Salvaging a Periodontally Compromised and Endodontically Involved Three- Rooted Mandibular First Molar With Cervical Enamel Projection
J. Sylvia Western, MDS; Vivek Vijay Gupta, MDS; and Srinivas Sulugodu Ramachandra, MDS
Abstract: This case report describes the management of a mandibular first molar with an additional distolingual root (radix entomolaris) and grade III cervical enamel projection through a multidisciplinary approach. Diagnosis for the case was endodontic-periodontal lesion due to non-vitality and associated advanced periodontal destruction. The patient was treated with drainage of the periodontal abscess with adjunct antibiotics, phase I periodontal therapy, endodontic therapy, radiculoplasty, regenerative periodontal therapy, replacement of the missing right mandibular second molar, and long-term maintenance. Follow-up of the patient up to 9 months has been uneventful. Cases of advanced periodontal destruction typically show some degree of tooth mobility, which was absent in this case. The article discusses the tripod effect as well as the increased surface area for periodontal attachment provided by the additional root contributing to the non-mobility of the involved tooth.
A major anatomical variant of the two-rooted mandibular first molar is an additional distolingual root, referred to as the radix entomolaris (RE).1 The scientific literature has extensive reports on three-rooted mandibular molars and their prevalence among different races.2-5 The prevalence of these three-rooted mandibular first molars appears to be less than 3% in African populations, no more than 4.2% in Caucasians, less than 5% in Eurasian populations, and more than 5% (even up to 40%) in populations with Mongolian traits.2-5 Scientific literature also includes occurrence of endodontic mishaps due to failure to identify the third root6,7 and incidence of advanced periodontal attachment loss attributed to the presence of the additional third root.8 Advanced periodontal disease may prompt the clinician to advise amputation of the RE or extraction of the involved tooth.1
Perhaps the most commonly occurring anatomic factor related to RE is cervical enamel projection (CEP), which is associated with attachment loss in the furcation areas of molars.9 Scientific literature supports the highest prevalence of CEP among the Taiwanese population and in mandibular second molars.9 Coexistence of RE and CEP in a mandibular molar and the management of this condition has not yet been documented. This article reports the successful management of a mandibular first molar with RE and a buccal grade III CEP through a multidisciplinary approach.
Case Report
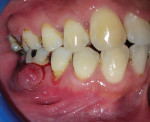
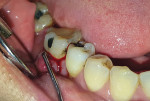
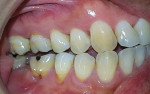
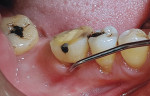
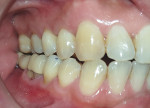
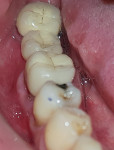
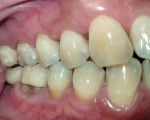
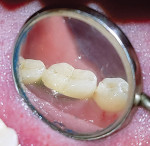
A 45-year-old male patient of Chinese origin reported to SEGi Oral Health Center, Malaysia, with a chief complaint of suppuration discharge in the right lower posterior tooth region. The patient was under medication for diabetes mellitus for the past 10 years. Past dental history revealed extraction of the mandibular right second molar (tooth No. 31) and mandibular left first molar (tooth No. 19). Extraction of tooth No. 31 was precipitated by caries, whereas removal of tooth No. 19 was due to periodontal reasons. Intraoral examination of the soft tissues revealed a sinus tract in the buccal alveolar mucosa in relation to the mandibular right first molar (tooth No. 30) (Figure 1). Although sinus tracing with gutta-percha is usually indicated to identify the source of infection, whether endodontic or periodontal, in this case clinical judgment and radiographic findings identified the source of infection in tooth No. 30 as being of both pulpal origin and periodontal origin, and therefore sinus tract tracing with gutta-percha was not needed. Hard-tissue examination revealed the presence of a large composite restoration in the occlusal aspect and an amalgam restoration on the buccal aspect of tooth No. 30 (Figure 2).
Basic periodontal examination scores for the patient were 3, 2, 3 (right to left) for the maxillary sextants and 4, 2, 2 (right to left) for the mandibular sextants. Detailed periodontal examination divulged a periodontal pocket of 10 mm at both distobuccal and distolingual aspects of the mandibular right first molar with drainage of pus from the sulcus (Figure 2). Probing at the furcal region using a Nabers probe revealed a grade II furcation involvement. The mandibular first molar was nonmobile. The tooth was nonresponsive to cold and electric pulp sensitivity tests indicating non-vitality.
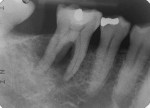
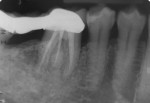
The intraoral periapical radiograph of the mandibular right first molar (tooth No. 30) showed radiolucency around the periapex with severe bone loss (Figure 3). Careful observation of this radiograph showed the presence of an additional distolingual root in relation to this tooth. The radiograph showed radiolucency in the furcation area with inter-radicular bone loss extending up to the apex of the distal and distolingual roots. Endodontically, the diagnosis was chronic apical abscess associated with necrotic pulp. Due to the associated advanced periodontal destruction, this lesion was classified as an endodontic-periodontal lesion. The formulated treatment plan comprised of drainage of the periodontal abscess with adjunctive antibiotics, phase I periodontal therapy (scaling and root surface debridement), endodontic therapy, and radiculoplasty, followed by regenerative periodontal therapy and replacement of the missing right mandibular second molar.
Informed consent was obtained from the patient after the formulated treatment plan, its advantages and disadvantages, and the prognosis for the involved tooth were explained to him.
Treatment Procedures
Drainage of the periodontal abscess through the sulcus using area-specific curettes and prescription of adjunctive antibiotics (tablet amoxicillin and clavulanic acid 625 mg three times daily for 5 days) constituted the emergency treatment. One week later, phase I therapy was initiated, which included supra- and subgingival scaling and root surface debridement. In the subsequent appointment, an endodontist initiated nonsurgical endodontic therapy in tooth No. 30. Pain control during endodontic and periodontal procedures at different time periods throughout this treatment was achieved by performing inferior alveolar nerve block by administering one cartridge of 2% lignocaine with 1:100,000 epinephrine. Access opening was performed under rubber dam isolation using an endodontic access bur. Initially, the prepared access cavity was triangular, and the mesiobuccal, mesiolingual, and distal root canal orifices were located using an endodontic explorer.
Based on observations from the preoperative radiographs, the root canal orifice corresponding to the RE root was anticipated to be just lingual to the distal root canal orifice. Further, the access cavity was modified to a trapezoidal shape to locate the fourth canal. A glide path was established using #08 and #10 size K-files. The working length of the canals was determined electronically using an apex locator and confirmed radiographically. Canals were then cleaned and shaped using rotary nickel-titanium files and a crown-down technique under copious irrigation using 3% sodium hypochlorite, 2% chlorhexidine, and 17% ethylenediaminetetraacetic acid (EDTA). Canal disinfection was carried out by placing non-setting calcium hydroxide as an intracanal medicament for 7 days.
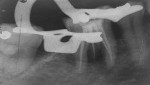
In the subsequent visit, the patient was asymptomatic. Clinically, there was no tenderness on percussion and no active pus drainage from the sinus tract, and the canal was dry. The periodontal status, however, remained unaltered. A master cone radiograph was taken (Figure 4) and obturation was completed using a single-cone technique and a mineral trioxide aggregate (MTA)-based root canal sealer. Restoration of the coronal access cavity was done using glass-ionomer cement followed by direct composite.
Case Re-evaluation
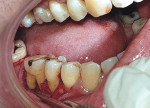
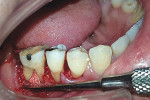
One month after endodontic therapy, the case was re-evaluated. At the re-evaluation visit, the patient presented with exposure of the buccal furcation in relation to tooth No. 30 due to gingival recession (Figure 5), revealing a grade III CEP (indicated by the arrows in Figure 5). The presence of deep periodontal pockets on both the buccal and lingual aspects with bleeding on probing indicated residual infection (Figure 6). The clinicians conveyed to the patient the need for further periodontal surgery to eliminate the residual infection in relation to tooth No. 30 and obtained his informed consent.
After administration of intraoral anesthesia, placement of a crevicular incision extending from tooth No. 28 to tooth No. 30 and a crestal incision in relation to the edentulous area between teeth Nos. 30 and 32 marked out the surgical area. A full-thickness mucoperiosteal flap was elevated. Removal of the tissue tags and granulation tissue provided access to and visibility of the bony defects and root surfaces (Figure 7). Elimination of the root roughness was accomplished by thorough root surface debridement. The CEP was smoothened by radiculoplasty. Bony architecture in the furcation area revealed a definite horizontal component, with the vertical component extending up to and beyond the root apex of the RE.
After complete debridement, synthetic bone graft (CompactBone S, Dentegris International GmbH, dentegris.eu) was placed to fill the bony defect in the furcation area (Figure 8). Placement of the mucoperiosteal flaps to their original position was followed by placement of interrupted sutures and covering of the surgical area with periodontal dressing. The patient was given a prescription of analgesics for pain control and postsurgical instructions after the surgery.
One week later the patient was recalled for suture removal. Grade I mobility was noticed during the 1-month follow-up. A temporary bridge was placed to replace the missing tooth No. 31, using teeth Nos. 30 and 32 as abutments. After 2 months, the patient was reviewed again. There was no mobility observed after removal of the temporary bridge. With teeth Nos. 30 and 32 as abutments, a three-unit metal-ceramic bridge was placed to replace the missing tooth No. 31.
Follow-up
Follow-up of the patient at 3 months, 6 months (Figure 9 and Figure 10), and 9 months (Figure 11 and Figure 12) was uneventful. Grade I mobility had been detected at 1 month. Oral prophylaxis done at three monthly intervals and a prescription of interdental cleaning aids has helped the patient maintain oral hygiene. At the 9-month follow-up, probing depth at tooth No. 30 was 3 mm buccally and 4 mm lingually. Radiographs at 9 months (Figure 13) showed radioopacity around the distolingual root, an evidence of continued hard-tissue healing.
Discussion
This patient was of Chinese origin. Considered to be an Asiatic trait, prevalence of RE is around 5% to 31.5% in the Chinese population.4 Therefore, the finding of RE in patients of Chinese origin is not rare. With a huge Chinese population spread across the world, dental clinicians may very well encounter a case of RE when treating patients who are Chinese. Scientific literature reports more common occurrence of three-rooted mandibular molars among males and on the right side.2,3,10 In the present case, the patient was male and the involved molar was on the right side. Previous extraction of the mandibular left first molar was due to periodontal reasons. Therefore, it is possible that a three-rooted mandibular first molar may also have existed on the left side and was subsequently extracted, though further discussion on this would be speculative.
The patient was suffering from chronic generalized periodontitis with moderate periodontitis throughout the mouth. Severe periodontitis with deep pockets up to 10 mm was seen around the right mandibular first molar on both the buccal and lingual aspects. Presence of RE results in higher probing depths and additional loss of attachment, particularly at the distolingual site.8 Presence of CEP on the buccal side could have precipitated furcation involvement resulting in a deep periodontal pocket.11,12 According to the classification of CEP by Masters and Hoskins,13 the present case can be classified as grade III CEP, as the enamel projection in tooth No. 30 extended from the cementoenamel junction to the furcation. Presence of swollen gingiva and periodontal abscess masked the presence of CEP on the buccal side. CEP was noticed following shrinkage and recession of the gingiva, which led to exposure of the furcation area on the buccal side. Presence of diabetes mellitus also could have contributed to additional attachment loss and bone loss.
Despite the presence of advanced periodontitis as evidenced by deep pockets and significant bone loss noticed on radiographs, there was no mobility before treatment. Grade I mobility was noticed 1 month after periodontal surgery. This transient mobility subsided and the tooth was firm at 3, 6, and 9 months' follow-up. The presence of the RE increases the surface area for attachment of the periodontal apparatus and acts as a tripod, increasing the firmness of the tooth. Due to these factors, attempts should be made to save such compromised teeth. The most common method used to identify the presence of RE is to take intraoral periapical radiographs at two different angles. Advances in radiography in the form of cone-beam computed tomography have heightened the chances of clinicians identifying RE earlier and more accurately.14,15 Identification of RE in the initial stages of the periodontal disease could aid the clinician in treating the disease in a more minimally invasive manner.
In many instances diagnosing the case as either primarily periodontally involved or primarily endodontically involved may be difficult.16 The existence of a large composite restoration that has been present for many years could result in the secondary carious process encroaching the pulp resulting in primary endodontic involvement. Deep pocketing and advanced bone loss around the distolingual root or on the buccal side could result in primary periodontal involvement. Effective treatment of endodontic-periodontal lesions and treatment of compromised teeth with RE is challenging.17 Successful treatment of these teeth requires a multidisciplinary approach comprised of two stages: elimination of the endodontic infection and regeneration of the periodontal structures.17
In the present case, the treatment plan indeed involved endodontic therapy and regenerative surgical periodontal therapy. Endodontic-periodontal lesions and periodontal abscesses consist of anaerobic microorganisms, which necessitates the inclusion of adjunctive antibiotics.18 A combination of amoxicillin and clavulanic acid is effective in most odontogenic infections. The shape of the access cavity for a mandibular first molar with three canals is triangular. In the presence of RE, the access cavity is made trapezoidal to gain straight-line access.1 Therefore, to gain straight-line access to the fourth canal the access cavity in this case was made trapezoidal. Identification of the root canal orifice corresponding to the third root is crucial for successful management of these cases. Attempting to locate the RE root canal orifice without adequate knowledge of the internal anatomy of pulp space may result in iatrogenic furcal perforations.6,7
Periodontal surgery and complete degranulation exposed the CEP and bony defects. Despite the advanced amount of bone destruction, presence of the additional root converted the defect into a "cul-de-sac"-like defect. Presence of the additional root could help in preventing dislodgement of bone grafts from the lingual side.19 The decision to place bone graft without guided tissue regeneration membrane was based on the presence of buccal gingival recession. Despite the advanced periodontal destruction, the successful outcome of this case could be due to endodontic therapy, the firmness of the tooth (due to increased surface area for attachment and tripod effect), regular follow-ups, and optimal maintenance of oral hygiene by the patient.
Conclusion
With early identification and by following a multidisciplinary approach clinicians can successfully treat compromised three-rooted mandibular molars with CEP. Patients also need to sustain good oral hygiene and be compliant with regular maintenance visits.
About the Authors
J. Sylvia Western, MDS
Lecturer, Faculty of Dentistry, SEGi University, Malaysia
Vivek Vijay Gupta, MDS
Senior Lecturer, Faculty of Dentistry, SEGi University, Malaysia
Srinivas Sulugodu Ramachandra, MDS, PhD Student
School of Dentistry, University of Queensland, Australia; Faculty of Dentistry, SEGi University, Malaysia, at time of writing
References
1. De Moor RJ, Deroose CA, Calberson FL. The radix entomolaris in mandibular first molars: an endodontic challenge. Int Endod J. 2004;37(11):789-799.
2. Curzon ME. Three-rooted mandibular permanent molars in English Caucasians. J Dent Res. 1973;52(1):181.
3. Quackenbush LE. Mandibular molar with three distal root canals. Endod Dent Traumatol. 1986;2(1):48-49.
4. Yew SC, Chan K. A retrospective study of endodontically treated mandibular first molars in a Chinese population. J Endod. 1993;19(9):471-473.
5. Jones AW. The incidence of the three-rooted lower first permanent molar in Malay people. Singapore Dent J. 1980;5(1):15-17.
6. Srinivasan R, Bhagabati N, Rajput A, Akhtar S. Non surgical repair of iatrogenic furcal perforation of radix entomolaris. Med J Armed Forces India. 2015;71(suppl 2):S422-S424.
7. Mirikar P, Shenoy A, Mallikarjun GK. Nonsurgical management of endodontic mishaps in a case of radix entomolaris. J Conserv Dent. 2009;12(4):169-174.
8. Huang RY, Lin CD, Lee MS, et al. Mandibular disto-lingual root: a consideration in periodontal therapy. J Periodontol. 2007;78(8):1485-1490.
9. Chan HL, Oh TJ, Bashutski J, et al. Cervical enamel projections in unusual locations: a case report and mini-review. J Periodontol. 2010;81(5):789-795.
10. Somogyi-Csizmazia W, Simons AJ. Three-rooted mandibular first permanent molars in Alberta Indian children. J Can Dent Assoc (Tor). 1971;37(3):105-106.
11. Zee KY, Bratthall G. Prevalence of cervical enamel projection and its correlation with furcation involvement in eskimos dry skulls. Swed Dent J. 2003;27(1):43-48.
12. Bhusari P, Sugandhi A, Belludi SA, Khan S. Prevalence of enamel projections and its co-relation with furcation involvement in maxillary and mandibular molars: a study on dry skull. J Indian Soc Periodontol. 2013;17(5):601-604.
13. Masters DH, Hoskins SW Jr. Projection of cervical enamel into molar furcations. J Periodontol. 1964;35(1):49-53.
14. Silva EJ, Nejaim Y, Silva AV, et al. Evaluation of root canal configuration of mandibular molars in a Brazilian population by using cone-beam computed tomography: an in vivo study. J Endod. 2013;39(7):849-852.
15. Zhang R, Wang H, Tian YY, et al. Use of cone-beam computed tomography to evaluate root and canal morphology of mandibular molars in Chinese individuals. Int Endod J. 2011;44(11):990-999.
16. Al-Fouzan KS. A new classification of endodontic-periodontal lesions. Int J Dent. 2014;2014:919173. doi: 10.1155/2014/919173.
17. Grudianov AI, Makeeva MK. Endo-perio lesions prevalence and awareness of dentists about diagnostics and treatment. Stomatologiia (Mosk). 2014;93(3):11-14.
18. Grudianov AI, Makeeva MK, Piatgorskaia NV. Modern concepts of etiology, pathogenesis and treatment approaches to endo-perio lesions. Vestn Ross Akad Med Nauk. 2013;(8):34-36.
19. Sachdeva S, Phadnaik MB. Three-rooted mandibular first molar: a consideration in periodontal therapy. J Indian Soc Periodontol. 2012;16
(2):286-289.