Achieving Esthetic and Functional Objectives with Additive Equilibration
Abstract:
In a case involving a patient with high esthetic demands who wanted to keep treatment conservative, minimal direct bonding was used to enhance anterior esthetics while creating acceptable function. Primary treatment goals in the case, in which the patient was diagnosed with a constricted chewing pattern, were to improve esthetics by lengthening the maxillary anterior teeth and to stop continued loss of anterior tooth structure. Through the use of a Kois deprogrammer, an additive equilibration with direct composite was done to provide proper occlusal function to support the esthetic outcome, and no tooth reduction was needed.
An esthetic solution for minimal tooth wear may seem simple. However, functional considerations can complicate treatment planning. The restorative dentist must assess the patient’s esthetic desires and financial expectations and consider the amount and length of treatment necessary for success while selecting the best option from the myriad of available restorative possibilities. In order to create and execute a restorative plan that maintains tooth structure as well as meets all aspects of the patient’s goals, a clinician needs a solid understanding of comprehensive treatment planning.
This case required minimal direct bonding to enhance the anterior esthetics and create acceptable function. Through use of the Kois deprogrammer, an additive equilibration with direct composite was done to provide proper occlusal function to support the excellent esthetic outcome.
Clinical Case Overview
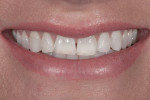
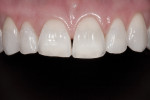
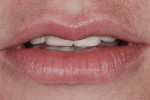
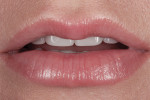
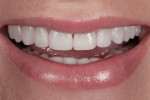
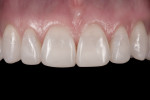
A 33-year-old female dental hygienist presented with a chief complaint regarding the esthetics of her maxillary anterior teeth. She disliked the irregular incisal edges that were thinning and desired longer teeth in general (Figure 1). While her esthetic demands were high, she wanted to keep the treatment as conservative as possible.
The patient’s medical history was unremarkable. Her dental history included two previous orthodontic treatments to correct mild crowding. She had been noncompliant with her retainers after the first orthodontic treatment and, therefore, completed orthodontic treatment a second time. She was a habitual soda drinker but was attempting to limit her intake.
Diagnostic Findings, Risk Assessment, and Prognosis
Extraoral examination and oral cancer screening were within normal limits.
Periodontal: Comprehensive periodontal probing revealed most pocket depths at 3 mm or less with no bleeding on probing. A few molars presented isolated 4-mm pocket depths with light bleeding on probing. Clinically, there were no signs of mobility. Radiographic examination of alveolar bone levels were within 2 mm of cementoenamel junctions with no infrabony defects. There were no shared risk factors for bone loss. Mild abrasion and recession of less than 1 mm was exhibited on teeth Nos. 5, 6, 11, and 12. The resulting periodontal diagnosis was AAP type 1.
Risk: Low
Prognosis: Good
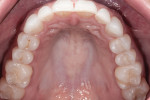
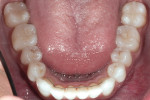
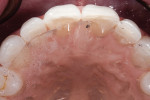
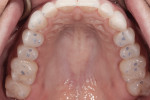
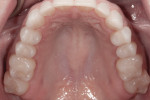
Biomechanical: There was mild erosion as a shared risk factor for non-cervical carious lesions on teeth Nos. 5, 6, 11, and 12. Upon clinical examination, several small direct restorations of acceptable condition in the pit and fissure areas of the premolars were noted. The glass silicate restorations present in teeth Nos. 12, 13, 20, 21, 28, and 29 had been placed more than 20 years ago (Figure 2 and Figure 3). There was no history of interproximal carious lesions, nor was there an indication of active caries, either clinically or radiographically.
Risk: Low (Although the frequent intake of soda was a high-risk social behavior, it had not resulted in the expression of caries at the present time.)
Prognosis: Good
Functional: The patient had a normal range of opening. An immobilization test and loading test produced no joint pain or muscle discomfort, and no temporomandibular joint noises were present. There was mild to moderate attrition noted on teeth Nos. 6 through 11 and 22 through 27 (Figure 4). The anterior wear facets noted on the lingual of the maxillary anterior teeth and incisal/facial aspects of the mandibular anterior teeth, along with the lack of posterior tooth wear, was evidence of a constricted envelope of function.1 In her case, the adaptation to the constriction was manifested in tooth wear and not muscular or joint dysfunction. There was no history of neurologic disorders, and the patient had no awareness of any sleep bruxism.
Risk: Moderate
Prognosis: Fair
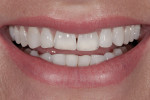
Dentofacial: Photography is essential for analyzing dentofacial esthetics. The repose position first determines the maxillary incisal edge position. The maxillary canines are the reference point when evaluating the amount of tooth exposed with the lips in repose since this is less dependent on lip length and is not age- or gender-specific.2 With lips at rest the canines should be at the same length as the lip, noted as the “0” display of the canine. The patient’s canines were at “0” position, but the maxillary centrals and laterals were deficient in length (Figure 5).
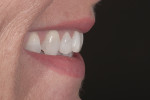
Although the repose photograph provided necessary information regarding the ideal incisor length, additional photographs were necessary to finalize the esthetic treatment plan. The full-smile photographs revealed the extent of the patient’s lip mobility (Figure 6), and the lateral photographs demonstrated the retrusive nature of the maxillary central incisors (Figure 7), which may not have been evident from the frontal view photographs. Risk assessment is based on amount of tooth and tissue display in full smile and in repose. The patient had medium lip dynamic as evidenced by an inability to fully display her gingival architecture. Exceeding the patient’s expectations, then, was more likely and less difficult considering the lip dynamics; however, the patient also had high esthetic demands as a result of her profession as a dental hygienist.
Risk: Moderate
Prognosis: Fair
Treatment Plan
The patient’s primary objective was to improve esthetics by lengthening the maxillary anterior teeth. She also wanted to stop continued loss of anterior tooth structure. Since the patient’s functional diagnosis was a constricted chewing pattern, the cause of the anterior wear was excess friction between the anterior teeth during function. Simply adding more length to the teeth would increase the amount of friction in the envelope of function and increase the risk of restorative failure. Therefore, additional treatment would be necessary to “unconstrict” the chewing pattern, decrease friction, and increase the freedom of movement.3 An orthodontic solution to labially reposition the maxillary anterior teeth and lingually reposition the mandibular anterior teeth was one treatment option.
Having had two previous orthodontic treatments, the patient was unwilling to undergo further orthodontic treatment. The other option was to open the vertical dimension of occlusion restoratively with an additive approach using direct resin bonding, which was the choice the patient accepted. This would create enough room for increased tooth length, thereby satisfying the patient’s esthetic desires while providing the stable occlusion necessary to improve function and protect the longevity of the restorations.4
Phase 1: Establish Centric Relationship and Complete Additive Equilibration
The Kois deprogrammer was used to establish an accurate and repeatable centric relation position. The patient wore the appliance continuously for 2 weeks, except during meals. Though she had no symptoms before treatment, it was important to ensure that no new symptoms arose while wearing the appliance.
The immobilization and loading tests were done again and produced no joint pain or muscle discomfort, and no temporomandibular joint noises were present. A reproducible, single point of contact with the absence of symptoms was accomplished and verified (Figure 8). When removing the deprogrammer, the first point of contact noted was the disto-lingual of tooth No. 8, thus confirming the diagnosis of a constricted chewing pattern.
A quick intraoral mock-up of the proposed incisal length was done for the patient to visualize the proposed incisal lengths, as well as to verify that the additive occlusal equilibration would provide adequate space for the new incisor length. The canines had previously been determined to be the correct length, so the amount added to the centrals and laterals leveled the occlusal plane and created an ideal smile design relative to the present position of the canines.5,6 The incisors were spot-etched and composite was added to the incisal edges, creating a tooth length that was acceptable to the patient.
Once the correct incisor length was determined, a new vertical dimension was established to provide adequate space to accommodate the new length without encroaching on the envelope of function. The platform of the Kois deprogrammer was adjusted to the new vertical dimension. With the deprogrammer in place, direct composite was added to the lingual surfaces of the maxillary canines and checked with shimstock (Almore International, www.almore.com). To achieve the treatment goal of a solid occlusal “home” at the new vertical dimension, the same protocol was followed, and composite was added to the occlusal surfaces of the maxillary teeth, beginning with the first premolars, then the second premolars and first molars. The deprogrammer was removed and the posterior contact points were refined with Trollfoil articulating paper (TrollDental, www.TrollDental.com) and verified with shimstock to assure equal, simultaneous, bilateral contacts on posterior teeth with light contacts in centric relation position on the lingual surfaces of the maxillary canines.
Phase 2: Execute Esthetic Solution
Immediately after completion of the additive occlusal adjustment, the composite mock-up on the maxillary incisors was removed and the teeth cleaned with pumice paste (Pumice Preppies™, Whipmix, www.whipmix.com) in a rubber cup in preparation for final bonding protocol. Since all enamel was unprepared, teeth Nos. 6 through 11 were microabraded with 27-micron aluminous oxide at 40 psi (PrepStart™, Danville Materials, www.danvillematerials.com) and etched with 35% phosphoric acid (Ultra-Etch®, Ultradent Products, Inc., www.ultradent.com) for 60 seconds. Adhesive resin (iBond®, Heraeus Kulzer, www.heraeus-dental-us.com) was bonded to the teeth, followed by placement of composite resin (Venus Diamond®, Heraeus Kulzer) to establish the previously accepted incisal edge position.7
The composites were shaped and polished with a series of discs and aluminum oxide paste (Enamelize™, Cosmedent, Inc., www.cosmedent.com). The anterior chewing envelope was then marked with 200-micron paper (Bausch, www.bauschdental.com) while the patient chewed gum and was seated in an upright position. All streaks on the lingual surfaces of the maxillary centrals and laterals were removed to ensure there was no friction. Bilateral, simultaneous posterior point-contacts and canine guidance were achieved intraorally (Figure 9 and Figure 10).
Conclusion
The patient was very pleased that absolutely no tooth reduction had been required to achieve her esthetic expectations and create an occlusion that would reduce the risk of further tooth wear (Figure 11 through Figure 14). While her chief concern had been esthetics, it was critical to understand all the risk factors in order to design a treatment plan that minimized all risks. The Kois deprogrammer was used to find, establish, maintain, and verify an acceptable vertical dimension in centric relation throughout the process. All composite restorations were kept in enamel, which did not increase biomechanical risk. Any risk of future failure would be in the restorations instead of tooth structure.
The constricted chewing pattern was resolved with occlusal management and decreased concern for wear on the anterior teeth. This lowered the patient’s functional risk and improved the prognosis. The periodontal risk and prognosis remained the same, while the dentofacial prognosis was raised from fair to good, and the patient’s desire for improved esthetics was achieved.
ACKNOWLEDGMENT
The author would like to thank John C. Kois, DMD, MSD, for his educational instruction and guidance through the years.
ABOUT THE AUTHOR
Amanda Seay, DDS
Private Practice, Mount Pleasant, South Carolina
REFERENCES
1. Kois JC. Functional Occlusion: Science Driven Management Manual. Seattle, WA: Kois Center; January 2011:79.
2. Kois JC. New Challenges In Treatment Planning- Part 2: Incorporating The Fundamentals of Patient Risk Management. Journal of Cosmetic Dentistry. 2011;27(1):110-123.
3. Dawson PE. Centric relation. In: Dawson PE. Evaluation, Diagnosis and Treatment of Occlusal Problems. 2nd ed. St. Louis, MO: Mosby; 1989:28-55.
4. Kois JC, Philips KM. Occlusal vertical dimension: alteration concerns. Compend Contin Educ Dent. 1997;18(12):1169-1177.
5. Terry DA. Aesthetic and Restorative Dentistry: Material Selection and Technique. Stillwater, MN: Everest Publishing Media; 2009.
6. Rufenacht CR. Principles of Esthetic Integration. Chicago, IL: Quintessence Publishing; 2000.
7. Fahl N Jr. Single-shaded direct anterior composite restorations: a simplified technique for enhanced results. Compend Contin Educ Dent. 2012;33(2):150-154.