The Metal–Zirconia Implant Fixed Hybrid Full-Arch Prosthesis: An Alternative Technique for Fabrication
Lambert J. Stumpel, DDS; and Walter Haechler, MDT
Abstract: The metal-resin hybrid full-arch prosthesis has been a traditionally used type of restoration for full-arch implant fixed dentures. A newer development has centered around the use of monolithic zirconia or zirconia veneered with porcelain. Being a ceramic, zirconia has the potential for fracture. This article describes a technique that utilizes a metal substructure to support a chemically and mechanically resin-bonded shell of zirconia. The workflow is discussed, ranging from in-office master cast fabrication to the CAD/CAM production of the provisional and the definitive metal-zirconia prosthesis. The article also highlights the advantages and disadvantages of various materials used for hybrid prostheses.
With the introduction of dental implants by professor P.I. Brånemark some five decades ago, the restoration of choice was a metal-resin implant fixed full denture, also known as a hybrid prosthesis.1 Traditionally, a cast gold framework was used with denture teeth connected with acrylic resin. Because dental implants are rigidly connected to the bone it was deemed necessary to have a passive fit of the prosthesis to the implants to avoid introducing detrimental stresses into the bone-titanium junction.2 Recent research has shown that a misfit of up to 230 microns does not seem to have negative biological consequences.3-5 Such a misfit, however, is directly related to prosthetic problems such as screw loosening.6-10 Precision fit has, thus, remained an important factor in the production of implant-supported prostheses.
The original protocol called for implants to be submerged for 3 to 6 months; after integration, the second phase included abutment connection to the oral cavity. Subsequently, the final restoration was produced. With the introduction of immediate loading of freshly placed implants it became common practice to utilize an all-acrylic interim prosthesis.11-16 It was shown that for osseointegration to occur and be maintained, a metal framework was not necessary.17 Unfortunately, monolithic acrylic does not reliably function in this capacity over time. Fracture rates of immediate loading prostheses of 14% to 88% have been reported.18-20
A metal framework is thus needed to support the acrylic and the denture teeth. Progress has been made in the production of the metal framework with the introduction of adhesive cylinder luted frameworks, allowing superior passive fit to be attained in a simple analog process.21-27 The introduction of CAD/CAM has brought about a variety of digitally based production methods. Superior fit of CAD/CAM-generated frameworks compared to cast gold frameworks was shown early on.28 The most recent development is the use of monolithic zirconia or zirconia veneered with porcelain for fabrication of full-arch implant fixed restorations.29-34 While short-term positive results are reported, most authors suggest to approach this new treatment option cautiously. Zirconia is a ceramic, and like all ceramics, it is stronger in compression then in tension. This would suggest that it not be used in cantilevered situations to prevent fractures.
This article aims to describe a technique for fabrication of a metal-supported zirconia implant fixed prosthesis. A simple in-office workflow allows generation of a master cast and a duplication of the initial implant fixed prosthesis. This information is then used in the dental laboratory to fabricate a polymethyl methacrylate (PMMA) provisional and, subsequently, a metal substructure and corresponding zirconia shell. The zirconia suprastructure is bonded to the metal bar with a composite luting resin. This approach provides support to the cantilevered zirconia to reduce detrimental bending forces. This technique should be considered experimental until further studies warrant its use.
Case 1
A healthy 63-year-old woman presented with an implant-supported metal-resin hybrid prosthesis. She had received five implants in the mandible 23 years prior. The implants were placed in, what was at that time, a common fashion resulting in a bilateral posterior cantilever. The denture teeth and acrylic had worn and now needed to be replaced. While simple replacement of these elements was an option, the patient elected to proceed with a metal-reinforced zirconia prosthesis to have a restoration that would be less wear-prone.
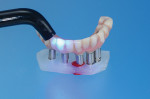
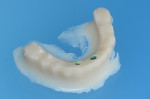
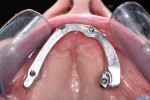
Because the existing hybrid prosthesis had an acceptable fit to the implants it was used to capture the implant position; hence, due to this ideal fit of the prosthesis there was no need for a verification jig. A pre-cured composite baseplate (Triad® Trutray™, Dentsply Sirona, dentsplysirona.com) was perforated to allow seating of laboratory implant analogs that were attached to the hybrid prosthesis. A small quantity of a low-shrinkage laboratory composite (primopattern LC Gel, Primotec, primotecusa.com) was then used to secure the analogs to the baseplate (Figure 1), as it is important to control the inevitable shrinkage of composite to attain a precise interrelationship among the laboratory analogs.
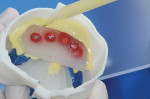
Because the fit of the acrylic intaglio was not ideal, the space between the tissue and the acrylic was impressed with a polyether material (Permadyne™ Garant™, 3M ESPE, 3m.com). Soft wax strips (Utility Wax Strips, Patterson Dental, pattersondental.com) were placed at the perimeter of the hybrid prosthesis, the analogs were attached to the hybrid, and baseplate wax was used to create a box. A dedicated casting vinyl polysiloxane (VPS) (Mach-SLO™, Parkell, parkell.com) was injected to fill the box (Figure 2).
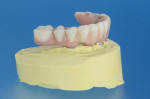
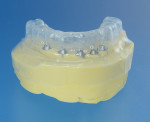
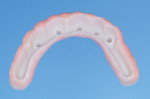
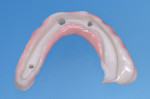
Upon setting of the VPS, the boxing wax was removed, revealing the precision master cast (Figure 3). A soft duplicating vacuform material 1-mm bleach tray and model duplication (Essix®, Dentsply Sirona) was used to create a vacuformed shell of the hybrid prosthesis and the landing areas of the master cast (Figure 4). Two adhesive luting cylinders (CAL cylinder, Attachments International, implantdirect.com) were placed on the anterior implants. The rest of the analogs were covered with healing caps. A self-polymerizing bis-acrylic provisional composite material (Luxatemp®, DMG America, dmg-america.com) was injected into the vacuformed shell, and the shell was repositioned over the cast (Figure 5). Because the composite will shrink upon setting, the 0.3-mm green spacer shims of the CAL cylinders were removed and the bis-acrylic provisional was bonded to the titanium cylinders with a luting composite (Panavia F, Kuraray, kuraraydental.com) to create a passive fit.
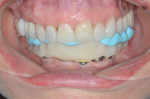
The flask was removed and the bis-acrylic provisional was fitted intraorally. Composite was applied to the anterior teeth, as a slight increase of the vertical relationship was required and more tooth structure needed to be visible. The bite registration was completed with a VPS bite registration material (BluMousse®, Parkell) (Figure 6). In the dental laboratory a new set-up with denture teeth was fabricated to meet the new requirements, which included longer anterior teeth and improved occlusion relations. A patient try-in approved the new blueprint, and the set-up was ready to scan. First, the master model was scanned (D800, 3Shape, 3shape.com) with the replica and the CAL titanium cylinders in place. The wax set-up was then scanned separately, and the two files were merged together. The resulting file of the new provisional was sent to a milling facility (Esthetic Dental Ceramics). Upon return to the lab, the PMMA provisional was treated with a PMMA-composite primer (Anaxblend bond LC, Anaxdent, anaxdent.com). The titanium cylinders were bonded with a luting composite (Panavia F) into the PMMA provisional.
Upon the clinician receiving the PMMA provisional, the existing hybrid was removed and the provisional was placed. After a few days the patient approved both the new design and the PMMA provisional.
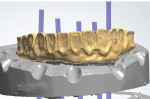
The PMMA provisional would be used as a guide to create the prosthesis in zirconia. The laboratory created a cutback of the approved provisional to generate space so that an esthetic layer of porcelain could be applied. This procedure may be done by hand or digitally. In this case the prosthesis was manually removed to better control the precise labial reduction from the incisal edge of the anterior and the occlusal edge of the posterior to keep all of the occlusion forces in zirconia. Once the design is finished a new scan is required. The modified PMMA prosthesis was placed back onto the master cast (Figure 7) and scanned. Because titanium was deemed not strong enough to support the prosthesis due to the considerable posterior cantilever, a nonprecious metal was selected for the metal substructure. A two-degree bar was designed in burnout resin (primopattern LC Gel) based on the adhesive abutment luting cylinders (CAL cylinders).
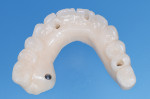
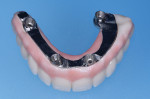
After casting, the titanium cylinders were bonded into the framework with luting composite (Panavia F) (Figure 8). The finished bar was placed onto the master cast and this assembly was scanned. The resulting file was merged with the scan of the approved PMMA bridge, and a file was generated signifying the zirconia suprastructure. This file was then transferred into zirconia by an external central processing facility (Esthetic Dental Ceramics). Upon return to the laboratory, tooth-colored porcelain was added to the zirconia into the previously made cutbacks. Finally, pink porcelain was added to provide a lifelike appearance (Figure 9).
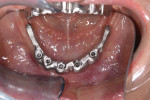
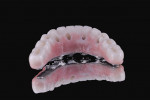
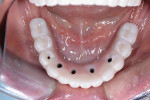
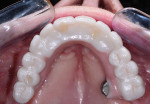
The zirconia shell was lightly air-abraded and bonded to the nonprecious metal bar with phosphate-modified luting composite (Panavia F). The flask was removed and polished (Figure 10). Clinically, the assembly was placed and secured with the prosthetic screws. Because the zirconia was an exact duplicate of the PMMA provisional no intraoral adjustments were needed (Figure 11).
Case 2
An 83-year-old woman with advanced Parkinson's disease presented with a terminal dentition in the maxilla. The teeth were extracted and four implants were placed, three regular and one zygomatic. An immediate-load all-acrylic prosthesis was made based on the clinician's best estimation. After 3 months of healing it was apparent that the current provisional prosthesis needed considerable modification. After duplication of the existing provisional and generation of the master cast, a similar workflow as described previously was utilized. This resulted in a new PMMA provisional prosthesis.
After the patient wore this prosthesis for some time, small modifications were still deemed necessary. The same information already available to the dental technician was used to generate a new PMMA provisional. The second PMMA bridge was placed and the patient functioned with it for 6 weeks to confirm full acceptance (Figure 12). Upon approval, the second PMMA provisional was removed and the first PMMA provisional was re-placed to function during fabrication of the final metal-zirconia prosthesis in the laboratory.
The second PMMA provisional was cut-back on the buccal to allow spacing for the placement of esthetic porcelain. It was then placed back onto the master cast, and the assembly was scanned on an optical laboratory scanner (NobelProcera 2G, Nobel Biocare, nobelbiocare.com). Dedicated laboratory flags were placed onto the analogs and the master cast was scanned independently. This allowed the merging of the two separate files. The two-degree titanium bar was designed to allow appropriate spacing and support for the zirconia suprastructure (Figure 13). Once the laboratory received the titanium bar from the central production facility, the bar was placed onto the master cast and scanned with a desktop scanner (D800). The images of the PMMA provisional and the titanium bar on the cast were merged in the dedicated dental CAD software (Dental System, 3Shape). This allowed the file for the zirconia shell to be generated, and this file was sent to a central processing facility. Upon the zirconia shell being received back at the laboratory, esthetic porcelain was applied for the buccal of the teeth and the pink section of the prosthesis (Figure 14). The titanium bar and zirconia shell were bonded with a luting composite (Figure 15). The finished metal-zirconia full-arch prosthesis was placed intraorally and secured with prosthetic screws (Figure 16). Occlusion was verified and approved.
Discussion and Conclusion
Traditionally, the restoration of choice for full-arch implant fixed prostheses has been a metal-resin hybrid prosthesis, ie, a metal substructure veneered with acrylic and denture teeth. Although this concept has remained essentially unchanged for more than 40 years, wear and chipping have been recognized. Increased use of zirconia in dentistry has created interest in using monolithic zirconia for full-arch implant fixed prostheses. Zirconia, which is a ceramic, is much stronger in compression as compared to tension. Cantilever situations may, therefore, not be particularly suited for it. A possible alternative in these situations is a metal framework that supports a bonded shell of zirconia.
Due to the limited experience of this technique at present, caution is warranted in using this material application until further research can prove its appropriateness.
Acknowledgment
The authors thank Kelly Haechler, RDH, and Chris Chahrestan for their CAD/CAM expertise.
About the Authors
Lambert J. Stumpel, DDS
Private Practice, San Francisco, California
Walter Haechler, MDT
Haechler Esthetic Design, Corte Madeira, California
References
1. Brånemark PI, Breine U, Adell R, et al. Experimental studies on intra-osseous anchorage of dental prosthesis. Arsb Goteb Tandlak Sallsk. 1970:9-25.
2. Adell R, Lekholm U, Rockler B, Brånemark PI. A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10(6):387-416.
3. Karl M, Taylor TD. Bone adaptation induced by non-passively fitting implant superstructures: a randomized clinical trial. Int J Oral Maxillofac Implants. 2016;31(2):369-375.
4. Winter W, Taylor TD, Karl M. Bone adaptation induced by non-passively fitting implant superstructures: a finite element analysis based on in vivo strain measurements. Int J Oral Maxillofac Implants. 2011;26(6):1288-1295.
5. Jokstad A, Shokati B. New 3D technologies applied to assess the long-term clinical effects of misfit of the full jaw fixed prosthesis on dental implants. Clin Oral Implants Res. 2015;26(10):1129-1134.
6. Abduo J, Judge RB. Implications of implant framework misfit: a systematic review of biomechanical sequelae. Int J Oral Maxillofac Implants. 2014;29(3):608-621.
7. Wood MR, Vermilyea SG; Committee on Research in Fixed Prosthodontics of the Academy of Fixed Prosthodontics. A review of selected dental literature on evidence-based treatment planning for dental implants: report of the Committee on Research in Fixed Prosthodontics of the Academy of Fixed Prosthodontics. J Prosthet Dent. 2004;92(5):447-462.
8. Kallus T, Bessing C. Loose gold screws frequently occur in full-arch fixed prostheses supported by osseointegrated implants after 5 years. Int J Oral Maxillofac Implants. 1994;9(2):169-178.
9. Kohavi D. Complications in the tissue integrated prostheses components: clinical and mechanical evaluation. J Oral Rehabil. 1993;20(4):413-22.
10. Jemt T, Book K. Prosthesis misfit and marginal bone loss in edentulous implant patients. Int J Oral Maxillofac Implants. 1996;11:620-625.
11. Balshi TJ, Wolfinger GJ. Conversion prosthesis: a transitional fixed implant-supported prosthesis for an edentulous arch-a technical note. Int J Oral Maxillofac Implants. 1996;11(1):106-111.
12. Maló P, de Araújo Nobre M, Lopes A, et al. "All-on-4" immediate-function concept for completely edentulous maxillae: a clinical report on the medium (3 years) and long-term (5 years) outcomes. Clin Implant Dent Relat Res. 2012;14 (suppl 1):e139-e150.
13. Nikellis I, Levi A, Nicolopoulos C. Immediate loading of 190 endosseous dental implants: a prospective observational study of 40 patient treatments with up to 2-year data. Int J Oral Maxillofac Implants. 2004;19(1):116-123.
14. Wolfinger GJ, Balshi TJ, Rangert B. Immediate functional loading of Brånemark system implants in edentulous mandibles: clinical report of the results of developmental and simplified protocols. Int J Oral Maxillofac Implants. 2003;18(2):250-257.
15. Maló P, de Araújo Nobre M, Lopes A, et al. Complete edentulous rehabilitation using an immediate function protocol and an implant design featuring a straight body, anodically oxidized surface, and narrow tip with engaging threads extending to the apex of the implant: a 5-year retrospective clinical study. Int J Oral Maxillofac Implants. 2016;31(1):153-161.
16. Niedermaier R, Stelzle F, Riemann M, et al. Implant-supported immediately loaded fixed full-arch dentures: evaluation of implant survival rates in a case cohort of up to 7 years. Clin Implant Dent Relat Res. 2017;19(1):4-19.
17. Thomé E, Lee HJ, Sartori IA, et al. A randomized controlled trial comparing interim acrylic prostheses with and without cast metal base for immediate loading of dental implants in the edentulous mandible. Clin Oral Implants Res. 2015;26(12):1414-1420.
18. Maló P, de Araújo Nobre M, Lopes A. The use of computer-guided flapless implant surgery and four implants placed in immediate function to support a fixed denture: preliminary results after a mean follow-up period of thirteen months. J Prosthet Dent. 2007;97(6 suppl):S26-S34.
19. Collaert B, De Bruyn H. Immediate functional loading of TiOblast dental implants in full-arch edentulous maxillae: a 3-year prospective study. Clin Oral Implants Res. 2008;19(12):1254-1260.
20. Agliardi E, Panigatti S, Clericò M, et al. Immediate rehabilitation of the edentulous jaws with full fixed prostheses supported by four implants: interim results of a single cohort prospective study. Clin Oral Implants Res. 2010;21(5):459-465.
21. Voitik AJ. The Kulzer abutment luting; Kal technique. A direct assembly framework method for osseointegrated implant prostheses. Implant Soc. 1991;2(1):11-14.
22. Stumpel LJ 3rd, Quon SJ. Adhesive abutment cylinder luting. J Prosthet Dent. 1993;69(4):398-400.
23. Stumpel LJ 3rd. The adhesive-corrected implant framework. J Calif Dent Assoc. 1994;22(2):47-53.
24. Menini M, Dellepiane E, Pera P, et al. A luting technique for passive fit of implant-supported fixed dentures. J Prosthodont. 2016;25(1):77-82.
25. Longoni S1, Sartori M, Maroni I, Baldoni M. Intraoral luting: modified prosthetic design to achieve passivity, precision of fit, and esthetics for a cement-retained, implant-supported metal-resin-fixed complete denture. J Prosthodont. 2010;19(2):166-170.
26. Menini M, Pera F, Migliorati M, et al. Adhesive strength of a luting technique for passively fitting screw-retained implant-supported prostheses: an in vitro evaluation. Int J Prosthodont. 2015;28(1):37-39.
27. Clelland NL, van Putten MC. Comparison of strains produced in a bone simulant between conventional cast and resin-luted implant frameworks. Int J Oral Maxillofac Implants. 1997;12(6):793-799.
28. Takahashi T, Gunne J. Fit of implant frameworks: an in vitro comparison between two fabrication techniques. J Prosthet Dent. 2003;89(3):256-260.
29. Rojas-Vizcaya F. Full zirconia fixed detachable implant-retained restorations manufactured from monolithic zirconia: clinical report after two years in service. J Prosthodont. 2011;20(7):570-576.
30. Limmer B, Sanders AE, Reside G, Cooper LF. Complications and patient-centered outcomes with an implant-supported monolithic zirconia fixed dental prosthesis: 1 year results. J Prosthodont. 2014;23(4):267-275.
31. Larsson C, et al. A prospective study of implant-supported full-arch yttria-stabilized tetragonal zirconia polycrystal mandibular fixed dental prostheses: three-year results. Int J Prosthodont. 2010;23(4):364-369.
32. Abdulmajeed AA, Lim KG, Närhi TO, Cooper LF. Complete-arch implant-supported monolithic zirconia fixed dental prostheses: a systematic review. J Prosthet Dent. 2016;115(6):672-677.
33. Altarawneh S, Limmer B, Reside GJ, Cooper L. Dual jaw treatment of edentulism using implant-supported monolithic zirconia fixed prostheses. J Esthet Restor Dent. 2015;27(2):63-70.
34. Papaspyridakos P, Lal K. Computer-assisted design/computer-assisted manufacturing zirconia implant fixed complete prostheses: clinical results and technical complications up to 4 years of function. Clin Oral Implants Res. 2013;24(6):659-665.