Treatment of Advanced Periodontal Disease: Keys to Achieving Restoration Longevity
Yoshihiro Ono, DDS; Kimio Nakamura, DDS, PhD; and Sachiko Maeda, DDS, PhD
Abstract: Dental treatment for periodontally compromised patients can be highly complicated and challenging. This article addresses the effectiveness of contemporary periodontal treatment modalities by depicting clinical cases of periodontal restoration and health that have been maintained for 20 or more years. The cases incorporate four key steps vital to achieving successful treatment of chronic adult periodontitis: debridement, occlusal stabilization, pocket elimination, and maintenance. These cases demonstrate proof of principle that if the treatment is carefully planned and executed precisely, the natural dentition can be maintained for long periods of time even in periodontally compromised patients.
In dentistry, a shift in philosophy seems to be occurring favoring implant therapy rather than saving teeth. Scientific evidence supports implant therapy as a reliable treatment modality to replace lost teeth when they cannot be saved.1 Treatment modalities for peri-implantitis, however, remain unclear,2,3 and therefore serious problems may oftenresult. There are many treatment modalities for periodontitis, including nonsurgical and surgical approaches such as resective and regenerative therapies. Nevins reported that four steps are needed to achieve successful treatment of chronic adult periodontitis.4-6 The four steps are debridement, occlusal stabilization, pocket elimination, and maintenance. The present authors have applied these steps to cases of severe periodontitis in their practice for 35 years and have consistently achieved excellent outcomes.
Three clinical cases with advanced periodontal disease are presented here to demonstrate the efficacy of the concept and elucidate the importance of achieving longevity of treatment outcomes for periodontal disease. It should be noted that for these cases the recall maintenance was every 3 months and radiographs were updated every 2 to 3 years. All patients who completed the treatment also were required to wear biteguards.
Case 1
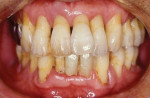
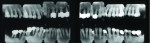
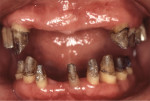
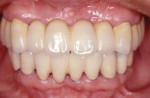
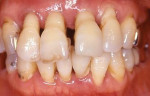
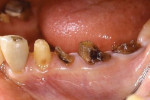
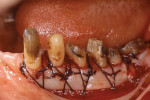
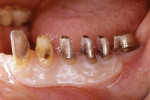
A 45-year-old male patient had been suffering from periodontal disease (Figure 1 and Figure 2). Extensive bone resorption was observed and all teeth were diagnosed as questionable to hopeless. The patient was adamant about wanting to save his teeth, thus it was decided to proceed with treatment without replacing any teeth with implants.
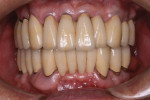
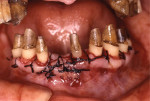
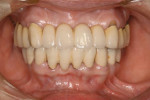
The concept of the four steps described above was utilized in this case. At the initial phase of treatment, complete debridement was done and hopeless teeth were eliminated. Then, all remaining dentition were splinted with full-arch splinted provisional restorations. Once occlusal stabilization was established, periodontal surgeries were performed to eliminate periodontal pockets. After healing, provisional restorations were relined to become the replica of the final prostheses. After delivery of the final prostheses, a nightguard was fabricated and the patient was placed on strict 3-month recalls (Figure 3).
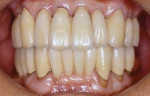
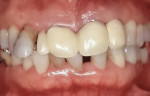
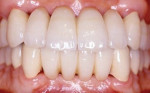
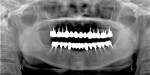
It was thought that the prostheses would be transitional, and the plan was to replace them with implant prostheses within 5 years. However, the patient has maintained the prostheses for 26 years and has never lost a single tooth since the treatment (Figure 4 and Figure 5).
Case 2
A 53-year-old woman's chief complaint was masticatory limitations due to tooth mobility. Severe bone loss and an irregular occlusal plane caused by pathologic tooth migration were recorded (Figure 6 and Figure 7).
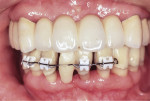
At the initial debridement phase, a cross-arch splinted provisional was provided to stabilize her bite. Hopeless teeth were removed and periodontal surgeries were performed, including osseous surgery and root resectioning for tooth No. 14 (Figure 8). After healing (Figure 9), orthodontic treatment was initiated for the mandibular arch to improve the occlusal plane (Figure 10).
Attachment loss can result in pathological migration, eg, pathological extrusion or inclination of teeth.7In such cases, orthodontic treatment should be provided in order to align the migrated teeth back into the proper position so the final prostheses can achieve the proper paralleling of abutment teeth, the proper posterior occlusal plane, and incisal guidance.
The final restoration for this patient was fabricated in 1991 (Figure 11). The prostheses were supported by all natural dentition and have been well maintained for 26 years (Figure 12 and Figure 13).
Case 3
A 50-year-old female patient presented seeking functional improvement without implant placement (Figure 14). The full-mouth radiographic series revealed generalized bone loss with severe bone loss in the anterior sextant (Figure 15).
At the initial phase treatment, the hopeless teeth in the anterior were removed and a full-arch splinted provisional was provided to replace the missing anterior teeth. Periodontal surgeries were carried out to access the root caries and eliminate osseous defects. The patient had very thin gingiva genetically and a narrow band of keratinized gingiva in general. Therefore, the flap preparation for osseous surgery was done with a partial-thickness flap so that a free gingival graft could be placed at the closure to enhance the width of the keratinized gingiva for the future prosthesis (Figure 16 through Figure 18). The other quadrants were treated in the same manner as this mandibular quadrant.
Full-arch final prostheses were delivered to the patient (Figure 19), and panoramic radiograph was updated 2 years after completion. A final panoramic radiograph was taken at the 20-year follow-up visit (Figure 20). Since the completion of the treatment, the patient has been well-maintained and no changes have been observed (Figure 21).
Discussion
Patients with severely compromised periodontal conditions often exhibit extensive malocclusion. Tooth malalignment can be a major cause of insufficient plaque control or traumatic occlusion and is a contributing factor to periodontal disease.8 Orthodontic treatment may benefit these patients by allowing improved oral hygiene, eliminating inflammatory elements, modifying osseous defects, and correcting occlusal trauma.9,10 Orthodontic tooth movement also can cause realignment of crowded or migrated incisors and reposition protrusive anterior teeth, which may be helpful for correcting esthetics.11
The treatment of periodontally compromised patients can be highly complicated and challenging. However, with careful planning and an interdisciplinary approach that encompasses periodontics, orthodontics, and restorative treatment, an excellent, enduring outcome can be achieved.
Some clinicians have reported that the prognosis for periodontally compromised patients is questionable and that implant treatment is a more reliable approach with a shorter treatment time.12 However, it could be argued that the opposite is true since there are increasing concerns with regard to peri-implantitis, especially in periodontally compromised patients,13 and because currently there is no scientific, dependable treatment modality for peri-implantitis.2,3
As shown in the three clinical cases presented, with careful planning utilizing four key steps-debridement, occlusal stabilization, pocket elimination, and maintenance-clinicians should be able to achieve a final outcome with no sulcus, bleeding on probing, vertical bone defects, or furcation involvement and with significant attached gingiva and stable occlusion. Doing so provides the patient with a cleanable periodontal environment, thus allowing patients themselves to easily maintain their prostheses and enhancing the long-term prognosis.
About the Authors
Yoshihiro Ono, DDS
Director, Japan Institute for Advanced Dental Studies (JIADS); Private Practice, periodontist, Tokyo and Osaka, Japan
Kimio Nakamura, DDS, PhD
Former Director, JIADS; Private Practice, prosthodontist, Osaka, Japan
Sachiko Maeda, DDS, PhD
Former Instructor, JIADS; Private Practice, orthodontist, Osaka, Japan
References
1. Kao RT. Strategic extraction: a paradigm shift that is changing our profession. J Periodontol. 2008;79(6):971-977.
2. Robertson K, Shahbazian T, MacLeod S. Treatment of peri-implantitis and the failing implant. Dent Clin North Am. 2015;59(2):
329-343.
3. Elemek E, Almas K. Peri-implantitis: etiology, diagnosis and treatment: an update. N Y State Dent J. 2014;80(1):26-32.
4. Nevins M. Long-term periodontal maintenance in private practice. J Clin Periodontol. 1996;23(3 Pt 2):273-277.
5. Nevins M, Skurow HM. The intracrevicular restorative margin, the biologic width, and the maintenance of the gingival margin. Int J Periodontics Rest Dent. 1984;4(3):30-49.
6. Nevins M. Periodontal pockets-predictable treatment. Compend Contin Educ Dent. 1999;20(5):467-472.
7. Towfighi PP, Brunsvold MA, Storey AT, et al. Pathologic migration of anterior teeth in patients with moderate to severe periodontitis. J Periodontol. 1997;68(10):967-972.
8. Alsulaiman AA, Kaye E, Jones J, et al. Incisor malalignment and the risk of periodontal disease progression. Am J Orthod Dentofacial Orthop. 2018;153(4):512-522.
9. Kessler M. Interrelationships between orthodontics and periodontics. Am J Orthod. 1976;70(2):154-172.
10. Ong MM, Wang HL. Periodontic and orthodontic treatment in adults. Am J Orthod Dentofacial Orthop. 2002;122(4):420-428.
11. Rosenberg MM, Kay HB, Keough BE, Holt RL. Periodontal and Prosthodontic Management for Advanced Cases. Chicago, IL: Quintessence Publishing; 1988:41-54.
12. Zitzmann NU, Krastl G, Hecker H, et al. Strategic considerations in treatment planning: deciding when to treat, extract, or replace a questionable tooth. J Prosthet Dent. 2010;104(2):80-91.
13. Heitz-Mayfield LJ. Peri-implant diseases: diagnosis and risk indicators. J Clin Periodontol. 2008;35(8 suppl):292-304.