Diagnostic, Evaluation, and Treatment Approaches Used in Dental Sleep Medicine
Stephen Poss, DDS
Abstract:
While some causes or symptoms of sleep-disordered breathing can be identified visually upon oral examination or by observing radiographic images, establishing a diagnosis of this disorder and determining its severity requires the use of specific diagnostic testing. This article reviews diagnostic and evaluation technologies, as well as surgical and nonsurgical treatments, currently available for dentists collaborating in the treatment of patients with sleep breathing disorders, including snoring and obstructive sleep apnea.
Sleep-disordered breathing (eg, snoring, obstructive sleep apnea) affects an estimated 24% or more of adults and contributes to such life-threatening conditions as hypertension and high blood pressure, heart failure, diabetes, stroke, depression, and obesity.1,2 It is also associated with serious motor vehicle, work-related, and at-home accidents.3 Characterized by recurring cessations or reductions in breathing during sleep, sleep-disordered breathing involves loss of the normal “awake” or “upright” tone and position of the oral cavity and oropharyngeal musculature. In some instances, the tongue falls back into the oropharynx, or the airway narrows, collapses, or otherwise becomes obstructed. Sleep-disordered breathing results from obstructions and/or upper airway collapse, some of the causes or symptoms of which can be identified visually upon oral examination and others by examining radiographic images.4,5
Among the anatomical characteristics that may contribute to sleep-disordered breathing that could be observed during a dental examination are macroglosia, narrow mandibular arch, high palatal vault, large uvula, and enlarged tonsils. Considering that dentists see most of their patients every 6 to 12 months, they may be the first healthcare professionals to suspect a patient is suffering from sleep-disordered breathing. Other contributing anatomical characteristics that can be observed radiographically include a larger distance between the mandibular plane and hyoid bone,6 posterior displacement of the symphysis,7 and other disproportionate relationships between the tongue base, soft palate, cranial base, pterygoid processes, cervical spine, and others.8
Visual examination and radiographic approaches are helpful for identifying the signs of, and anatomical characteristics potentially contributing to, sleep-disordered breathing. However, establishing a diagnosis of sleep-disordered breathing and determining the severity of the disorder (ie, snoring, obstructive sleep apnea, mild-moderate-severe) require the use of specific diagnostic testing (eg, polysomnography, portable home sleep study). Depending upon the state in which dentists practice, they may be limited to screening for the condition or administering a sleep apnea test, and prohibited from rendering a diagnosis or prescribing a specific treatment because the tests must be interpreted—and a correct diagnosis rendered—by a physician.9,10
Fortunately, since dental sleep medicine began gaining greater attention more than 20 years ago, dentists and sleep physicians are increasingly collaborating to enhance the timeliness of sleep-disordered breathing diagnoses and appropriateness of treatment. Further, a variety of diagnostic/evaluation technologies and treatment approaches have been studied and reviewed in recent years to enable dentists and their sleep physician colleagues to determine the most appropriate treatment options for individual patients, based on the cause of their sleep-disordered breathing and the extent of the problem. This article briefly reviews diagnostic and evaluation technologies and surgical and nonsurgical treatments currently available for dentists collaborating in the treatment of patients with sleep breathing disorders.
Diagnostic Technologies
Because some of the anatomic features that contribute to sleep-disordered breathing can be observed during an oral examination, dentists with training in dental sleep medicine can identify patients with the signs and symptoms of this condition. When signs of sleep-disordered breathing are discovered, asking questions about the patient’s sleep habits and sleep quality can confirm the need for diagnostic testing and referral to a board-certified sleep medicine physician.
Polysomnography
Polysomnography was originally the “go-to” method for diagnosing sleep apnea and sleep-disordered breathing. Although considered the most accurate approach for diagnosing patients with this condition, simpler and less complicated methods were needed to overcome the expense, labor intensity, and poorly tolerated instrumentation inherent with polysomnography.11
Portable Home Sleep Study
Portable home sleep studies gained in popularity as an alternative, largely because they can be performed at home and involve a less complicated procedure (Figure 1). Requiring less monitoring and well-tolerated by patients, portable home sleep studies have been shown to demonstrate high specificity and sensitivity for identifying patients with sleep apnea.11
When the diagnosis reveals moderate to severe sleep apnea and/or obstructive sleep apnea, further diagnostics and evaluation of maxillofacial, oropharyngeal, and upper airway anatomy are required. These additional diagnostics and evaluations help to identify the anatomical cause and extent of the obstruction, and guide dentists and sleep physicians in their decisions regarding the most appropriate treatment approach for the patient.
Radiographs and CBCT
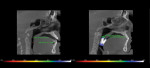
Dental radiographs and cone-beam computed tomography (CBCT) play significant roles in assessing patients with sleep-disordered breathing, enabling more precise identification of the areas and extent of airway obstructions.8 In particular, 3-dimensional (3-D) CBCT images allow analysis of the airways and specific maxillofacial, oropharyngeal, and other anatomy that may be involved with sleep-disordered breathing. Considering that years of research have identified radiographically visible anatomical characteristics and obstructions in patients with sleep-disordered breathing, CBCTs in the dental practice can be a valuable screening and treatment planning tool.8
For example, attempts were made to identify upper airway abnormalities in patients with idiopathic obstructive sleep apnea. Cross-sectional analysis of cephalometric roentgenograms revealed that the patients studied had smaller mandibles and overall posterior displacement of the mandibular symphysis, and that there was a correlation between the number of apnea episodes and posterior displacement. This suggested a correlation between idiopathic obstructive sleep apnea and upper airway occlusion that is not visible during an oral examination.7
Similarly, cephalometric roentgenograms have been studied and shown to indicate the presence of small posterior airway space and inferiorly placed hyoid bone in patients with obstructive sleep apnea who required palatopharyngoplasty (PPP) in order to better identify the soft-tissue obstruction location.12 Additionally, other dentofacial features (eg, retrognathia, micrognathia, skeletal Class II, long soft palate, tonsillar hypertrophy, inferior hyoid bone position) of patients with obstructive sleep apnea have been identified and categorized through cephalometric evaluation and found to correspond to specific types of obstructive sleep apnea.13
In more recent years, studies have focused on the manner in which the use of CBCT scans could potentially lend greater precision to analyzing the maxillofacial and airway characteristics of patients with sleep-disordered breathing. However, more research and discussion are needed to confirm the full extent to which CBCTs can benefit dentists when collaborating with sleep physicians in the diagnosis, screening, and treatment planning of patients with sleep-disordered breathing.
Among the relevant research conducted, a 2009 study compared imaging information about nasopharyngeal airway size between lateral cephalometric headfilms and 3-D CBCT scans and found considerable variability in the airway volumes of patients with similar airways among the lateral headfilms, whereas the 3-D CBCT scans were found to be simple and effective for accurately analyzing the airway.5 Subsequently, CBCTs have been used to determine linear, volumetric, and cross-sectional airway area measurements in patients with sleep-disordered breathing, ultimately determining that the areas where most airway constriction occurs can vary, with the variation correlating in part to age and gender.14
Other research has also suggested that CBCT airway analysis could be useful in assessing the presence and severity of obstructive sleep apnea, noting that these parameters are associated with a narrow lateral dimension of the airway, among other individual traits.15 What’s interesting to note, however, is that what may affect the accuracy and utility of CBCT scans in dental sleep medicine is the position in which the patient is situated at the time the scans are taken. Whereas images taken with the patient in an upright position (eg, cephalometric views) do not realistically reflect a patient’s airway during sleeping, the supine position required for CBCTs may enable more accurate assessment of airway, soft palate, and volumetric measurements and identification of obstruction locations.15
Treatments for Sleep-Disordered Breathing
The results of these radiographic-based investigations suggest that using CBCTs in screening, diagnosing, and treatment planning patients with sleep-disordered breathing—and particularly obstructive sleep apnea—can be beneficial, especially prior to planning surgical interventions. They also underscore the need to consider the location of the obstruction along the airway to ensure treatment efficacy.16 For example, the further down the airway an obstruction is located, the less likely that an oral appliance will be effective in treating the sleep-disordered breathing condition.16
Continuous Positive Airway Pressure (CPAP)
The most prescribed and recommended treatment for moderate to severe obstructive sleep apnea is continuous positive airway pressure (CPAP). With a 70% acceptance rate, CPAP machines require patients to wear a mask during nighttime sleep. The unit introduces air into a person’s nasal passage and exerts positive pressure to open the upper airway, which enables him or her to breathe.11
Appliance Therapy
Oral appliances have been widely used to treat sleep-disordered breathing and have been shown to lessen the severity of the condition by 60%; additionally, like CPAP machines, they have an acceptance rate of approximately 70%.17,18 Currently, there are more than 40 types of oral appliances available, all categorized according to their design or mechanism of action (eg, tongue-retaining or mandibular advancement).
Mandibular advancement oral appliances (either fixed or adjustable) have been the nonsurgical method of choice and shown to be successful in the treatment of sleep-disordered breathing when patients cannot tolerate CPAP machines and have mild to moderate sleep apnea (Figure 2).1,9-11,16-18 In fact, mandibular advancement devices have been shown to reduce both systolic and diastolic blood pressure among patients with obstructive sleep apnea,16 as well as improve blood oxygen saturation levels and reduce apnea-hypopnea index.11 However, these devices may present complications, including occlusal changes, temporomandibular joint discomfort, fabrication issues, and high cost.19
Additionally, despite the relatively high acceptance rate associated with oral appliances, consistent patient compliance in terms of nightly wear remains an issue. An oral device (SomnoDent® with CR, SomnoMed, www.somnomed.com), however, was recently introduced that incorporates some of the compliance features used with a CPAP. Designed specifically to objectively record compliance measurements when patients use the oral appliance to treat obstructive sleep apnea, the device contains a thermal sensor and accelerometer “chip” (DentiTrac®) embedded and sealed within it to measure hours worn and record head position.20
Surgical Interventions
Upper airway surgery is considered the last resort and reserved for patients who have not responded to other available treatment options (eg, CPAP, oral appliance). The variety of surgeries performed to reduce upper airway obstructions range from those focused on nasal obstructions (ie, septoplasty, turbinectomy, turbinate radiofrequency ablation) to those that reduce soft-palate redundancy (ie, uvulopalatopharyngoplasy, uvulopalatal flap, laser-assisted uvulopalatoplasty, and soft-palate radiofrequency ablation with adenotonsillectomy).21 More drastic procedures for more severe cases of obstructive sleep apnea include genioglossal advancement, hyoid suspension, distraction osteogenesis, tongue radiofrequency ablation, lingualplasty, and maxillomandibular advancement.21
Nasal surgeries—Nasal surgeries address obstructions created by hypertrophied, cartilaginous, or bony tissues in the nasal airway.21 Although they cannot significantly improve sleep breathing in patients with moderate to severe sleep-disordered breathing, nasal surgeries do help to enhance CPAP compliance, as well as prevent or minimize the mouth breathing that can ultimately force the tongue into the posterior pharyngeal area, thereby exacerbating sleep breathing conditions.
Mandibular osteotomy with genioglossus advancement—When upper airway obstruction occurs at the base of the tongue, moving the geniotubercle or the hyoid complex forward will stabilize the tongue base as well as the related pharyngeal dialators.21 With mandibular osteotomy with genioglossus advancement, a limited parasagittal mandibular osteotomy is used to advance the geniotubercle of the mandible forward, force an anterior advancement of the tongue base, and enlarge the retrolingual airway. Depending on the severity of the sleep-disordered breathing, success rates for this procedure have ranged from 35% to 60%, with the most serious complications being mandibular fracture, infection, permanent anesthesia, and seroma.21 However, it is usually performed with uvulopalatopharyngoplasty (UPPP) to enhance the upper airway space and eliminate the need for additional procedures, such as hyoid myotomy suspension.
Hyoid myotomy suspension—Considered part of phase I treatment—although not necessarily performed simultaneously with mandibular osteotomy with genioglossus advancement—hyoid myotomy suspension focuses on moving the hyoid complex forward to enhance the airway space behind the tongue.21 Many patients, however, find this procedure difficult to tolerate, which is why alternative approaches (eg, mandibular osteotomy with genioglossus advancement combined with UPPP) are undertaken.21
Uvulopalatopharyngoplasty (UPPP)—This surgical approach excises the uvula, posterior palatal area, and trims and reorients the posterior and anterior lateral pharyngeal pillars in order to enlarge the retropalatal airway, and is also considered part of phase I treatment.21,22 In recent years, lasers have been used for tissue incisions and vaporization when shortening the uvula and modifying the soft palatal tissue.23 Usually performed in combination with other procedures (eg, adenotosillectomy, advancement), UPPP has only been 41% successful in treating sleep-disordered breathing—particularly obstructive sleep apnea syndrome—is quite uncomfortable, and only 5% effective if retrolingual narrowing exists.22 Complications have included dysphagia, persistent dryness, and nasopharyngeal stenosis,21 and, overall, inconsistent outcomes and adverse effects have been reported as a result of pharyngeal surgeries.23
Further, the success of such surgical interventions is predicated on precisely locating the soft tissue and obstruction,12 which underscores the need for appropriate techniques when analyzing cephalometric and/or radiographic images. UPPP is not recommended when imaging has confirmed a retrolingual narrowing or retrolingual collapse during apneas.22 Instead, maxillofacial surgery is recommended for patients suspected of having hypopharyngeal collapse.22
Maxillomandibular advancement osteotomy (MMA)—In MMA surgery, the velo-orohypopharyngeal airway is enlarged by advancing the soft palate, tongue base, and suprahyoid musculature (ie, anterior pharyngeal tissues) that are attached to the maxilla, mandible, and hyoid bone.23 The multilevel skeletal surgery also involves LeFort I and bilateral sagittal split rami osteotomies and stabilization using bone grafts, plates, or screws.23 Considered part of phase II treatment, MMA has been shown to produce substantial and consistent reductions in the apnea-hypopnea index (AHI).23
Although MMA surgery can help to reduce the health risks associated with obstructive sleep apnea,24 the efficacy of surgical interventions overall for the treatment and management of sleep-disordered breathing remains a topic of debate and study, particularly when the condition cannot be attributed to specific anatomic attributes of the upper airway.8 Nevertheless, advancing the mandibular arch through MMA has proven more successful than other surgical techniques in reducing AHI, but more research is still needed in the areas of morbidity, patient selection, and long-term efficacy.23
Conclusion
Several screening, diagnostic, and treatment advancements for patients with sleep-disordered breathing—and published literature regarding their efficacy and appropriateness for identifying and resolving different types of obstructions—have become available in recent years. Combined, they provide dentists and their sleep physician colleagues with resources on which to base their decisions regarding how best to treat patients with sleep-disordered breathing.
Paramount to the success of any treatment that is undertaken is knowledge of the cause of the problem (ie, type, extent, and location of the obstruction). Although some of these causes can be determined through a visual oral examination, others must be more thoroughly identified through precise diagnostic imaging. Additionally, given the growing body of evidence that supports and/or cautions against the application of different diagnostic techniques and treatment approaches, it is incumbent upon dentists working with patients with sleep-disordered breathing conditions to pursue quality and reputable ongoing continuing education and training, as well as develop strong and mutually respectful collaborative relationships with sleep physician colleagues.
About the Author
Stephen Poss, DDS
Private Practice
Poss Dental Designs
Brentwood, Tennessee
References
1. Institute of Medicine (US) Committee on Sleep Medicine and Research; Colten HR, Altevogt BM (eds). Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem. Washington, DC: National Academies Press (US); 2006.
2. Obstructive Sleep Apnea. American Academy of Dental Sleep Medicine website. August 7, 2015. http://www.aadsm.org/sleepapnea.aspx. Accessed January 20, 2016.
3. Davidson TM. The role of the dental profession in the diagnosis and treatment of sleep-disordered breathing. Dent Today. 2005;24(9):118-120.
4. Young T, Peppard PE, Gottlieb DJ. Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med. 2002;165(9):1217-1239.
5. Aboudara C, Nielsen I, Huang JC, et al. Comparison of airway space with conventional lateral headfilms and 3-dimensional reconstruction from cone-beam computed tomography. Am J Orthod Dentofacial Orthop. 2009;135(4):468-479.
6. Riley R, Powell N, Guilleminault C. Cephalometric roentgenograms and computerized tomographic scans in obstructive sleep apnea. Sleep. 1986;9(4):514-515.
7. Rivlin J, Hoffstein V, Kalbfleisch J, et al. Upper airway morphology in patients with idiopathic obstructive sleep apnea. Am Rev Respir Dis. 1984;129(3):355-360.
8. Hatcher DC. Cone beam computed tomography: craniofacial and airway analysis. Dent Clin North Am. 2012;56(2):343-357.
9. Ivanhoe JR, Attanasio R. Sleep disorders and oral devices. Dent Clin North Am. 2001;45(4):733-758.
10. Rodriguez-Lorenzo FJ, Sáez-Yuguero Mdel R, Linares Tovar E, Bermejo Fenoll A. Sleep apnea and mandibular advancement device. Revision of the literature. Med Oral Patol Oral Cir Bucal. 2008;13(9):E549-E554.
11. Padma A, Ramakrishnan N, Narayanan V. Management of obstructive sleep apnea: A dental perspective. Indian J Dent Res. 2007;18(4):201-209.
12. Riley R, Guilleminault C, Powell N, Simmons FB. Palatopharyngoplasty failure, cephalometric roentgenograms, and obstructive sleep apnea. Otolaryngol Head Neck Surg. 1985;93(2):240-244.
13. Baik UB, Suzuki M, Ikeda K, et al. Relationship between cephalometric characteristics and obstructive sites in obstructive sleep apnea syndrome. Angle Orthod. 2002;72(2):124-134.
14. Chiang CC, Jeffres MN, Miller A, Hatcher DC. Three-dimensional airway evaluation in 387 subjects from one university orthodontic clinic using cone beam computed tomography. Angle Orthod. 2012;82(6):985-992.
15. Enciso R, Nguyen M, Shigeta Y, et al. Comparison of cone-beam CT parameters and sleep questionnaires in sleep apnea patients and control subjects. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2010;109(2):285-293.
16. Bratton DJ, Gaisl T, Wons AM, Kohler M. CPAP vs mandibular advancement devices and blood pressure in patients with obstructive sleep apnea. A systematic review and meta-analysis. JAMA. 2015;314 (21):2280-2293.
17. Lockerman LZ. Oral appliance management of obstructive sleep apnea: a case report. J Mass Dent Soc. 2006;55(2):18-20.
18. Mohsenin N, Mostofi MT, Mohsenin V. The role of oral appliances in treating obstructive sleep apnea. J Am Dent Assoc. 2003;134(4):442-449.
19. Ihara K, Ogawa T, Shigeta Y, et al. The development and clinical application of novel connectors for oral appliance. J Prosthodont Res. 2011;55(3):184-188.
20. SomnoMed receives FDA 510(k) approval for SomnoDent devices with wearable compliance microrecording. Dentistry IQ website. June 25, 2015. http://www.dentistryiq.com/articles/2015/06/somnomed-receives-fda-510-k-approval-for-somnodent-devices-with-wearable-compliance-micro-recording.html. Accessed January 20, 2016.
21. Won CH, Li KK, Guilleminault C. Surgical treatment of obstructive sleep apnea: upper airway and maxillomandibular surgery. Proc Am Thorac Soc. 2008;5(2):193-199.
22. Bettega G, Pépin JL, Veale D, et al. Obstructive sleep apnea syndrome. Fifty-one consecutive patients treated by maxillofacial surgery. Am J Respir Crit Care Med. 2000;162(2 Pt 1):641-649.
23. Caples SM, Rowley JA, Prinsell JR, et al. Surgical modifications of the upper airway for obstructive sleep apnea in adults: a systematic review and meta-analysis. Sleep. 2010;33(10):1396-1407.
24. Prinsell JR. Maxillomandibular advancement surgery for obstructive sleep apnea syndrome. J Am Dent Assoc. 2002;133(11):1489-1497.