Treatment of Oral Mucosal Lesions Associated With Overlapping Psychodermatologic Disorders
Sausan Alfaris, BDS, MPH; Katherine France, DMD, MBE; Thomas P. Sollecito, DMD; and Eric T. Stoopler, DMD
Abstract: Delusional infestations are psychodermatologic disorders in which those affected have a false belief they are infested by parasites and/or "growing" inanimate objects from cutaneous surfaces. Individuals with delusional parasitosis (DP) believe parasites, bacteria, worms, mites, or other living organisms are the source of cutaneous symptoms, while those with Morgellons disease (MD) attribute their symptoms to growth of small fibers or inorganic material. In both DP and MD, self-inflicted, non-healing cutaneous lesions caused by scratching at the affected areas to alleviate symptoms are commonly observed. This report describes a case of oral mucosal lesions in a patient demonstrating overlapping symptoms of DP and MD. It is important for oral healthcare providers to recognize oral signs and symptoms that may be associated with psychodermatologic disorders.
Delusional infestations (DIs) are psychodermatologic disorders in which parasites or inanimate objects are associated with cutaneous symptoms, such as itching and/or burning.1 DIs were first described in 1894 and are also known as Ekbom syndrome, acarophobia, and parasitaphobia.2 These types of disorders are thought to be caused by increased levels of dopamine in the striatum and limbic cortex and can present as a primary complaint or secondary to medication, addictions, or infection.3-5 They have an estimated annual incidence of 0.7 to 3 per 100,000 individuals, and the most common type of DI is delusional parasitosis (DP), with higher prevalence in women 50 to 80 years of age.2,3 Unlike DP, Morgellons disease (MD) is characterized by cutaneous "growth" of small fibers and/or inorganic material.1,2 Controversy exists if DP and MD are independent conditions as they share similar epidemiological and clinical characteristics.1-3 Patients often produce parasites, hair, inorganic material, etc, collected from various sources and stored in containers to demonstrate the "infestation," commonly referred to as the "matchbox" or "specimen" sign.1-3 Self-inflicted, non-healing cutaneous lesions are typically observed in both DP and MD, as patients attempt to alleviate symptoms by continuously scratching the affected areas.
Psychiatric counseling and use of antipsychotics are first-line therapies for management of these conditions.1-3 Historically, patients were treated with pimozide (dopaminergic receptor blocker); however, this medication was associated with high prevalence of extrapyramidal side effects and elongated QT.6,7Second generation antipsychotics are now used more frequently, such as olanzapine, aripiprazole, and risperidone, which are effective with significantly fewer side effects.2,5,8,9 Patients may also benefit from supplementary anxiolytic and antidepressant medications, such as fluoxetine and doxepin. This is particularly effective when patients present with additional complaints and are nonresponsive to initial therapy.10 Non-pharmacologic treatments of DIs include biofeedback, relaxation, hypnosis, and talk therapy.
Due to wide variation in treatment efficacy, patients with DIs often express frustration and distrust of the medical system, which frequently results in them resorting to self-treatment, often with pesticides, or seeking help online.8 Patients may be resistant to psychiatric management due to insistence of the physicality of their symptoms and a perceived stigma associated with psychiatric disorders.11 Intraoral lesions associated with DIs have been previously reported; however, these lesions have been attributed primarily to a single diagnosis.12 The aim of this report is to describe a case of oral mucosal lesions in a patient demonstrating overlapping symptoms of DP and MD.
Case Report
A 53-year-old woman presented for evaluation of lip lesions of 6 months' duration. She described her lesions as "round horns" that felt rubbery and stretched and were symptomatically relieved by her scratching them. The patient reported the lesions started as a swelling associated with burning and itching, and she believed they were caused by a "parasite trying to crawl out of her lip." The patient had been evaluated previously for this complaint by several healthcare providers and was empirically treated with nystatin, cephalexin, mupiricin, prednisolone, valacyclovir, and intra-lesional steroid injections without benefit. She underwent multiple diagnostic tests that were negative for viral, fungal, and bacterial organisms, and previous biopsy of a lip ulcer revealed nonspecific ulceration, granulation tissue, and necrosis.
Past medical history was significant for attention deficit hyperactivity disorder, hypothyroidism, C-spine spondylosis treated with C5-7 discectomy with fusion and glaucoma. Review of systems was unremarkable. Medications included dextroamphetamine, levothyroxine, bromfenac sodium, and timolol maleate. Physical examination revealed a well-nourished, well-developed female.
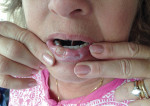
Extraoral examination did not reveal lymphadenopathy, salivary gland enlargement, or cutaneous lesions. Intraoral examination demonstrated multiple ulcerations primarily on the right lower labial mucosa and lip (Figure 1). At that time, clinical findings were suggestive of DP, and treatment recommendations included a referral for psychiatric evaluation and fabrication of a maxillary occlusal appliance and mandibular soft splint for daily use to prevent self-mutilation from biting.
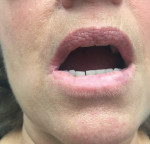
The patient was resistant to psychiatric referral and treatment, but open to medical and physical therapeutics. On subsequent evaluations, she reported that a clear wire or ingrown hair might be the cause of her lesions, suggestive of MD, and she scratched her lips to allow the hair to exfoliate. At that time, she was prescribed topical clindamycin 1% and topical doxepin 5% for application to the lesions daily, in addition to the soft splints, with clinical improvement after 1 year of treatment (Figure 2). Of interest, the patient did not produce a "matchbox" or "specimen" sign at any time, nor did she pursue or receive any type of psychiatric care for her suspected psychodermatologic disorder(s), although it was recommended to her on multiple occasions.
Discussion
Psychiatric disorders commonly encountered in dental practice include depression, anxiety, adjustment, and somatoform disorders.13-15 Psychodermatologic conditions are less common in the general population; therefore, oral healthcare providers (OHCPs) are less likely to be familiar with these disorders. In this case, the patient initially stated the cause of her oral lesions was a parasite, which is suggestive of DP. However, on subsequent evaluations the patient believed her oral lesions were attributed to inanimate objects, specifically a wire or a hair, which is suggestive of MD. Therefore, the authors concluded that overlapping features of DP and MD were present in this patient. The authors continue to encourage psychiatric evaluation as part of her overall treatment. In this case, the patient resisted recommendations to consult with a psychiatrist for evaluation and management of possible DIs.
If OHCPs recognize signs and symptoms of undiagnosed DIs, it is important to be sympathetic to the patient's complaints and to discuss referral, psychiatric evaluation, and management in a supportive manner. If a patient has been previously diagnosed with a type of DI, OHCPs should determine if the patient is receiving care from a psychiatrist and if the patient's condition is being actively managed. Oral mucosal lesions associated with DIs may be managed with topical medications, such as anesthetics, antibiotics, and/or corticosteroids.12 In addition, fabrication of occlusive splints can potentially minimize trauma to the affected areas.
In the present case, it should be noted that topical antibiotic and steroid treatment was administered prior to the patient presenting to the authors. The authors presumed that the rationale for that treatment was a possible inflammatory reaction, which the steroid would have helped, while recognizing that the mouth ulcer may have been secondarily infected, warranting the antibiotics. The authors note, however, that indiscriminate use of steroid on the vermillion surface will result in atrophy.
Patients managed with antipsychotics may experience increased sedation and are at risk for further central nervous system depression with concomitant use of narcotics and/or anxiolytics.12 In addition, adverse oral effects, such as xerostomia, dental caries, candidiasis, glossitis, sialadenitis, and extrapyramidal movements of oral structures may be evident in patients using antipsychotics, all of which may impact provision of oral healthcare.12
Conclusion
OHCPs are not only responsible for maintaining optimal oral health, but also for being able to potentially identify systemic diseases, including psychiatric disorders.16 DIs are rare psychodermatologic conditions, and it is imperative for OHCPs to: (1) recognize these conditions; (2) refer patients to the appropriate healthcare provider for further evaluation and/or management, if warranted; (3) understand the impact of DIs on the oral and maxillofacial region; and (4) provide safe and appropriate oral healthcare to patients with these conditions.
About the Authors
Sausan Alfaris, BDS, MPH
Postdoctoral Student, Department of Oral Medicine, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania
Katherine France, DMD, MBE
Resident, Department of Oral Medicine, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania
Thomas P. Sollecito, DMD
Professor and Chair of Oral Medicine, Department of Oral Medicine, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania
Eric T. Stoopler, DMD
Associate Professor of Oral Medicine, Department of Oral Medicine, University of Pennsylvania School of Dental Medicine, Philadelphia, Pennsylvania
References
1. Heller MM, Wong JW, Lee ES, et al. Delusional infestations: clinical presentation, diagnosis and treatment. Int J Dermatol. 2013;52(7):775-783.
2. Freudenmann RW, Lepping P. Delusional infestations. Clin Microbiol Rev. 2009;22(4):690-732.
3. Lepping P, Freudenmann RW. Delusional parasitosis: a new pathway for diagnosis and treatment. Clin Exp Dermatol. 2008;33(2):113-117.
4. Koo J, Lebwohl A. Psycho dermatology: the mind and skin connection. Am Fam Physician. 2001;64(11):1873-1878.
5. Thakkar A, Ooi KG, Assaad N, Coroneo M. Delusional infestation: Are you being bugged? Clin Ophthalmol. 2015;9:967-970.
6. Brown GE, Malakouti M, Sorenson E, et al. Psychodermatology. Adv Psychosom Med. 2015;34:123-134.
7. Bhandary SK, Peter R, Bhat S. Delusional parasitosis in ENT. Indian J Otolaryngol Head Neck Surg. 2008;60(4):387-389.
8. Bhatia MS, Jhanjee A, Srivastava S. Delusional infestation: a clinical profile. Asian J Psychiatr. 2013;6(2):124-127.
9. Bhushan P, Thatte SS. The dermatoscope: a new tool for delusional parasitosis. Clin Exp Dermatol. 2016;41(6):690-691.
10. Delacerda A, Reichenberg JS, Magid M. Successful treatment of patients previously labeled as having "delusions of parasitosis" with antidepressant therapy. J Drugs Dermatol. 2012;11(12):1506-1507.
11. Vulink NC. Delusional infestation: state of the art. Acta Derm Venereol. 2016;96(217):58-63.
12. Grosskopf C, Desai B, Stoopler ET. An oral ulceration associated with Morgellons disease: a case report. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2011;112(2):e19-e23.
13. Brodine AH, Hartshorn MA. Recognition and management of somatoform disorders. J Prosthet Dent. 2004;91(3):268-273.
14. George S, Saksena A, Oyebode F. An update on psychiatric disorders in relation to dental treatment. Dent Update. 2004;31(8):488-494.
15. Kino K, Sugisaki M, Ishikawa T, et al. Preliminary psychologic survey of orofacial outpatients. part 1: Predictors of anxiety or depression. J Orofac Pain. 2001;15(3):235-244.
16. Stoopler ET, Sollecito TP. Focusing on the medicine in dental medicine. Spec Care Dentist. 2016;36(2):59.