socket does not have enough bone to stabilize the implant without engaging the outer walls of the socket.6
Managing the buccal gap-According to various authors, grafting a buccal gap of more than 2 mm is recommended in conjunction with immediate implant placement.7,8 However, other authors reported bone fill in sites with initial gaps of more than 2 mm even when no bone graft material was placed.9-11
Case Report
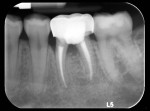
A 24-year-old patient presented to the Postgraduate Periodontics Clinic at the Columbia University College of Dental Medicine with the chief complaint of sensitivity around her mandibular left first molar (tooth No. 19). Upon clinical examination, gingival inflammation and purulence from the furcal area of No. 19 were noted. Radiographic bone loss was evident in the furcation, and possible recurrent decay was seen in the furcal aspect of tooth No. 19 (Figure 1). Additionally, this tooth had had previous root canal treatment with a stainless-steel crown more than 10 years prior. The patient also indicated that at the time of root canal treatment, a file had broken off in one of the canals. After consultation with the patient's general dentist and endodontist, tooth No. 19 was deemed to be nonrestorable, and the patient opted for extraction and implant placement.
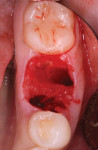
A CBCT was taken to determine the location of the inferior alveolar nerve relative to tooth No. 19. The patient was premedicated with 2 grams of amoxicillin taken 1 hour before the procedure. The patient was anesthetized with 2% lidocaine with 1:100,000 epinephrine via left inferior alveolar nerve block and local infiltration buccal and lingual of No. 19. The tooth was sectioned and extracted without raising a flap. The individual sockets were degranulated and irrigated with sterile saline (Figure 2).
The extraction socket had intact buccal and lingual plates as well as intact septal bone, which widened apically. According to the Smith and Tarnow classification of molar sites, this was a type B socket, where the implant could be stabilized in, but not fully surrounded by, septal bone.6 It was determined that immediate implant placement was viable.
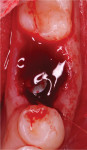
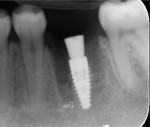
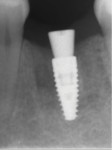
The osteotomy was prepared with the surgical kit (Straumann®, straumann.com) to a dimension of 3.8 mm x 10 mm relative to the septal bone. The 4.1 mm x 10 mm fixture implant (Straumann® BLT SLActive, Straumann) was placed and locked at 35 Ncm. The threads of the implant buccolingually were stabilized within the bone; however, mesially and distally approximately three to four threads of the implant were exposed within the socket. A 3.5 mm tapered healing abutment was placed and a blood clot was allowed to form and fill the socket (Figure 3). No bone graft material or barrier membrane was placed. A periapical radiograph was taken to confirm implant placement (Figure 4). One 4-0 chromic gut suture was placed in the mesial papilla of site No. 19.
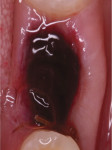
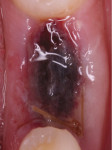
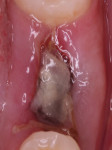
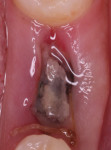
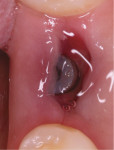
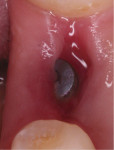
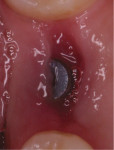
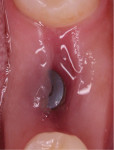
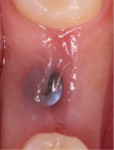
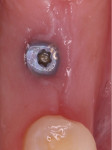
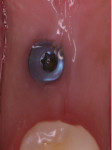
The patient was placed on 875 mg amoxicillin twice per day for 1 week and advised to avoid brushing the area for the first 2 weeks. She was instructed to rinse twice per day with chlorhexidine 0.12% rinse. Healing proceeded uneventfully. The healing was photographed throughout the first week (Figure 5 through Figure 9), then every week for the first month (Figure 10 through Figure 12), and then once a month until 6 months postoperatively (Figure 13 through Figure 16).
Typically, after extraction the socket fills with blood. As mentioned earlier, the blood clot plugs severed vessels and stops the bleeding. Within 2 to 3 days many inflammatory cells migrate to the wound to clean the site before new tissue forms. Combinations of inflammatory cells (eg, PMNs, macrophages, etc), vascular sprouts, and immature fibroblasts form the granulation tissue. Granulation tissue is replaced with provisional connective tissue matrix that is rich in collagen fibers and cells (osteoid tissue).1
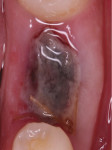
In the present case, a fibrin clot clearly developed during the first week of healing and the blood clot appeared to be stable throughout the initial healing process (Figure 5 through Figure 9). From weeks 2 through 8 vascularization progressed as evidenced by the reddish hue around the implant and connective tissue fill (Figure 10 through Figure 13). Epithelial fusion appeared complete by 3 months (Figure 14).
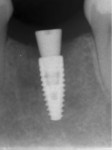
A periapical radiograph taken at 4 months demonstrated bone apposition against the implant and almost complete mineralization of the mesial and distal sockets (Figure 17). The clinicians decided to wait an additional 2 months before taking the final impression to allow for more complete remineralization and remodeling of the site. A periapical radiograph at 6 months demonstrated increased mineralization of the site (Figure 18).
Discussion
When planning to replace missing teeth with implants, clinicians should consider whether immediate implant placement is a viable option, as it can help decrease overall treatment time and circumvent the need for multiple procedures. Several considerations must be taken into account when proceeding with immediate implant placement, including whether adequate bone in which primary implant stability may be achieved is present, whether to proceed with a flap or flapless approach, and how to manage the gap around the implant.
In considering flap versus flapless extraction, studies suggest that a flapless approach may be advantageous in preserving blood supply to the bone, especially in the esthetic zone.1,12,13 Other studies, however, show that there is no difference between flap and flapless approaches in terms of bone loss and soft-tissue recession.14 Relative to managing the gap around implants placed in a fresh extraction socket, numerous authors suggest bone grafting if the gap is greater than 2 mm.7,8 However, other authors reported bone fill in sites with initial gaps greater than 2 mm even when no bone graft material was placed.9-11
This case report demonstrates that an implant placed in a fresh extraction socket with no flap elevation, graft material, or barrier membrane and is allowed to heal by secondary intention will osseointegrate and have bone fill around the implant despite the presence of a gap larger than 2 mm. Although histology was not performed in this case, Tarnow and Chu in a similar case of an immediate implant placement without flap elevation, grafting material, or barrier membrane and a buccal gap of 4.2 mm demonstrated histologically intimate bone contact with the first thread in the coronal portion and establishment of biologic width coronal to the bone contact with connective tissue and junctional epithelium.11
While this case had similar success to the aforementioned case, clinicians must consider the potential of increased risk of failure should the implant be unable to hold the clot to the level of the platform. If the clot were to shrink during the initial healing and several threads were to become exposed, then implant removal would be necessary. Therefore, despite what should be biologically plausible, careful planning must be done in an effort to minimize risks involved that could lead to treatment failure. Botticelli et al demonstrated that implant surface characteristics play a role in initial clot stabilization and that a roughened surface provides better clot stabilization and, therefore, enhanced osseointegration.15
In this case, the success of the treatment can likely be partly attributed to the utilization of a roughened implant surface, which may have helped adequately stabilize and hold the blood clot during healing. Additionally, the fact that the overall socket (buccal and lingual plates) was completely intact played a role in the socket healing and blood clot stabilization in that the implant was able to be placed approximately 2 mm subcrestally and fully contained within the socket.
Conclusion
This case report provides clinical evidence that immediate implant placement into a fresh extraction site with intact buccal and lingual plates can result in osseointegration without the use of graft materials or a barrier membrane to stabilize the blood clot despite having implant threads exposed within the extraction site and a more-than 2 mm gap distance. Further research should be conducted to evaluate the predictability of this type of wound healing.
About the Authors
Noam Saltzburg, DDS
Former Resident, Postgraduate Periodontics Program, Columbia University College of Dental Medicine, New York, New York
Philip Kang, DDS
Associate Professor, Division of Periodontics, Section of Oral, Diagnostic and Rehabilitation Sciences, Columbia University College of Dental Medicine, New York, New York
References
1. Araújo MG, Silva CO, Misawa M, Sukekava, F. Alveolar socket healing: what can we learn? Periodontol 2000. 2015;68(1):122-134.
2. Tan WL, Wong TLT, Wong MCM, Lang NP. A systematic review of post-extractional alveolar hard and soft tissue dimensional changes in humans. Clin Oral Implants Res. 2012;23(suppl 5):1-21.
3. Job S, Bhat V, Naidu EM. In vivo evaluation of crestal bone heights following implant placement with ‘flapless' and ‘with-flap' techniques in sites of immediately loaded implants. Indian J Dent Res. 2008;19(4):320-325.
4. Barros RRM, Novaes AB Jr, Papalexiou V. Buccal bone remodeling after immediate implantation with a flap or flapless approach: a pilot study in dogs. Titanium. 2009;1:45-51.
5. Lang NP, Pun L, Lau KY, et al. A systematic review on survival and success rates of implants placed immediately into fresh extraction sockets after at least 1 year. Clin Oral Implants Res. 2012;23(suppl 5):39-66.
6. Smith RB, Tarnow DP. Classification of molar extraction sites for immediate dental implant placement: technical note. Int J Oral Maxillofac Implants. 2013;28(3):911-916.
7. Chen ST, Wilson TG Jr, Hämmerle CH. Immediate or early placement of implants following tooth extraction: review of biologic basis, clinical procedures, and outcomes. Int J Oral Maxillofac Implants. 2004;19 suppl:12-25.
8. Greenstein G, Cavallaro J. Managing the buccal gap and plate of bone: immediate dental implant placement. Dent Today. 2013;32(3):70-77.
9. Akimoto K, Becker W, Persson R, et al. Evaluation of titanium implants placed into simulated extraction sockets: a study in dogs. Int J Oral Maxillofac Implants. 1999;14(3):351-360.
10. Botticelli D, Berglundh T, Lindhe J. Hard-tissue alterations following immediate implant placement in extraction sites. J Clin Periodontol. 2004;31(10):820-828.
11. Tarnow DP, Chu SJ. Human histologic verification of osseointegration of an immediate implant placed into a fresh extraction socket with excessive gap distance without primary flap closure, graft, or membrane: a case report. Int J Periodontics Restorative Dent. 2011;31(5):515-521.
12. Schropp L, Wenzel A, Kostopoulos L, Karring T. Bone healing and soft tissue contour changes following single-tooth extraction: a clinical and radiographic 12-month prospective study. Int J Periodontics Restorative Dent. 2003;23(4):313-323.
13. Araújo MG, Lindhe J. Dimensional ridge alterations following tooth extraction. An experimental study in the dog. J Clin Periodontol. 2005;32
(2):212-218.
14. Maló P, Nobre MD. Flap vs. flapless surgical techniques at immediate implant function in predominantly soft bone for rehabilitation of partial edentulism: a prospective cohort study with follow-up of 1 year. Eur J Oral Implantol. 2008;1(4):293-304.
15. Botticelli D, Berglundh T, Persson LG, Lindhe J. Bone regeneration at implants with turned or rough surfaces in self-contained defects. An experimental study in the dog. J Clin Periodontol. 2005;32(5):448-455.