Assessing Treatment Options Based on Expected Long-Term Results: Case Report Demonstrates 6-Year Outcomes
Abstract:
A patient whose chief concern was the esthetics of her anterior teeth presented for a second opinion after it had been recommended that crowns be placed throughout her mouth. Examination revealed numerous defective and some fractured restorations with recurring caries. With treatment goals including creating and maintaining a healthy periodontal environment, leveling the occlusal plane, and decreasing biomechanical risk, the treatment plan incorporated an interdisciplinary approach that utilized orthodontics, a Kois deprogrammer, and implant therapy. Demonstrating 6-year outcomes, this report discusses use of a method to assess treatment options based on expected long-term results.
Patients are often overwhelmed when they receive various recommendations for treatment. This report demonstrates 6-year outcomes using a method to assess treatment options based on the expected long-term results. While the overall treatment time was extended due to the inclusion of orthodontic therapy, the results demonstrate a favorable long-term prognosis as a result of this careful and comprehensive approach.
Clinical Case Overview
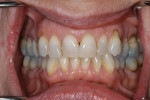
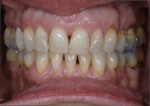
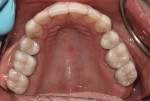
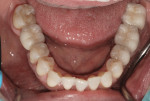
A 63-year-old female patient presented for a second opinion soon after her dentist had recommended extensive treatment. She was aware of many large and dark restorations, and she stated that she felt her teeth “were going down the tubes” (Figure 1). She did not like the appearance of her front teeth, and wanted her teeth to be whiter and straighter. She also expressed a desire to remedy the areas in her mouth that trapped food. In response to her chief concerns, the previous office had recommended crowns for every tooth.
The patient’s medical history included hypertension, hypercholesterolemia, and occasional migraine headaches. All conditions were controlled with medication. The dental history described biannual prophylaxis and was otherwise non-remarkable.
Diagnosis, Risk Assessment, and Prognosis
Periodontal: Comprehensive periodontal evaluation revealed generalized bleeding on probing with isolated sites of suppuration and pocket measurements up to 6 mm in all quadrants. Recession was noted on teeth Nos. 2 through 6, 11 through 15, 18 through 23, and 26 through 31. No signs of abnormal mobility were noted. Teeth Nos. 2, 14, 15, 18, 19, 30, and 31 demonstrated a combination of grades 1 and 2 furcation involvements. Alveolar bone levels were within 3 mm to 5 mm of the cemento-enamel junction (CEJ) on the majority of the teeth, with a vertical defect present on the distal of No. 18, resulting in a diagnosis of AAP type III1 (Figure 2). Abrasion was present on teeth Nos. 3, 6, 14, 18 through 21, and 28 through 31, and teeth Nos. 3, 5, and 11 through 14 had Class V restorations in areas of recession.
Risk: Moderate
Prognosis: Overall fair with a poor prognosis for tooth No. 18
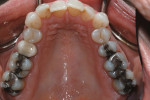
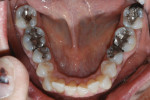
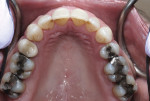
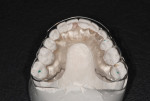
Biomechanical: The examination revealed defective restorations with recurring caries in teeth Nos. 3, 8, 11, 12, 14, 19, 20, and 29 through 31. Additionally, existing restorations were noted as fractured and thus defective in teeth Nos. 14 and 31. Due to the size of the existing restorations, teeth Nos. 2 through 4, 14, 15, 18 through 20, 29, and 30 were structurally compromised (Figure 3 and Figure 4).
Risk: High
Prognosis: Poor; hopeless for teeth Nos. 3,8,11,12,14,19,20,29-31
Functional: The patient had no functional concerns or observations and gave no positive responses to any dental history questions referencing function. She demonstrated a normal range of motion, no deviation upon opening, and slight-to-no wear on all teeth. A slight intermittent click was noted on the right temporomandibular joint (TMJ), while both joints accepted loading without discomfort. Muscles exhibited no tenderness with palpation. The presence of a TMJ click is an added risk factor. However, as the patient was unaware of this and had no challenges with mastication, the diagnosis is acceptable function.
Risk: Moderate
Prognosis: Fair
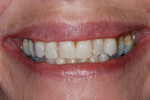
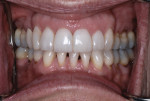
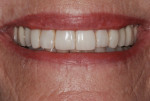
Dentofacial: When the patient smiled widely, the interdental papillae of the maxillary teeth showed, and there was no display of the mandibular gingiva (Figure 5). A small black triangle of space could be seen between the upper central incisors, and the occlusal plane was canted down to the left (Figure 6). Due to tooth positions and recession, horizontal gingival asymmetry was present in both arches.
Risk: Moderate
Prognosis: Fair
Medical: There were no contraindications to dental treatment at the time. The patient stated a history of tobacco smoking, a shared risk factor for periodontal disease.
Risk: Moderate
Prognosis: Fair
Treatment Goals
Treatment goals included the following:
• create and maintain a healthy periodontal environment
• brighten and straighten teeth
• level the occlusal plane
• decrease the biomechanical risk of caries, abrasion, and sensitivity
• eliminate or minimize food traps
Treatment Plan
During the consultation with the patient and her husband, it was explained that more conservative dentistry could be considered if her teeth were better aligned prior to restorative dentistry. A consultation with an orthodontist was recommended.2 Additionally, with the patient’s esthetic and food impaction concerns, it was explained that due to her risk of periodontal disease, changes in the appearance at the gum line may be noticeable over time, depending on both the type of restorations used and further changes in periodontal health.
Pre-restorative orthodontic treatment needed to address the crowding without compromising the periodontal structures. The patient was unwilling to consider orthognathic surgery, therefore it was necessary to treat the existing anterior-posterior skeletal discrepancies without excessive tooth tipping to manage the periodontal and esthetic goals.3,4 After the orthodontic consultation, the patient accepted a treatment plan to stabilize periodontal health by scaling and root planing, followed by diligent homecare efforts and 3-month intervals of periodontal maintenance. Teeth Nos. 5, 12, and 25 would be removed to reduce crowding and facilitate completion of orthodontic treatment. Once orthodontics was completed, a final esthetic treatment plan would be created and the posterior teeth in need of treatment would be restored using porcelain-fused-to-high-noble-metal crowns.
Treatment Phases
Phase 1: Stabilization of Periodontal Health And Preliminary Restorative Treatment
Full-mouth scaling and root planing was completed over multiple appointments. Existing restorations and caries were removed in teeth Nos. 30 and 31. A considerable fracture was noted on the pulpal floor of tooth No. 30, and the patient was informed that if this tooth failed to remain healthy, it would be best sacrificed and replaced with a dental implant.5 The remaining teeth were stable enough to restore after completion of orthodontics.
Phase 2: Extraction of Teeth, Orthodontic Alignment, And Positioning Teeth for Restorative Phase
Teeth Nos. 5, 12, and 25 were extracted prior to orthodontic treatment, which extended for 18 months. Tooth No. 30 abscessed prior to completion of orthodontic treatment, and as previously discussed, extraction was performed rather than interim, short-term endodontic therapy.
Phase 3: Post-Orthodontic Records, Creation of Upper Incisal Edge Position And Upper Occlusal Plane
New records consisting of extraoral and intraoral photography and mounted models were obtained (Figure 7 and Figure 8). Creating a final esthetic treatment plan required presenting several choices. The patient was given options that included whitening with no modifications to the front teeth, direct composite resin veneers, or porcelain laminate veneer restorations. At the time, she was reluctant to use porcelain restorations and requested direct composite resin veneers as a method to improve the esthetics of the front teeth and close spaces at the gum line. She understood that porcelain restorations could be created later for a longer-term solution.6,7 During the direct composite resin veneer procedure, teeth were lightly prepared to reduce the heavily contoured facial regions of the upper cuspids, as well as the occlusal of upper posterior teeth, to create a level occlusal plane for the entire upper arch8 (Figure 9 and Figure 10).
Phase 4: Establish Centric Relation And Maximum Intercuspation Position (MIP)
Six months after the completion of orthodontics, the patient wore a Kois deprogrammer for 2 weeks (Figure 11), after which time equilibration was performed both subtractively with tooth reduction and additively with composite resin (Renamel® Microhybrid, Cosmedent, Inc., www.cosmedent.com). The deprogramming stop was slowly removed, with modifications to the teeth, until MIP was achieved with cuspid coupling.9
Phase 5: Placement of Dental Implant
A 4.5-mm x 13-mm titanium dental implant (Osseospeed™, DENTSPLY Implants, www.dentsplyimplants.com) was placed by a periodontist in preparation for restoration of tooth No. 30, utilizing a single-stage approach.
Phase 6: Final Prosthetic Restorations
Final restorations were fabricated using porcelain-fused-to-high-noble-metal for teeth Nos. 2 through 4, 13 through 15, 18 through 20, 30 and 31 utilizing a custom abutment for the implant in the No. 30 position. Since the vertical dimension of occlusion and the esthetic positioning of the upper arch had previously been established and stabilized, the restorative dentistry was able to be completed one quadrant at a time (Figure 12 and Figure 13).
Discussion and Conclusion
While the patient came to the office seeking a second opinion regarding the proposed treatment, the treatment completed was somewhat different than what had been proposed, and it was not necessarily more or less expensive. The completed treatment was able to satisfy her desires to improve esthetics, minimize food impaction, and upgrade many aged and unsightly existing restorations. Had the earlier proposed treatment been performed on all of the teeth in the existing positions, a compromise to esthetics and an increased biomechanical risk would have been likely.
The patient responded favorably to initial periodontal treatment, with the elimination of bleeding and suppuration. Mobilities were present immediately after orthodontic treatment, however 6 years after orthodontic completion, there are no remaining mobilities. Radiographs taken 7.5 years after the initial records demonstrate bone levels consistent with the pre-treatment films. The risk for periodontal disease is still moderate. However, with her response to treatment and the lack of inflammation, as well as evidence of stability and remaining expected longevity, her prognosis has improved considerably (Table 1).
Biomechanical risk to the posterior teeth is still present as a result of the need for full-coverage preparations on most of the posterior teeth. The removal of caries with subsequent creation of cuspal support has served to lower the risk from high to moderate. The prognosis is better managed with full-coverage restorations, increasing the prognosis from poor to fair. Additionally, because very little preparation was done to the anterior teeth, the direct composite resin veneers have served to keep the biomechanical risk low for all the anterior teeth, with a good prognosis.
This patient initially presented with moderate functional risk. All efforts were made to create a harmonious occlusion with anterior coupling and guidance. An updated and completed dental history with more thorough questioning reveals the patient has responded well. There are no joint sounds or any other signs or symptoms of functional problems present at this time, indicating both low risk and a good prognosis.
The dentofacial risk remains unchanged with the same display of gingival papilla. However, as a result of a more esthetic repositioning of the teeth, combined with the direct composite resin veneers, her prognosis has improved to good, as demonstrated by her desire to keep the existing direct composite resin veneers over the consideration of porcelain laminate restorations.
After 6.5 years of service (Figure 14) the patient is still very pleased with the appearance of her upper front teeth and has no desire to convert to porcelain restorations at this time.
Acknowledgments
The author wishes to recognize the following colleagues for their dedication to interdisciplinary treatment: Tom Blase, DDS, MS, Tucson, Arizona, for his orthodontic abilities; Graig Brown, DDS, MS, Tucson, Arizona, for placement of the implant; and Aesthetic Oral Arts, Livingston, Montana, for providing laboratory expertise.
About the Author
Douglas E. McMaster, DDS
Mentor
Kois Center
Seattle, Washington
Private Practice
Tucson, Arizona
References
1. Armitage GC. Development of a classification system for periodontal diseases and conditions. Ann Periodontol. 1999;4(1):1-6.
2. Chalifoux P, Noxon S. Changing tooth position with orthodontics or restorative dentistry: both perspectives. Inside Dentistry. 2005;1(1):52-55.
3. Safavi S, Namazi A. Evaluation of mandibular incisor extraction treatment outcome in patients with bolton discrepancy using peer assessment rating index. J Dent (Tehran). 2012;9(1):27-34.
4. Rinchuse DJ, Busch LS, DiBagno D, Cozzani M. Extraction treatment part 1: the extraction vs. nonextraction debate. J Clin Orthod. 2014;48(12):753-760.
5. Berman LH, Kuttler S. Fracture necrosis: diagnosis, prognosis assessment, and treatment recommendations. J Endod. 2010;36(3):442-446.
6. McMaster DE. Achieving esthetic success while avoiding extensive tooth reduction. Compend Contin Educ Dent. 2014;35(6):398-402.
7. Hatkar F. Preserving natural tooth structure with composite resin. Journal of Cosmetic Dentistry. 2010;26(3):26-34.
8. Kois JC. Interdisciplinary Treatment Planning I, Course I. Kois Center; June 9-11, 2005; Seattle, WA.
9. Kois JC. Functional Occlusion I, Course II. Kois Center; March 6-8, 2006; Seattle, WA.