Technique Using a Novel Verification Guide for Complete Seating of Open-Tray Impression Copings
Agnetha Valladares, DDS; Alessandro Grisa, DDS; Sang-Choon Cho, DDS; and Stuart J. Froum, DDS
Abstract: The purpose of impression-taking is to attain the accurate transfer of intraoral information for extraoral use. It is a crucial step in performing a successful dental implant restorative procedure. To accurately replicate the implant position for adaptation of an abutment that will completely engage with the implant, a pick-up impression is taken with an impression coping. Several factors can affect seating of the impression coping, including soft-tissue interference, the size of the impression coping, angulation, proximity or contact with adjacent teeth, damage to the coping, misfit caused by use of other manufacturers’ parts, and differences between seating in an external- versus internal-connection implant. This article presents use of a novel verification guide that is intended to ensure complete seating of the impression coping with the implant.
Successful dental implant restorative procedure begins with the accurate transfer of intraoral information for extraoral use, which is achieved through impression-taking. Typically, impressions are done using one of several techniques: pick-up, whereby the guide pin is untightened prior to removing the impression tray via an access window in the tray, and the impression coping is subsequently retained in the impression; or transfer, in which the coping is transferred from the mouth to the impression with the impression analog.1 Studies have shown that the pick-up impression technique is more accurate than the transfer technique.1-5 Alternatively, a third technique is to take a digital impression with an intraoral scanner, whereby a scan abutment is used instead of an impression coping to create a digital model.
To accurately replicate the implant position for adaptation of an abutment that will completely engage with the implant, a pick-up impression may be taken with an impression coping. This registers the position of the implant or abutment in the impression, with a guide pin securing the coping initially to the implant during the impression-taking procedure and later to the implant replica in the master cast. Once seated, the impression coping and guide pin must be verified with a radiograph to confirm the coping has fully engaged with the implant.
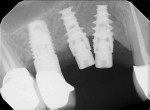
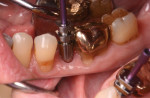
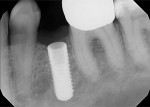
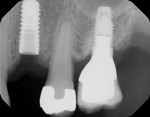
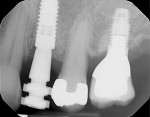
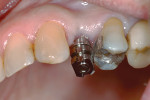
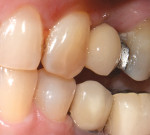
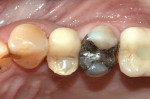
Several factors can affect the seating of the impression coping and prevent it from fully engaging with the implant. These include soft-tissue interference, the impression coping size, angulation (Figure 1), proximity or contact with adjacent teeth (Figure 2 and Figure 3), damage to the coping, misfit caused by use of parts from other manufacturers, and differences between seating in an external- versus internal-connection implant.
The purpose of this article is to present a novel verification guide that is intended to ensure complete seating of the impression coping with the implant without the need for confirmation with a radiograph. The article will describe the steps necessary in using the verification guide as well as other benefits of the guide, which is aimed at overcoming some of the limitations of other current guides. These limitations, too, will be discussed.
Verification Guide and Its Clinical Application
The novel verification guide is a device that can be placed intraorally with the impression coping to verify complete seating with an audible and tactile click. It may be used for both maxillary and mandibular implants when taking an open-tray impression. The advantages of the guide are that it allows seating of the coping to be verified without the need for radiographic confirmation, it enables errors that may be due to poor angulation of radiographs to be avoided, and it allows for easier verification of malposed implants or implants in the second and third molar region. The novel verification guide is shown in Figure 4 in comparison to a conventional guide pin, and its intended usage is depicted with a laboratory analog in Figure 5. A description of how to use the novel verification guide is presented below. A clinical example of its use is illustrated in Figure 6 through Figure 10.
The clinical application of the verification guide may be summarized in four steps. First, an assessment of the soft tissue surrounding the healing abutment is made to evaluate whether there is an adequate band of keratinized tissue. A minimum of 2 mm thickness is required in preparation for an impression to fabricate the prosthesis. If less than 2 mm of keratinized tissue is present a soft-tissue connective graft may be needed prior to impression-taking. Next, the healing abutment is removed, and the impression coping is seated by hand without the use of the guide pin. The verification guide is then seated into the coping; a click with both audible and tactile sensations confirms that the impression coping has been accurately seated. Thus, the need for a radiograph to confirm the seating is eliminated, although an example is shown for demonstrative purposes (Figure 7 and Figure 8).
The verification guide is then removed while the impression coping is held firmly in the verified position, and the guide is replaced with the guide pin, which is then tightened to secure the coping to the implant (Figure 5, lower right). Lastly, the clinician then proceeds to take the impression via an open-tray techniquefor fabrication and subsequent delivery of a final prosthesis (Figure 9 and Figure 10).
Discussion
No data is available regarding modifications to improve seating of the impression coping, as the literature focuses more on overall impression accuracy with regard to impression materials, comparisons between pick-up and transfer techniques, and impression copings.1,3 Conventional guide pin design consists of a threaded tip that engages with the implant, a long narrow body that is unthreaded to enable ease of removal through the impression material, and a screw head that can be untightened before removal of the impression from the mouth. The screwdriver connection of the guide pin, therefore, is limited to being in a vertical direction. Thus, to verify that the guide pin and impression coping have fully engaged with the internal implant structure, a radiograph must be taken. Poorly angled radiographs may indicate an accurate seating when, in fact, one does not exist and thereby lead to a poorly fitting crown.6
Rashidan and colleagues found that the impression-coping shape affected impression accuracy more than the material or technique used.1 The more retentive the features of the coping and the straighter the design, as opposed to a tapered design, the less distortion and drag occurred within the material. Limitations of this study were that all copings were placed parallel to each other and the impression was removed in a direction perpendicular to the occlusal plane, hence implant position was not a variable.
A systematic review by Moreira et al examined implant systems that use copings with tactile sensation, which depend greatly on clinical experience and expertise as to whether they have been correctly seated.2 Compared with metal copings, plastic impression copings resulted in less accuracy, poorer fit, and greater angular displacement.
Jung and Bashutski adjusted the guide pin design to improve its access for open-tray impressions.3 The method proposed used the shaft of a cotton swab to engage with the head of the pin to extend the guide pin's length and provide easier access through the impression material and open-tray window. For guide pins with a flat head used in cross-section, to engage a screwdriver a hollow plastic tube can be fashioned over the pin head to achieve the same purpose.
Nicoll and coinvestigators assessed the precision fit between impression copings and implant replicas in vertical, horizontal, and rotational positions using external hexagon, internal trilobe, and internal conical connections.4 They found that precision of the vertical fit was dependent on the joint type and the tightening force applied to the guide pin, and that changes to the angular position of the impression coping had repercussions in subsequent prosthesis fabrication, such as inaccuracies in seating the prosthesis.
Papaspyridakos et al conducted a systematic review comparing three impression techniques: pick-up, transfer, and digital.5 They found that the pick-up technique was the most accurate for complete edentulous cases; however, for partially edentulous cases they reported no difference between the pick-up and transfer impression techniques. They concluded that further research is necessary to assess the accuracy of digital impression techniques.
In a case report, Mahoorkar and colleagues described a technique that simply utilizes the implant mount to take the impression rather than an impression coping via a transfer impression technique.7 The connection of their modified implant mount is comparable to the verification guide presented herein in that it is a press fit connection with the implant. Their use of the modified implant mount as an alternative to an impression coping, however, limits the option of impression technique to only the transfer technique, and therefore accuracy of the impression becomes a risk in cases of multiple implants.8
Use of the novel verification guide can reduce the number of radiographs needed for an impression-taking procedure. The guide can also be used in situations with soft-tissue interferences, deeply placed implants, and adjacent teeth that may restrict accurate seating of the coping. Examples of such situations include cases of implant angulation or multi-implant cases where implants are too close or converging (Figure 1) or where there may be limited interproximal space (Figure 2 and Figure 3). These complications may be overcome with the aid of the novel verification guide.
The verification guide may also benefit patients with limited mouth opening and sensitive gag reflexeswho consequently have difficulty tolerating intraoral radiographs needed for verification.9-11 The audible and tactile click sensation of the guide that occurs upon seating allows reproducibility and lets the clinician know that the impression coping has been seated completely. The authors are not aware of any comparable devices to verify seating of an impression coping.
At present the verification guide described herein is still a prototype and is not yet available commercially.The design of the guide requires further development. Specifically, the platform of the guide needs to be made flush with the platform of the coping. Furthermore, retrieval of the guide currently relies on the aid of mosquito forceps and a more user-friendly means of retrieving the guide from the coping once seating is verified, such as a longer handle that is easier to grip by hand, would be beneficial.
Conclusion
The novel verification guide has applications in clinical practice to improve impression accuracy, and thereby the accuracy of the final prosthesis, by ensuring correct seating of the impression coping. There are also benefits to reducing the number of radiographs required per procedure, particularly in full-arch restorative cases, such as minimizing patient radiation exposure and eliminating associated radiographical errors that may affect accuracy. Additional benefits may be realized for patients with limited mouth opening and sensitive gag reflexes, and to overcome situations where implant depth, proximity, angulation, and soft-tissue interferences are issues. Evaluation of the guide in various clinical scenarios and comparison of its use with other implant systems is needed before it may be recommended for general use.
Disclosure
The authors have no relevant or material financial interests related to the research described in this article.
About the Authors
Agnetha Valladares, DDS
Implant Resident, Department of Periodontology and Implant Dentistry, New York University College of Dentistry, New York, New York
Alessandro Grisa, DDS
Implant Fellow, Department of Periodontology and Implant Dentistry, New York University College of Dentistry, New York, New York
Sang-Choon Cho, DDS
Clinical Assistant Professor, Department of Periodontology and Implant Dentistry, New York University College of Dentistry, New York, New York
Stuart J. Froum, DDS
Clinical Adjunct Professor and Director of Clinical Research, Department of Periodontology and Implant Dentistry, New York University College of Dentistry, New York, New York; Private Practice, New York, New York
References
1. Rashidan N, Alikhasi M, Samadizadeh S, et al. Accuracy of implant impressions with different impression coping types and shapes. Clin Implant Dent Relat Res. 2012;14(2):218-225.
2. Moreira AH, Rodrigues NF, Pinho A, et al. Accuracy comparison of implant impression techniques: a systematic review. Clin Implant Dent Relat Res. 2015;17(suppl 2):e751-e764.
3. Jung SR, Bashutski JD. Method to simplify a direct implant impression using an extended guide pin. J Prosthet Dent. 2010;104(2):137-138.
4. Nicoll RJ, Sun A, Haney S, Turkyilmaz I. Precision of fit between implant impression coping and implant replica pairs for three implant systems. J Prosthet Dent. 2013;109(1):37-43.
5. Papaspyridakos P, Chen CJ, Gallucci GO, et al. Accuracy of implant impressions for partially and completely edentulous patients: a systematic review. Int J Oral Maxillofac Implants. 2014;29(4):836-845.
6. Goll GE. Production of accurately fitting full-arch implant frameworks: Part I-clinical procedures. J Prosthet Dent. 1991;66(3):377-384.
7. Mahoorkar S, Jain A, Cauvery K, et al. Modification of fixture mount to be used as an impression coping in closely placed implants. J Clin Diagn Res. 2014;8(4):ZD8-ZD10.
8. Sabouhi M, Bajoghli F, Dakhilalian M, et al. Effects of impression coping design, impression technique, and dental undercuts on the accuracy of implant impressions assessed by 3-dimensional optical scanning: an in vitro study. Implant Dent. 2016;25(2):238-246.
9. Sheridan P, Koka S. Complete seating of an implant impression coping. J Prosthet Dent. 1995;73(3):322-324.
10. Linkevicius T, Svediene O, Vindasiute E, et al. The influence of implant placement depth and impression material on the stability of an open tray impression coping. J Prosthet Dent. 2012;108(4):238-243.
11. Raviv E, Hanna J, Raviv R, Harel-Raviv M. A clinical report on the use of closed-tray, hex-lock-friction-fit implant impression copings. J Oral Implantol. 2014;40(4):449-453.