Autotransplantation: An Alternative to Dental Implants— Case Report With 4-Year Follow-Up
Toyoaki Kobayashi, DDS; and Markus B. Blatz, DMD, PhD
Abstract
Autotransplantation can be a viable alternative to dental implant placement for partially edentulous patients when case selection and surgical procedures are performed properly. Moreover, in the event of a failed autotransplantation, implant placement may still be possible. Autotransplantation offers several benefits compared with dental implants, however the surgical procedure is technique sensitive. This case report demonstrates the clinical steps and healing process of an autotransplanted third molar tooth with complete root formation with a 4-year follow-up.
While tooth transplantation between individuals has been performed for hundreds of years, autotransplantation was first described in the 1950s.1 Autotransplantation, however, is rarely considered as an option for partially edentulous patients. Conversely, implant therapy has become routine in dentistry and has developed significantly over the past several decades. Jung and coworkers reported that survival of implants supporting single crowns at 5 years amounted to 97.2%, and 95.2% at 10 years.2
Although the survival rate is very high, peri-implantitis has become a primary complication in dental implant therapy.3-5 Many dentists and researchers have endeavored to prevent and treat peri-implantitis, but a consensus on proper management has not yet been established.3-5 Derks and Tomasi estimated the weighted mean prevalence of peri-implant mucositis and peri-implantitis at 43% and 22%, respectively.6 The meta-regression showed a positive relationship between prevalence of peri-implantitis and time of function. In other words, the longer the implant is in the mouth, the higher the risk of peri-implantitis.
With another option, dentists may be able to delay the time of implant placement in cases of severe tooth destruction. One alternative is autotransplantation, which is transplantation of a patient's own embedded, impacted, or erupted tooth or teeth from one site to another, into extraction sites or surgically prepared sockets.7 Several researchers assessed clinical outcomes of autotransplanted teeth with complete root formation, and the survival rates were 81.4% to ~100%.8-15 In addition, periodontal ligament (PDL) management is key for successful autotransplantation.16 With proper case selection and correct surgical procedures, survival rates with autotransplantation are fairly high.7-17 Even if the autotransplantation fails, implant placement may still be possible.
This case report demonstrates the clinical steps and healing process of an autotransplanted third molar tooth with complete root formation with a 4-year follow-up.
Case Presentation
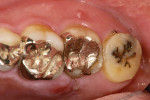
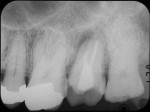
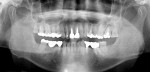
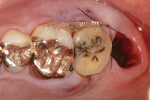
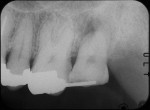
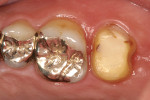
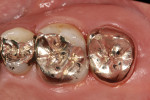
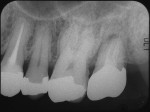
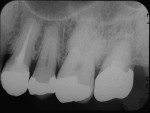
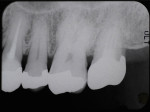
A 50-year-old male patient presented with discomfort in the left upper jaw. He was a nonsmoker with moderate plaque control, and his medical history revealed no problems. After clinical and radiographic examinations, a root fracture was observed on tooth No. 15, which had been endodontically treated and restored with a cast metal inlay (Figure 1 and Figure 2). After a detailed examination, the situation was explained to the patient and autotransplantation was suggested as the preferred treatment. Because the patient had a nonfunctional wisdom tooth No. 16 that had no periodontal pathologies and a root morphology that was similar to No. 15, it was determined that it would be an adequate donor tooth (Figure 3).
Clinical Procedures
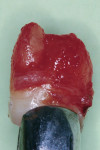
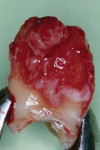
First, tooth No. 16 was extracted (Figure 4) under local anesthesia with a minimally invasive approach to prevent damage to the PDL on the root surface. The tooth was then submerged in a tooth storage solution (Teeth Keeper NEO, Neo Dental Chemical Products Co., LTD, neo-dental.com) in a sterile container. Subsequently, tooth No. 15 was extracted (Figure 5), and infected granulation tissue was carefully removed from the extraction socket. To fit the donor tooth into the socket, the bone housing was prepared using a stainless-steel round bur at low speed under copious irrigation with saline.
Tooth No. 16 was placed lightly into the prepared socket and fit well. It should be noted that to avoid damaging the PDL the root should not contact the extraction socket walls.Next, suturing with 4-0 nylon suture (MANI, mani.co.jp) was performed on the distal aspect to ensure close adaptation of the gingival flap around the donor tooth. The donor tooth was then splinted to No. 14 with a 0.9-mm cobalt-chrome metal wire (Sun-Cobalt Clasp-Wire, DENTSPLY-Sankin, dentsply-sankin.com) and methyl methacrylate (MMA)-based adhesive resin cement (Super-Bond C&B, Sun Medical, sunmedical.co.jp) to minimize micromovement (Figure 6 and Figure 7). Generally, any cement that stabilizes the donor tooth in the socket can be used. There were no occlusal contacts at this stage.
Like in the present case, it is recommended that the patient chew on the other side of the mouth as much as possible for at least 2 weeks, as it has been reported that for optimal PDL healing to occur, reattachment between the connective tissues of the root and the recipient socket wall requires 2 weeks.16The splint should remain stable, and no occlusal contacts should occur during this time. The patient used a mouthwash for the donor tooth for 2 weeks, and after that he brushed the donor tooth.
Four weeks after the surgery, endodontic treatment was performed. Because the donor tooth had complete root formation within less than 1 mm of the apical foramen, endodontic treatment was needed 3 to 4 weeks after surgery to avoid pulp infection.8 This is because if the apical foramen is within less than 1 mm of the root, the pulp becomes nonvital after the surgery, and pulp infection can cause inflammatory root resorption. Thus, endodontic treatment should be done within this time period to avoid root resorption. Because the key to successful autotransplantation is PDL management, less time extraorally means less PDL damage. Compared to a re-implantation technique, a properly selected donor tooth for autotransplantation does not have any pulp infection.
With regard to bone healing, in autotransplantation the healing of the PDL is the higher priority. Once favorable PDL healing is achieved, it is anticipated that favorable bone healing will follow. The splint was removed after the root canal treatment (Figure 8), as wire splinting for a long duration may increase the risk of tooth ankylosis.9
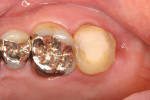
Three months after the autotransplantation surgery, the transplanted tooth was evaluated using mobility testing and periodontal probing. Favorable healing was obtained and a provisional crown was temporarily cemented. Re-evaluation 8 months after the surgery through clinical and radiograph examinations revealed no periodontal or functional problems. A definitive impression for final restoration fabrication was made (Figure 9). A cast metal crown was selected for the final restoration, as the tooth was not in the esthetic zone and fracture by occlusal trauma should be avoided (Figure 10). Occlusal contacts were marked with articulating paper and adjustments were made to ensure adequate occlusion.
Radiography showed a large space between the donor tooth and the alveolar bone on the day of the autotransplantation. However, this space was reduced over time due to new bone formation (Figure 11 through Figure 13). After 4 years of follow-up, no functional or periodontal problems were observed and the patient was satisfied with the result.
Discussion
This case report described the autotransplantation of a third molar tooth with complete root formation with a 4-year follow-up. Mejare and coworkers investigated 50 autotransplanted third molar teeth with complete root formation and reported that the cumulative survival rate during the 4-year follow-up was 81.4%.10 Chung and coworkers investigated autotransplanted teeth with complete root formation and showed the 5-year estimated survival rate to be 90.5% while root resorption and ankylosis rates were 2.1% and 1.2%, respectively.9 The survival rate was high and the complication rates low.
Autotransplantation offers several benefits. One is its suitability for use in growing adolescents when adequate donor teeth are available. In general, implant therapy should be avoided in growing adolescents because the implant does not erupt along with the adjacent teeth. Also, in contrast to osseointegrated implants, autotransplanted teeth can be moved orthodontically. Kokai and coworkers investigated 100 autotransplanted teeth with complete root formation with subsequent orthodontic force.11 They reported that the survival rate was 93% for a mean observation time of 5.8 years and concluded that the early orthodontic force may increase the success rate when proper surgical treatment is performed. Other benefits are that a successful autotransplanted tooth has normal proprioception just as natural adjacent teeth do, and the autotransplanted tooth preserves and promotes alveolar bone volume. Additionally, gingival contour is often better than that around a dental implant.
Despite these benefits, autotransplantation is rarely considered as an option for partially edentulous patients because the procedure is technique sensitive. Additionally, in the past, before dental implants were an option, one could speculate that autotransplantation may have often failed due to improper case selection and incorrect clinical treatment, which may have further prompted clinicians to avoid the procedure. Also, compared with dental implants, indications for autotransplantation are limited. For example, if the donor tooth is conical and the extracted tooth is multirooted with a distinct furcation, this would make the procedure more difficult. In such a case, the extraction of the donor tooth and the fitting procedure into the extracted socket would be somewhat complicated. Whether a donor tooth has a conical root or multiple roots, the clinician should carefully consider the case selection, because, to reiterate, favorable PDL healing is the critical factor for success. Yet another reason why this procedure is not readily considered may be that, despite its benefits, dental schools typically do not teach it in detail.
To increase the survival rate and decrease complications, Tsukiboshi suggested that PDL management is vital for success.16 He proposed that there were two main reasons why PDL damage was caused during this surgery: the difficulty in attempting to fit the donor tooth into the socket in the proper position, and extended extraoral time. Should these two factors be improved, a better survival rate may be achievable. Digital technologies, including cone-beam computed tomography (CBCT) and 3-dimensional (3D) printing can be employed to fabricate a replica of the donor tooth. Verweij et al reported that by using a donor tooth replica produced by CBCT and 3D printing during surgery, the authors needed only one attempt to fit the donor tooth into the socket and dramatically reduced extraoral time to less than 1 minute.17
Therefore, use of CBCT and a replica donor tooth may potentially improve the survival and success rates further. Even if an autotransplanted tooth fails at a later stage, implant therapy usually may still be performed. Autotransplantation can be considered as an alternative to dental implant placement and a well-documented treatment approach with high success rates when appropriate parameters are followed.
Conclusion
This case report demonstrated that tooth autotransplantation can be a viable treatment option when adequate donor teeth are available. Proper case selection and correct clinical treatment that includes suitable PDL healing are essential for long-term success.
About the Authors
Toyoaki Kobayashi, DDS
Visiting Scholar, Department of Preventive and Restorative Sciences, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania
Markus B. Blatz, DMD, PhD
Professor of Restorative Dentistry, Chairman, Department of Preventive and Restorative Sciences, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania
References
1. Cross D, El-Angbawi A, McLaughlin P, et al. Developments in autotransplantation of teeth. Surgeon. 2013;11(1):49-55.
2. Jung RE, Zembic A, Pjetursson BE, et al. Systematic review of the survival rate and the incidence of biological, technical, and aesthetic complications of single crowns on implants reported in longitudinal studies with a mean follow-up of 5 years. Clin Oral Implants Res. 2012;23(suppl 6):2-21.
3. Figuero E, Graziani F, Sanz I, et al. Management of peri-implant mucositis and peri-implantitis. Periodontol 2000. 2014;66(1):255-273.
4. Heitz-Mayfield LJ, Mombelli A. The therapy of peri-implantitis: a systematic review. Int J Oral Maxillofac Implants. 2014;29(suppl):325-345.
5. Mahato N, Wu X, Wang L. Management of peri-implantitis: a systematic review, 2010-2015. Springerplus. 2016;5:105.
6. Derks J, Tomasi C. Peri-implant health and disease. A systematic review of current epidemiology. J Clin Periodontol. 2015;42(suppl 16):S158-S171.
7. Natiella JR, Armitage JE, Greene GW. The replantation and transplantation of teeth. A review. Oral Surg Oral Med Oral Pathol. 1970;29(3):397-419.
8. Sugai T, Yoshizawa M, Kobayashi T, et al. Clinical study on prognostic factors for autotransplantation of teeth with complete root formation. Int J Oral Maxillofac Surg. 2010;39(12):1193-1203.
9. Chung WC, Tu YK, Lin YH, Lu HK. Outcomes of autotransplanted teeth with complete root formation: a systematic review and meta-analysis. J Clin Periodontol. 2014;41(4):412-423.
10. Mejare B, Wannfors K, Jansson L. A prospective study on transplantation of third molars with complete root formation. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2004;97(2):231-238.
11. Kokai S, Kanno Z, Koike S, et al. Retrospective study of 100 autotransplanted teeth with complete root formation and subsequent orthodontic treatment. Am J Orthod Dentofacial Orthop. 2015;148(6):982-989.
12. Akiyama Y, Fukuda H, Hashimoto K. A clinical and radiographic study of 25 autotransplanted third molars. J Oral Rehabil. 1998;25(8):640-644.
13. Bae JH, Choi YH, Cho BH, et al. Autotransplantation of teeth with complete root formation: a case series. J Endod. 2010;36(8):1422-1426.
14. Jang Y, Choi YJ, Lee SJ, et al. Prognostic factors for clinical outcomes in autotransplantation of teeth with complete root formation: survival analysis for up to 12 years. J Endod. 2016;42(2):198-205.
15. Watanabe Y, Mohri T, Takeyama M, et al. Long-term observation of autotransplanted teeth with complete root formation in orthodontic patients. Am J Orthod Dentofacial Orthop. 2010;138(6):720-726.
16. Tsukiboshi M. Autotransplantation of teeth: requirements for predictable success. Dent Traumatol. 2002;18(4):157-180.
17. Verweij JP, Moin DA, Mensink G, et al. Autotransplantation of premolars with a 3-dimensional printed titanium replica of the donor tooth functioning as a surgical guide: proof of concept. J Oral Maxillofac Surg. 2016;74(6):1114-1119.