Importance of Prototype Use for Implant-Supported Complete Fixed Dental Prosthesis (ICFDP)
Jonathan H. Dawson, DMD, MSD; Grady Dix, CDT; Bryan T. Harris, DMD; and Wei-Shao Lin, DDS
Abstract
Restorative material options for implant-supported complete fixed dental prostheses (ICFDP) have progressed from traditional metal-acrylic or metal-ceramic combinations to today's monolithic zirconia or high-performance polymer designs. To avoid potential errors that may be introduced into the restorative process in the interim phase and to provide a more predictable clinical outcome of the definitive ICFDP, a clinical protocol utilizing a prototype prosthesis is described in this case report.
Having to make excessive adjustments on zirconia or ceramic definitive restorations may induce damage and reduce the strength of the prosthesis. Hence, such restorative materials are less forgiving for clinicians during clinical impression and record-taking procedures. The need for obtaining accurate clinical records and communicating effectively with the dental laboratory technicians becomes increasingly important for dental clinicians when zirconia or ceramic is the chosen restorative material.
The options of restorative materials for an implant-supported complete fixed dental prosthesis (ICFDP), commonly referred to as a full-arch implant hybrid prosthesis, have evolved recently from traditional metal-acrylic or metal-ceramic combinations to presently used monolithic zirconia or high-performance polymer designs. When treating patients with an ICFDP, an interim removable denture is often converted into an interim ICFDP.1 This interim ICFDP can be utilized throughout the healing period after dental implant placement and provide a reference for the diagnostic tooth arrangement of the definitive ICFDP. After obtaining the definitive impression and facebow and maxillomandibular relation record, a trial insertion of the diagnostic tooth arrangement is then completed prior to the fabrication of the definitive framework and ICFDP.2,3
Throughout the aforementioned process, possible errors may be introduced during the various steps, such as inaccurate maxillomandibular relation record or denture teeth movement in the diagnostic tooth arrangement. To provide a more predictable clinical outcome on a definitive ICFDP fabricated with new, less forgiving restorative materials, this report describes a clinical protocol of the use of a prototype prosthesis.
Clinical Report
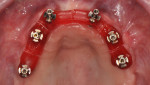
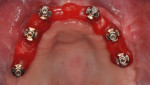
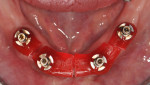
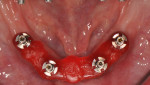
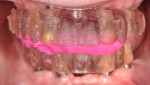
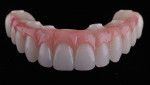
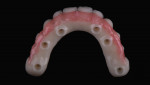
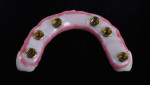
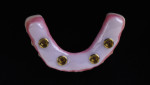
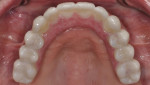
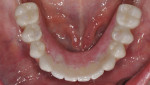
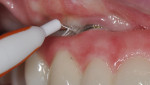
In this case, maxillary and mandibular definitive monolithic zirconia ICFDP were planned using digital prosthetic planning prior to implant surgery.4-6 The implant surgery was completed with delayed placement and immediate loading protocol. The patient presented in the prosthodontics clinic after implant surgery to begin clinical appointments for the definitive prostheses. The verification devices were made with Pattern Resin™ (GC America, gcamerica.com) and allowed to polymerize for 24 hours prior to the definitive impression appointment.7 The segmented verification devices were inserted intraorally with 15 Ncm onto screw-retained abutments, and reconnected together with Pattern Resin (Figure 1 through Figure 4).
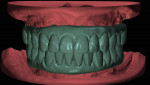
A custom tray was then used to make an abutment-level definitive impression with polyvinyl siloxane material (Virtual® XD, Ivoclar Vivadent, ivoclarvivadent.com). Verified master casts were poured with type IV dental stone (ResinRock, Whip Mix Corp., whipmix.com). Clear duplicates of the interim ICFDP prostheses were replaced on the verified master casts and used to articulate these casts using the facebow and maxillomandibular relation records (Figure 5). By using duplicate prostheses, the proposed changes to tooth position and occlusal plane were communicated to the laboratory for a wax trial insertion to verify those changes (Figure 6). With the patient's approval of functional and esthetic outcomes, the wax trial insertion can be rearticulated with a new occlusal record if necessary, and sent back to the dental laboratory for CAD/CAM prototype fabrication.
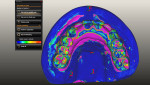
The dental laboratory technician can host a virtual Internet-based meeting for clinicians' review and approval of the CAD/CAM prototype design prior to the milling of polymethyl methacrylate (PMMA) prototypes (Figure 7). At this stage, the goal of the dental technician is to provide all of the details required on the definitive prostheses, such as convex-shaped soft-tissue contours necessary for the patient to be able to maintain optimal oral hygiene.
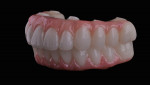
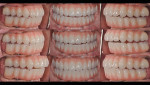
After obtaining the clinician's approval, the dental technician milled the PMMA prototypes in the desired shade and finished the milled prototypes with layered pink composite resin to mimic soft tissue (Figure 8 through Figure 10). The completed prototypes were delivered after occlusal adjustments were made to achieve desired occlusal contacts. Not only were the centric occlusal contacts achieved, but all the eccentric occlusal contacts also were verified to achieve the preferred occlusal scheme (Figure 11). The patient was dismissed to function with the prototypes for 4 weeks to allow any possible wear patterns to be introduced onto the occlusal surfaces of the prototypes.
In addition to testing for function, the patient was able to thoroughly test the phonetics and oral hygiene regimens with the convex intaglio surfaces provided by the prototype. The patient did not report or demonstrate any phonetic or hygienic issues. An ovate contour in the incisor area provided tissue contact and air seal. All ICFDP should maintain convex hygienic contours at the intaglio surfaces and should not have a flange or ridgelap design because of the hygienic and maintenance issues that can arise from these contours.
After 4 weeks of occlusal function, the prototypes were removed and the previous interim ICFDP were replaced onto the patient. The prototypes were sent back to the dental laboratory for the fabrication of the monolithic zirconia definitive prostheses. The dental laboratory technician then scanned the occlusal surfaces of the prototypes, which were modified based on the clinical occlusal adjustments and/or the patient's occlusal functions (Figure 12). Once the changes were made in the CAD software (Zirkonzahn, zirkonzahn.com), the full-contour monolithic zirconia definitive prostheses were milled.
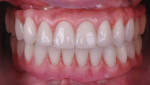
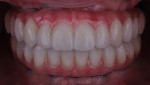
The final prostheses had highly polished intaglio tissue surfaces, and convex contours from the design were maintained (Figure 13 and Figure 14). It should be noted that the titanium inserts were luted into the zirconia prostheses on the master cast in the dental laboratory. Insertion of the definitive prostheses was completed by torqueing the prosthetic screws to the abutments at 15 Ncm and sealing the screw access with teflon tape and composite resin (Figure 15 and Figure 16). Final occlusal check was completed with shimstock to validate the occlusal contacts for the occlusion desired. Homecare oral hygiene regimens were reviewed with the patient that would utilize a number of adjunctive hygiene aides, including an interproximal brush (Figure 17 and Figure 18).8
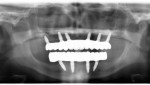
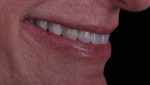
A final post-insertion panoramic radiograph was made as a baseline status of the patient and to validate the complete seating of the prostheses (Figure 19). The patient was satisfied with the clinical outcomes of the definitive prostheses (Figure 20 and Figure 21).
Discussion
It is important to consider the final restorative material prior to performing implant surgery for ICFDP. When choosing restorative materials, a key consideration is the workflow needed to achieve predictable and accurate prosthetic outcomes. The use of prototypes has benefits to the clinician, dental technician, and patient in providing high levels of predictability and accuracy. Prototype is a predictable clinical tool to ensure minimal to no alteration to the definitive ICFDP, enabling satisfactory functional, esthetic, and hygienic clinical outcomes to be achieved. This is of particular importance when choosing monolithic zirconia as the restorative material for definitive ICFDP.
Most zirconia prostheses (as a monolithic design or framework for veneered prostheses) are milled from pre-sintered ceramic blanks, and the milled restorations are sintered at high temperature to the final state. In addition, stabilizing oxides such as 3mol% yttria (Y2O3) are usually added in biomedical-grade zirconia as a stabilizer (3Y-TZP), which allows control of the stress-induced transformation and efficient arrest of crack propagation of the zirconia prosthesis.9 The excessive adjustment after sintering of zirconia can induce damage to the prosthesis and create surface flaws that initiate crack propagation and dramatically reduce strength and fatigue life of the zirconia prosthesis.10 The prototype prosthesis can be designed as an exact copy of the proposed definitive prosthesis and provided to the patient for clinical trial insertion. By using the prototype prosthesis, the resulting definitive prosthesis can be fabricated without significant need for post-sintering modifications in its contour and occlusion.
About the Authors
Jonathan H. Dawson, DDS, MSD
Private Practice limited to Prosthodontics, Greensboro, North Carolina
Grady Dix, CDT
Owner and Laboratory Manager, Sunwalt Dental Works Inc., Asheboro, North Carolina
Bryan T. Harris, DMD, CDT
Private Practice, Louisville, Kentucky
Wei-Shao Lin, DDS
Associate Professor, Department of Prosthodontics, Indiana University School of Dentistry, Indianapolis, Indiana
References
1. Balshi TJ, Wolfinger GJ. Conversion prosthesis: a transitional fixed implant-supported prosthesis for an edentulous arch-a technical note. Int J Oral Maxillofac Implants. 1996;11(1):106-111.
2. Zhang XX, Shi JY, Gu YX, Lai, HC. Long-term outcomes of early loading of Straumann implant-supported fixed segmented bridgeworks in edentulous maxillae: a 10-year prospective study. Clin Implant Dent Relat Res. 2016;18(6):1227-1237.
3. De Bruyn H, Raes S, Östman PO, Cosyn J. Immediate loading in partially and completely edentulous jaws: a review of the literature with clinical guidelines. Periodontol 2000. 2014;66(1):153-187.
4. Maló P, de Araújo Nobre M, Lopes A, et al. "All-on-4" immediate-function concept for completely edentulous maxillae: a clinical report on the medium (3 years) and long-term (5 years) outcomes. Clin Implant Dent Relat Res. 2012;14(suppl 1):e139-e150.
5. Rojas Vizcaya F. Restrospective 2- to 7- year follow-up study of 20 double full-arch implant-supported monolithic zirconia fixed prostheses: measurements and recommendations for optimal design. J Prosthodont. 2016. doi:10.1111/jopr.12528. [Epub ahead of print]
6.Abdulmajeed AA, Lim KG, Närhi TO, Cooper LF. Complete-arch implant-supported monolithic zirconia fixed dental prostheses: a systematic review. J Prosthet Dent. 2016;115(6):672-677.
7. Ercoli C, Geminiani A, Feng C, Lee H. The influence of verification jig on framework fit for nonsegmented fixed implant-supported complete denture. Clin Implant Dent Relat Res. 2012;14 (suppl 1):e188-e195.
8. Heitz-Mayfield LJ, Needleman I, Salvi GE, Pjetursson BE. Consensus statements and clinical recommendations for prevention and management of biologic and technical implant complications. Int J Oral Maxillofac Implants. 2014;29(suppl):346-350.
9. Denry I, Kelly JR. State of the art of zirconia for dental applications. Dent Mater. 2008;24(3):299-307.
10. Rekow ED, Silva NR, Coelho PG, et al. Performance of dental ceramics: challenges for improvements. J Dent Res. 2011;90(8):937-952.