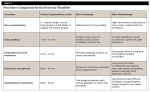
Q: How consistent are vertical augmentation procedures in anterior versus posterior regions?
Craig M. Misch, DDS, MSD; Michael S. Block, DMD; Michael A. Pikos, DDS; and Homa H. Zadeh, DDS, PhD
Dr. Misch
When discussing vertical bone augmentation, it is important to distinguish whether the osseous defect is within the bony contour (intrabony) or outside the bone envelope (extrabony). Vertical bone defects inside the bony contour are more predictable to reconstruct because they have a higher regenerative capacity from the surrounding osseous walls and more easily achieve soft-tissue coverage. These defects also have better space maintenance and graft protection from loading during healing, which explains the high predictability of sinus bone grafting. Vertical augmentation to enhance ridge height, ie, onlay augmentation, is more biologically and clinically challenging.
Several surgical techniques can be used for vertical augmentation, including block bone grafting, guided bone regeneration (GBR), titanium mesh grafting, interpositional grafting, and distraction osteogenesis, though no one method has proven to be superior. Many reviews focus on implant survival as the measure of vertical augmentation success.1 This parameter can skew the surgeon’s perspective. The choice of technique and/or graft material should depend on the amount of bone gain needed. Smaller vertical augmentations (< 5 mm) can be predictably achieved by a number of methods, while larger vertical gains will usually require the use of autogenous bone as part or all of the graft substrate.2
The developing field of tissue engineering offers a strategy to replace the need for harvesting bone from the patient, with the use of growth factors being the main focus in dental applications. Bone morphogenetic protein with a titanium mesh scaffold has shown promise as an alternative to autograft.3 There are a lack of follow-up studies, however, on implant survival and marginal bone loss. A concern with vertical bone grafts is stability of the augmentation over time. Favorable bone maintenance has been documented with GBR techniques and onlay bone grafting.4,5
Though achieving consistent results is possible, vertical bone augmentation is a complex and technique-sensitive surgical procedure with a considerable risk of morbidity and complications.6 As such, it should be performed by well-trained, experienced clinicians. One paramount requirement is a passive, tension-free flap closure over the grafted site. Patient factors, however, such as poor compliance, smoking, or compromised health, may lower outcomes. Retreatment of a failed augmentation also has a less predictable prognosis.
Onlay augmentation of the posterior jaws and anterior mandible is less demanding because the main goal is to provide a bony foundation for implant prosthetic support. There is growing evidence that short implants are effective in the posterior maxilla and mandible and that their usage may well eliminate the need for vertical bone augmentation.7 This option decreases morbidity, treatment length, and costs, and I would consider it as a primary option in many cases. The anterior maxilla is obviously more challenging, especially in a patient with a high smile line. Even when the surgery is skillfully performed, the development of an ideal tooth morphology and soft-tissue profile is often elusive (especially in the replacement of interdental papilla).8
Clinicians today have a better understanding of the esthetic limitations in reconstructing esthetic zone defects. This often shifts the burden onto the dental laboratory and restorative dentist to replace the missing hard and soft tissue with a natural-appearing prosthesis. This approach, however, may be more predictable and preferred in achieving satisfactory esthetics.
Dr. Block
Vertical augmentation of the alveolar crest is a well-established procedure, with much work having been done concerning this treatment in the edentulous mandible and maxilla to aid in denture retention. Onlay graft procedures are among the methods to perform this therapy. Grafting bone on the superior surface of the residual alveolar cortical bone is accomplished by first gaining access to the cortical bone, then placing and securing a bone graft to the region to be augmented, and closing the soft tissue. Various graft materials have been used, such as iliac crest cortical and cancellous bone, calvarial bone, symphyseal and ramus bone, and bank bone, including both allograft and xenograft. Grafts include blocks of material, particulate material with membrane coverage, or a combination of both.
Advantages of using an onlay graft include avoidance of the inferior alveolar nerve (IAN), ease of placement of the graft, and immediate postoperative vertical augmentation. Incision breakdown over the graft may result in reduction of the long-term augmentation, however, especially when using grafts predominantly composed of cortical bone.9-11 Cordaro and coworkers10 reported that, in the mandible, an average of 2.4 mm of vertical gain was achieved, though only 1.4 mm of the graft remained at the time of implant placement. The onlay grafts decreased by 41.5% during the first 6 months. Proussaefs and colleagues11 performed intraorally harvested autogenous block grafts for vertical alveolar ridge augmentation. Their results showed a vertical augmentation of 5.75 mm 1 month after surgery and 4.75 mm 4 to 6 months after surgery. There was total bone loss of 17.4% during the first 6 months.
Incisional dehiscence and exposure of the graft are common complications with any onlay graft method. When using symphyseal or ramus bone blocks, incisional dehiscence results in the loss of the entire block of bone graft.8 When cancellous iliac crest bone or particulate bone is exposed through incisional dehiscence, a portion of the graft may still be viable, which can result in partial bone augmentation. When the incision breakdown occurs over a particulate graft with membrane coverage, the membrane may require removal and, depending on the status of graft revascularization, a portion of the underlying graft may be retained. Autogenous bone harvested from the iliac crest or ribs has been shown to result in significant resorption.9-11
The use of particulate bone with membrane coverage allows for both horizontal and vertical augmentation of the mandible. The membrane is designed to prevent infiltration of the particulate graft with connective tissue and allow bone to infiltrate into the particulate graft mass rather than the connective tissue, resulting in the formation of bone sufficient to support implants and, through implant functional loading, retain the bone that is formed.12 Three mm to 6 mm of vertical bone augmentation has been reported.12 Besides being technically difficult and requiring some level of expertise to attain successful results, the main disadvantage of the use of membranes is premature exposure of the membrane through the mucosa.12
The use of metallic mesh has been advocated to form and retain a particulate graft for vertical ridge augmentation. Boyne and colleagues13 used mesh to form a new maxillary ridge in anterior combination syndrome patients and others with an atrophic maxillary ridge. If the mesh did not become exposed early after placement, bone formation was predictable. When the mesh became exposed during the healing process, however, it required removal, which, depending on the time from placement, resulted in either good or poor bone ridge augmentation. The use of mesh with smaller pores and more flexibility for posterior mandibular ridge augmentation showed excellent results, but the exposure of the mesh is still a factor to consider.14
Interpositional bone grafting has a long history with numerous methods of reconstructing the posterior edentulous mandible having been used.15-20 When performing an interpositional osteotomy and moving the mobilized alveolar bone segment vertically, the clinician must decide on the optimal material to graft the defect. Particulate cancellous marrow grafts have shown more rapid vascularization and more osteogenic activity compared with autogenous block grafts.21 Schettler, who proposed the sandwich technique for vertical augmentation of the mandible, believed that less bone resorption would occur in interpositional grafts because the graft is surrounded by bone and periosteum on all sides, which facilitates a rapid vascular connection with the surrounding tissues.18 Jensen, reporting on interpositional or sandwich osteotomies in the posterior edentulous mandible before implant placement, achieved up to 8 mm of vertical augmentation of the posterior mandible by interpositional osteotomy.22 Preoperative bone height was 3 mm to 7 mm above the IAN canal. Horizontal osteotomies were created 2 mm above the IAN canal. The lingual-based flap was stretched superiorly 4 mm to 8 mm. A miniplate was used for rigid fixation. A cortical wedge of bone from the external oblique ridge and particulate autograft were placed in the interpositional graft site. After 4 months of healing, the miniplates were removed, and short implants (8 mm to 11 mm) were placed. The implants were loaded 3 to 4 months after placement. The average vertical augmentation of the posterior mandible achieved with this technique was 6 mm. Bone resorption was between 0 mm and 1 mm with a follow-up of 1 to 4 years. Marchetti and coworkers,23 using autogenous cancellous particulate bone as the graft, reported similar results.
Interpositional grafting of the mandible has limitations. It only corrects vertical defects, not horizontal ones, and there is an anatomic limitation to the amount of vertical gain that can be achieved that involves the stretch of the soft-tissue attachments to the pedicled mobilized alveolar segment of bone. Interpositional grafting, though, is a safe, predictable method of achieving from 5 mm to 8 mm of vertical augmentation in the posterior mandible.8
Dr. Pikos
While a number of procedures are available for vertical ridge augmentation, such as GBR, titanium mesh particulate grafting including recombinant human bone morphogenetic protein-2 (rhBMP-2), autogenous block bone grafting, distraction osteogenesis, and interpositional bone grafting, the literature is not clear on which procedure is optimal as numerous parameters are not measured within the respective reported bone-grafting protocols.6,24,25 First, the exact nature and extent of the bony defect typically is not indicated. Some defects are more compromised than others and, thus, more challenging. Such defects are usually extrabony in nature with essentially only one wall providing blood supply for the grafted bone. It is important to appreciate the overall 3-dimensional extent as this will, in turn, dictate the specific protocol and surgical approach for reconstruction. The more compromised the defect, the greater the need is for procedures that provide optimal regenerative potential.
In addition, defining successful bone augmentation is problematic as, once again, the literature is conflicted. Typically, implant survival rate is used to assess overall bone-graft efficacy. A better way to define a successful bone graft might be to gauge adequate bone volume attained in both the short and long term. Also, implant success versus survival might be a better way to assess the efficacy of the procedure. Five key principles are vital for predictable bone augmentation: (1) incision design/flap management; (2) recipient site preparation; (3) space maintenance; (4) graft stability; and (5) tension-free primary closure, including appropriate suturing.26-28
In general, achieving predictable outcomes with vertical bone-grafting procedures in the anterior or posterior maxilla and mandible is more challenging than with horizontal bone grafting.25 This is because it is more difficult to achieve appropriate flap management, space maintenance, graft stability, and adequate soft-tissue closure for the entire duration of graft healing in these cases. If any of these principles are compromised, the end-result is often a compromise of the bone graft, which could include bone-graft failure and partial loss of the original recipient site (hard and soft tissue). Thus, it is important that the clinician be equally skilled in both soft-tissue management/grafting and bone grafting. This concept is consistent with the Hybrid Surgeon™ philosophy that I have fostered at the Pikos Institute in courses that focus on both hard- and soft-tissue grafting protocols. I adhere to the basic principles outlined here for predictable vertical and horizontal bone augmentation in all areas of the mouth. For vertical defects up to 3 mm to 4 mm, I usually use an autogenous block graft29-31 or GBR procedure.28,32 For larger defects, I typically use titanium-mesh/particulate grafting, including rhBMP-2.33,34
In my opinion, the anterior maxilla (ie, esthetic zone) and posterior mandible pose the greatest challenges for predictable vertical augmentation. The esthetic zone affords little to no room for error. Defects in this area requiring vertical bone augmentation demand a high level of clinician experience in both soft- and hard-tissue grafting concepts with appropriate restorative requirements. Here, soft-tissue relaxation for the most part can only be obtained from the facial flap.
In the posterior mandible, complications can occur with vertical bone augmentation if clinicians are unaware of the importance of lingual flap release and appropriate facial flap relaxation for primary closure. Since 1990, I have used a blunt dissection-based lingual flap release protocol that I learned from mandibular tripodial subperiosteal implant surgical protocols.
Finally, the importance of operator experience cannot be emphasized enough when it comes to successful vertical bone grafting. As Aghaloo and Moy6 stated, alveolar ridge augmentation procedures are highly technique and operator-experience sensitive.
Dr. Zadeh
The predictability of vertical augmentation depends on the initial risk assessment. Defect morphology, size, oral location (eg, maxilla versus mandible; anterior versus posterior), mucosal quality and health, and systemic conditions are among the primary factors to consider. In addition, practical considerations include the clinician’s experience, availability of intraoral donor bone and soft tissues, and patient expectations and willingness to undergo multiple procedures, if necessary.
The defect morphology and size can be an important predictor of the outcome. Vertical defects that have a wide base and sloped walls, such as saddle-shaped ridges, respond better than those with flat morphology and a thin crest.35 The periodontal condition of the adjacent teeth is important because the height of the crest of adjacent teeth is the maximum level to which regeneration can occur. In treating defects adjacent to teeth with periodontal attachment loss, orthodontic extrusion or extraction may be necessary to improve the outcome. Alveolar bone with inner trabecular spongy bone provides a better blood supply than those with dense monocortical bone. The size of the defect is also important: the larger the defect, the less likelihood there is of complete defect repair.36
After performing a thorough initial risk assessment, the clinician can answer several questions: (1) Is the patient a good candidate for regeneration, and what is the likelihood of complete defect repair?; (2) Is the patient willing to undergo repeated procedures, if necessary?; (3) Does the clinician possess sufficient expertise and experience to perform the treatment?
The next step is to select an appropriate protocol, material, and sequence. Selecting the appropriate protocol and material depends somewhat on the clinician’s preference. Some common techniques used for vertical augmentation include GBR, onlay grafting, and distraction osteogenesis, or a combination of these. Various form-stable devices, such as titanium mesh, titanium-reinforced membrane, or tenting screws, may be used for creating a protected space. The choice of biomaterial autogenous bone (block or particulate), xenograft, allograft, or alloplastic material must be made. Biologics, such as recombinant growth factors or autologous platelet concentrates, may be used to modulate the biologic wound healing. I believe the more challenging the defect morphology, the more important it is to use autogenous bone.
Each of the oral regions presents its unique set of challenges, requiring different strategies. In particular, flap management, one of the most critical aspects of ridge augmentation, varies for each oral site. The quality and quantity of the oral mucosa has to be carefully assessed. Any inflammation that may be the consequence of existing teeth or prostheses has to be resolved before regenerative surgery can be performed. Although the quantity and quality of mucosa is important, performing soft-tissue augmentation before alveolar ridge augmentation is ill-advised.37 Any surgical intervention is likely to cause scarring of the mucosa and periosteum and complicate the release of the mucosa to achieve a tension-free primary flap approximation. It is best to defer soft-tissue augmentation until after bone augmentation, perhaps at the time of implant placement.
In conclusion, vertical augmentation is a challenging procedure that requires thorough risk assessment and selection of appropriate protocol, material, and sequence of therapy. Also, clinicians should determine their own level of comfort for performing the procedure and the suitability of the patient to undergo the therapy. Otherwise, an alternative to vertical ridge augmentation may be considered.
About The Authors
Craig M. Misch, DDS, MDS
Clinical Associate Professor, Departments of Periodontics and Prosthodontics
University of Florida College of Dentistry
Gainesville, Florida
Private Practice
Oral and Maxillofacial Surgery and Prosthodontics
Sarasota, Florida
Michael S. Block, DMD
Private Practice
Oral and Maxillofacial Surgery
Metairie, Louisiana
Michael A. Pikos, DDS
Clinical Associate Professor, Departments of Periodontics and Prosthodontics
University of Florida College of Dentistry
Gainesville, Florida
Founder and CEO
Pikos Institute
Private Practice
Oral and Maxillofacial Surgery
Palm Harbor, Florida
Homa H. Zadeh, DDS, PhD
Associate Professor
University of Southern California Herman Ostrow School of Dentistry
Los Angeles, California
Private Practice
Periodontology
Woodland Hills, California
References
1. Chiapasco M, Casentini P, Zaniboni M. Bone augmentation procedures in implant dentistry. Int J Oral Maxillofac Implants. 2009;24(suppl):237-259.
2. Milinkovic I, Cordaro L. Are there specific indications for the different alveolar bone augmentation procedures for implant placement? A systematic review. Int J Oral Maxillofac Surg. 2014;43(5):606-625.
3. Misch CM, Jensen O, Pikos M, Malmquist J. Vertical bone augmentation using recombinant bone morphogenetic protein (rhBMP-2), mineralized bone allograft and titanium mesh: a retrospective cone beam computed tomography study. Int J Oral Maxillofac Implants. 2015;30(1):202-207.
4. Urban IA, Jovanovic SA, Lozada JL. Vertical ridge augmentation using guided bone regeneration (GBR) in three clinical scenarios prior to implant placement: a retrospective study of 35 patients 12 to 72 months after loading. Int J Oral Maxillofac Implants. 2009;24(3):502-510.
5. Schmitt C, Karasholi T, Lutz R, et al. Long-term changes in graft height after maxillary sinus augmentation, onlay bone grafting, and combinations: a long-term retrospective cohort study. Clin Oral Implants Res. 2014;25(2):e38-e46.
6. Aghaloo TL, Moy PK. Which hard tissue augmentation techniques are the most successful in furnishing bony support for implant placement? Int J Oral Maxillofac Implants. 2007;22(suppl):49-70.
7. Thoma DS, Zeltner M, Hüsler J, et al. EAO Supplement Working Group 4 - EAO CC 2015 Short implants versus sinus lifting with longer implants to restore the posterior maxilla: a systematic review. Clin Oral Implants Res. 2015;26(suppl 11):154-169.
8. Salama M, Coachman C, Garber D, et al. Prosthetic gingival reconstruction in the fixed partial restoration. Part 2: diagnosis and treatment planning. Int J Periodontics Restorative Dent. 2009;29(6):573-581.
9. Chiapasco M, Zaniboni M, Rimondini L. Autogenous onlay bone grafts vs. alveolar distraction osteogenesis for the correction of vertically deficient edentulous ridges: a 2-4 tear prospective study on humans. Clin Oral Implants Res. 2007;18(4):432-440.
10. Cordaro L, Amade DS, Cordaro M. Clinical results of alveolar ridge augmentation with mandibular block bone grafts in partially edentulous patients prior to implant placement. Clin Oral Impl Res. 2002;13:103-111.
11. Proussaefs P, Lozada J. The use of intraorally harvested autogenous block grafts for vertical alveolar ridge augmentation: a human study. Int J Periodontics Restorative Dent. 2005;25(4):351-363.
12. Simion M, Trisi P, Piattelli A. Vertical ridge augmentation using a membrane technique associated with osseointegrated implants. Int J Periodont Rest Dent. 1994;14(6):496-511.
13. Boyne PJ, Cole MD, Stringer D, Shafgat JP. A technique for osseous restoration of deficient edentulous maxillar ridges. J Oral Maxillofac Surg. 1985;43(2):87-91.
14. Louis PJ, Gutta R, Said-Al-Naief N, Bartolucci AA. Reconstruction of the maxilla and mandible with particulate bone graft and titanium mesh for implant placement. J Oral Maxillofac Surg. 2008;66(2):235-245.
15. Clementschitsch F. In: Pichler H, Trauner R, eds. Mund-und Kieferchirurgie. 2 Aufl. Berlin: Schwarzenberg; 1948.
16. Davis WH, Delo RI, Ward WB, et al. Long term ridge augmentation with rib grafts. J Maxillofac Surg. 1975;3(2):103-106.
17. Frame JW, Browne RM, Brady CL. Biologic basis for interpositional autogenous bone grafts to the mandible. J Oral Maxillofac Surg. 1982;40 (7):407-411.
18. Schettler D. Sandwich-technique with cartilage transplant for raising the alveolar process in the lower jaw. Fortschr Kiefer Gesichtschir. 1976;20:61-63.
19. Harle F. Visor osteotomy to increase the absolute height of the atrophied mandible: A preliminary report. J Maxillofac Surg. 1975;3(4):257-260.
20. Stoelinga PJ, de Koomen HA, Tideman H, Huijbers TJ. A reappraisal of the interposed bone graft augmentation of the atrophic mandible. J Maxillofac Surg. 1983;11(3):107-112.
21. Burchardt H. The biology of bone graft repair. Clin Orthop Relat Res. 1983;(174):28-42.
22. Jensen OT. Alveolar segmental “sandwich” osteotomies for posterior edentulous mandibular sites fro dental implants. J Oral Maxillofac Surg. 2006;64(3):471-475.
23. Marchetti C, Trasarti S, Corinaldesi G, Felice P. Interpositional bone grafts in the posterior mandibular region: a report on six patients. Int J Periodontics Restorative Dent. 2007;27(6):547-555.
24. Chiaposco M, Casentini P, Zaniboni M. Bone augmentation procedures in implant dentistry. Int J Oral Maxillofac Implants. 2009;24(suppl): 237-259.
25. Esposito M, Grusovin MG, Felice P, et al. The efficacy of horizontal and vertical bone augmentation procedures for dental implants—a Cochrane systematic review. Eur J Oral Implantol. 2009;2(3):167-184.
26. Wang HL, Boyapati L. “PASS” principles for predictable bone regeneration. Implant Dent. 2006;15(1):8-17.
27. Schmid J, Wallkamm B, Hämmerle CH, et al. The significance of angiogenesis in guided bone regeneration. A case report of a rabbit experiment. Clin Oral Implants Res. 1997;8(3):244-248.
28. Schenk RK, Buser D, Hardwick WR, Dahlin C. Healing pattern of bone regeneration in membrane-protected defects: a histologic study in the canine mandible. Int J Oral Maxillofac Implants. 1994;9(1):13-29.
29. Pikos MA. Block autografts for localized ridge augmentation: Part I. The posterior maxilla. Implant Dent. 1999;8(3):279-285.
30. Pikos MA. Block autografts for localized ridge augmentation: Part II. The posterior mandible. Implant Dent. 2000;9(1):67-75.
31. Misch CM. Ridge augmentation using mandibular ramus bone grafts for the placement of dental implants: presentation of a technique. Pract Periodontics Aesthet Dent. 1996;8(2):127-135.
32. Buser D, Dula K, Belser UC, et al. Localized ridge augmentation using guided bone regeneration. II. Surgical procedure in the mandible. Int J Periodontics Restorative Dent. 1995;15(1):10-29.
33. Louis PJ, Gutta R, Said-Al-Naief N, Bartolucci AA. Reconstruction of the maxilla and mandible with particulate bone graft and titanium mesh for implant placement. J Oral Maxillofac Surg. 2008;66(2):235-245.
34. von Arx T, Hardt N, Wallkamm B. The TIME technique: a new method for localized alveolar ridge augmentation prior to placement of dental implants. Int J Oral Maxillofac Implants. 1996;11(3):387-394.
35. Khojasteh A, Motamedian SR, Sharifzadeh N, Zadeh HH. The influence of initial alveolar ridge defect morphology on the outcome of implants in augmented atrophic posterior mandible: an exploratory retrospective study. Clin Oral Implants Res. 2016. [Epub ahead of print].
36. Sanz-Sánchez I, Ortiz-Vigón A, Sanz-Martín I, et al. Effectiveness of lateral bone augmentation on the alveolar crest dimension: a systematic review and meta-analysis. J Dent Res. 2015;94(9 suppl):128S-142S.
37. Urban IA, Monje A, Nevins M, et al. Surgical management of significant maxillary anterior vertical ridge defects. Int J Periodontics Restorative Dent. 2016;36(3):329-337.