Biomechanics and Function: Altering Paradigms to Treat a Patient’s Esthetic Disability Conservatively
Kris Swanson, DDS; and Leon Hermanides, CDT
Abstract: As conservative dentistry has progressed in recent years, new developments in bonding protocols have enabled clinicians to predictably utilize restorative material on any surface of the tooth to achieve treatment goals. One such advancement is the bonding of composite and indirect restorations to the occlusal surfaces of posterior teeth to modify the occlusal vertical dimension (OVD). In this case presentation involving a patient with a constricted chewing pattern (CCP) who did not want orthodontic therapy, conservative treatment focused on increasing the patient's OVD using a combination of direct and indirect restorations in an attempt to alleviate the CCP. This minimally invasive additive approach addressed the esthetics in the case while limiting functional and biomechanical risks.
Dentists are trained to be as conservative as possible when attempting to meet both esthetic and functional goals in any given case. This often has dictated the use of orthodontics to move teeth into proper position to minimize the amount of restorative work necessary. With the advent in recent years of predictable bonding protocols for lithium disilicate, zirconium, and composite a paradigm shift has occurred in how a restorative dentist might treatment plan.1 It is now possible to predictably add restorative material to any surface of the teeth to achieve the treatment goals. This includes bonding of composite and indirect restorations to the occlusal surfaces of posterior teeth (when mostly in enamel) in order to alter the occlusal vertical dimension (OVD).
The case presented involves a patient with a constricted chewing pattern (CCP) who wanted to significantly improve his smile but was adamant at the initial examination that he was unwilling to undergo any orthodontic treatment. After data collection, careful analysis, and diagnosis a conservative treatment plan was devised that included the use of a 10-step approach (10 Step Management Considerations, Kois Center, koiscenter.com) and multidisciplinary restorative procedures. The treatment would involve alleviating the patient's CCP by increasing the OVD utilizing a combination of direct and indirect restorations. To avoid increasing any biomechanical risk, preparations mostly in enamel would be used on the maxillary posterior teeth. These conservative additive restorations would be the key to minimizing the overall functional and biomechanical risks and treating the esthetic disability of the case.2
Clinical Case Overview
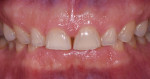
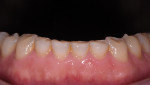
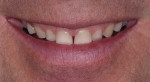
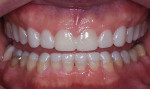
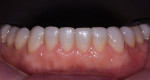
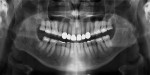
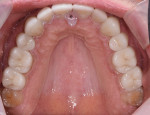
A 63-year-old male patient presented with concerns that his teeth were small in size and wanted them to be made to appear larger. He also was concerned about their discoloring and requested that they be made whiter. Additionally, he noted that his anterior teeth were chipping and breaking (Figure 1 and Figure 2). He was absolutely opposed to orthodontic treatment because of his professional public speaking but was open to other solutions with the goal of achieving "a million dollar smile," he said.
Using the Kois risk assessment and treatment planning protocol3,4 a conservative plan was developed comprising a combination of direct composites, full-coverage crowns, and minimally prepared additive veneer onlays (AVOs). These additive indirect restorations would prove to be critical in achieving both the functional and esthetic goals of the treatment.
Medical and Dental History
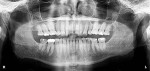
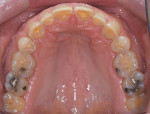
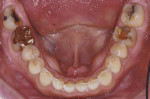
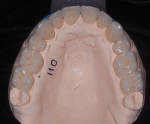
The patient's medical history revealed no significant concerns or contributors to his dental health. He did not drink alcohol, smoke, or take any medications. He was American Society of Anesthesiologists (ASA) classification II due to his age. Upon examination, significant attrition and some erosion was evident, particularly on teeth Nos. 6 through 11 and 22 through 27 (Figure 3). He was tested for acid reflux and found negative, and after exploring his dietary intake no contributors for erosion were found. His dental history included orthodontics from ages 15 through 17. He reported worn, chipped anterior teeth and that he needed to "squeeze" to get his posterior teeth to touch. The patient was very self-conscious about his smile, and upon further conversation it was quite apparent that he wanted a smile he could be proud of.
Diagnosis, Risk Assessment, and Prognosis
Periodontal: The patient had no evidence of periodontal disease. He had mild attachment loss with 1 mm recession on teeth Nos. 19 through 21 and less than 2 mm of horizontal bone loss (Figure 4). The periodontal diagnosis was American Academy of Periodontology (AAP) stage 1, grade A.5
Risk: Low
Prognosis: Good
Biomechanical: The patient presented with no active caries. There were defective amalgam restorations on teeth Nos. 2, 15, and 18, a missing onlay on tooth No. 19, and tooth No. 31 had fractured off both lingual cusps below the gingival margin. In addition, teeth Nos. 19, 30, and 31 had structural compromises, with tooth No. 31 having a crown margin location issue. Teeth Nos. 6 through 11 and 22 through 27 had a poor prognosis due to severe attrition and areas of erosion. If left untreated, teeth Nos. 19 and 31 would have a hopeless prognosis.
Risk: Moderate
Prognosis: Poor
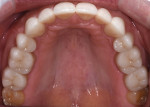
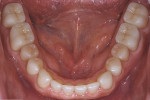
Functional: Moderate attrition of 1 mm to 2 mm was present on teeth Nos. 1 through 4, 13 through 16, 18 through 21, and 28 through 31, and severe attrition-more than 2 mm-was present on teeth Nos. 6 through 11 and 22 through 27. Attrition was most evident on the palatal surfaces of the maxillary anterior teeth and labial surfaces of the mandibular anterior teeth (Figure 5 and Figure 6). This suggested an adaptive-mediated CCP.6-8 The patient reported that he felt he had to push his jaw back in order to get his posterior teeth to touch and that his mandibular anterior teeth hit the back of his maxillary anterior teeth; he also said he often placed his tongue between his teeth. The positive answers on his dental history and his attrition pattern confirmed the diagnosis of a CCP.
Risk: Moderate
Prognosis: Poor
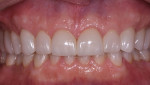
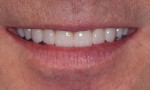
Dentofacial: Photographic documentation revealed considerable gingival display, undersized teeth, a slight diastema between the central incisors, and a deficient buccal corridor (Figure 7). Chairside smile evaluation included assessment of both a "normal" smile and a Duchenne smile, in which maximum lip dynamics occur to create a full smile.9 The patient demonstrated high lip dynamics, which made these esthetic shortcomings even more obvious. As a public speaker, the patient considered these characteristics debilitating and throughout the diagnosis continued to express his strong desire for his teeth to appear larger and whiter and to have a less "gummy" smile.
Risk: High
Prognosis: Hopeless
Treatment Goals
The patient's smile left him feeling self-conscious when speaking in front of people. With the exception of orthodontics, he was willing to do whatever treatment was necessary to achieve an attractive smile. The treatment plan was designed to create a pleasing esthetic outcome, treat the CCP, and establish bilateral simultaneous posterior tooth contact. This would involve clinical crown lengthening for the maxillary anterior teeth and opening the vertical dimension10 using a combination of direct and indirect restorations in order to achieve the functional and esthetic goals without significantly raising the biomechanical risk.
Treatment Plan
Phase 1: Pre-treatment-Deprogram, Wax-Up, and Consult
The patient wore a Kois deprogrammer for 3 weeks to determine the reference condylar position and centric relation (CR) and confirm the initial diagnosis of CCP; the orthopedic mandibular position moved anteriorly during deprogramming. A bite registration was taken in CR, and a Kois dentofacial analyzer was used to articulate the casts on a Panadent articulator (Panadent, panadent.com). A diagnostic wax-up was then fabricated using the aforementioned 10-step diagnostic approach. Maxillary and mandibular incisal positions were determined to establish vertical dimension. Bilateral simultaneous centric contacts were established on the posterior teeth. The envelope of function was "flattened" by increasing the OVD. This was intended to relieve the CCP, reduce the overbite, and allow for more ideal tooth proportions.
Polyvinylsiloxane (PVS) putty matrices of both arch wax-ups were fabricated. A consult was then scheduled with the patient to present the proposed treatment plan, which would include referral to a periodontist for clinical crown lengthening of teeth Nos. 6 through 11 and 23 through 26, bleaching teeth Nos. 20 through 29 during the crown-lengthening healing period, and restorative treatment as follows: teeth Nos. 2 through 4 and 13 through 15, minimally prepared AVOs; teeth Nos. 6 through 11, 18, 19, 30, and 31, full-coverage crowns; and teeth Nos. 20 through 29, direct composite bonding.
During the consult the wax-up was tried in using provisional material (Luxatemp®, DMG America, dmg-america.com) and PVS matrices.11 Upon seeing the mock-up in his mouth and his potential new smile, the patient was thrilled and immediately accepted treatment (Figure 8).
Phase 2: Clinical Crown Lengthening and Bleaching
With the temporary stints (Luxatemp) being used as a surgical guide, the patient had clinical crown lengthening (approximately 1 mm) done in the periodontist's office. This procedure was necessary to achieve a less "gummy" smile and more ideal tooth proportions. A 3-month healing period followed during which the patient was able to use a custom tray to bleach teeth Nos. 20 through 29. The final shade of these natural teeth was then used as a guide for both the direct and indirect restorations.
Phase 3: Tooth Preparation and Provisionalization
The patient returned to the office to begin the restorative phase. Teeth that were to receive indirect restorations were prepared, direct composite was bonded to the mandibular teeth, and provisional restorations were fabricated from the PVS matrices. The minimally prepared AVOs required no interproximal reduction and were left mostly in enamel. These ultraconservative restorations were vital to this case as they helped enable the structural integrity of the teeth to be retained,12 facilitated opening the OVD, and filled out the buccal corridor (Figure 9) to allow the patient to have the broad, full smile he envisioned.
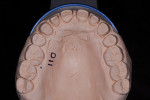
With financial considerations in mind, and in an effort to remove as little tooth structure as possible, the decision had been made to bond direct composite on teeth Nos. 20 through 29 (Figure 10). When placed with the proper protocol and attention to detail, direct composite bonding constitutes a predictable long-term restoration.13 Putty matrices were used to transfer the precise anatomy and occlusion of the diagnostic wax-up to the mouth.
The patient returned a week later to evaluate his provisional restorations for chewing, speech, and joint comfort, all of which were deemed to be appropriate. New photographs were taken to confirm the esthetics and to see if any adjustments to the final restorations would be needed during fabrication. In order to capture an occlusal record as close to the final OVD as possible a small deprogrammer was bonded to the palatal surface of the provisional restorations between the maxillary central incisors, slightly separating (0.5 mm) the posterior teeth. After removal of the posterior provisional restorations, the record was taken using a PVS bite material (Regisil® Rigid, Dentsply Sirona, dentsplysirona.com). Study models were made of the provisional restorations with a new Kois dentofacial analyzer registration to transfer the information to the dental laboratory.
Phase 4: Fabrication and Seating of Indirect Restorations
PVS impressions (Aquasil Ultra Smart Wetting® Impression Material, Dentsply Sirona) of the patient's prepared teeth and provisional restorations were poured in a type IV die stone and scanned with a digital scanner, and the restorations were virtually designed. The designs were then milled in either zirconia (anterior) or lithium disilicate (posterior) and verified using dies, articulated working casts, and solid models for complete seating (fit), occlusion, and proximal contacts. The anterior crowns were microlayered on the facials to replicate the natural dentition, while the posterior crowns were completed as monolithic prostheses to maintain the structural integrity of the material. The intaglio surfaces were prepared for delivery according to the manufacturer's recommendations (Figure 11).
The maxillary restorations were fabricated and seated first (Figure 12). The anterior full-coverage crowns were fabricated in zirconia to keep the palatal surface as thin as possible, thereby requiring less tooth reduction (Figure 13 and Figure 14). The crowns were seated cohesively using a self-adhesive resin cement (RelyX™ Unicem 2, 3M Oral Care, 3m.com). Next, the posterior lithium-disilicate (e.max®, Ivoclar Vivadent, ivoclarvivadent.com) AVOs were seated using an adhesive bonding protocol (All-Bond® 2, Bisco, bisco.com; Variolink® II Esthetic Cementation System, Ivoclar Vivadent). Finally, a new PVS impression was made of the mandibular preparations and a bite registration was taken of the completed maxillary arch relationship to the mandibular preparations utilizing a 3D-printed Kois deprogrammer (Figure 15).14
The patient returned several weeks later for seating of the mandibular molar crowns (Figure 16). These lithium-disilicate full-coverage restorations were seated using cohesive protocols. The printed deprogrammer was used to adjust the occlusion into bilateral simultaneous posterior contact.14 The patient requested that a nightguard be fabricated because he had always worn one and believed it would protect his investment; therefore, impressions were taken for production of a maxillary nightguard, which was seated at a follow-up appointment.
The final outcome is shown in Figure 17 and Figure 18.
Discussion
In the initial consultation, it was clear that the patient viewed his smile as a disability.2 After considering the outcome, which was achieved without significant structural compromise to the restored teeth, it was apparent that orthodontics may not have improved the result.
The final restorations added both cervical and incisal length to the maxillary incisors to improve esthetics. Clinical crown lengthening provided the apical tooth length required, as the patient's periodontal risk was classified as low. With the incisal edges needing additional length, orthodontic intrusion was determined to offer no benefit to the tooth reduction required.
The maxillary anterior teeth demanded cohesively retained ceramic restorations because of the exposed palatal dentin. Orthodontic tooth movement to relieve a CCP requires, in part, that the maxillary incisors be rotated out of the path of the chewing envelope. In this case that would have resulted in unnecessary facial tooth reduction. Without orthodontic treatment, space for restorative materials on the maxillary incisors was managed by increasing tooth length, increasing OVD, and the choice of restorative materials, thus protecting the structural integrity of the teeth through the preparation design.
A negative curve in the patient's maxillary anterior-posterior occlusal plane provided sufficient inter-occlusal space for restorative materials with a change in the OVD. To satisfy the patient's esthetic demands for visible tooth display, minimal axial reduction was necessary because of the additive capability of the AVOs.
Some discussion of the AVOs is warranted. The clinical rationale and utilization of these restorations is multifaceted. Adding volume to the buccal surfaces of the posterior teeth (veneering) allowed for larger, more proportionate teeth, broadened the patient's smile, and filled out the buccal corridor. Adding to the occlusal surfaces of the posterior teeth (onlaying) allowed for opening of the OVD. Predictably opening vertical dimension restoratively, without increasing biomechanical risk, is a relatively recent capability. With the advent and continuing success of lithium disilicate clinicians can reduce occlusal posterior surfaces minimally, preparing mostly in enamel.11 The AVO can be relatively thin, much like a veneer, and cover all posterior cusps, similar to an onlay. Lithium-disilicate restorations calibrated for increased OVD are adhesively applied to tooth structure (mostly in enamel) via silane coupling of the restorations and adhesive resin protocols.
Conclusion
This treatment was successful in altering the visible tooth display in the patient's smile and the size and proportion of his teeth while minimizing the chances of anticipated long-term complications. Since this case was completed, the patient has had two 6-month recall appointments without reported complications. The patient's needs were met in that the smile he desired was achieved without increasing the risks for predictable negative events to his dentition.
The patient has since shared with the author that his new smile has changed his professional outlook and self image, stating how much he appreciates "the power of a simple smile" and feeling much better and more confident about his appearance. As a clinician, nothing is more rewarding than providing treatment that is life changing.
Acknowledgment
The authors thank John Kois, DMD, MSD, for providing the structure and fundamental protocols to create the vision necessary to treat this case successfully. They also thank periodontist Will Fernyhough, DDS, MSD, for providing the clinical crown-lengthening procedure, and Protea Dental Studio for the indirect restorations.
About the Authors
Kris Swanson, DDS
Mentor, Kois Center, Seattle, Washington; Private Practice, Bellevue, Washington
Leon Hermanides, CDT
Clinical Instructor and Scientific Advisor, Kois Center, Seattle, Washington; Founder, Protea Dental Studio, Redmond, Washington
References
1. Zarone F, Di Mauro MI, Ausiello P, et al. Current status on lithium disilicate and zirconia: a narrative review. BMC Oral Health. 2019;19(1):134.
2. Baiju RM, Peter E, Varghese NO, Sivaram R. Oral health and quality of life: current concepts. J Clin Diagn Res. 2017;11(6):ZE21-ZE26.
3. Kois JC. New challenges in treatment planning-part 1. Shifting the paradigm toward risk assessment and perceived value. J Cosmet Dent. 2010;26(4):62-69.
4. Kois JC. New challenges in treatment planning-part 2. Incorporating the fundamentals of patient risk assessment. J Cosmet Dent. 2011;27(1):110-121.
5. Tonetti MS, Greenwell H, Kornman KS. Staging and grading of periodontitis: framework and proposal of a new classification and case definition. J Periodontol. 2018;89 suppl 1:S159-S172.
6. Kois JC. Functional Occlusion: Science Driven Management Manual. Seattle, WA: Kois Center; January 2011:79.
7. Van't Spijker A, Kreulen CM, Bronkhorst EM, Creugers NH. Occlusal wear and occlusal condition in a convenience sample of young adults. J Dent. 2015;43(1):72-77.
8. Schierz O, Dommel S, Hirsch C, Reissmann DR. Occlusal tooth wear in the general population of Germany: effects of age, sex, and location of teeth. J Prosthet Dent. 2014;112(3):465-471.
9. Duchenne de Boulogne G B. The Mechanism of Human Facial Expression. Cambridge, UK: Cambridge University Press; 1990.
10. Kois JC, Phillips KM. Occlusal vertical dimension: alteration concerns. Compend Contin Educ Dent. 1997;18(12):1169-1177.
11. Kois DE, Schmidt KK, Raigrodski AJ. Esthetic templates for complex restorative cases: rationale and management. J Esthet Restor Dent. 2008;20(4):239-250.
12. Kois DE, Chaiyabutr Y, Kois JC. Comparison of load-fatigue performance of posterior ceramic onlay restorations under different preparation designs. Compend Contin Educ Dent. 2012;33(spec no 2):2-9.
13. Swanson KK. Predictable, conservative closure of black triangles. Inside Dentistry. 2018;14(12):32-38.
14. Hermanides L, Larson K. Maxillary esthetics, mandibular function: a rationale for predictable treatment of the moderately worn dentition. Compend Contin Educ Dent. 2014;35(8):583-587.