Dental Unit Waterline Contamination: A Review of Research and Findings from a Clinic Setting
Abstract
The interior of small-diameter tubing in dental unit waterlines (DUWLs) creates an attractive environment for the growth of biofilm and bacteria. Substantial research shows that troublesome and potentially pathogenic bacteria have been found in DUWLs, and scant peer-reviewed information from which to evaluate chemical treatment options has been historically available. The authors' research compares three DUWL cleaners—an alkaline peroxide product, a freshly mixed chlorine dioxide product, and a buffer-stabilized chlorine dioxide product—in 16 dental units with self-contained water systems over a 10-day working period to determine the optimal chemical treatment option. The study found chlorine dioxide waterline cleaners to be most effective in containing DUWL contaminations.
Patients arrive at their dentists' offices with preconceived notions about the practice, including its cleanliness, the appropriateness of its instrumentation and equipment, and the knowledge and skills of its healthcare practitioners. Like other healthcare professionals, dentists have an ethical obligation to provide patients with a safe, clean clinical environment.
Occasionally, news reports about unsafe practices in dental offices place concerns about dental infection control procedures in the national spotlight, causing patients to question the safety of the dental offices they visit.1,2 When patients consider the cleanliness of their dentist's office, they are likely to focus on the appearance of the office or on the dental instruments they see used. However, it is often the unseen aspects of the practice that pose health and contamination risks, unbeknownst to the patient and possibly even to the dentist, hygienists, and other clinical personnel.
In light of these concerns, the authors review here the current status of the issue of dental unit waterline (DUWL) contaminations and, more specifically, their research on the optimal methods of treating those contaminations.
Background
Dr. G.C. Blake in Great Britain first reported the existence of contaminated water in dental units 50 years ago, finding that large numbers of bacteria were present in the water bottles and resultant aerosol sprays. Since then, dental unit water contamination findings have been confirmed in dozens of published research articles in dental journals worldwide.3-5 Research has, in fact, demonstrated that microbial counts can reach close to 200,000 colony-forming units per milliliter (CFU/mL), absent any contamination control procedures.6
Current research shows that worrisome and potentially pathogenic bacteria have indeed been found in DUWLs—including Legionella pneumophila, the causative agent of Legionnaire's disease, and Pseudomomas aeruginosa, which is associated with a wide range of opportunistic infections and pneumonia in hospital settings. However, measuring the amount of contamination and showing that it can lead to health risks for both patients and healthcare practitioners alike can be difficult. According to William Costerton, former Director of the Center for Biofilm Engineering at Montana State University-Bozeman, "current culturing techniques...may not represent the true microbial flora" present in and protected by the biofilm.7
Further complicating the issue in today's dental practices is practitioners' limited ability to provide dental care under specific, tightly controlled conditions such as those found in DUWL contamination studies, where infection from other sources can be controlled and systematically ruled out. This challenge was noted by Jennifer Cleveland of the Centers for Disease Control and Prevention (CDC), who said, "It is extremely difficult to establish an epidemiologic association between infection and recent exposure to dental unit water...because dentistry is typically performed in an outpatient setting, [and] patients are not monitored for post-treatment illness."8
Regulatory Approach
Despite the paucity of evidence indicating that DUWL contaminations have direct negative impact on public health, the CDC recognized that exposing patients to water of uncertain microbiological quality was inconsistent with accepted infection-control principles. In a 2000 article, Mills wrote, "[m]ost dental practices expend considerable effort and expense...as an everyday matter through surface disinfection, instrument sterilization, hand washing, and use of antimicrobial mouthrinses... As with recommendations to improve the quality of dental treatment water, few of the aforementioned procedures are based on strong epidemiologic evidence."5
Furthermore, an expert panel convened by the CDC found that, while this bacterial contamination may not be a concern to healthy individuals, it might place elderly or other immune compromised patients at unnecessary risk. Based on these findings, the CDC included recommendations in its dental practice guidelines in 2003 for management of DUWL contaminations.9
The American Dental Association (ADA) recommends that all practicing dentists and dental hygienists use standard precautions to protect patients and themselves by preventing the spread of disease.10 In 1995, the ADA Board of Trustees and ADA Council on Scientific Affairs adopted a joint statement on DUWLs, recognizing that the dental industry must "assume responsibility for assessing and improving the quality of dental care provided to patients" and requiring "widespread adoption of enhanced infection control methodologies by dental practitioners."11 The ADA challenged manufacturers of dental equipment to develop new approaches to improve dental water quality by the year 2000, so that water delivered to patients during nonsurgical dental procedures consistently contained no more than 200 CFU/mL of bacteria at any point in time.a Since 1995, according to ADA, technological advances have made this goal possible.11
In April 2012, the ADA reiterated, updated, and reinforced its Statement on Dental Unit Waterlines, noting that the scientific literature continued to support the need for the improvement in dental unit water quality; however, the ADA did not change or alter its prior recommendations regarding DUWL treatment specifications or standards.11
Treatment Options
While both the CDC and the ADA have recommended that DUWLs be flushed at the beginning of the clinic day to reduce the microbial load and then again between patients,12 numerous studies have demonstrated conclusively that this practice does not reliably improve the quality of water used during dental treatment.13,14 Other mechanical recommendations included chemical treatment regimens, the use of filters, and drying of DUWLs overnight.11 Of these latter two recommendations—filters and overnight drying—studies have shown that they are not very effective contaminant control mechanisms.15
Of the remaining recommendation—use of chemical treatment regimens—there was scant peer-reviewed information available in the early part of this decade from which to evaluate the options, and as a consequence, dentists knew little about the relative effectiveness of the various options that existed.7 Many dental practices began to use diluted concentrations of common household bleach, not only because it was deemed effective in controlling contaminations but also because it was easy to obtain and relatively inexpensive. Although research indicated that the use of bleach could improve water quality and reduce contamination, it was also found that multiple treatments were required to obtain those results, increasing the burden on staff time. This treatment option was also prone to operator error and was found to cause damage to the internal workings of dental unit water systems, and thus was deemed an ineffective option over time. Using sodium hypochlorite also has the potential for introducing potentially cancer-causing by-products, such as trihalomethanes, which are formed when chlorine interacts with the natural organic materials found in water.16
Study Description and Findings
Objective
The authors' research was intended to determine which of the three most commonly available chemical treatment options on the market were best in treating DUWL contaminations, considering their overall impact on contamination as well as the expense and staff time required to use each treatment.
Materials and Methods
Beginning in 2001, the authors began evaluating three of the most common remaining chemical treatment options under as tightly a controlled clinical regimen as possible. This research, which was conducted at the University of California San Francisco (UCSF) postgraduate periodontology clinic, considered the following three treatments over a 10 working-day period: an alkaline peroxide product (Sterilex® Ultra, Sterilex, www.sterilex.com); a freshly mixed chlorine dioxide treatment solution (DioxiClear™, Frontier Pharmaceutical, Inc., www.frontierpharm.com), and a stabilized chlorine dioxide treatment solution (MicroCLEAR, Rowpar Pharmaceuticals, www.rowpar.com).17,b
The UCSF clinic had 16 new chair-mounted dental units, which were divided into three separate treatment groups. All of the dental units were provided with a quick-connect fitting and approximately 8 feet of tubing to be attached during flushing to the base of the chair where the ultrasonic scaler waterlines are connected. The last chair served as the untreated control, which was maintained according to the manufacturer's suggestions: each night, the water bottle was emptied and reinstalled and the entire unit was purged of water; then each morning, the bottle was filled with tap water and the entire unit was flushed with water for 2 minutes. The only departure from the manufacturer's suggestions was that no disinfectant was used.
For the remaining test groups, the authors again followed the manufacturers' suggestions on use of the individual treatments. For Sterilex Ultra, one single-unit-dose packet was dissolved (the product forms a pink liquid in dissolution), placed in the water bottle, and the unit was flushed with product until the pink solution appeared at the end of the lines. The unit was allowed to stand with the product in it overnight. The next day, the unit was flushed through with hot water, and the bottle was then refilled with water for patient use. (Each bottle on the total of the 15 test units was filled during the day with either tap water for standard dental work or sterile saline for surgical procedures, as required.) This "shock" treatment was conducted on the first 3 days of the first week of testing, and the first day of week 2, for a total of 4 days of shock treatment. On the remaining 6 days, these chairs were treated the same as the control chair.
For DioxiClear, the "mix-upon-use" chlorine dioxide product, 60 mL each of the two-part product was mixed, placed in the water bottle, and the unit was flushed with the product until the bottle was empty. The unit was then flushed through with tap water, the bottle emptied, and the entire unit was purged of fluid and allowed to stand dry overnight. The next day, the water bottle was filled with tap water and with 1 mL of each of the two-part product, then flushed through for 2 minutes. As required during the day, the water bottle was refilled with the same amount of product and water.
Finally, for MicroCLEAR, the stabilized chlorine dioxide product, 150 mL of the product was put into the water bottle; the unit was flushed for 30 seconds and allowed to stand with the product in it overnight.c This "shock" treatment was conducted on the first day of the first week of testing. The next day, the water bottle was filled with tap water plus 75 mL of product, and flushed for 30 seconds. As required during the day, the water bottle was refilled with the same amount of product and water. (No product was added when sterile saline was used for surgical procedures.)
Samples were taken from each chair in the three test groups every morning after each of the waterlines was flushed for an additional 2 minutes, and were incubated for 7 days at room temperature.17 At the end of the incubation period, bacterial colonies were counted under a microscope, and repeat counts were conducted to ensure accuracy, without reference to the dental unit number, treatment regimen, or previous count. A second investigator did an independent count on each of the samples as well.
Results
The authors' criterion for "success" in conducting this research was whether or not the treatment was able to maintain the bacterial colony counts at or below the goal set by the ADA in 1995 of no more than 200 colony-forming units per mL of bacteria at any point in time in the DUWLs.
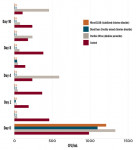
The control chair that was untreated with any specific bactericide seldom reached that goal of less than 200 CFU/mL. This is not surprising based on prior research on the efficacy of the use of flushing as a treatment method. Out of 10 samples over a 2-week period, counts were below 200 on the control chair only four times, with remaining counts ranging from 265 to 444 (Figure 1). The treatment process took approximately 4.5 minutes twice per day at no cost.
Of the three treatments investigated, the alkaline peroxide product was the least effective, meeting the ADA goal only on the 4 days immediately after the shock treatments (Figure 1). Although counts on those days were well under 100, they quickly climbed between shock treatments, with counts ranging widely from 257 to 575. The treatment itself took roughly the same amount of time as the control treatment (4.5 minutes), so it does not present a significant additional resource burden for the office staff. However, there were reports of the pink mix oozing out of the DUWL overnight, requiring cleanup. In addition, while the daily cost per dental unit was not prohibitive at only $0.86/day, it was 50% more expensive compared to the other treatments. There were no reports from patients of any odor, taste, or irritation from the presence of the product.
In contrast, both chlorine dioxide treatments were found to be extremely effective methods of treating the dental units for bacterial contamination, with dramatic drops from baseline counts in excess of 1,000 for both. Neither product showed counts in excess of 200 on any day and most counts were at 0 (Figure 1).
The DioxiClear product reduced the count to 0 on 7 of the 10 days, with the remaining counts lower than 5. However, the initial shock treatments took approximately 17 minutes in the evening and 9 minutes on subsequent mornings, and the daily care with diluted product took almost 6 minutes on a daily basis due to the need to measure and mix the two-part product. Based on the retail price of the product at the time, the daily cost per dental unit was the most affordable of all the treatments, at $0.11/day. There was only one report of a mild adverse reaction, with one patient commenting that the odor of the concentrate was irritating to nasal and air passages.
The MicroCLEAR product, after the initial shock treatment, had all counts on all samples and all chairs at 0 for the remainder of the study. The initial shock treatments took approximately 8 minutes in the evening and 6 minutes on subsequent mornings, and the daily care with diluted product took less than 4 minutes on a daily basis. Based on the retail price of the product at the time, the daily cost per dental unit was $0.35/day. There was only one report of a mild adverse reaction, with one patient commenting on a slight chlorine scent.
Conclusion
Any exposure of patients to water of uncertain microbiological quality is clearly inconsistent with high-quality standards of care in dental practice, and allowing this to happen is a failure to meet accepted principles of infection control. This is especially true for patients whose immune systems may be compromised and require a higher degree of care in these matters. Similar biofilms and bacteria present in hospital water systems have been shown to cause infections in hospitalized patients. There is also concern that the bacteria present in DUWLs may be associated with a refractory periodontitis that does not respond well to treatment.18,19 Clearly, dentists and dental hygienists need a reliable, efficient, and cost-effective method to treat these bacterial contaminations in dental unit waterlines.
Like many previous studies, the authors' research demonstrated that simply flushing the DUWLs and leaving them dry when not in use is an ineffective and inconsistent method of treating the contamination issue. Alkaline peroxide treatments require no more time for treatment than simply flushing, but have been found to be equally ineffective and inconsistent in reducing contamination and were among the more expensive treatment options available.
The chlorine dioxide products such as DioxiClear and MicroCLEAR were the most effective in treating the contamination, with MicroCLEAR consistently reducing bacterial counts to 0 after initial shock treatment.
Disclosure
Ms. Roth serves as a research consultant to Rowpar Pharmaceuticals, Inc., Scottsdale, Arizona.
About the authors
M. Robert Wirthlin, DDS, MS
Clinical Professor, Emeritus, Department of Oral and Craniofacial Sciences, Division of Periodontology, University of California San Francisco, San Francisco, California
Mollie Roth, JD
Managing Partner, PGx Consulting, Phoenix, Arizona
Footnotes
a. This threshold was based on the quality assurance standard established by organizations including the Environmental Protection Agency, the American Public Health Association, and the American Water Works Association for dialysate fluid used in hemodialysis and exceeded standards at the time for safe drinking water quality.
b. It was the authors' understanding that the two chlorine dioxide-generating products differed in their method of activation. DioxiClear is activated when the chlorite solution reacts to an acid upon mixing, generating a certain amount of chlorine dioxide gas. MicroCLEAR is activated when the stabilized chlorine dioxide reacts with acidogenic bacteria, generating a certain amount of chlorine dioxide gas. It was beyond the scope of their research to determine the optimum method for generating chlorine dioxide for the treatment of biofilms in the DUWL.
c. The manufacturer's recommendations for MicroCLEAR were modified by increasing the dosage by 50 mL based on the modifications made to the equipment required to conduct the testing.
References
1. Lupkin S. Rogue dentist may have exposed 7,000 patients to HIV, Hepatitis. ABC News. March 28, 2013. https://abcnews.go.com/Health/rogue-dentist-exposed-7000-patients-hiv-hepatitis/story?id=18834611. Accessed January 7, 2015.
2. Ricci ML, Fontana S, Pinci F, et al. Pneumonia associated with a dental unit waterline. Lancet. 2012;379(9816):684.
3. Atlas RM, Williams JF, Huntington MK. Legionella contamination of dental-unit waters. Appl Environ Microbiol. 1995;61(4):1208-1213.
4. Kelstrup J, Funder-Nielsen TD, Theilade J. Microbial aggregate contamination of water lines in dental equipment and its control. Acta Pathol Microbiol Scand B. 1977;85(3):177-183.
5. Mills SE. The dental unit waterline controversy: defusing the myths, defining the solutions. J Am Dent Assoc. 2000;131(10):1427-1441.
6. Barbeau J, Tanguay R, Faucher E, et al. Multiparametric analysis of waterline contamination in dental units. Appl Environ Microbiol. 1996;62(11):3954-3959.
7. Depaola LG, Mangan D, Mills SE, et al. A review of the science regarding dental unit waterlines. J Am Dent Assoc. 2002;133(9):1199-1206.
8. Organization for Safety, Asepsis and Prevention (OSAP). Dental Unit Waterlines: Questions and Answers. https://www.osap.org/?page=Issues_DUWL_1. Accessed January 7, 2015.
9. Centers for Disease Control and Prevention. Guidelines for Infection Control in Dental Health-Care Settings–2003. https://www.cdc.gov/mmwr/preview/mmwrhtml/rr5217a1.htm. Accessed January 7, 2015.
10. American Dental Association. ADA Statement on Infection Control in Dental Settings. March 29, 2013. https://www.ada.org/en/press-room/news-releases/2013-archive/march/ada-statement-on-infection-control-in-dental-setti. Accessed January 7, 2015.
11. American Dental Association. Oral Health Topics. Dental Unit Waterlines. https://www.ada.org/1856.aspx. Accessed January 7, 2015.
12. Centers for Disease Control and Prevention. Recommended Infection-Control Practices for Dentistry, 1993. https://www.cdc.gov/mmwr/preview/mmwrhtml/00021095.htm. Accessed February 6, 2015.
13. Williams JF, Johnston AM, Johnson B, et al. Microbial contamination of dental unit waterlines: prevalence, intensity and microbiological characteristics. J Am Dent Assoc. 1993;124(10):59-65.
14. Santiago JI, Huntington MK, Johnston AM, et al. Microbial contamination of dental unit waterlines: short- and long-term effects of flushing. Gen Dent. 1994;42(6):528-535.
15. Pankhurst CL, Philpott-Howard JN, Hewitt JH, Casewell MW. The efficacy of chlorination and filtration in the control and eradication of Legionella from dental chair water systems. J Hosp Infect. 1990;16(1):9-18.
16. Centers for Disease Control and Prevention. The Safe Water System. Disinfection By-Products. https://www.cdc.gov/safewater/chlorination-byproducts.html. Accessed February 6, 2015.
17. Wirthlin MR, Marshall GW Jr, Rowland RW. Formation and decontamination of biofilms in dental unit waterlines. J Periodontol. 2003;74(11):1595-1609.
18. Barbeau J, Gauthier C, Payment P. Biofilms, infectious agents, and dental unit waterlines: a review. Can J Microbiol. 1998;44(11):1019-1028.
19. Listgarten MA, Lai CH, Young V. Microbial composition and pattern of antibiotic resistance in subgingival microbial samples from patients with refractory periodontitis. J Periodontol. 1993;64(3):155-161.