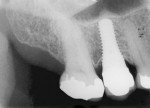
Immediate Implant Placement in Posterior Areas, Part 2: The Maxillary Arch
Abstract:
In Part 1, the authors discussed general principles regarding implant placement in the mandibular molar areas. Here in Part 2, the focus is on implant placement in maxillary posterior regions along with various restorative considerations. The objective is to impart an understanding of the potentials and limitations of various restorative therapies to enable clinicians to determine the circumstances under which they should select a particular option among the available therapies in the treatment of compromised posterior teeth.
A discussion of general principles and implant placement in the mandibular molar areas was carried out in Part 1 (Compendium, July/August 2012, Vol. 33 No. 7, pp 494-507). While Part 2 will focus upon implant placement in maxillary posterior regions and additional restorative considerations, it is imperative to realize that the conceptual and treatment planning tenets discussed in Part 1 apply equally as well to the maxillary arch.
Maxillary Molar Replacement with Implant-Restored Prosthetics
A variety of treatment options present themselves at the time of maxillary molar tooth extraction, including the following:
1. Augmentation of the extraction socket defect utilizing particulate material and a secured covering membrane may be mandated when faced with one or more of the following:
Anticipated implant placement and restoration within the patient’s esthetic zone, in the face of a severely compromised buccal alveolar ridge
Anticipated implant placement in an extraction socket defect with inadequate residual interradicular bone for fixation of the implant in the desired restorative position, due to root morphology or pathologic bone destruction
Anticipated implant placement in a residual extraction socket that is too wide to stabilize the implant in the desired restorative position
2. Implant placement in a residual extraction socket defect followed by utilization of appropriate particulate materials and covering membranes to facilitate regeneration of alveolar bone in the residual extraction socket defect surrounding an appropriately sized implant.
3. Implant placement in the extraction socket following implosion of a core of autogenous bone apical to the extraction socket. Particulate materials and a covering membrane are then placed to facilitate regeneration of alveolar bone in the residual extraction socket defect surrounding the implant.
4. Lateral sinus augmentation therapy and augmentation of the residual extraction socket defect utilizing particulate material and membrane.
5. Lateral sinus augmentation therapy with simultaneous implant placement and regeneration of alveolar bone in the residual extraction socket defect surrounding the implant, through the use of particulate material and the appropriately secured covering membranes.
It is imperative that the definition of success following augmentation of extraction socket defects be established prior to material and treatment selection. A comprehensive definition of success following such therapy must include both regeneration of bone within the extraction socket and regeneration of prepathologic alveolar ridge morphology, including buccal and palatal/lingual alveolar bone line angles, so as to ensure adequate thickness of bone on the buccal and palatal/lingual aspects of the implant and appropriate hard-tissue support of the soft-tissue drape of esthetics around the restored implant. Such conceptualization, while more technically rigorous and demanding of specific materials and treatment protocols, at least diminishes and usually eliminates the need for secondary soft-tissue grafting procedures.
Placement of implants in maxillary posterior areas is highly patient- and site-specific. Prior to initiating such therapy, whether at the time of tooth removal or in edentulous areas, a determination must be made regarding the minimum implant dimensions necessary in the context of the patient’s individualized treatment plan. Following such a determination, an assessment must be made of whether or not an implant of the desired dimensions may be placed in an ideal restorative position either at the time of tooth removal, or in an edentulous site with or without concomitant regenerative therapy. If such a determination is in the negative, regenerative treatments must be undertaken prior to considering implant placement.
Augmentation and Implant Placement at Time of Maxillary Molar Extraction
Augmentation without Simultaneous Implant Placement
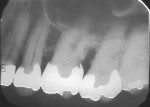
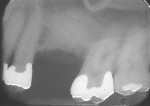
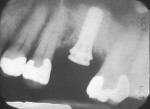
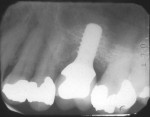
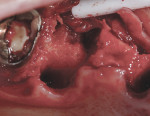
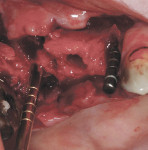
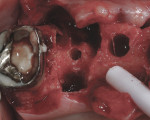
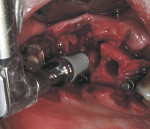
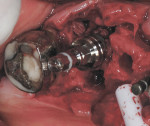
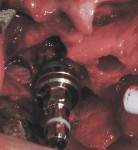
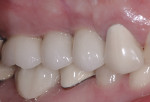
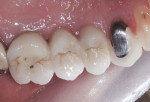
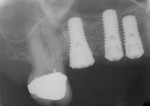
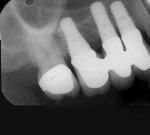
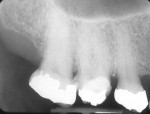
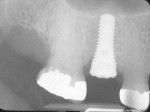
If either the root morphology of the maxillary molar to be replaced or the extent of periodontal alveolar bone destruction around the hopeless tooth preclude appropriate implant placement at the time of tooth extraction, an augmentation should be carried out upon tooth removal, and the implant placed in a subsequent surgical session. In this situation, the tooth is sectioned and each root is removed utilizing piezo surgery and specifically designed periotomes, with care being taken to preserve the interradicular bone. Upon defect debridement, a trephine with sufficient diameter to encompass the interradicular bone is placed over the interradicular bone, and an osteotomy is prepared to within 1 mm of the sinus floor. If the sinus membrane appears to invaginate around the extraction socket radiographically, thus presenting a potential compromise should any apical preparation of the extraction socket be carried out with a trephine, an osteotome is applied to the interradicular bone prior to trephine utilization, and gently malleted. In such situations, if the interradicular bone implodes upon such gentle malleting, no trephine use is necessary. However, should the interradicular bone prove immobile in the face of osteotome malleting without trephine utilization, the trephine is employed as described above, and an osteotome is subsequently utilized to displace the prepared bone core apically, thus lifting the sinus membrane in the area of the interradicular bone.
A core is always imploded to a depth 1 mm less than the depth of the trephine cut. If no trephine had been utilized, the core is imploded 1 mm less than the height of the interradicular bone. Such care is taken so as to both help preserve the intact nature of the displaced sinus membrane and to keep the core within the borders of the alveolar bone, thus ensuring it does not become “free-floating” in the sinus. Particulate materials are placed, the appropriate covering membrane is secured with fixation tacks, and flap designs are utilized to ensure passive primary closure, as described in previous publications.1-3 Following bone regeneration, sufficient bone will be present in the previous interradicular area for appropriate implant placement.
A clinical example of this treatment approach is evident in Figure 1 through Figure 4.
Implant Placement at Time of Maxillary Molar Extraction
If adequate interradicular bone is present to effect placement of an implant of the desired dimensions in an ideal restorative position following tooth sectioning and gentle extraction of a maxillary molar, both the interradicular bone morphology and the need or lack of need for additional bone height must now be assessed. Following such an assessment, therapy will proceed in one of the following four manners.
If No Additional Alveolar Bone Height Is Required:
1. When a wide interradicular septum is present—with wide being defined as a septum that will completely cover the rough surface of the implant following its manipulation—a 2.2-mm guide drill is used to prepare the initial osteotomy to its final depth. Tapered osteotomes, of sequential diameters that correspond to the implant drilling sequence, are utilized to spread the interradicular bone. While the most crestal aspect of the interradicular bone is usually split or lost, this is of no consequence. The interradicular bone manipulation creates an osteotomy of sufficient dimension to accept the planned implant and compacts the bone laterally, which helps stabilize the inserted implant. Either a parallel walled wide platform implant or a tapered implant with a 4.8-mm-wide “apex” and a 6.5-mm-wide platform is inserted, depending on the final morphology of the manipulated interradicular bone. If utilization of a tapered implant would result in loss of significant portions of the interradicular bone as it broadens in its most crestal third, a parallel walled implant is placed. The advantages to tapered end implant use are both greater obliteration of the residual extraction socket defect surrounding the implant, and an increased implant surface area available for osseointegration. If particulate materials and the appropriate secured covering membrane are placed around the implant, the flaps are manipulated as previously described to ensure passive primary closure throughout the course of regeneration. However, if the use of a tapered implant has either obliterated the residual extraction socket defect or resulted in a horizontal defect dimension of 3 mm or less, no regenerative materials are employed. The ability to eliminate the need for regenerative materials and, thus, place the implant in a one-stage manner is also dependent upon having extracted the tooth as atraumatically as possible and leaving the alveolar walls of the extraction socket intact.
2. When a narrow interradicular bony septum is evident following tooth sectioning and extraction—with narrow being defined as a septum that will not encompass the rough surface of the implant
body following its manipulation—different site preparation protocols and implant selection are employed. Piezo surgery is used to notch the most crestal aspect of the interradicular bone, providing a set point for use of a tapered osteotome, which is employed to the final depth of the planned osteotomy. Sequentially widening tapered osteotomes, whose diameters correspond to the drilling sequence of the implant system to be utilized, spread and shape the residual interradicular bone to the final osteotomy depth. The osteotomy is only widened to 3.5 mm, not 4.2 mm as would be necessary for placement of a parallel walled or tapered end conventional wide platform implant. Instead, an implant is used that has a 4.1-mm-wide “apex” and a 6.5-mm-wide platform, affording the opportunity to place the implant into the manipulated interradicular bone and attain primary stability without unduly widening this interradicular bone, which could cause loss of its integrity and its stabilizing function. Appropriate regenerative materials and covering membranes are placed and flap designs are utilized, as previously described. This approach is demonstrated in Figure 5 through Figure 14.
If Additional Bone Height Is Required in the Interradicular Area:
When inadequate alveolar bone height is present crestal to the floor of the sinus for placement of an implant of the desired dimensions, therapy proceeds in one of the following two manners, depending on the morphology of the interradicular bone.
3. If a wide interradicular septum is present, a 2.2-mm-wide trephine and flat-ended osteotome are utilized to implode the interradicular bone. The osteotomy site is widened with sequentially sized osteotomes, whose diameters correspond to the drilling sequence for the implant system to be used. Each osteotome is brought to the desired depth, with care once again being taken to ensure that the most crestal millimeter of the imploded interradicular core still rests within the apical confines of the residual alveolar bone. Once the desired osteotomy site has been prepared, either a straight walled implant with a 6.5-mm-wide platform or a tapered end implant with a 4.8-mm-wide “apex” and a 6.5-mm-wide restorative platform is placed, depending on the final morphology of the manipulated alveolar bone, as previously described. An example is shown in Figure 15 through Figure 17.
4. If a narrow interradicular septum is present, sequentially widening tapered end osteotomes are utilized to both implode the interradicular bone coronal to the floor of the sinus and widen the interradicular bone, in anticipation of accepting a tapered end implant with a 4.1-mm-wide “apex” and a 6.5-mm-wide restorative platform. The interradicular osteotomy is widened to 3.5 mm, the implant is inserted, and appropriate regenerative materials and flap designs are employed as previously described.
It should be noted that appropriate diagnosis of the morphology and health of the residual interradicular bone cannot usually be carried out prior to tooth sectioning and root removal. The only view afforded to the clinician by a periapical radiograph is the interradicular bone morphology and quantity between the mesio-buccal and disto-buccal roots of the first molar. The implant will be stabilized by the bone between the buccal roots and the palatal root. Therefore, a radiograph taken prior to tooth removal will offer limited information in situations where the buccal roots are convergent and/or fused.
The decision tree described above offers a framework in which to predictably augment the posterior maxilla with or without simultaneous implant placement at the time of maxillary molar extraction. In a study4 documenting 391 sites treated via implant placement at the time of maxillary molar extraction, a combination of parallel wall and tapered implants were utilized; after a mean time of 30.9 months in function, the cumulative success rate of the implants was 99.5%.
Implant Placement at Time of Maxillary Premolar Extraction
Tooth extraction of a maxillary premolar and defect debridement are carried out as previously discussed. The presence of periapical pathology is not a contraindication to either implant placement or regenerative therapy. Recent publications have documented implant survival rates for implants placed immediately in sites demonstrating active periapical pathology that are equal to those for implants placed in sites with no periapical pathology, both through retrospective studies and a study comparing both treatment modalities in 64 patients.5,6
Treating clinicians face a number of decisions regarding 3-dimensional (3-D) implant placement, implant dimension, and implant design when treating such an area.
When removing a two-rooted maxillary bicuspid, the tooth is hemisected and the roots are removed, as previously described. The most coronal aspect of the interradicular bone septum is removed with a rongeur, thus providing a more stable bony base for osteotomy preparation. When a single-rooted bicuspid is extracted, this step is omitted.
A ratio of the bucco-palatal to mesio-distal dimensions of the average maxillary first bicuspid demonstrates the unique morphology of the tooth. As such, a number of bucco-palatal implant positioning options present to the treating clinician, assuming a stable bony base has been established for osteotomy initiation, through removal or modification of the residual interradicular bone. These options include the following:
1. Implant placement in the area of the buccal root socket in the instance of a two-rooted bicuspid, or the buccal third of the extraction socket in instances where a one-rooted bicuspid is being replaced—While such an approach at first seems advantageous, as the implant is positioned close to the buccal corridor and in line with the buccal aspects of the adjacent teeth, it is undesirable for multiple reasons. The implant will be placed close to thin buccal bone, eliminating the possibility of placing a slow resorbing graft material between the implant and the buccal bony plate in anticipation of postoperative resorption of the thin, labile buccal bundle bone that is present. In addition, in order to provide the patient with a final restoration of acceptable size and dimensions, the final crown will exhibit a significant palatal cantilever, which is undesirable due to both force distribution and home care considerations.
2. Implant placement in the area of the palatal root socket in the instance of a two-rooted bicuspid, or the palatal third of the extraction socket in instances where a one-rooted bicuspid is being replaced—Such positioning is preferable to placement in the buccal third of the extraction socket, as procedures can be carried out to “preserve” bone on the buccal aspect of the implant. In addition, the restorative dentist is afforded greater flexibility in managing final restorative contours to help ensure the desired esthetic treatment outcome. The disadvantages to positioning the implant in the palatal third of the extraction socket include the creation of a buccal cantilever and ridge lap, and the possibility that the restoration will impinge on the tongue during speech and/or function, leading to patient dissatisfaction.
3. Implant placement in the interradicular bone or central third of the extraction socket, depending upon whether a two- or one-rooted tooth had been removed—In most instances, this approach is most desirable. While attainment of this position following extraction of a two-rooted tooth will require manipulation/removal of the interradicular bone and use of a differential pressure osteotomy technique, the result is an implant that is easily restored in a healthy, stable, and esthetic manner.
Implant Diameter and Depth
Limited mesio-distal dimension in the area of the average maxillary first bicuspid and the desire to have at least 2 mm between the implant and adjacent teeth have led many clinicians and manufacturers to advocate the use of a narrower diameter implant (3.3 to 3.8 mm) in this region. Because the maxillary first bicuspid bears a significant load during function, concerns have arisen regarding implant and abutment strength over time when such implant selection is made. The use of a titanium-zirconium alloy implant, which is considerably stronger than a corresponding titanium implant, helps ameliorate the concern regarding implant strength. However, when a narrower diameter implant is employed, a ceramic abutment should be chosen with great caution, because it will be more prone to fracture than an abutment on a wider implant. It is often advisable to restore a narrower implant in a maxillary first bicuspid area with a titanium abutment.
Implant depth is a function of the diameter of the implant as related to the desired diameter of the restoration at the cervical area as it exits the gingiva. There should be a fluid transition from the implant neck through the gingiva, to the supragingival restorative contours, with no significant ridge lap. Therefore, a narrower implant will have to be placed more deeply than its wider counterpart in a given situation.
Following implant placement, regenerative therapy is carried out as needed, as previously discussed.
For implant placement at the time of maxillary premolar extraction, the following principles must be considered. Due to the greater ratio of the bucco-lingual dimension to the mesio-distal dimension of the mandibular premolar when compared to the maxillary premolar, the clinician can often choose between a tissue-level and a bone-level implant. This decision should be wholly restorative driven, as will be discussed below.
The maxillary molar region tends to present with the reverse issue to that described in the mandibular arch. Disease and atrophy of the alveolar process in the maxillary molar region is characterized by bone loss that is apical and medial in direction. The surgeon will also have to consider the sinus cavity and possible pneumatization. In seeking bone to stabilize the implant, there is a tendency to place the implants toward the patient’s palate. In such a situation, implant positioning will be in a bucco-palatal direction. The restorative challenges can be significant.
Placement of an implant in a bucco-palatal direction may result in off-axis loading, depending upon the degree of bone atrophy that is present. Apical palatal movement of the implant often forces the restorative crown(s) into the maxillary “neutral zone,” interfering with the patient’s tongue. A perception of crowding may result. A more palatal placement of the restorative element will also challenge the restorative dentist’s ability to generate an acceptable occlusal scheme. An extreme example would be the need to build the occlusion in cross-bite.
A separate but related issue often overlooked is the protective service provided by a maxillary molar in its correct position in the arch. The buccal overjet of a maxillary molar affords protection to the buccal mucosa and helps the patient avoid “cheek biting.” There is a delicate balance to be reached in the placement of a maxillary molar restoration between excessive overjet and inadequate overjet. The former will be annoying to the patient, and may even cause soreness in the area of the mucosa that comes in contact with the crown. The latter placement will cause repeated laceration and damage to the mucosa, as the mucosa is trapped between the maxillary and mandibular teeth.
When treating the maxillary molar region, the restorative dentist must be aware of the increase in interarch space as bone loss occurs. The restorations will need to be placed on implants that are more apical than where the original teeth were located. The crown(s) will be larger occluso-apically and often will feel bulky to the patient.
Esthetically, the molar region is far less demanding than other areas of the dental arch. The selection of tissue-level or bone-level implants is based less upon perceived esthetic needs than on the implant system being used and the ease of implant restoration. Implant diameter also has a bearing in the restorative decision. Restorative dentists usually are more comfortable placing molar restorations on implants that are closer to 6 mm in diameter. Ease of restorability favors a tissue-level implant approach. Such a platform is simple to restore. The opportunity to use stock abutments in most instances makes this a less costly platform to restore when compared to bone-level implants.
When considering implant restoration in the premolar region, there are fewer anatomical issues for the restorative dentist. Well-positioned implants placed in alignment mesially and distally along the ridge, and bucco-lingually within the ridge, can be restored with little concern for the curve of Wilson. However, implants placed in the premolar region of either arch are likely to have significant esthetic concerns. These greater esthetic demands favor the use of bone-level-style implants. Implants placed at the bone level permit the restorative dentist to develop an esthetic emergence profile by transiting from the bone through the soft tissues into the restorative space. The tissues surrounding the implant-supported restoration can be manipulated to provide the appearance of a natural tooth framed by the gingival tissues. Bone-level implants are technically more difficult to restore than tissue-level implants. However, the benefits and the versatility that accompany this approach outweigh the higher skill level required.
The mandibular premolar area has less esthetic demands than those found in the maxillary premolar area. The lower lip and buccal mucosa usually mask the cervical aspects of the mandibular teeth. The selection of tissue-level or bone-level implants thus becomes a choice driven by the placement environment as well as the operators’ preferences.
Restorative options and versatility favor the bone-level implant. Often, the extra depth and emergence from a lower point in the alveolus permits the use of a wider platform than if a tissue-level implant was placed. Papillary development is not compromised, as the interproximal spacing is controlled by a custom abutment and not the implant head. The use of a wider implant also results in greater strength.
Such a concept segues easily into the concept of “platform switching.”7,8 Rather than using an abutment with the same diameter as the implant platform, a narrower abutment is employed. The narrower diameter abutment has less impact on the junctional epithelium and soft connective tissue, allowing the biologic width to form higher on the implant and resulting in less peri-implant crestal bone than in non-platform-switching situations.
The restorative dentist must be aware of this attribute of platform switching, especially in areas where the buccal plate is thin. When platform switching is employed, the inflammatory zone associated with the microgap of the implant–abutment junction occurs further away from the bone–implant interface, and the damage to the crestal bone surrounding the implant is minimized, thereby helping preserve the esthetics of the area.
Implant placement should be carried out in a manner that simplifies the restorative dentist’s tasks of restoring the implant, and returning the patient to the desired form and function in the restored area. The position of the implant should correspond to the tooth that is being replaced, although frequently this may not be possible, as anatomic considerations and/or restrictions in the arch space force placement that is not uniform within the alveolus.
Lack of inter-arch space may cause a mesial-distal implant angulation, forcing the mesial aspect of the implant platform deeper into the tissues than the distal aspect. The choice of a tissue-level implant in this situation will result in a subgingival mesial margin and may require the use of a custom abutment to bring the cement line to an area where it can be cleaned. A bone-level implant choice may place the marginal aspect of the implant into an area where the bone on the mesial aspect of the implant and on the distal aspect of the adjacent tooth prevents seating of the impression coping and/or the custom abutment. In the maxilla, the additional consideration of the thick, deep palatal tissue found in some patients exacerbates this concern. The buccal aspect of the implant platform may be supragingival, while the palatal area of the implant is deep below the palatal tissues, forcing the use of a custom abutment to raise the cement line to a cleansable area.
In a situation that forces the implant placement to be off of the ideal buccal-lingual center of the alveolus, the restorative dentist will need to resort to prosthetic “gimmicks” to achieve the desired restorative result. An implant placed too close to the buccal plate of bone is more difficult to restore, and the esthetics of the area is challenged by the lack of space prosthetically for porcelain while still having the crown reside in the buccal corridor, without appearing overbulked. Such a position may lead to resorption of the buccal plate of bone over time, creating an unsightly restorative result. From a restorative perspective it is better to err to the lingual or palatal aspect of the ridge, within reason. Such misplacement can be addressed by cantilevering the buccal aspect of the crown to bring the implant-supported crown(s) into alignment with adjacent and opposing teeth. However, this restorative option results in the patient’s increasingly challenging maintenance of the restoration.
Restorative Scenarios
The dentition opposing the implant restoration needs to be considered in the restorative plan. This is of particular importance in the posterior areas, as failure to design a proper occlusal scheme will be detrimental to the longevity of the implant. There are three scenarios that the restorative dentist may face: implant-supported restorations opposing natural teeth; implant-supported restorations opposing a removable prosthesis; and implant-supported restorations opposing implant-supported restorations.
When an implant restoration is opposed by the natural dentition, the forces of occlusion are not less than those generated by tooth-to-tooth function. The proprioception feedback mechanism that exists with natural teeth and a periodontal ligament is diminished by the fact that the implant-supported restorations do not have such neural control. This may compromise the patient’s self-protective system and allow overloading of the implant if the implant and restoration are not properly fitted into the occlusal scheme. This generally means that the natural tooth has a centric contact with the implant-supported crown. The degree of force that this contact exerts needs to be calibrated to the end load point of the periodontal ligament of the natural teeth. The force on the implant crown should coincide with that amount of force that would load the natural tooth and not overload that tooth or adjacent natural teeth. This can be measured by careful articulation and fabrication of the restorative element on a master model that has been accurately mounted on an articulator. Additionally, the patient will be able to give feedback to the restorative dentist during placement, and fine-tuning of the occlusion can be accomplished.
The implant-supported restoration opposed by a removable prosthesis has the least risk of overloading. This restoration will benefit from the cushioning that comes from acrylic teeth and, in non-tooth-supported edentulous areas, the soft-tissue cushioning that comes from the tissue overlaying the ridge.
Implant-supported restorations opposing implant-supported restorations present by far the most complex occlusal scheme to develop. The absence of a periodontal ligament means there is no protective feedback mechanism that will signal to the patient that the forces are excessive. This challenging situation demands accurate mounting of the master models and careful attention to the occlusion during delivery. Overloading of the restorations can get overlooked and go undetected. Generally, there is a material failure such as porcelain fracture that indicates excessive forces on that element of that restoration.
Selecting the Appropriate Treatment Modality
In addition to technical competence, the clinician must be well versed in the indications, contraindications, and expected long-term treatment outcomes of each therapeutic approach. The clinician’s level of perception will have a significant impact on his or her development of treatment algorithms.
For example, if a patient presents with an endodontic perforation of a maxillary first molar which condemns its mesial-buccal root, available treatment options include root resection and subsequent restoration, tooth removal and replacement with a three-unit bridge, or tooth removal and replacement with an implant, abutment, and crown. Following extraction of an upper molar, should the clinician believe that the area must be allowed to heal, a subsequent sinus augmentation procedure must be performed, and an implant be placed at a third surgical session, it is highly unlikely that such a treatment algorithm would be chosen. However, should the clinician understand that the tooth can be extracted, an implant placed at the time of tooth removal, concomitant therapy be performed if necessary, and the tooth restored approximately 5 months later, the idea of implant utilization becomes much more attractive.
Conscientious clinicians perform both therapeutic and cost/benefit analyses prior to developing treatment algorithms. Unfortunately, discussion of a cost/benefit analysis all too often focuses on only the financial ramifications of therapy. A true cost/benefit analysis begins by analyzing the biologic cost of each treatment option. If one option is superior biologically, it should be chosen and actuated.
Only if two or more treatment options offer equal biologic benefits should the next level of cost/benefit analysis, that of esthetic assessment, be carried out. Once again, if one option is esthetically superior, it should be chosen.
The next cost/benefit analysis, assuming the biologic and esthetic analyses yielded no preference, is therapeutic—what treatments the patient must undergo.
Only if these three analyses—biologic, esthetic, and therapeutic—yield equal results is a financial cost/benefit analysis carried out. It is important to factor predictability and future costs into such a financial analysis.
Conclusions
The continued development of new techniques and the evolution of dentistry’s understanding of the potentials and limitations of various therapies afford conscientious clinicians ample information to ascertain when to utilize periodontal, implant, and/or regenerative therapies in the treatment of compromised posterior teeth. It is incumbent upon all clinicians to employ this knowledge to maximize treatment outcomes in the most efficient and reasonable manner. Dental patients deserve no less.
ACKNOWLEDGMENT
The figures in this article originally appeared in “Implant and Regenerative Therapy in Dentistry: A Guide to Decision Making” by Paul A. Fugazzotto (Wiley Blackwell); 2009. Used with permission.
ABOUT THE AUTHORS
Paul A. Fugazzotto, DDS
Visiting lecturer at Tufts University, Boston, Massachusetts; Boston University, Boston, Massachusetts; and the University of Ancona, Ancona, Italy; Fellow, International Team for Implantology (ITI), Basel, Switzerland; Private Practice, Milton, Massachusetts
Frederick O. Hains, DDS
Faculty Member and Course Director, Boston University Goldman School of Dental Medicine, Boston, Massachusetts; Private Practice, Braintree, Massachusetts
REFERENCES
1. Fugazzotto PA. Report of 302 consecutive ridge augmentation procedures: technical considerations and clinical results. Int J Oral Maxillofac Implants. 1998;13(3):358-368.
2. Fugazzotto PA. Maintenance of soft tissue closure following guided bone regeneration: technical considerations and report of 723 cases. J Periodontal. 1999;70(9):1085-1097.
3. Fugazzotto PA. Maintaining primary closure after guided bone regeneration procedures: introduction of a new flap design and preliminary results. J Periodontol. 2006;77(8):1452-1457.
4. Fugazzotto PA. Implant placement at the time of maxillary molar extraction: treatment protocols and report of results. J Periodontol. 2008;79(2):216-223.
5. Fugazzotto PA. A retrospective analysis of implants immediately placed in sites with and without periapical pathology in sixty-four patients. J Periodontol. 2012;83(2):182-186.
6. Fugazzotto PA. A retrospective analysis of immediately placed implants in 418 sites exhibiting periapical pathology: results and clinical considerations. Int J Oral Maxillofac Implants. 2012;27(1):194-202.
7. Canullo L, Fedele GR, Iannello G, Jepsen S. Platform switching and marginal bone-level alterations: The results of a randomized-controlled trial. Clin Oral Implants Res. 2010;21(1):115-121.
8. Vela-Nebot X, Rodríguez-Ciurana X, Rodado-Alonso C, Segalà-Torres M. Benefits of an implant platform modification technique to reduce crestal bone resorption. Implant Dent. 2006;15(3):313-320.