Hand Hygiene in the Dental Setting: Reducing the Risk of Infection
Abstract:
Hand hygiene remains the single most important measure for reducing the risk of healthcare-associated infections. In the past 20 years, hand-washing recommendations and guidelines have become increasingly complex, and a plethora of products have become available. This article aims to discuss and clarify the fundamentals of appropriate hand hygiene in dentistry.
Hand washing once seemed so simple. At home, hands were to be washed before meals, after personal functions, and before bed. However, no specific instructions were given other than, “Go wash your hands.” Children might dip their hands into water, then smear them on a towel to complete this seemingly meaningless chore, which was performed without a sense of exactly what constituted a “job well done” and why it was important. While hand hygiene for healthcare professionals is more involved than household hand care, similar misunderstandings exist. This may lead to inadequate or non-compliance, and suggests the need for further education and clarification of hand hygiene in healthcare settings.
During the past 20 years, hand-washing recommendations and guidelines have seemingly become increasingly complex. The term “hand washing” has been replaced with “hand hygiene,” and there seems to be excessive information about indications and techniques. There is also a plethora of products available. Knowing exactly what hand hygiene information is relevant, credible, or necessary for dental personnel can be confusing. The purpose of this article is to discuss and clarify the “who, where, when, what, and how” of appropriate hand hygiene in dentistry.
Who Needs to Perform Hand Hygiene?
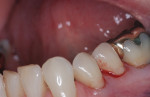
Every year, organisms on the hands of healthcare personnel are responsible for many of the more than 2 million documented healthcare-associated infections, the majority of which occur in in-patient settings such as hospitals and long-term care facilities.1 Hand hygiene is considered to be the single most critical measure for reducing the risk of transmitting organisms to patients and healthcare workers.2 As the principles of infection control are universal, hand hygiene is equally important in the dental setting. A routine dental treatment such as dental prophylaxis, matrix band placement, crown preparations near gingival margins, and endodontic procedures all provide opportunities for microorganisms on a clinician’s hands to be transferred to the patient’s mucous membranes or into the patient’s bloodstream (Figure 1). In addition, personnel who touch contaminated dental instruments, surfaces, tissue, or body fluids with their bare hands may transfer microorganisms to themselves. Because dental personnel visit several rooms and touch numerous clinical and non-clinical objects throughout the work day (Figure 2), their hands may become a mode of infection transmission and they, therefore, must be cleaned at specific times during the course of patient care. As effective hand hygiene protects both the patient and dental professional, hand hygiene practices combined with wearing gloves are essential elements of infection control.3
Where on the Skin Are Microorganisms Found?
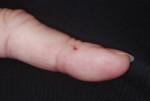
Microorganisms are located in both the outer surface and deeper layers within the skin. Deeper layers within the skin contain the resident flora—microorganisms that normally reside on a person’s body. These microorganisms are not easily removed and are not commonly associated with disease transmission. The transient flora consist of microorganisms on the outer surface of the skin that are associated with healthcare acquired infections.1 In the dental operatory, these microorganisms may be acquired by touching contaminated body fluids such as blood, saliva, or dental plaque, or contaminated surfaces and objects. These microbes may pass through defects in the epidermis and infect dental personnel or be transferred to other patients (Figure 3). The transient flora are more easily removed or inactivated by hand hygiene. The goal of hand hygiene is to reduce resident flora and remove transient flora from the hands of dental healthcare personnel.2
When Should Hand Hygiene Be Performed; What Products Should Be Used?
Clinicians should wash hands with either plain soap or an antimicrobial hand wash at the beginning of the work day for 1 full minute. Hands should also be washed when they are visibly soiled, after they have become contaminated, before glove donning, and after glove removal. If gloves have been torn or punctured, they should be removed, and hand hygiene should be repeated (Figure 4).4
Acceptable products for hand hygiene and hand care in a clinical setting include plain soap, antimicrobial soap, alcohol hand rubs, and appropriate lotions. It is recommended that products used are manufactured for healthcare personnel, as these products are generally unscented, have fewer allergenic components, and are meant to be used repeatedly throughout the work day.1 These products also contain emollients such as glycerin or aloe to soften hands and keep the epidermis intact. Alcohol-based hand rubs kill microorganisms more effectively and more quickly than hand washing with soap and water.5 They are also less damaging to skin, resulting in less dryness and irritation. In addition, they require less time, and since they may be placed at the point of care, they are also more accessible and may enhance compliance.6 However, alcohol hand rubs do not physically remove debris from hands; thus these products should not be used if hands are visibly soiled (Figure 5).
Specific recommendations for hand hygiene products include the following:
Plain soap is recommended: if hands are visibly soiled; before donning gloves and after glove removal; before eating; and after personal functions.
Antimicrobial soap is recommended: if hands are visibly soiled or contaminated with blood or other body fluids; before donning gloves and after glove removal; before eating; and after personal functions.
Alcohol-based hand rubs are recommended: if hands are not visibly soiled; and before donning gloves and after glove removal.
Surgical hand scrub or soap antisepsis (either antimicrobial soap or a combination of non-antimicrobial soap, water, and alcohol-based surgical hand rub) is recommended before surgical procedures. Follow manufacturer’s instructions for quantity of product to be used.
Lotions: The frequent use of lotions is suggested to ease the dryness resulting from frequent hand washing and to prevent dermatitis. Petroleum-based lotions can weaken latex and synthetic gloves and increase permeability and should not be used in a clinical setting. It is recommended to use products specifically manufactured for healthcare providers, as these are generally compatible with gloves and they contain fewer scents that may be offensive or allergenic to clinicians or patients.7
How Should Hand Hygiene Be Performed?
Although proper techniques may appear to be simply common sense, specific steps are required for hand washing in the dental setting:
• Wet hands completely with warm water. Extremely hot or cold water should be avoided, as temperature extremes may increase the risk of dermatitis.
• Rub hands together thoroughly for at least 15 seconds, making sure to cover all surfaces of the hands and fingers (Figure 6).
• Rinse hands thoroughly (Figure 7).
• Dry hands thoroughly.
• Turn off manual faucets using a disposable towel to prevent recontamination of hands (Figure 8).8
If using an alcohol-based hand rub, it should be applied to dry hands using the amount specified by the manufacturer (Figure 9).4 Rub hands together, covering all surfaces and fingers, for at least 15 seconds until hands are dry. (If hands are dry after 10 seconds of alcohol-based hand rub usage, it is likely that too little of the product was used.)9
Surgical hand antisepsis is more technique-sensitive and elaborate than hand hygiene for routine dental procedures. Rings, bracelets, and all other hand and wrist jewelry must first be removed. Under running water, fingernails are cleaned to remove debris. Since bacteria on skin can multiply rapidly under gloves, it is highly recommended that surgical hand antisepsis be performed using products with “persistent activity.” Antimicrobial soaps or alcohol-based hand rubs with persistent activity prevent pathogens from surviving on hands for an extended period of time after application. Although over-the-counter antimicrobial products may be purchased at virtually any store, clinicians should use products for surgical hand antisepsis (as well as products for routine dental care) that have been manufactured specifically for healthcare professionals.1
For surgical hand antisepsis using an antimicrobial soap, hands and forearms should be scrubbed together for the length of time recommended by the manufacturer of the product—typically 2 to 6 minutes. Hands and forearms should be rinsed and dried thoroughly before donning surgical gloves.
For surgical hand antisepsis using an alcohol-based hand rub, hands and forearms should be prewashed with a non-antimicrobial soap and dried thoroughly. The hand-rub product should be applied following the manufacturer’s instructions for quantity of product to use (typically, a greater quantity than for routine hand hygiene), and hands and forearms should be allowed to dry thoroughly prior to donning sterile surgical gloves.4
Why Shouldn’t Jewelry or Artificial Nails Be Worn?
The effectiveness of hand hygiene can be reduced by both the presence of jewelry and artificial nails.10 Long or artificial nails as well as rings make glove donning and removal more difficult and make glove tears more likely. Additionally, bacterial counts are higher on hands with long or artificial nails and nails with chipped polish.11 Thus, it is recommended to keep fingernails unpolished and short with rounded, filed edges (Figure 10). Therefore, the wearing of hand jewelry while providing routine dental care is strongly discouraged; it is prohibited during surgical procedures.
Conclusion
The past 20 years have brought about changes in hand care recommendations and guidelines for healthcare professionals. Research and development of new products and techniques may seem to have complicated the hand hygiene process, but the fundamental principle remains: Hand hygiene is the single most important measure for reducing the risk of healthcare-associated infections. Contaminated hands continue to be a mode of infection transmission during patient care, and effective hand hygiene practices protect both patients and team members. Although many products are available for hand care, it is recommended that healthcare workers use products that are manufactured for use in healthcare settings. All dental team members should be educated on the importance of proper hand hygiene, as it is critical to the success of any infection control program.
ABOUT THE AUTHOR
Marie T. Fluent, DDS
Clinical Instructor, Dental Assisting Program, Washtenaw Community College, Ann Arbor, Michigan;
Private Practice, Arbor Lodge Dental, Ann Arbor, Michigan;
Assistant Editor, THE DENTAL ADVISOR
REFERENCES
1. Andrews N, Cuny E, Molinari JA. Antisepsis and hand hygiene. In: Molinari JA, Harte JA, eds. Cottone’s Practical Infection Control in Dentistry. 3rd ed. Philadelphia, PA: Lippincott, Williams, and Wilkins; 2010:125.
2. Kohn WG, Collins AS, Cleveland JL, et al. Guidelines for infection control in dental health-care settings—2003. MMWR Recomm Rep. 2003;52(RR-17):14.
3. Girou E, Chai SH, Oppein F, et al. Misuse of gloves: the foundation for poor compliance with hand hygiene and potential for microbial transmission? J Hosp Infect. 2004;57(2):162-169.
4. Boyce JM, Pittet D. Guideline for Hand Hygiene in Health-Care Settings. Recommendations of the Healthcare Infection Control Practices Advisory Committee and the HICPAC/SHEA/APIC/IDSA Hand Hygiene Task Force. Society for Healthcare Epidemiology of America/Association for Professionals in Infection Control/Infectious Diseases Society of America. MMWR Recomm Rep. 2002;51(RR-16):1-45.
5. Kampf G, Kramer A. Epidemiologic background of hand hygiene and evaluation of the most important agents for scrubs and rubs. Clin Microbiol Rev. 2004;17(4):863-893.
6. Erasmus V, Daha TJ, Brug H, et al. Systematic review of studies on compliance with hand hygiene guidelines in hospital care. Infect Control Hosp Epidemiol. 2010;31(3):283-894.
7. Littau, CA, Thompson KM. Keep consumer hand lotions at home. American Nurse Today. April 2011;6(4). https://www.americannursetoday.com/article.aspx?id=7700&fid=7658. Accessed July 12, 2013.
8. World Health Organization. WHO Guidelines on Hand Hygiene in Health Care. Geneva, Switzerland: World Health Organization; 2009. https://whqlibdoc.who.int/publications/2009/9789241597906_eng.pdf. Accessed July 12, 2013.
9. Molinari JA. Clinic experiences with waterless alcohol-based hand hygiene antiseptics. Compend Contin Educ Dent. 2006;27(2):84-86.
10. Hedderwick SA, McNeil SA, Lyons MJ, Kauffman CA. Pathogenic organisms associated with artificial fingernails worn by healthcare workers. Infect Control Hosp Epidemiol. 2000;21(8):505-509.
11. Gupta A, Della-Latta P, Todd B, et al. Outbreak of extended-spectrum beta-lactamase-producing Klebsiella pneumoniae in a neonatal intensive care unit linked to artificial nails. Infect Control Hosp Epidemiol. 2004;25(3):210-215.