Achieving Optimal Esthetic Outcome With Previously Placed, Compromised Implants
Tal Morr, DMD, MSD
Abstract: The management of previously placed, periodontally compromised implants can be quite challenging for clinicians. This challenge can be compounded when there are adjacent, facially angled implants and bony and soft-tissue defects associated with these conditions. Not only is esthetic integration of the new prosthetics highly difficult to manage, but a contingency plan needs to be factored into the prosthesis to make it retrievable in case there are future problems. Understanding the thought processes of how to manage such a case prosthetically and implementing critical nuances into the treatment plan, as described in this case report, is vital.
Replacing a single missing tooth with a single-tooth implant can be challenging but fairly predictable if the right scenario exists. If the interproximal bone levels are correct, the interproximal papilla may be maintained in the correct or near correct positions, because the papillary height is determined by the interproximal peaks of bone on the teeth adjacent to the implant, not the bone around the implant.1-3 The height of the papilla will generally remain or regenerate to around 4 mm to 4.5 mm above the bone level. If the facial plate of bone is deficient, it can be grafted to the height of the interproximal bone levels of the teeth adjacent to the implant site, and, therefore, generally be regenerated with bone and a connective tissue (CT) graft to an even more coronal position than the initial scenario. Bear in mind that although this situation may seem straightforward in theory, in reality replacement of a single anterior tooth may not always be this predictable.
Pontics also can be successfully utilized as part of a bridge when a tooth is extracted. In this scenario, the papilla height is also influenced by the bony peaks on the teeth adjacent to the implant site, but the height of the papilla can be even longer around a pontic as compared to an implant. In fact, research found that after soft-tissue grafting, up to 9 mm of height can be obtained between a tooth and a pontic in some patients, with an average of 6.5 mm.4 By comparing the height of the papilla around an implant (4.5 mm) to a pontic (6.5 mm), it is quite evident that the use of pontics between implants can be helpful in maintaining or rebuilding a closer-to-ideal esthetic outcome.
Multiple Missing Teeth
When adjacent teeth are extracted and implants are placed in both sites, the bone on the remaining teeth adjacent to the implants will support the papilla. However, between the implants there generally will be dramatic changes of the soft-tissue form. For example, if two central incisors are extracted and implants placed adjacent to each other, the lateral incisors will maintain the papilla on the mesial aspect of the laterals due to the interproximal bone levels, but the bone and soft tissue between the central incisors will flatten out to approximately 3 mm to 3.5 mm in height, which is about 1.5 mm shorter than between an implant and a tooth.5 To better understand this phenomenon, it is important to know what occurs around natural teeth as compared to implants. With two natural anterior teeth, the soft-tissue margin generally follows the scallop of the bone with a distance of approximately 3 mm on the facial aspect from bone to soft tissue.6,7 In the interproximal area between teeth, the average height of the papilla is approximately 4.5 mm to 5 mm, which is about 1.5 mm higher than the facial margin, thereby enhancing the scallop of the soft tissue.8 Teeth have a periodontal ligament (PDL), which, under function, will stimulate the bone to "turn over," hence maintaining its form. The soft tissue around teeth is supported by the supracrestal fiber attachment (CT attachment), the epithelial attachment, and the sulcus. These three entities form the biologic width.9-11
When teeth are extracted and implants placed, the supracrestal fiber attachment is severed and the PDL is eliminated. Implants generally are placed with their platform at a level 3 mm to 4 mm apical to the facial gingival margins. This means that the head of the implant is subosseous in relationship to the interproximal bone, and, therefore, this interproximal peak of bone between two implants is no longer being stimulated by the PDL to turn over. Also, the supracrestal fiber attachment, which held the tissue in its position by being inserted perpendicularly into the cementum of the tooth, is severed when the tooth is extracted. After implant placement and healing, the connective tissue fibers do not connect directly to the implant as with a tooth, but rather run vertically and circumferentially.12 In essence, the loss of both the PDL and the supracrestal fiber attachment causes the bony architecture and papilla to flatten when two adjacent implants are placed next to each other. Although this flattening of the architecture may be acceptable in some situations, it could create an esthetic failure, especially when the patient puts a high priority on esthetics.
It would seem logical to utilize pontics between implants given the potential for enhanced tissue thickness as compared to placing adjacent implants. This will generally improve the chances of creating a more esthetic soft-tissue profile. Unfortunately, although the biology of adjacent implant placement and the associated subsequent loss of volume of bone and soft-tissue architecture is generally understood in dentistry, it is not uncommon for patients to present with multiple implants placed next to each other. This may be a result of the patient desiring single-unit restorations to enable flossing between them. Or perhaps trauma resulted in the loss of teeth at different times and rather than being proactive, the dental team decided to wait to place implants as the teeth became unrestorable. Regardless of why this situation occurred, such a case has a high potential to become problematic, and it may be difficult to obtain a reasonable esthetic result.
The following sections provide guidance as to the objectives and considerations for restorative options for the management of four missing incisors.
Replacement of Four Maxillary Incisors: Treatment Planning Options, Requirements, and Possible Surgical Procedures
Treatment objectives should, of course, include making the final restorations esthetic, cleansable, and maintainable long term. Given that most scenarios with missing upper incisors will entail a ridge deficiency both vertically and horizontally, this situation will typically necessitate a surgical procedure utilizing a bone and/or CT graft to improve the ridge form. The surgical procedure aims to idealize the sites for esthetic purposes and/or make the restoration cleansable and maintainable. Even when such regeneration is successful, the end-result will have unsatisfactory papilla and gingival esthetics.13 In some situations, if implants cannot be placed predictably they may not be indicated at all. By understanding the biologic limitations in deficient-site regeneration and these regenerative procedures themselves, clinicians can be proactive in trying to minimize the trauma of multiple surgical procedures that still may not achieve an ideal result.14
Pink ceramics can be useful in restoring missing hard and soft tissue when defects are simply too large to regenerate. Even when the plan calls for a pink and white restoration, clinicians must understand the requirements and objectives when preplanning the case to avoid subsequent issues. For example, the interface of the prosthetic gingiva should be positioned so that the interface is hidden, the implant should be positioned to create a proper emergence form (depth), and proper angulation of the implant must be ensured to make it retrievable.15
All treatment planning should begin with a facial analysis and evaluation of the relationship of the teeth to the face, ie, a "facially generated treatment plan."16 This is done by first determining where the teeth belong in the face and working backward to ascertain the proper treatment plan vis-à-vis white versus pink and white restorations. The following questions may be asked to help determine which approach will provide the optimal esthetic outcome for the specific case:
Where is the ideal incisal edge position as it relates to the lips, and where does the cementoenamel junction (CEJ) of the tooth belong to create an ideal width/length (w/l) ratio of 75% to 85%?17,18
What is the existing ridge position in three dimensions in relationship to the proposed CEJ position of the future tooth?
Where is the future papilla position relative to the existing ridge?
Is there enough bone to accommodate implants, and if there is not, can the bone be regenerated predictably?
Where is the existing ridge position relative to the lip (ie, above the lip, or below it in a high smile)?
Once these questions are answered, a logical approach can be used to determine the best option for treatment. Restorative options, based on the above questions, are as follows:
Six- to Eight-Unit Tooth-Supported Bridge With Four Ovate Pontics-White Ceramics Only
The requirements for this treatment option include structurally and periodontally sound teeth adjacent to the site, and minimal vertical and horizontal deficiency. The incisal edge to ridge length is close to ideal, with a w/l ratio of 75% to 85% whether the ridge is under or above the lip during high smile. The ridge and papilla both can be regenerated surgically through CT grafting to an acceptable level based on patient expectations. There is not enough bone for implants, and the patient either does not want a hard-tissue grafting procedure to augment for implant placement or does not want implants at all.
Possible surgical procedures to idealize the ridge for restoration-Horizonal and/or vertical augmentation with bone and/or CT graft for improved ovate pontics form. If bone graft is utilized to augment for ovate pontics, a slow-resorbing material must be used.
Six- to Eight-Unit Tooth-Supported Bridge-White and Pink Ceramics
The requirements for this treatment option include structurally and periodontally sound teeth adjacent to the site, and significant vertical and horizontal deficiency below the lip. The incisal edge to ridge length is not ideal, with a less-than 75% w/l ratio. The position of the gingival margin on the distal of the extraction site is below or at the lip border in the canine region, and the ridge position is below the lip. There is not enough bone for implants, and the patient either does not want a hard-tissue grafting procedure to augment for implant placement or does not want implants at all. The bridge is not removable, therefore the pink portion should be made out of ceramics to enhance long-term maintenance.
Possible surgical procedures to idealize the ridge for restoration-If the residual ridge is not in view in a high smile line, horizonal augmentation is performed with bone and/or CT graft to create a flat ridge form and eliminate ridge lapping.
If the residual ridge is in view in a high smile line, the following options may be considered: possible vertical bone reduction to flatten the ridge, and the junction of the ridge and pink ceramics is placed below the lip; possible crown lengthening to position the margin of the canines under the lip; horizontal augmentation only, with bone and/or CT graft used to create a flat ridge form and eliminate ridge lapping.
Four-Unit Implant Bridge-White Ceramics Only
The requirements for this treatment option include structurally and periodontally sound teeth adjacent to the site and either enough bone to accommodate implants or the ability to regenerate bone for implants. There is minimal vertical and horizontal deficiency. The incisal edge to ridge length is close to ideal, with a w/l ratio of 75% to 85% whether the ridge is under or above the lip during high smile. The ridge and papilla both can be regenerated surgically through bone and/or CT grafting to an acceptable level based on patient expectations. The depth of the implant should be 3 mm apical from the CEJ of the future gingival margin position. Implants should be placed in alternating positions with pontics in between, and the preferable position of implants is away from the midline with pontics in between (eg, implants in lateral positions and central pontics).15 Bucco-lingual positioning of implants will accommodate screw-retained restorations for retrievability.
Possible surgical procedure to idealize the ridge for restorations-Planning is needed prior to extractions to minimize future soft-tissue and bony defects. The procedure should utilize flapless, immediate implant placement, along with ridge preservation techniques, including CT and bone grafts, and/or root submergence or partial extraction therapy techniques.
Four-Unit Implant Bridge-Pink and White Ceramics
The requirements for this treatment option include structurally and periodontally sound teeth adjacent to the ridge. The incisal edge to ridge length is not ideal, with a less-than 75% w/l ratio. The residual ridge position is below the lip, and the position of the gingival margin on the distal of the extraction site is below or at the lip border in the canine region. There is either enough bone for implant placement or the ability to regenerate bone for implant placement. There should be alternate implant positions with a flat ridge in between, and the preferable position of implants is away from the midline with the edentulous ridge in between (eg, implants in lateral positions).15 The depth of the implant should be 3 mm to 4 mm apical to accommodate the future pink prosthetic margin position. Implant angulation is toward the cingulum area to enable a screw-retained restoration for retrievablility.15 There is a flat and wide ridge form between implants to eliminate ridge lapping.17 The pink portion should be made in ceramics to enhance long-term maintenance. Pink papilla extensions, ie, "floating papilla,"17 must have a path of draw next to adjacent teeth, therefore undercuts on canines need to be minimized.
Posslble surgical procedures to idealize the ridge form-Horizontal augmentation with bone and/or CT graft (bone replacement type should be slow-resorbing); possible crown lengthening to position the canine gingival margin at or below the lip; possible ridge reduction if the residual ridge is in view during high smile.
Case Presentation
The aforementioned treatment planning options are for replacement of four missing incisors. Occasionally, clinicians do not have the luxury to treatment plan a case prior to implant placement and are forced into a non-ideal situation. The following case is an example of such a situation, in which four adjacent implants had been placed to replace missing or lost incisors. This report describes the thought process behind the treatment and the execution of the case.
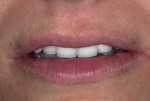
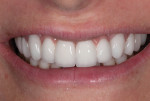
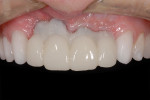
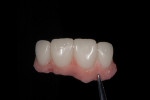
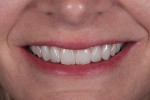
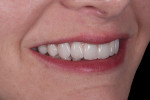
A 41-year-old woman presented to the office requesting an improvement in her smile (Figure 1 and Figure 2). She described a history of riding a bicycle and hitting a car when she was 8 years old. Tooth No. 8 was avulsed due to the trauma, and her parents immediately took her to the hospital and had the tooth re-implanted. At the hospital, she was told that all four of her incisors were broken and would eventually need endodontic therapy and restoration. Ultimately, all four teeth required endodontic treatment followed by apicoectomies and retreatments.
At age 26, while pregnant, the patient lost tooth No. 8. A bridge was placed, but 5 years later tooth No. 7 had an endodontic abscess. It was decided at the time to place two implants in position Nos. 7 and 8 and an implant bridge. The patient did not remember having any grafting done. She did recall that the implants were placed too far facial and that her gum and bone began receding on the facial aspect of Nos. 7 and 8.
An implant placed too far facially with a thin phenotype often results in a dehiscence of the buccal cortical plate and leads to a high potential for gingival recession, as seen in this case.14,19,20 At this point, the patient had been restored at least twice. Eventually, at the age of 34-35, she lost the remaining upper incisors, Nos. 9 and 10, and had two more implants placed in those positions. Again, she did not recall having any grafting procedures done, just extractions and implant placement. Later, two bridges were made, one for the Nos. 7-8 implants, the other for the Nos. 9-10 implants, both with pink ceramics. Also, the canines and bicuspids were restored with veneers to improve the patient's smile.
Extraoral Examination
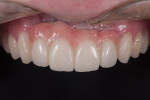
The patient considered the existing upper restorations to be opaque and artificial-appearing in form and wanted her teeth to look more realistic. Upon evaluation, at rest the incisal edge appeared acceptable in length (Figure 1), but during a high smile, due to the patient's high lip mobility, the teeth appeared slightly too long incisally (Figure 2). Given that there was approximately 4 mm of tooth exposure at rest, there was room to shorten the teeth to create better teeth proportions while still maintaining the patient's youthful appearance.
As a result of the patient having been restored with two bridges, Nos. 7-8 and 9-10, a number of esthetic shortcomings were visible, including the long contact and short papilla between the central incisors, a junction line between the central incisors at the papillary level, and a discrepancy between the pink ceramic on the distal of the lateral incisors and the canine natural papilla (Figure 2). With the pink ceramic and the natural soft-tissue junction in view, it would be difficult to achieve an esthetic result.
Intraoral Examination
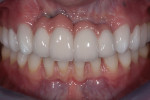
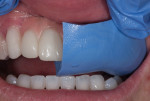
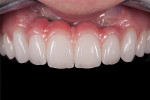
Intraorally, large vertical and horizontal defects were noted (Figure 3). These appeared to be a result of the labial positioning of the implants and the resorption of the buccal plate of bone around the implants. The patient recalled that no attempt was made to augment this area at the time of implant placement.
Poor tissue quality existed throughout the upper and lower anterior segments. The patient, being a dental hygienist, was aware of the problems with the soft tissues and the recession on the lower anterior area but, unfortunately, due to an autoimmune issue that affected healing, she could not undergo a surgical procedure to improve the tissue quality at the current time. Additionally, the junction lines between the implant bridges were quite evident along with the unusual papillary form between the central incisors created by the junction of the pink ceramic between the two bridges.
The intraoral examination also revealed a color difference between the lateral incisor pink ceramic and the papilla on the mesial of the canines, and a class I canine relationship. Additionally, veneers were on teeth Nos. 4 through 6 and 11 through 13.
Radiographic Examination
Radiographically, it could be seen that implant Nos. 7 and 8 already had three to four threads exposed while Nos. 9 and 10 appeared normal (Figure 4). Although compromised, implant Nos. 7 and 8 had been in place for 9 years.
Esthetic Improvement of Implant Nos. 7 through 10
To create a natural-looking pink and white restoration, it was decided that a bridge connecting all of the implants should be made in one piece to eliminate any junctions of pink ceramic. Such a junction would always be obvious if the bridge was broken into segments. Secondly, the distal papilla would begin in the area under the lip, such as the mesial of the canine, to avoid a visible line between ceramic and soft tissue.
Given the lack of realistic pigmentation available today for pink ceramic, it is extremely difficult to match pink ceramic to soft tissue perfectly. If the junction of the pink ceramic to the soft tissue begins under the lip, the color difference will be less evident. Based on these factors, a plan was developed to make these changes and improve the patient's smile. Unfortunately, as in this case, what the clinician may find under old restorations is unpredictable.
Treatment Plan and Execution Steps Based on the Determined Esthetic Changes
Step 1. Impressioning and wax-up-Impressions were taken and a wax-up was made to reshape the teeth on a model, making them slightly shorter and giving them a nicer contour.
Step 2. Four-unit provisional-The final wax-up was sent to the laboratory to make a four-unit provisional restoration from a milled polymethyl methacrylate (PMMA) material, which is highly resistant to staining due to its fabrication process in which porosity is eliminated, making the material more dense, esthetic, and resistant to wear.
Step 3. Upper provisionalization-The upper provisionalization appointment, which is the most critical of all the steps, allows the clinician to visualize what is under the old restoration, determine if the esthetic changes that have been incorporated are appropriate, assess function and speech, and, especially so in this case, evaluate and manipulate the form of the teeth so that the anterior implant bridge will draw relative to the adjacent canines. The provisional restoration also will allow the soft tissue to be formed to make it more cleansable.
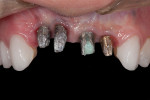
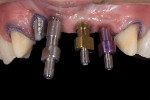
The existing implant bridges were removed to allow evaluation of the existing abutments and implants (Figure 5). Upon removal of the bridges, implant No. 7 was found to have a solid implant abutment, and the implant and abutment appeared to have been prepared together. This prohibited the removal of the existing abutment. Implant No. 8 was found to have been prepared with a bur into the implant body; however, replacing the existing abutment seemed to be possible. Finally, the abutments on Nos. 9 and 10 were found to be removable and the implants in better condition than Nos. 7 and 8.
Although the implants on the upper right (Nos. 7 and 8) were quite compromised, to reiterate, the patient had medical issues that precluded removal of the existing implants and grafting of the site. It was, therefore, decided that the abutment on No. 7 would be used just as it was, and the other abutments would be removed and a substructure frame made to extend to the head of the implants. For the provisionalization, the existing abutments were modified slightly and maintained to support the provisionals.
The provisional shell milled by the laboratory was sent to the office with no pink ceramic (Figure 6). The shell was relined with cold-cure acrylic resin and marginated with the same material utilizing the "salt and pepper technique," which entails dipping a brush into the monomer liquid and then into the powder, and using the brush to flow the resin circumferentially around the margins, allowing the resin to capture the details of the margins. Once hardened, the shell was trimmed to create a precise fit. A CEJ form was delineated in the cervical region to allow definition of the final crown contour, taking into consideration the w/l ratio. Cold-cure pink acrylic was applied intraorally again utilizing the salt and pepper technique; it was applied to the apical portion of the provisional above the CEJ level and to the papillary area distal of the laterals to create wings (Figure 7). Once the material began setting, the provisional was pumped in and out until set to eliminate undercuts next to the canines and ensure a path of draw so that the implant segment would be removable.
Next, the canines and bicuspids were prepared for temporaries. After removal of the existing veneers, the canines were prepared for 3/4 crowns and the bicuspids for veneers. Vaseline was applied to the distal aspect of the anterior provisional to prevent anything from sticking to it. A putty matrix of the wax-up was filled with cold-cure acrylic until it reached the doughy state and was placed in the mouth (Figure 8). Again, the putty matrix was pumped in and out until set. Once set, it was removed and trimmed, and the margins were idealized with cold-cure acrylic resin. The veneer temporaries were polished and cut distal to the canines to allow the canine crowns to be fabricated with the anterior implant restorations to ensure a path of draw. Because veneer provisionals do not stick well for a long period of time due to lack of mechanical retention they were bonded permanently to allow visualization of the projected esthetic outcome and to evaluate function.
The posterior bicuspid temporaries were trimmed and polished. The bicuspids were etched, and bonding agent was applied to the teeth and the intaglio surfaces of the temporaries. A permanent resin cement was then applied, the veneers positioned and light-cured for 3 seconds, and the excess cement cleaned. A viscous oxygen barrier solution was applied to the margins, and the veneers were light-cured for 40 seconds each. Bonding the veneers permanently enabled visualization of the projected final smile and allowed the temporaries to remain in place until the implant bridge and canine crowns were fabricated. Once the posterior veneer temporaries were bonded, the remaining provisionals were cemented with temporary cement (Figure 9).
Step 4. Surgical augmentation-Given that the bone levels of the implants on the right side (Nos. 7 and 8) were already at the fourth thread and the implant bodies were damaged, it would have been ideal to extract these implants and then perform bone and CT grafting to rebuild the site and improve the tissue quality. This would have then been followed by placement of a new implant in the area of No. 7 and a pontic in the area of No. 8. Unfortunately, due to the patient's aforementioned health issue she was unable to undergo a surgical procedure. Even a CT graft would have benefited the patient given her tissue quality, but this was not an option.
Step 5. Final impression-As discussed earlier, a pink implant reconstruction should be removable or retrievable. Utilizing all of the exiting abutments would require a cement-retained restoration. Because of the compromised status and questionable prognosis of the implants in this case, it was imperative to somehow fabricate a removable final restoration. Another significant issue was that because all of the existing implants were flared to the facial, a standard screw access would emerge straight out of the facial of the teeth. As mentioned previously, it was decided to utilize the abutment on implant No. 7 "as is" due to the damage to the implant head and body. The abutments on the remaining implants were removed, and open-tray impression copings were placed. Cord was packed around the canines, and a final impression was taken of Nos. 6 through 11 utilizing a polyvinyl siloxane (PVS) (Figure 10). A lower model, an upper provisional model, and a bite record were taken as well.
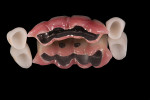
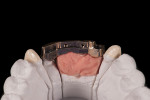
Step 6. Final restoration fabrication in the laboratory-In the laboratory, the case was cross-mounted with the provisional model to place the preparations and provisional in the same 3-dimensional position. To make the final prosthesis removable, a frame was designed out of wax and modeling resin (GC Pattern Resin™, GC America, gcamerica.com) onto UCLA-type abutments. Lingual set-screw frames were embedded into this pattern, which was then milled to create a retentive form for the superstructure. Once milled, the pattern was cast in high-noble metal. A separate abutment was waxed and milled in wax for implant No. 7. The designed frames were invested and cast in yellow gold. The single implant abutment No. 7 was soldered on the model to the remaining substructure.
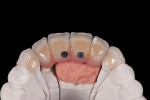
Once the substructure was cast and finished, a metal overlying superstructure was fabricated, also out of high-noble alloy, waxed, and cast to fit the underlying frame. The screw holes were developed in the wax phase to proper positioning relative to the threads in the substructure. The canine 3/4 crowns were pressed in lithium disilicate (IPS e.max, Ivoclar Vivadent, ivoclarvivadent.com) and layered facially to mimic the contour of the provisional. Once the canines were finished and the mesial contour idealized to eliminate any undercut on the facial, the final ceramics were baked on the superstructure. A path of draw was determined for the pink papilla extension as was done with the provisional, but this time in pink ceramic (Figure 11 through Figure 13).
Step 7. Delivery of case-At the delivery phase, the provisional restorations were removed in the anterior area, as were the abutments on Nos. 8 through 10. The frame and superstructure were tried in to ensure adequate spacing for interproximal cleaning and were modified slightly to allow for a brush and floss to be passed under the bridge in the interproximal areas.
Once the space was idealized, the frame was polished and cleaned with discs. Crown Nos. 6 and 11 were placed in the mouth, followed by the superstructure for the implant restoration to ensure a passive path of insertion and draw. Upon confirmation, temporary dental cement (Temp-Bond™, Kerr Dental, kerrdental.com) was placed into the abutment No. 7, and the substructure frame was torqued to 35 Ncm (Figure 14). Teflon tape was inserted into the access hole and covered with composite resin (Fermit™, Ivoclar Vivadent). Then, #000 retraction cord was packed in the sulcus of Nos. 6 and 11, and the e.max crowns were etched with hydrofluoric acid for 20 seconds and silinated, and bonding agent was applied to the intaglio surfaces. The canines were etched and the crowns bonded with resin cement. Once cured and cleaned, the superstructure was placed onto the substructure and the lingual set screws were inserted and tightened. The occlusion was checked and adjusted, and polishing was performed.
Step 8. Veneer preparation-The veneer temporaries were still bonded to teeth Nos. 4, 5, 12, and 13. An impression was taken of the upper arch and poured in stone, and two putty matrices were made from this model. One was cut incisally to allow visualization of the preparation in relationship to the final contour of the tooth, and the other was a full matrix for fabrication of the final veneer temporaries. The permanently cemented veneer temporaries were prepared as if they were intact teeth until the proper reduction was achieved. The cut putty matrix was used to ensure proper reduction. A new set of temporaries was fabricated with cold-cure acrylic placed in the mouth ultilizing the full matrix. Once removed, the veneer temporaries were finished and polished. The provisional restorations were measured to ensure proper spacing for the final veneers, and once this was confirmed, the final impression was taken in PVS. A bite registration record was not necessary because the occlusal surfaces of the bicuspids were not touched. The bicuspids were spot-etched, and the veneer temporaries were cemented with a resin cement.
Step 9. Veneer fabrication and delivery-The bicuspid veneers were fabricated in e.max to allow for bonding and to ensure a shade match to the canines. They were pressed, cut back, and layered on the facial.
The temporary veneers were then removed, cords packed, and the veneers treated prior to bonding as described previously for the 3/4 canine crowns. The teeth were treated the same also, the veneers were bonded, and excess cement was removed. The final result provided a dramatic improvement in the overall esthetics (Figure 15 through Figure 17), as the elimination of the junctions that had resulted from multiple segments and the incorporation of the distal pink ceramic extensions made it quite difficult to discern between the pink ceramic and the natural pink soft tissue. The changes in the overall form and contour of the teeth improved dramatically. Additionally, the cervical contours of the pink ceramic was made to be more cleansable, and because of the frame design, the bridge was removable in case of future problems.
Discussion
As stated previously, this case was compromised from many aspects. Rather than placing two implants in alternating positions, four implants were placed. This may have been done because instead of proactively treating the patient when she was having problems with her anterior teeth, the previous surgeon apparently decided to treat one or two teeth at a time, thereby replacing them as they were lost. The upper right implants, which were prepared with a bur, already had some threads exposed. Unfortunately, the patient could not undergo surgical procedures due to medical issues. Not only were the implants biologically and structurally compromised, but their angulation made it impossible to utilize a standard lingual access hole, as would have been the case with ideally placed implants.
The ideal solution would have been to extract the upper right implants, place a new implant in the upper right lateral position, and graft bone and soft tissue to horizontally augment and improve the quality of the tissue. This, however, is typically a difficult procedure for patients and would require considerable time and money, and the patient would incur much discomfort. Again, at the wishes of the patient in the present case, the existing implants were utilized. The decision to employ the metal frame was based largely on the ability of the technician as well as his experience and skill in dealing with lingual set screws and frames. Different technicians have different specialties, and in this case the technician was highly skilled working with porcelain fused to metal. If zirconia was used instead of metal, it would have been difficult to create the proper channel for a screw-retained superstructure. Although possible, this would require bonding a metal channel and screw channel into zirconia, which is not ideal in terms of strength. The strength of this type of connection would be dependent on bonding of the channel to the zirconia as compared to the channel being formed directly into the gold frames. Overall, although compromised from a biologic standpoint, the patient is doing well and is happy with the outcome.
Acknowledgment
The author thanks Thomas Sing, MDT, for his exceptional laboratory work.
About the Author
Tal Morr, DMD, MSD
Private Practice limited to Esthetic, Implant, and Complex Restorative Dentistry, Aventura, Florida; internationally recognized author and speaker on such topics as esthetics, implants, and full-mouth rehabilitation
References
1. Choquet V, Hermans M, Adriaenssens P, et al. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001;72(10):1364-1371.
2. Grunder U. Stability of the mucosal topography around single-tooth implants and adjacent teeth: 1-year results. Int J Periodontics Restorative Dent. 2000;20(1):11-17.
3. Kan JY, Rungcharassaeng K, Umezu K, Kois JC. Dimensions of peri-implant mucosa: an evaluation of maxillary anterior single implants in humans. J Periodontol.2003;74(4):557-562.
4. Salama H, Salama MA, Garber D, Adar P. The interproximal height of bone: a guidepost to predictable aesthetic strategies and soft tissue contours in anterior tooth replacement. Pract Periodontics Aesthet Dent.1998;10(9):1131-1141.
5. Tarnow D, Elian N, Fletcher P, et al. Vertical distance from the crest of bone to the height of the interproximal papilla between adjacent implants. J Periodontol. 2003;74(12):1785-1788.
6. Elian N, Jalbout ZN, Cho SC, et al. Realities and limitations in the management of the interdental papilla between implants: three case reports. Pract Proced Aesthet Dent. 2003;15(10);737-744.
7. Saadoun AP, Le Gall MG, Touati B. Current trends in implantology: part II-treatment planning, aesthetic considerations, and tissue regeneration. Pract Proced Aesthet Dent. 2004;16(10):707-714.
8. Tarnow DP, Magner AW, Fletcher P. The effect of distance from the contact point to the crest of bone on the presence or absence of the interproximal dental papilla. J Periodontol. 1992;63(12):995-996.
9. Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontol. 1961;32(3):261-267.
10. Rateitschak KH, Rateitschak EM, Wolf HF, Hassell TM. Color Atlas of Dental Medicine: Periodontology. 2nd ed. New York, NY: Thieme Medical Publishers, Inc; 1989:4-7.
11. Stern IB. Current concepts of the dentogingival junction: the epithelial and connective tissue attachments to the tooth. J Periodontol. 1981;52(9):465-476.
12. Berglundh T, Lindhe J, Ericsson I, et al. The soft tissue barrier at implants and teeth. Clin Oral Implants Res. 1991;2(2):81-90.
13. Belser UC, Bernard JP, Buser D. Implant-supported restorations in the anterior region: prosthetic considerations. Pract Periodontics Aesthet Dent. 1996;8(9):875-883.
14. Coachman C, Salama M, Garber D, et al. Prosthetic gingival reconstruction in a fixed partial restoration. Part 1: introduction to artificial gingiva as an alternative therapy. Int J Periodontics Restorative Dent. 2009;29(5):471-477.
15. Salama M, Coachman C, Garber D, et al. Prosthetic gingival reconstruction in a fixed partial restoration. Part 2: diagnosis and treatment planning. Int J Periodontics Restorative Dent. 2009;29(6);573-581.
16. Spear F. Facially generated treatment planning. Paper presented at American Academy of Esthetic Dentistry Annual Meeting; 1986; Colorado Springs, CO.
17. Sterret JD, Oliver T, Robinson F, et al. Width/length ratios of normal clinical crowns of the maxillary anterior dentition in man. J Clin Periodontol. 1999;26(3):153-157.
18. Chiche GJ, Pinault A. Replacement of deficient crowns. In: Chiche GJ, Pinault A, eds. Esthetic of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence Publishing; 1994:53-73.
19. Buser D, Martin W, Belser UC. Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants. 2004;19 suppl:43-61.
20. Tarnow DP, Eskow RN. Considerations for single-unit esthetic implant restorations. Compend Contin Educ Dent. 1995;16(8):778-784.