Effect of Curing Light and Restoration Location on Energy Delivered
Abstract:
This study determined how long it would take skilled operators to deliver 16 J/cm2 to an anterior or a posterior restoration using different light-curing units (LCUs). Three skilled operators used the following LCUs at two locations in the MARC-patient simulator: Optilux 501 standard mode for 20 s; Sapphire Supreme for 5 s; Elipar™ S10 for 5 s and 20 s; Demi™ Plus standard mode for 5 s; SmartLite® Max boost mode for 5 s and continuous mode for 20 s; Radii Plus for 30 s; Valo (main version) in standard mode for 20 s and Xtra Power mode for 3 s; and Valo Cordless in standard mode for 20 s and Xtra Power mode for 3 s. The three MARC-trained operators made 30 readings with each light over 7 days. The energy (J/cm2) delivered to the anterior Class III and posterior Class I simulated restorations in MARC was recorded using a laboratory-grade spectroradiometer, and the time each light would take to deliver 16 J/cm2 calculated. ANOVA and Fisher’s PLSD tests compared differences in the time to deliver 16 J/cm2 of energy, α = 0.05. Three-way ANOVA showed there was no significant difference between the operators, but there was a difference between the lights and locations. The Valo main and Valo Cordless in the Xtra Power mode delivered 16 J/cm2 in the shortest time at both locations. The Radii Plus took the longest to deliver 16 J/cm2, taking twice as long in the posterior location.
As the general population becomes increasingly conscious of the esthetic appearance of their teeth, composite resins will continue to increase in popularity over amalgam.1 Dental material companies have responded to this market by producing a variety of bonding agents, resins, and light-curing units (LCUs). In order to maintain the quality and longevity of composite fillings, a clinician must know how to evaluate the performance of these materials and use them with proper technique.2 Studies have shown that composite resins must be layered in at most 2-mm increments in order to achieve predictable and adequate hardness.3,4 The Phillip’s textbook5 suggests that at least 16 J/cm2 should be delivered to each 2-mm-thick layer of composite resin; however, other studies have reported a minimum energy range from 6 J/cm2 to 24 J/cm2, depending on the shade and opacity of the resin.6,7
Inadequate curing can negatively affect the longevity and success of a composite restoration. Delivering less than the proper amount of light energy results in greater deterioration at the margins of the restoration, decreased bond strength between the tooth and restoration, greater cytotoxicity, and reduced hardness.8-12 These factors will all result in clinical failure of the restoration.2
Four variables have been found to affect the extent to which a resin is polymerized within a tooth: curing light, operator technique, restoration characteristics, and energy requirement. These variables are represented by the acronym CORE.13 Additionally, an article published by the American Dental Association suggested that proper curing technique includes the following: wearing appropriate blue-light–blocking safety glasses; correct positioning of the patient so the provider has maximum visibility of and access to the restoration; placing the central axis of the LCU directly over and perpendicular to the resin surface; and stabilizing the LCU 1 mm away from the restoration for the first 1 second, then moving the tip of the LCU as close as possible to the surface for the remainder of the curing time.14
Previous studies intending to establish a correlation between energy received by the restoration and the qualities of the cured restoration have used conventional radiometer readings to record the irradiance of the LCU.3,15-17 However, conventional dental radiometers can be inaccurate and do not take into account the clinical challenges faced by an operator positioning a LCU in the oral cavity or the anatomical topography of teeth.18,19
Simulation Device
A recently introduced simulation device, Managing Accurate Resin Curing-Patient Simulator (MARC-PS) (BlueLight Analytics™, www.curingresin.com), uses a laboratory-grade spectroradiometer to accurately measure the irradiance, spectrum, and energy received by simulated resin restorations in a dental mannequin.20,21 Irradiance relates to energy delivered by the equation (I x T)/1000 = E where: I is the irradiance of the LCU measured in mW/cm2; T is the time the LCU is used for, measured in seconds (sec); and E is the energy delivered, measured in J/cm2. The system allows clinicians to see the irradiance they are delivering in real-time, as well as how changes in their technique can affect both the irradiance and energy delivered by their light. Specifically, one study done using this system found that energy delivered by operators to a Class I and Class V preparation site varied by individual operator and with curing light.20
Purpose
As the use of resin-based composite materials continues to increase in the dental setting, it is critical that practitioners employ proper curing technique to maximize the clinical efficacy of the restoration. The purpose of this study was to determine how the energy delivered to a restoration varied with the LCU used for curing and the location of the restoration. The first hypothesis was that different LCUs would deliver different amounts of energy to the simulated restorations. The second hypothesis was that there would be a difference in the amount of energy delivered by a given LCU to the anterior and posterior simulated restorations—ie, an LCU would deliver less energy to a posterior restoration versus one in the anterior.
Methods
Eight LCUs were selected to be tested in this study: one halogen curing light, the Optilux 501 (Kerr Dental, www.kerrdental.com), one plasma arc curing light, the Sapphire Supreme (DenMat Corp., www.denmat.com), and six LED curing lights, which were the Elipar™ S10 (3M ESPE, www.3MESPE.com), Demi™ Plus (Kerr Dental), SmartLite® Max (DENTSPLY Caulk, www.caulk.com), Radii Plus (Southern Dental Industries [SDI], www.sdi.com), Valo® (main version)(Valo/Ultradent Products, www.valo-led.com), and Valo Cordless (Valo/Ultradent).
Each light was tested in standard mode for a cure time consistent with the manufacturer’s specifications. In addition, the SmartLite Max and both Valo units were tested in a high-power mode (boost mode and Xtra Power mode, respectively), again using a cure time consistent with the manufacturer’s specifications. The Elipar S10 was tested for both 5 and 20 seconds, for a total of 12 LCU modes tested.
Each LCU mode was tested by three operators following proper curing technique on the MARC-PS. Proper curing technique included wearing appropriate blue-light–blocking safety glasses, correctly positioning the patient to provide maximum visibility and access to the restoration, placing the central axis of the LCU directly over and perpendicular to the resin surface, and stabilizing the LCU 1 mm away from the restoration for the first second, then moving the tip of the LCU as close as possible to the surface for the remainder of the curing time (Figure 1).
The irradiance received was measured with a CC3 light detector (Ocean Optics, www.OceanOptics.eu) attached by a fiber-optic cable to a laboratory-grade spectrometer (USB 4000, Ocean Optics) placed at the bottom of the cavity preparations. To simulate a posterior Class I restoration, the CC3 detector was fixed at a depth of 1 mm from the cavosurface margin and 4 mm from the cusp tip on tooth No. 15. To simulate an anterior Class III restoration, the CC3 detector was fixed at a depth of 1 mm from the labial surface on the interproximal of tooth No. 8 (Figure 2). Each operator used each LCU mode to deliver energy to both the anterior and posterior sensors, completing one cycle of tests. Each operator conducted three cycles of tests per day for 7 days.
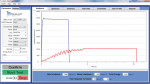
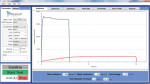
Before use, the MARC-PS system was calibrated using a NIST-traceable (National Institute of Standards and Technology), high-power light source (HL-2000-HP, Ocean Optics). The MARC software calculated the energy (J/cm2) delivered to each simulated restoration using the irradiance (mW/cm2) received by the sensor for the cure time of the LCU. To control for the variation in cure times between the LCUs, the time for each cure to deliver a clinically significant5 standard of 16 J/cm2 was calculated for data comparison (Figure 3). Analysis of variance (ANOVA) and Fisher’s PLSD tests were conducted to compare time differences to deliver 16 J/cm2 to the simulated restorations (α = 0.05).
Results
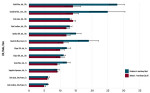
A three-way ANOVA test showed there was no significant difference in the energy delivered by the LCU modes between the three operators. However, the ANOVA test did show a significant difference in the amount of time needed to deliver 16 J/cm2 between both the LCU modes and the two simulated restorations (P < 0.05) (Table 1). Valo LCUs on Xtra Power mode were in the statistical group for shortest mean time to deliver 16 J/cm2 for both the anterior and posterior restoration (t < 6 sec). The Valo main, SmartLite Max, and Radii Plus all in their regular mode were in the statistical group with the longest mean time to deliver 16 J/cm2 for the anterior restoration (t = 14 sec). The Radii Plus took the longest for the posterior restoration (t = 28 sec). Radii Plus had the largest standard deviation for anterior cures (σ = 2.4 sec), while SmartLite Max in its regular mode had the largest standard deviation for posterior cures (σ = 5.6 sec).
Discussion
The hypothesis that there would be a difference in the energy delivered among the LCUs was confirmed (Figure 3, Figure 4, and Figure 5). LCUs tested in their plasma or boost mode delivered more energy than in their standard modes. The hypothesis that more energy would be delivered to an anterior restoration versus a posterior restoration was also supported (Figure 3, Figure 4, and Figure 5). For all LCU modes except the Valo main on standard mode, the average times to deliver 16 J/cm2 to the anterior simulated restoration were as fast or faster than the times for the posterior simulated restoration. This can possibly be attributed to the topographical differences between a Class I restoration and a smooth-surface Class III restoration, which increases the distance between the simulated restoration and the LCU. Furthermore, a posterior Class I restoration offers less visibility and direct access versus an anterior Class III restoration. Three LCU modes had a difference between the anterior and posterior mean times greater than 3 seconds; these were the SmartLite Max, used on both standard and boost modes (8 and 11 seconds, respectively), and the Radii Plus (14 seconds). This study supports previous research that has shown preparation location can affect the energy delivered to a restoration.20
Further investigation should be conducted into why some LCUs show a more significant variation between energy delivered to the anterior sensor versus the posterior sensor than other LCUs. Possible factors influencing this difference may include the design of the LCU’s optics and the ability of the operator to effectively position the LCU in the oral cavity.
Conclusion
This study has shown that not only do LCUs vary in the amount of energy delivered to a given restoration, but they also deliver different amounts of energy depending on the characteristics of the restoration. Clinicians should be aware of the performance of their LCU, and if using an LCU mode that demonstrates substantial variation in the energy delivered, depending on the characteristics of the restoration, it would be advised for clinicians to increase the cure time for resin layers in deeper preparations or preparations that have anatomical or topographical challenges for access.
Disclosure
This study was funded in part by a grant from Ivoclar Vivadent, Inc.
About the Authors
Sapan Bhatt, DMD
Tufts University School of Dental Medicine
Boston, Massachusetts
Coralie D. Ayer, DDS
Dalhousie University School of Dentistry
Halifax, Nova Scotia, Canada
Richard B. Price, BDS, DDS, MS, PhD
Professor,
Department of Dental Clinical Sciences
Dalhousie University School of Dentistry
Halifax, Nova Scotia, Canada
Ronald Perry, DMD, MS
Director of the Gavel Center for Restorative Research,
Associate Clinical Professor
Tufts University School of Dental Medicine
Boston, Massachusetts
References
1. Bohaty BS, Ye Q, Misra A, et al. Posterior composite restoration update: focus on factors influencing form and function. Clin Cosmet Investig Dent. 2013;5:33-42.
2. Yearn JA. Factors affecting cure of visible light activated composites. Int Dent J. 1985;35(3):218-225.
3. Rueggeberg FA, Caughman WF, Curtis JW Jr. Effect of light intensity and exposure duration on cure of resin composite. Oper Dent. 1994;19(1):26-32.
4. Marais JT, Dannheimer MF, Germishuys PJ, Borman JW. Depth of cure of light-cured composite resin with light-curing units of different intensity. J Dent Assoc S Afr. 1997;52(6):403-407.
5. Anusavice KJ, Shen C, Rawls HR. Phillps’ Science of Dental Materials. 12th ed. St. Louis, MO: Elsevier/Saunders; 2013.
6. Calheiros FC, Daronch M, Rueggeberg FA, Braga RR. Degree of conversion and mechanical properties of a BisGMA:TEGDMA composite as a function of the applied radiant exposure. J Biomed Mater Res B Appl Biomater. 2008;84(2):503-509.
7. Fan PL, Schumacher RM, Azzolin K, et al. Curing-light intensity and depth of cure of resin-based composites tested according to international standards. J Am Dent Assoc. 2002;133(4):429-434.
8. Price RB, Ferracane J. Effect of energy delivered on the shear bond strength to dentin. Can J Restor Dent Prosthodont. 2012;5:48-55.
9. Polydorou O, Konig A, Hellwig E, Kummerer K. Long-term release of monomers from modern dental-composite materials. Eur J Oral Sci. 2009;117(1):68-75.
10. Chen RS, Liuiw CC, Tseng WY, et al. The effect of curing light intensity on the cytotoxicity of a dentin-bonding agent. Oper Dent. 2001;26(5):505-510.
11. Quinlan CA, Zisterer DM, Tipton KF, O’Sullivan MI. In vitro cytotoxicity of a composite resin and compomer. Int Endod J. 2002;35(1):47-55.
12. Jadhav S, Hegde V, Aher G, Fajandar N. Influence of light curing units on failure of direct composite restorations. J Conserv Dent. 2011;14(3):225-227.
13. Price RB. Light energy matters. J Can Dent Assoc. 2010;76:a63.
14. Effective Use of Dental Curing Lights: A Guide for the Dental Practitioner. ADA Professional Product Review. 2013;8(2):2-12. https://www.ada.org/~/media/ADA/Publications/PPR/PPR_SPRING_2013_FINAL.ashx. Accessed February 17, 2015.
15. Shinkai K, Suzuki S, Katoh Y. Effect of high light intensity on cavity wall adaptation of a resin composite with a self-etching primer system. J Biomed Mater Res B Appl Biomater. 2006;79(2):420-424.
16. Hofmann N, Markert T, Hugo B, Klaiber B. Effect of high intensity vs. soft-start halogen irradiation on light-cured resin-based composites. Part II: Hardness and solubility. Am J Dent. 2004;17(1):38-42.
17. Barros GK, Aguiar FH, Santos AJ, Lovadino JR. Effect of different intensity light curing modes on microleakage of two resin composite restorations. Oper Dent. 2003;28(5):642-646.
18. Roberts HW, Vandewalle KS, Berzins DW, Charlton DG. Accuracy of LED and halogen radiometers using different light sources. J Esthet Restor Dent. 2006;18(4):214-222.
19. Leonard DL, Charlton DG, Hilton TJ. Effect of curing-tip diameter on the accuracy of dental radiometers. Oper Dent. 1999;24(1):31-37.
20. Price RB, Felix CM, Whalen JM. Factors affecting the energy delivered to simulated class I and class v preparations. J Can Dent Assoc. 2010;76:a94.
21. Price RB, McLeod ME, Felix CM. Quantifying light energy delivered to a Class I restoration. J Can Dent Assoc. 2010;76:a23.