Rotational Restoration Resistance and Future Possibilities for Digital Impression Technology: Literature Review and Survey Data
John F. Bowley, DDS, MS; and Wen-Fu Thomas Lai, DDS, MS, DMSc
Abstract
Digital impression procedures increasingly have been utilized to capture final impressions of fixed prosthodontic preparations in the natural tooth and single-implant restorations as well as for fixed partial dentures in both conditions. The literature related to restoration resistance to rotational displacement has been reviewed. Many digital camera systems have “open architecture” with the generation of generic standard tessellation language (STL) files. These STL files can be analyzed by software to determine preparation attribute-compliance with evidence-based standards. This literature review presents an overview of the knowledge base and survey data of US certified dental technicians (CDTs) and Canadian registered dental technicians (RDTs). The technician data reveal opinions about the level of clinician compliance with standards from the literature and possible future developments for additional applications of this emerging technology.
Fixed prosthodontics with natural tooth and implant-retained restorations have evolved considerably from the 1800s to the present day. The advent of technological advancements has produced significant changes in clinical procedures with digital impression systems, CAD/CAM-milled restorations, as well as 3D printed casts and restorations. Although not completely universal at this time, this state-of-the-arttechnology and its use by the dental profession has been growing continuously. As a result of these technological advancements, many areas of clinical periodontology, oral maxillofacial surgery, prosthodontics, and general dentistry have responded with changes in methods to accomplish clinical care. In addition to changes in clinical care methods, dental education and the dental laboratory industry have also evolved technologically.
This article will review the literature related to rotational stability of fixed restorations in five main literature categories (listed in chronological order in References1-40): (1) a classical literature review article,16 (2) a large body of literature spanning from the late 1980s to the present aimed at clinical practice,1-5,7-9,11-13,15,18-21,28,30,32,33,38,39 (3) another relatively large body of literature related to dental education,6,10,14,17,22-27,29,31,34-37 (4) recent data obtained through an anonymous survey of certified/registered dental laboratory technicians (Figure 1 through Figure 4), and, lastly, (5) a priority emphasis of federal agency funding for healthcare improvement applied to digital dentistry.40 The 40 references cover these five areas ranging from the late 1980s to the present with many citations not being reviewed; the literature prior to the 1980s was extensive and served as the foundation of fixed prosthodontics from which the present day technology has evolved.
The conformation and attributes of natural tooth preparations and implant milled abutments follow classical standards for resistance to displacement in function. One of the basic standards of the tooth/abutment is its taper of two opposing, vertical walls to form the convergence angle. A classical review of the literature has shown the ideal standard for convergence angles to be in the range of 6 degrees to 12 degreesor 3 degrees to 6 degrees per wall of two opposing, vertical walls.16 These standards were originally published by Tylman in 1930s. In addition to the convergence angle another factor is the vertical height of the tooth preparation or the implant abutment.16
This additional factor interacts with one wall of the convergence angle through its relationship to a rotational axis. The rotational axis of the restoration is located at the restoration-tooth preparation or restoration-implant abutment interface. The restoration can be viewed as rotating around this rotational axis at the tooth-restoration finish line with the opposite tapered wall providing resistance to rotational displacement. The preparation's ability to resist the rotation of the restoration around this axis is dictated by the angulation of this wall combined with the vertical height of the tooth.1-3,7,8
In general, the taller the preparation height, the greater the allowable maximum angulation of this wall will be to resist rotational displacement. The literature has utilized trigonometric and geometric formulas to calculate the maximum allowable wall taper to resist rotational displacement based on vertical wall height and distance of the rotational axis from the opposing wall.21
Provider Ability to Prepare or Assess Taper Level
The literature has demonstrated that providers are not reliable judges of preparation taper by visual inspection. Several studies have demonstrated that preclinical students are not able to prepare typodont teeth to the ideal standard.6,10,14,17,22-27,29 In addition, both faculty and predoctoral students were unable to reliably judge the preparation level when compared to a range of known tooth convergence angles. Both groups tended to generate a large number of false-positive results in underestimating the degree of taper, eg, 10-degree taper estimate in an actual 30-degree known taper. These two areas of evidence suggest a large gap between provider judgment and skill in assessing these ideal standards. In addition, the literature has determined that students as well as experienced clinicians, generally, are not able to accomplish these ideal levels of resistance form.
Digital Impression Software Analysis
CAD/CAM-milled custom screw-retained implant abutments can be milled to these rigorous standards. However, the natural tooth preparation is still prepared in the patient's mouth by a clinician, which requires very high levels of clinical skill to attain the 6-degree to 12-degree taper. Dental education has adapted software to allow the student's typodont preparation to be assessed for many attributes, including preparation taper, as students learn and build their skills in preclinical fixed prosthodontics courses.30 At least two digital impression systems have software that enable the final tooth preparation analysis compared to an ideal standard; this software facilitates the student's learning as well as objective faculty grading assessment.30,31,34-37
Some commercially available digital impression systems have software capable of a similar analysis to digital standard tessellation language (STL) files. These systems enable the clinical provider to compute the natural tooth preparation's vertical height and the convergence angle. With computer manipulations of the STL file data, the clinician can compute these two attributes; however, to improve tooth preparation attributes, this analysis would need to be accomplished during tooth preparation rather than after completion of the final impression. After computation of convergence angle, follow-up procedures are recommended to improve the degree of taper or supplement with strategically placed grooves or boxes.16
Dental Technician Survey Data
The authors conducted a survey of certified dental technicians (CDTs) and registered dental technicians (RDTs) in the United States and Canada, respectively, from September 2017 through January 2018; the survey was distributed to technicians through LinkedIn connections with an anonymous SurveyMonkey® link. The eight-question survey produced data on dental technician opinions about the quality of tooth preparation attributes and the potential need for computer software to analyze specific criteria during clinical treatment. Responses from 68 CDTs/RDTs (out of 400+ surveys sent) produced data that reflected significant deviations from "ideal" tooth preparation standards in both vertical height and taper levels; their opinions indicated 40% of tooth preparations by digital and conventional elastomeric impression methods were not up to these standards. All of the questions were designed to reveal respondents' cumulative opinions about clinical preparations submitted to their laboratory facility by clinical providers.
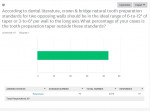
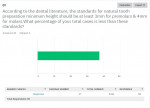
Question No. 1 (Figure 1) asked what percentage of tooth preparations were outside of the "ideal" range of convergence 6 degrees to 12 degrees, with 67 respondents saying an average of 43% were outside of this range. Question No. 2 (Figure 2) asked about the percentage of tooth preparations on premolars and molars that were more than the recommended vertical height of 3 mm and 4 mm, respectively; 68 respondents revealed that an average of 37% were outside of these standards as per the literature. In Question No. 3 (Figure 3), the technicians were asked how valuable they felt a computer software program would be for their dental provider clients to provide feedback related to adherence to evidence-based dentistry standards, ie, 6-degree to 12-degree convergence angle and 3 mm to 4 mm in vertical height. A range of responses was available to the 67 respondents, with an average of 7.5 at the "Very Valuable" level.
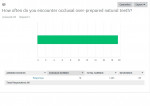
Question Nos. 4 and 5 (Figure 4 and Figure 5) asked the technicians the percentage of teeth they encounter that are under- and overprepared, respectively, in the occlusal dimension. Question No. 4 had 65 responders with average of 44%, and Question No. 5 had 66 responders with average of 19%. Question No. 6 (Figure 6) asked the technicians, based on their opinions in Questions 4 and 5, whether they felt a computer software program to analyze the tooth preparation adherence to evidence-based standards would improve the quality of care. This question was scaled from "1. Not Valuable At All" to "10. Extremely Valuable," with 65 responders averaging 8.2, "Very Valuable." Question No. 8 (Figure 7) (Note: Question No. 7 data was not used) asked the technicians if they felt that there was any merit to analyzing rotational resistance of fixed partial dentures with many abutments; 67 responders answered with an average of 7.2, "Very Valuable."
Future Software Development Opportunities
The dental profession is on the threshold of patient care levels of excellence only possible in the past by "master clinicians." Digital impression systems can generate very high-quality STL files that may be analyzed for convergence angles, surface area determinations, and possible recommendations for supplemental adjunct procedures to improve resistance form and surface area. The sequence of mid-treatment assessment with a digital impression could be done after initial tooth preparation, then corrective procedures, followed by the final digital impression. Clinical decision analysis tied to evidence-based standards from the literature has become a high priority for federal healthcare research funding published by the Agency for Healthcare Research and Quality.40
Finite element analysis (FEA) has been published in the dental literature for analysis and prediction of the effects of force, tooth, and dental materials.9,11,12,15,32 Generally, these theoretical calculations take a great deal of time due to the large amount of data generated in these models. In the near future, with increasing computer speeds and capacities, FEA may be more practical for use in clinical situations, which could enable clinicians to analyze the preparation attributes and predict how the physiological combination of tooth and materials might occur; computer-predicted results may eventually enable clinicians to predict modes of failure, etc.
Currently, some commercially available software packages associated with digital impression and CAD/CAM restoration milling procedures are available; these software packages are either add-on or system-component programs. Some can calculate convergence angles and over- or underpreparation, with some tied to the typodont-tooth confirmation in a preclinical mannequin application only. In order to coordinate evidence-based data from the literature, a program to calculate the following preparation attributes would be recommended: preparation surface area, maximal rotational resistance angle of an opposing vertical wall, two-wall convergence angles, and possible supplemental grooves or boxes with the increased surface area provided.
This type of data could be used in a "certification process" to ensure the patient, treating restorative dentist, insurance company third-party payers, professional liability legal applications, clinical board examiners, and institutional dental providers the quality of documentation within evidence-based dentistry standards from the literature. Future scenarios might see this certification process as being mandated by some of these other areas of dentistry that function as "indirect customers" or be utilized by individual providers to promote the high level of care in a practice to their patients. It is clear that this software could provide the profession with highly valuable data for decision analysis and facilitate improved clinical care in a timely manner.
About the Authors
John F. Bowley, DDS, MS
Chief, Dental Service, Department of Veterans Affairs Boston Healthcare System, Jamaica Plain, Massachusetts; Lecturer, Restorative Dentistry & Biomaterials Science, Harvard School of Dental Medicine, Boston, Massachusetts; Professor, Restorative Sciences & Biomaterials, Boston University Henry M. Goldman School of Dental Medicine, Boston, Massachusetts
Wen-Fu Thomas Lai, DDS, MS, DMSc
Professor Emeritus, Center for Nano-tissue Engineering & Imaging Research, Taipei Medical University Hospital, Taipei, Taiwan, ROC; Research Associate-Psychiatry, Brain Imaging Center McLean Hospital, Harvard Medical School, Belmont, Massachusetts
References
1. Zuckerman GR. Factors that influence the mechanical retention of the complete crown. Int J Prosthodont. 1988;1(2):196-200.
2. Zuckerman GR. Resistance form for the complete veneer crown: principles of design and analysis. Int J Prosthodont. 1988;1(3):302-307.
3. Parker MH, Gunderson RB, Gardner FM, Calverley MJ. Quantitative determination of taper adequate to provide resistance form: concept of limiting taper. J Prosthet Dent. 1988;59(3):281-288.
4. Nordlander J, Weir D, Stoffer W, Ochi S. The taper of clinical preparations for fixed prosthodontics. J Prosthet Dent. 1988;60(2):148-151.
5. Zuckerman GR. Analysis of resistance and retention of complete veneer crown retainers. Quintessence Int. 1990;21(8):629-635.
6. Noonan JE Jr, Goldfogel MH. Convergence of the axial walls of full veneer crown preparations in a dental school environment. J Prosthet Dent.1991;66(5):706-708.
7. Parker MH, Malone KH, Trier AC, et al. Evaluation of resistance form for prepared teeth. J Prosthet Dent. 1991;66(6):730-733.
8. Parker MH, Calverley MJ, Gardner FM, Gunderson RN. New guidelines for preparation taper. J Prosthodont. 1993;2(1):61-66.
9. Wiskott HW, Nicholls JI, Belser UC. The relationship between abutment taper and resistance of cemented crowns to dynamic loading. Int J Prosthodont. 1996;9(2):117-139.
10. Annerstedt A, Engström U, Hansson A, et al. Axial wall convergence of full veneer crown preparations. Documented for dental students and general practitioners. Acta Odontol Scand. 1996;54(2):109-112.
11. Wiskott HWA, Nicholls JI, Belser UC. The effect of tooth preparation height and diameter on the resistance of complete crowns to fatigue loading. Int J Prosthodont. 1997;10(3):207-215.
12. Augereau D, Renault P, Pierrisnard L, Barquins M. Three-dimensional finite element analysis of the retention of fixed partial dentures. Clin Oral Investig. 1997;1(3):141-146.
13. Trier AC, Parker MH, Cameron SM, Brousseau JS. Evaluation of resistance form of dislodged crowns and retainers. J Prosthet Dent.1998;80(4):405-409.
14. Sato T, Al Mutawa N, Okada D, Hasegawa S. A clinical study on abutment taper and height of full cast crown preparations. J Med Dent Sci. 1998;45(3):205-210.
15. Wiskott HW, Krebs C, Scherrer SS, et al. Compressive and tensile zones in the cement interface of full crowns: a technical note on the concept of resistance form. J Prosthodont. 1999;8(2):80-91.
16. Goodacre CJ, Campagni WV, Aquilino SA. Tooth preparations for complete crowns: an art form based on scientific principles. J Prosthet Dent.2001;85(4):363-376.
17. Poon BK, Smales RJ. Assessment of clinical preparations for single gold and ceramometal crowns. Quintessence Int. 2001;32(8):603-610.
18. Zidan O, Ferguson GC. The retention of complete crowns prepared with three different tapers and luted with four different cements. J Prosthet Dent.2003;89(6):565-571.
19. Parker MH. Resistance form in tooth preparation. Dent Clin North Am. 2004;48(2):387-396.
20. Proussaefs P, Campagni W, Bernal G, et al. The effectiveness of auxiliary features on a tooth preparation with inadequate resistance form. J Prosthet Dent.2004;91(1):33-41.
21. Bowley JF, Sun AF, Barouch KK. Effect of margin location on crown preparation resistance form. J Prosthet Dent.2004;92(6):546-550.
22. Al-Omari WM, Al-Wahadni AM. Convergence angle, occlusal reduction, and finish line depth of full-crown preparations made by dental students. Quintessence Int. 2004;35(4):287-293.
23. Arnetzl G, Dornhofer R. PREPassistant: a system for evaluating tooth preparations. Int J Comput Dent. 2004;7(2):187-197.
24. Ayad MF, Maghrabi AA, Rosenstiel SF. Assessment of convergence angles of tooth preparations for complete crowns among dental students. J Dent. 2005;33(8):633-638.
25. Patel PB, Wildgoose DG, Winstanley RB. Comparison of convergence angles achieved in posterior teeth prepared for full veneer crowns. Eur J Prosthodont Restor Dent.2005;13(3):100-104.
26. Okuyama Y, Kasahara S, Kimura K. Quantitative evaluation of axial wall taper in prepared artificial teeth. J Oral Sci. 2005;47(3):129-133.
27. Rafeek RN, Marchan SM, Seymour KG, et al. Abutment taper of full cast crown preparations by dental students in the UWI School of Dentistry. Eur J Prosthodont Restor Dent. 2006;14(2):63-66.
28. Cameron SM, Morris WJ, Keesee SM, et al. The effect of preparation taper on the retention of cemented cast crowns under lateral fatigue loading. J Prosthet Dent. 2006;95(6):456-461.
29. Nick DR, Clark M, Miler J, et al. The ability of dental students and faculty to estimate the total occlusal convergence of prepared teeth. J Prosthet Dent. 2009;101(1):7-12.
30. Renne WG, McGill ST, Mennito AS, et al. E4D compare software: an alternative to faculty grading in dental education. J Dent Educ. 2013;77(2):168-175.
31. Hey J, Kupfer P, Urbannek M, Beuer F. Objective analysis of preparations in dental training: development of analytical software. Int J Comput Dent. 2013;16(4):317-325.
32. Bowley JF, Ichim IP, Kieser JA, Swain MV. FEA evaluation of the resistance form of a premolar crown. J Prosthodont. 2013;22(4):304-312.
33. Güth JF, Wallbach J, Stimmelmayr M, et al. Computer-aided evaluation of preparations for CAD/CAM-fabricated all-ceramic crowns. Clin Oral Investig. 2013;17(5):1389-1395.
34. McPherson KR, Mennito AS, Vuthiganon J, et al. Utilizing self-assessment software to evaluate student wax-ups in dental morphology. J Dent Educ. 2015;79(6):697-704.
35. Callan RS, Cooper JR, Young NB, et al. Inter- and intrarater reliability using different software versions of E4D compare in dental education. J Dent Educ. 2015;79(6):711-718.
36. Callan RS, Haywood VB, Cooper JR, et al. The validity of using E4D compare's "% comparison" to assess crown preparations in preclinical dental education. J Dent Educ. 2015;79(12):1445-1451.
37. Mays KA, Crisp HA, Vos P. Utilizing CAD/CAM to measure total occlusal convergence of preclinical dental students' crown preparations. J Dent Educ. 2016;80(1):100-107.
38. Alter D. CAD/CAM technologies allowing restorative dentistry to "push the envelope." Compend Contin Educ Dent. 2017;38(10):690-691.
39. Muruppel AM, Thomas J, Saratchandran S, et al. Assessment of retention and resistance form of tooth preparations for all ceramic restorations using digital imaging technique. J Contemp Dent Pract.2018;19(2):143-149.
40. Agency for Healthcare Research and Quality.Evidence-based decision making. Agency for Healthcare Research and Quality website. 2017. https://www.ahrq.gov/professionals/prevention-chronic-care/decision/index.html. Updated April 2018. Accessed August 22, 2019.