Digital Workflow: From Guided Surgery to Final Full-Arch Implant Prosthesis in Three Visits
Panos Papaspyridakos, DDS, MS, PhD; Daniel Ben Yehuda, DDS; Neha Rajput, BDS; and Hans-Peter Weber, DMD, Dr. Med. Dent.
Abstract
The purpose of this article is to report a digital workflow protocol for full-arch implant rehabilitation from guided surgery to final prosthesis in only three visits. This expedited protocol allows for implant placement with a surgical template generated from preoperative virtual planning and production of the CAD/CAM prosthodontic rehabilitation using a digital workflow. At the first visit, a guided implant placement protocol with the All-on-4 concept and immediate loading with the conversion prosthesis technique was done. At the same visit, final impression and interocclusal records, cast verification and mounting, as well as digital scanning of the conversion prosthesis were carried out. During the second visit, the framework try-in was performed. Lastly, the third visit included delivery of the final full-arch prosthesis opposed by a maxillary complete denture.
Several concepts are currently used for the treatment of the edentulous jaw with dental implants, as advances such as rough implant surfaces, immediate loading protocols, digital dentistry, and CAD/CAM technology have had a significant impact on the evolution of implant dentistry.1-8 Digital technology is gaining popularity, and its applications translate into the so-called digital workflow.9 This workflow includes digital 3-dimensional (3D) imaging, computer-guided implant placement, digital impressions with intraoral scanner (IOS) systems, and CAD/CAM prosthodontics.10-12
This article describes a step-by-step digital workflow protocol that enables clinicians to perform guided implant placement and fabricate an immediately loaded provisional prosthesis and a final fixed prosthesis in only three visits.
Case Report
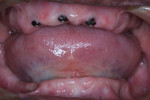
A 71-year-old edentulous man with complete dentures presented for implant consultation (Figure 1). Clinical and radiographic examination was performed, and the quality of the dentures was assessed and deemed unacceptable due to collapsed vertical dimension of occlusion (VDO) and poor esthetics. After being presented different treatment options, the patient selected fixed mandibular implant rehabilitation and a maxillary complete denture.
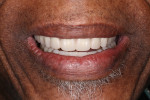
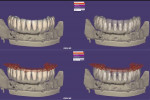
A new set of complete dentures was fabricated (Figure 2). A duplicate of the mandibular complete denture was used as a radiographic template for cone-beam computed tomography (CBCT) scanning using the dual-scan technique,10 followed by virtual implant planning using commercially available software (NobelClinician®, Nobel Biocare, nobelbiocare.com).10 Due to anatomic limitations and financial issues, the use of four axial and tilted implants (All-on-4 protocol) was implemented.
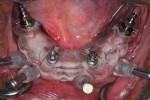
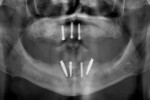
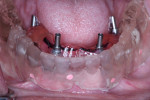
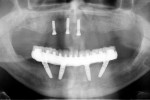
During the first clinical visit, guided surgery was performed following a strict surgical protocol in which four dental implants were placed (NobelGuide®, Nobel Biocare) in the mandible.13-15 Primary stability greater than 35 Ncm was achieved (Figure 3). After implant placement and profiling of the crestal bone, two straight and two 30-degree angled multi-unit abutments were torqued onto the implants.13-15 Temporary abutments were connected on the multi-unit abutments, and rubber dam was used to isolate the underlying soft tissue.10 After the mandibular denture was hollowed out, the temporary abutments were picked-up with acrylic resin using the conversion prosthesis technique.10 While the conversion prosthesis was being trimmed and contoured in the laboratory, two multi-unit abutment-level impressions were taken: one conventional impression (followed by digitization with a laboratory scanner) and a digital one with an IOS system (TRIOS®, 3Shape, 3shape.com). However, the impression used for fabrication of the final prosthesis was the conventional one after digitization with a laboratory scanner; this is because full-arch digital implant impressions with IOSs were not scientifically validated in 2016 during the treatment of this case.
The radiographic template, which was a denture duplicate, was first assessed for intimate fit with the soft tissue to confirm adequate fit. This template was used for the conventional impression, as a custom tray with polyether material used as a wash was employed to take the final impression. The radiographic template-custom tray simultaneously recorded the VDO and centric relation (Figure 4).10 Prior to the impression, the VDO was recorded with the use of soft-tissue landmarks (tip of the nose and chin point), while the patient was in occlusion with the denture. The same soft-tissue landmarks were maintained during the fit of the radiographic template (duplicate of the denture) so as not to increase the VDO while maintaining adequate soft-tissue contact without the presence of impression material that might otherwise increase the VDO.
The impression was poured in type IV stone. A facebow transfer was used to articulate the maxillary cast on a semi-adjustable articulator, and the mandibular working cast was cross-articulated with the aid of the radiographic template-custom tray (Figure 5).The mandibular working cast and the conversion prosthesis were digitally scanned with an extraoral scanner (Activity 880, Smart Optics, smartoptics.de) and standard tesselation language (STL) files were saved.
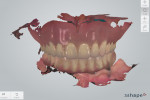
For the digital impression, scan bodies were tightened onto the multi-unit abutments and an intraoral digital impression was made using an IOS system (TRIOS). Subsequently, the conversion prosthesis was delivered to the patient with postoperative instructions on how to clean it and maintain a soft diet for the next 8 weeks. A second intraoral digital impression of the conversion prosthesis was made using the same IOS system (TRIOS). The STL files from intraoral scanning of the implants and the conversion prosthesis were also saved (Figure 6).
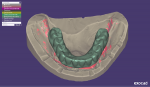
The previously generated STL files from conventional and digital impressions were imported into a CAD software (Exocad® DentalCAD, Exocad, exocad.com), and the files were made to overlap each other (Figure 7).10-12 Virtual cutback was performed with the CAD software to create a screw-retained framework with individual abutment preparations for multiple single crowns in a digital workflow. This virtually designed framework was sent to a CAM facility (NobelProcera®, Nobel Biocare), where the definitive framework was milled from titanium block.
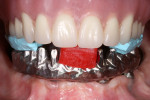
At the second clinical visit, which occurred after 8 weeks of uneventful healing, the patient presented for try-in of the titanium framework. The accuracy of fit was confirmed clinically and radiographically.10,12 Interocclusal records were taken again for the purpose of mounting verification (Figure 8). Shade selection for the gingiva and teeth also was done.
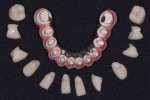
In the laboratory, the titanium framework was digitally scanned with the extraoral scanner (Activity 880), and the STL file was overlapped with the previous STL file of the conversion prosthesis, which had been saved into the CAD software (Exocad DentalCAD).10,12 With the aid of the CAD software, single crowns were digitally designed, and they were milled on a CAM milling unit (Tizian Cut Eco plus, Schuetz Dental, schuetz-dental.de/en) from prefabricated lithium-disilicate blocks (Figure 9 and Figure 10).10,12,16 Gingiva-colored composite resin (GRADIA®, GC America, gcamerica.com) was used. The lithium-disilicate single crowns were etched for 20 seconds with 4.9% hydrofluoric acid, rinsed with water for 1 minute, and air-dried with oil-free air.10,16 Then, silane coupling agent (Clearfil™ Ceramic Primer, Kuraray, kuraray.com) was applied on the crowns before adhesive cementation was performed with self-adhesive resin cement (Clearfil™ SA Cement, Kuraray).
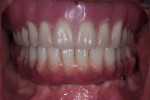
During the third clinical visit, the screw-retained titanium framework with cemented single crowns on individual abutments was inserted.10,16 The final prosthesis was torqued at the multi-unit abutments at 15Ncm, and the screw-access holes were filled with Teflon tape and composite resin (Filtek™ Z250, 3M ESPE, 3m.com). Oral hygiene instructions were given to the patient to help him clean around the prosthesis.
The 1-year clinical and radiographic follow-up showed a stable outcome (Figure 11 and Figure 12). The patient was so satisfied that he expressed his desire to undergo fixed implant rehabilitation in the maxilla as well.
Discussion
The application of digital technology in implant prosthodontics has aided in simplifying many of the steps involved in full-arch implant rehabilitation. In the present case, a digital workflow was used with a three-visit treatment protocol. Ercoli et al showed how to manage the impression, maxillo-mandibular relationship, and cast articulation in a single appointment through conventional workflow.17 They conducted a retrospective study with 48 edentulous arches treated with either an experimental or conventional technique. For the experimental technique, prosthesis fabrication and delivery required an average of four appointments, while the conventional technique required an average of 7.8 appointments to deliver the definitive prosthesis. The prostheses fabricated with the experimental technique showed a clinically passive fit on the implants in 17 of 18 arches. The frameworks fabricated with the conventional technique achieved a clinically passive fit in 18 of 30 arches.17
The present report shows how the digital workflow can be used to efficiently streamline and expedite implant treatment for an edentulous predicament. With the presented protocol, chairside time is reduced, the cost of implant treatment may be lowered, and treatment acceptance may potentially be increased.10 The primary advantage of this expedited protocol is that all the information necessary for final prosthesis fabrication is acquired from the radiographic template-custom tray impression and the conversion prosthesis at the first visit.10 The digital scanning of the conversion prosthesis and the master cast leads to STL files that can be imported into CAD software, simplifying the design and fabrication of the final prosthesis. The use of computer-guided 3D implant planning and tilted implants offers an alternative to extensive grafting and has been shown to achieve favorable long-term outcomes.10-15 It should be noted that this case involved a patient whose situation was well-suited for this treatment concept, ie, there were no or minimal issues concerning vertical dimension, bone volume, or restorative space requirements.
The digital workflow for implant planning and placement implemented in the present patient treatment was important in achieving prosthodontically driven implant positioning with clinical accuracy. Guided implant surgery was followed by immediate implant loading. During the treatment of this patient in 2016, digital impressions with IOSs were not scientifically validated.10 Hence, two impressions were taken: a conventional impression (followed by digitization with a laboratory scanner) and a digital one (using a TRIOS scanner). The impression used for fabrication of the final prosthesis was the conventional one after digitization with a laboratory scanner, as at the time of treatment the technology did not allow for the utilization of the STL file from the digital impression. Comparative studies are currently emerging showing that full-arch digital implant impressions (with TRIOS, CEREC Omnicam [Dentsply Sirona, sirona.com], and True Definition [3M ESPE] scanners) display the same accuracy or better as those produced conventionally.18-20 Additionally, recent advances demonstrate that STL files from full-arch digital implant impressions can be imported into CAD software and facilitate the fabrication of polymethyl methacrylate (PMMA) prototypes and final prostheses.10 The clinical implications suggest that a complete digital workflow for rehabilitation with full-arch implant prostheses is not yet attainable but could be in the near future.5
Regarding prosthetic materials and design, gold or titanium frameworks veneered with acrylic resin have been used for full-arch implant rehabilitation.21-24 A significant number of technical complications have been reported, such as prosthetic material chipping and fracture, prompting the emergence of newer prosthodontic concepts in efforts to reduce such problems.7,8,10,16,21,25 These concepts include the use of one-piece, screw-retained titanium frameworks with abutment preparations and individual single crowns, and the use of monolithic ceramics with partial or no veneering.8,10,16 The monolithic prosthetic design with either lithium-disilicate or zirconia has been reported to obtain satisfactory esthetic results. In regard to full-arch implant rehabilitation with individual monolithic single crowns on titanium frameworks, a study reported satisfactory clinical outcomes at up to 10 years of follow-up.10
Summary
Computer-guided surgery and digital technology have radically heightened the possibility of optimally using available bone for implant support, reducing the need for extensive grafting procedures and allowing for prosthodontically driven implant placement in the atrophic mandible. This three-visitprotocol enables accurate placement of implants using a flapless technique with the guidance of a surgical template generated from preoperative virtual implant planning and CAD/CAM prosthodontic rehabilitation using a digital workflow.
Acknowledgment
The authors would like to thank Mr. Yukio Kudara, Division of Postgraduate Prosthodontics, Tufts University School of Dental Medicine, for his expertise in the CAD/CAM fabrication of the final prosthesis.
About the Authors
Panos Papaspyridakos, DDS, MS, PhD
Assistant Professor, Division of Postgraduate Prosthodontics, Tufts University School of Dental Medicine, Boston, Massachusetts
Daniel Ben Yehuda, DDS
Resident, Division of Postgraduate Prosthodontics, Tufts University School of Dental Medicine, Boston, Massachusetts
Neha Rajput, BDS
Resident, Division of Postgraduate Prosthodontics, Tufts University School of Dental Medicine, Boston, Massachusetts
Hans-Peter Weber, DMD, Dr. Med. Dent.
Professor and Chairman, Division of Postgraduate Prosthodontics, Tufts University School of Dental Medicine, Boston, Massachusetts
References
1. Gallucci GO, Benic GI, Eckert SE, et al. Consensus statements and clinical recommendations for implant loading protocols. Int J Oral Maxillofac Implants.2014;29(suppl):287-290.
2. Papaspyridakos P, Chen CJ, Chuang SK, Weber HP. Implant loading protocols for edentulous patients with fixed prostheses: a systematic review and meta-analysis. Int J Oral Maxillofac Implants.2014;29(suppl):256-270.
3. Malo P, de Araújo Nobre M, Lopes A, et al. All-on-4® treatment concept for the rehabilitation of the completely edentulous mandible: a 7-year clinical and 5-year radiographic retrospective case series with risk assessment for implant failure and marginal bone level. Clin Implant Dent Relat Res.2015;17(suppl 2):e531-e541.
4. Balshi TJ, Wolfinger GJ, Stein BE, Balshi SF. A long-term retrospective analysis of survival rates of implants in the mandible. Int J Oral Maxillofac Implants. 2015;30(6):1348-1354.
5. Monaco C, Ragazzini N, Scheda L, Evangelisti E. A fully digital approach to replicate functional and aesthetic parameters in implant-supported full-arch rehabilitation. J Prosthodont Res. 2017;S1883-1958(17)30114-30117.
6. Wismeijer D, Brägger U, Evans C, et al. Consensus statements and recommended clinical procedures regarding restorative materials and techniques for implant dentistry. Int J Oral Maxillofac Implants. 2014;29(suppl):137-140.
7. Abdulmajeed AA, Lim KG, Närhi TO, Cooper LF. Complete-arch implant-supported monolithic zirconia fixed dental prostheses: a systematic review. J Prosthet Dent. 2016;115(6):672-677.
8. Malo P, de Araújo Nobre M, Borges J, Almeida R. Retrievable metal ceramic implant-supported fixed prostheses with milled titanium frameworks and all-ceramic crowns: retrospective clinical study with up to 10 years of follow-up. J Prosthodont. 2012;21(4):256-264.
9. Chochlidakis KM, Papaspyridakos P, Geminiani A, et al. Digital versus conventional impressions for fixed prosthodontics: a systematic review and meta-analysis. JProsthet Dent. 2016;116(2):184-190.
10. Papaspyridakos P, Rajput N, Kudara Y, Weber HP. Digital workflow for fixed implant rehabilitation of an extremely atrophic edentulous mandible in three appointments. J Esthet Restor Dent. 2017;29(3):178-188.
11. Papaspyridakos P, Kang K, DeFuria C, et al. Digital workflow in full-arch implant rehabilitation with segmented minimally veneered monolithic zirconia fixed dental prostheses: 2-year clinical follow-up. J Esthet Restor Dent.2018;30(1):5-13.
12. Amin S, Weber HP, Kudara Y, Papaspyridakos P. Full-mouth implant rehabilitation with monolithic zirconia: benefits and limitations. Compend Contin Educ Dent.2017;38(1):e1-e4.
13. Lopes A, Maló P, de Araújo Nobre M, et al. The NobelGuide® All-on-4® treatment concept for rehabilitation of edentulous jaws: A retrospective report on the 7-years clinical and 5-years radiographic outcomes. Clin Implant Dent Relat Res. 2017;19(2):233-244.
14. Yamada J, Kori H, Tsukiyama Y, et al. Immediate loading of complete-arch fixed prostheses for edentulous maxillae after flapless guided implant placement: a 1-year prospective clinical study. Int J Oral Maxillofac Implants. 2015;30(1):184-193.
15. Meloni SM, Tallarico M, Pisano M, et al. Immediate loading of fixed complete denture prosthesis supported by 4-8 implants placed using guided surgery: a 5-year prospective study on 66 patients with 356 implants. Clin Implant Dent Relat Res. 2017;19(1):195-206.
16. Malo P, de Sousa ST, de Araújo Nobre M, et al. Individual lithium disilicate crowns in a full-arch, implant-supported rehabilitation: a clinical report. J Prosthodont.2014;23(6):495-500.
17. Ercoli C, Geminiani A, Lee H, et al. Restoration of immediately loaded implants in a minimal number of appointments: a retrospective study of clinical effectiveness. Int J Oral Maxillofac Implants. 2012;27(6):1527-1533.
18. Papaspyridakos P, Gallucci GO, Chen CJ, et al. Digital versus conventional implant impressions for edentulous patients: accuracy outcomes. Clin Oral Implants Res.2016;27(4):465-472.
19. Amin S, Weber HP, Finkelman M, et al. Digital versus conventional full-arch implant impressions: a comparative study. Clin Oral Implants Res. 2017;28(11):1360-1367.
20. Vandenweghe S, Vervack V, Dierens M, De Bruyn H. Accuracy of digital impressions of multiple dental implants: an in-vitro study. Clin Oral Implants Res. 2017;28(6):648-653.
21. Papaspyridakos P, Chen CJ, Chuang SK, et al. A systematic review of biologic and technical complications with fixed implant rehabilitations for edentulous patients. Int J Oral Maxillofac Implants. 2012;27(1):102-110.
22. Balshi TJ, Wolfinger GJ, Alfano SG, Balshi SF. The retread: a definition and retrospective analysis of 205 implant-supported fixed prostheses. Int J Prosthodont. 2016;29(2):126-131.
23. Drago C. Ratios of cantilever lengths and anterior-posterior spreads of definitive hybrid full-arch, screw-retained prostheses: results of a clinical study. J Prosthodont. 2018;27(5):402-408.
24. Krennmair S, Weinländer M, Malek M, et al. Mandibular full-arch fixed prostheses supported on 4 implants with either axial or tilted distal implants: a 3-year prospective study. Clin Implant Dent Relat Res. 2016;18(6):1119-1133.
25. Malo P, de Araujo Nobre MA, Guedes CM, Almeida R. Outcomes of immediate function implant prosthetic restorations with mechanical complications: a retrospective clinical study with 5 years of follow-up. Eur J Prosthodont Restor Dent. 2017;25(1):26-34.