A Novel, Minimally Invasive Approach to Replacing Missing Teeth: Two Case Reports
Wendy Auclair Clark, DDS, MS; Alexandra B. Yarborough, DDS; David A. Garber, DMD; and Craig J. Holland
Abstract: For the replacement of missing teeth, resin-bonded fixed partial dentures (RBFPDs) are a routine, minimally invasive option clinicians can use on patients who either cannot or will not move forward with surgical interventions. Advances in materials and design have greatly improved the longevity and prognoses for these prostheses. In some patients, however, debonding remains a clinical problem. In this clinical report, novel RBFPD designs are presented with the aim of improving retention and esthetics while offering short treatment time and minimal preparation without the need for local anesthesia.
Replacing missing single teeth is common in clinical practice, whether the edentulous space is due to congenital reasons or a tooth extraction. When considering nonremovable tooth replacement options, implant-supported crowns (ISCs), traditional fixed partial dentures (FPDs), and resin-bonded fixed partial dentures (RBFPDs) are typically among the choices included. Numerous factors must be considered in treatment planning, including cost, longevity, and the extent of treatment.1,2 For example, ISCs and traditional FPDs are usually deemed a more long-term solution. However, one must consider that ISCs require at least one surgical visit, and the complications associated with FPDs often are more extensive than those associated with RBFPDs. These complications may include recurrent caries and the need for endodontic treatment, whereas the most notable complications associated with RBFPDs are debonding and prosthesis fracture.2-5 With these factors in mind, RBFPDs may be considered a viable tooth replacement option for certain patients.
Advances in zirconia and bonding protocols have greatly changed the nature and application of RBFPDs since Rochette first described them decades ago.6-11 This is particularly true in the area of esthetics, where the most common complication of significance, aside from debonding, has been discoloration of the teeth due to the presence of metal wings.3,12 In the past few decades, considerable improvement has been made in the long-term prognosis for all complications with RBFPDs.13 However, this success is dependent on preparation design and case selection. This includes mechanical retention in the preparation as well as a single-retainer design. When the recommended preparation is followed in an ideal case, the literature reports success rates of 95% or higher.14 When considering all cases, a 2013 meta-analysis found success rates as low as 72.5% for all-ceramic restorations at 3 years.15
Contraindications for RBFPDs include limited interocclusal space, parafunctional habits, and short clinical crowns. Additionally, esthetic contraindications include highly translucent teeth and interdental spaces that may allow the wings to be visible. There are times, however, when a patient may fall into one or more of these categories that offer a decreased prognosis, yet is not a candidate for dental implants. The purpose of this clinical report is to describe a novel way to decrease the likelihood of debonding and esthetic complications of an RBFPD in less-than-ideal cases through the use of a unilateral approach with a "c-wing" design.
Clinical Report
Case 1
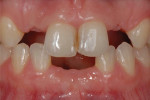
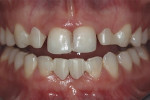
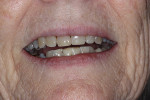
A 25-year-old female patient presented to a private practice with congenitally missing maxillary lateral incisors and mandibular central incisors (Figure 1). She had not previously sought tooth replacement, because she had only been aware of fixed replacement options that involved surgery or significant tooth preparation. Although physically healthy, the patient was adamant about avoiding surgery, removable prosthetics, and what she considered to be invasive treatment options. She had extensive interdental edentulous spacing on both arches, as well as limited bonding surface on the lingual of the maxillary canines, making her a less-than-ideal candidate for RBFPDs.
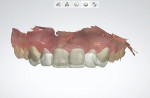
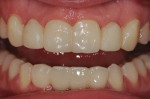
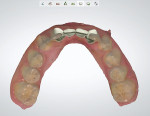
Because the edentulous spaces were disproportionately large and the adjacent teeth were relatively small, redistribution of the space with restorative material was proposed. To confirm this plan, a digital smile design and subsequent trial smile were completed. An intraoral scan was taken, and the smile design was performed with smile design software (3Shape Dental System, 3Shape, 3shape.com) (Figure 2). The design was then milled in polymethyl methacrylate (PMMA), allowing the trial smile to fit over the patient's unprepared teeth (Figure 3). This let the patient see an attainable result with minimal preparation while enabling the clinician and laboratory technician to realistically evaluate the space distribution.
Once it was determined that restorative space was adequate and the proposed tooth proportions were acceptable, the design was finalized. In addition to the standard single lingual retainer wing, a buccal extension was added to the zirconia frameworks (Figure 4), in a "c-wing" design. The frameworks were milled in zirconia and tried in to confirm fit and retention (Figure 5). Following the approved smile design, individual lithium-disilicate veneers(IPS e.max® CAD, Ivoclar Vivadent, ivoclarvivadent.com)were then pressed to fit retainer teeth, adjacent teeth, and prepared pontics on the framework (Figure 6).
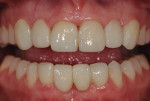
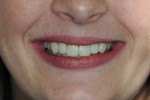
After try-in and patient approval, the zirconia frameworks (IPS e.max® ZirCAD, Ivoclar Vivadent) were treated and bonded per manufacturer's instructions and excess cement was cleaned. The veneers were then treated and bonded with a dual-cure resin cement (Variolink® Esthetic, Ivoclar Vivadent) per manufacturer's instructions (Figure 7). At follow-up, the occlusion was verified, and the patient's home care was evaluated.
At 24 months post-delivery, the patient was experiencing no discomfort and the prostheses were stable. She has remained very satisfied with the outcome.
Case 2
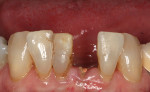
A 77-year-old female patient presented to a private practice as an emergency with her endodontically treated lower right central incisor fractured at the gumline (Figure 8). Her primary objective was to find a long-term fixed prosthetic solution. She was at a relatively high risk for implant failure, as her medical history included a diagnosis of osteopenia and bisphosphonate use. Combined with her narrow ridge width, a treatment option that minimized surgery was chosen.
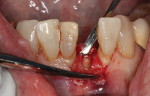
After discussing treatment options, root submergence and a minimal-preparation cantilever FPD was chosen as the most conservative approach. The surgical treatment included reducing the fractured tooth structure to a slightly subcrestal position using a coarse diamond bur (Figure 9) and subsequently obtaining primary soft-tissue closure.
Upon review of the risks, benefits, and costs of treatment, the patient was concerned about the possibility of debonding, because she often traveled for several months at a time. There were also esthetic concerns with the proposed retainer tooth (lower left central incisor) and apprehension regarding the adequacy of restorative space. Additionally, the proposed retainer tooth was short with mottled enamel, making long-term bonding unpredictable. As such, facial coverage of the retainer tooth with restorative material was proposed to improve esthetics and decrease the potential for debonding. To confirm clearance and esthetics, and following the same protocol as the previous case, a digital smile design and subsequent trial smile were completed. After clinician and patient approval, the design was finalized.
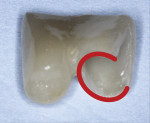
The esthetic goal for this case was not as extensive as in the previous case, therefore a design modification was proposed. The entire case was designed in monolithic zirconia, and the buccal wing was extended to function as a veneer (Figure 10 and Figure 11). This satisfied the patient's esthetic concerns while improving retention.
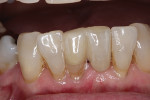
After try-in and patient approval, the zirconia restorations were treated with silane and bonded with a dual-cure resin cement (Panavia™ V5, Kuraray America Inc., kuraraydental.com) per manufacturer's instructions, and excess cement was cleaned (Figure 12). At 12 months post-delivery, the prosthesis and tissue levels were stable. New impressions for a retainer were made and the composite resin restoration on the adjacent tooth was refinished (Figure 13). At time of publication, the prosthesis has been in service for 2.5 years. Clinical evaluation revealed no functional or biologic complications.
Discussion
Although the designs in both cases deviated from the standard, the RBFPDs were fabricated with a single retainer. This was in accordance with literature that indicates a more favorable prognosis for a single-retainer (cantilevered) RBFPD versus a fixed-fixed two-wing RBFPD.2,7,8,16-19 Zirconia was chosen as the framework material due to its esthetic properties, as well as its physical properties. Literature indicates that it may be a suitable alternative to metal for RBFPDs2,20,21 and that a relatively predictable bond can be attained.7,10,11
This design was proposed as a modification of the Encore® bridge (trademark of Jeneric/Pentron, pentron.com). The Encore bridge is a RBFPD with a resin framework that achieves additional mechanical retention and improved esthetics with porcelain veneers on the pontic and adjacent teeth, because there is a dual path of insertion between the framework and the overlaying veneers.22
A recent report by Mourshed et al reviewed the literature regarding anterior cantilever RBFPDs and suggested that cantilever RBFPDs had better survival than two-retainer RBFPDs.23 Their report agrees with a 2016 systematic review and meta-analysis study by Wei et al.24 The use of unilateral RBFPDs shows promising results and high survival rates. The use of zirconia ceramic and phosphate monomers containing resin cements was also suggested, as this helped to minimize the debonding rate and/or fracture of anterior all-ceramic cantilever RBFPDs.
The primary advantage of the treatments presented in this report is that while neither patient was an ideal candidate for a conventional RBFPD, an alternative minimally invasive option was completed. The veneers and RBFPD both required minimal preparation, and the patients' goals were achieved. These goals included short treatment time, minimal preparation, and no administration of local anesthesia. In addition, the "c-wing" design and the material choices should address the two most common complications with RBFPDs: debonding and discoloration. In a unilateral approach, the pontic will move with the abutment tooth during function, which can prevent shear and torque forces that result when splinting to the adjacent teeth bilaterally.
There are a few notable disadvantages of this technique. The long-term success depends primarily on the bond of zirconia to enamel, which, albeit promising, still requires further evidence. Additionally, execution of this prosthesis demands excellent communication between the clinician and laboratory technician. Fortunately, this is now easier to accomplish with CAD/CAM technology, which was utilized in both of these cases. Lastly, the "c-wing" design is an untested RBFPD design, with short follow-ups to this point. Additional cases, larger in vitro studies, and a longer follow-up are indicated to consider this a proof-of-concept rather than a clinical report.
Summary
Two clinical reports were presented to describe restorative solutions for patients who desire minimal interventions with short treatment times. To manage edentulous spaces, minimal-preparation RBFPDs and veneers were designed and fabricated using CAD/CAM technology for improved communication and predictability. A novel "c-wing" design was utilized to improve mechanical retention and esthetic results for patients who are not ideal candidates for RBFPDs but still desire a nonsurgical approach.
About the Authors
Wendy Auclair Clark, DDS, MS
Assistant Professor, Department of Prosthodontics, University of North Carolina at Chapel Hill, Chapel Hill, North Carolina
Alexandra B. Yarborough, DDS
Assistant Professor, Department of Prosthodontics, University of North Carolina at Chapel Hill, Chapel Hill, North Carolina; Fellow, American College of Prosthodontists
David A. Garber, DMD
Private Practice, Atlanta, Georgia
Craig J. Holland
Owner, 3 Point Dental Studio, Fremont, Ohio
References
1. Antonarakis GS, Prevezanos P, Gavric J, Christou P. Agenesis of maxillary lateral incisor and tooth replacement: cost-effectiveness of different treatment alternatives. Int J Prosthodont. 2014;27(3):257-263.
2. Thoma DS, Sailer I, Ioannidis A, et al. A systematic review of the survival and complication rates of resin-bonded fixed dental prostheses after a mean observation period of at least 5 years. Clin Oral Implants Res. 2017;28(11):1421-1432.
3. Goodacre CJ, Bernal G, Rungcharassaeng K, Kan JY. Clinical complications in fixed prosthodontics. J Prosthet Dent. 2003;90(1):31-41.
4. Goodacre CJ, Bernal G, Rungcharassaeng K, Kan JY. Clinical complications with implants and implant prostheses. J Prosthet Dent. 2003;90(2):121-132.
5. Pjetursson BE, Tan WC, Tan K, et al. A systematic review of the survival and complication rates of resin-bonded bridges after an observation period of at least 5 years. Clin Oral Implants Res. 2008;19(2):131-141.
6. Rochette AL. Attachment of a splint to enamel of lower anterior teeth. J Prosthet Dent. 1973;30(4 Pt 1):418-423.
7. Sasse M, Eschbach S, Kern M. Randomized clinical trial on single retainer all-ceramic resin-bonded fixed partial dentures: influence of the bonding system after up to 55 months. J Dent. 2012;40(9):783-786.
8. Kern M. Clinical long-term survival of two-retainer and single-retainer all-ceramic resin-bonded fixed partial dentures. Quintessence Int. 2005;36(2):141-147.
9. Bottino MA, Valandro LF, Scotti R, Buso L. Effect of surface treatments on the resin bond to zirconium-based ceramic. Int J Prosthodont. 2005;18(1):60-65.
10. Attia A, Kern M. Long-term resin bonding to zirconia ceramic with a new universal primer. J Prosthet Dent. 2011;106(5):319-327.
11. Komine F, Blatz MB, Matsumura H. Current status of zirconia-based fixed restorations. J Oral Sci. 2010;52(4):531-539.
12. Gilmour AS, Ali A. Clinical performance of resin-retained fixed partial dentures bonded with a chemically active luting agent. J Prosthet Dent. 1995;73(6):569-573.
13. Alraheam IA, Ngoc CN, Wiesen CA, Donovan TE. Five-year success rate of resin-bonded fixed partial dentures: a systematic review. J Esthet Restor Dent. 2019;31(1):40-50.
14. Botelho MG, Chan AW, Leung NC, Lam WY. Long-term evaluation of cantilevered versus fixed-fixed resin-bonded fixed partial dentures for missing maxillary incisors. J Dent. 2016;45:59-66.
15. Miettinen M, Millar BJ. A review of the success and failure characteristics of resin-bonded bridges. Br Dent J. 2013;215(2):E3.
16. van Dalen A, Feilzer AJ, Kleverlaan CJ. A literature review of two-unit cantilevered FPDs. Int J Prosthodont. 2004;17(3):281-284.
17. Kuijs R, van Dalen A, Roeters J, Wismeijer D. The resin-bonded fixed partial denture as the first treatment consideration to replace a missing tooth. Int J Prosthodont. 2016;29(4):337-339.
18. Koutayas SO, Kern M, Ferraresso F, Strub JR. Influence of framework design on fracture strength of mandibular anterior all-ceramic resin-bonded fixed partial dentures. Int J Prosthodont. 2002;15(3):223-229.
19. Rosentritt M, Ries S, Kolbeck C, et al. Fracture characteristics of anterior resin-bonded zirconia-fixed partial dentures. Clin Oral Investig. 2009;13(4):453-457.
20. Komine F, Tomic M. A single-retainer zirconium dioxide ceramic resin-bonded fixed partial denture for single tooth replacement: a clinical report. J Oral Sci. 2005;47(3):139-142.
21. Rosentritt M, Kolbeck C, Ries S, et al. Zirconia resin-bonded fixed partial dentures in the anterior maxilla. Quintessence Int. 2008;39(4):313-319.
22. Leal FR, Cobb DS, Denehy GE, Margeas RC. A conservative aesthetic solution for a single anterior edentulous space: case report and one-year follow-up. Pract Proced Aesthet Dent. 2001;13(8):635-641.
23. Mourshed B, Samran A, Alfagih A, et al. Anterior cantilever resin-bonded fixed dental prostheses: a review of the literature. J Prosthodont. 2018;27(3):266-275.
24. Wei YR, Wang XD, Zhang Q, et al. Clinical performance of anterior resin-bonded fixed dental prostheses with different framework designs: a systematic review and meta-analysis. J Dent. 2016;47:1-7.