The Digitalizing of Implant Dentistry: A Clinical Evaluation of 15 Patients
Abstract
This article introduces intraoral scanning technology as it applies to custom-fabricated implant abutments. The author discusses its use and clinical applications, and provides an overview of the benefits of such a system in the clinical setting. In this clinical evaluation of 15 patients, the BellaTek™ Encode® Impression System was combined with iTero™ intraoral scanning technology to demonstrate the technical feasibility of combining these two CAD/CAM technologies. The BellaTek™ Encode® impression system protocol was established to allow the clinician to digitally impress special codes embedded on the occlusal surface of the BellaTek™ Encode® healing abutment. Once a digital file was prepared for CAD/CAM processing, a duplicate STL file could be sent to iTero for fabrication of a polyurethane model of the definitive BellaTek™ abutment, from which an implant restoration could be created. This definitive prosthesis was able to be fabricated simultaneously while the definitive BellaTek™ abutment was being milled.
The digital era for implant and tooth-supported prosthetics based on computer-aided design and computer-aided manufacturing (CAD/CAM) has progressed in the past two decades, mainly due to market-driven development of various generations of visible light impressions.1 Integration and application of this technology within the realm of implant dentistry has been limited, as a greater emphasis has been placed on conventional crown and bridge applications. In 1994 Jemt and Lie2,3 described a technique called photogrammetry, which uses a series of 3-dimensional (3-D) photographs to record implant positions for manufacturing implant frameworks. They determined that photogrammetry was a valid option for recording implant positions and had a precision comparable to that of conventional impression techniques.4 Del Corso5 demonstrated that optical 3-D scanning acquisition could be used to determine the position of osseointegrated implants and that image-acquiring technology could be used as an alternative to traditional impression techniques. The entire manufacturing process begins with the correct impression procedure and depends on the accuracy of the master cast.
Digital impression systems have offered the possibility of better-fitting restorations and greater productivity for the general dentist.6 These systems offer users the ability to capture a digital image of the preparation and submit that information electronically, resulting in fabrication of a working model and die system for fabrication of the restoration. A comparison of crowns made with a digital scan versus those created with a traditional impression found that the scanned restorations showed a greater number of perfect interproximal contacts, better marginal fit, and more accurate occlusion.7,8
The iTero™ digital impression device (Align Technology, Inc., www.aligntech.com) has been developed as an office-based intraoral scanning system, which is connected by the Internet to a centralized milling center and to the partnering dental laboratory. The system’s enhanced visualization and real-time analytical tools enable clinicians to adjust measurements before completing the intraoral digital scanning of patients.9-11 Digital scanning technology has significantly enhanced clinical accuracy and productivity in comparison to conventional impression techniques. Standard impressions can be prone to the following shortcomings: pulls and tears; bubbles and voids; distortion; tray-to-tooth contact; poor tray bond; de-lamination; sensitivity to temperature, technique, time, and chemistry; varying shrinkage; stone model pouring; and die trimming discrepancies. Digital scanning technology eliminates these issues,12 consistently displaying highly accurate digital impressions.
The iTero intraoral scanning device used in this case series consisted of a mobile cart (central processing unit [CPU] device) on castors equipped with a wireless mouse and keyboard, hands-free navigation using a wireless foot control/pedal, and a handheld scanning wand (electronic impression device [EID]) that is used to obtain the scan data. The scanner head houses the analog-digital converter, video camera, focusing mirrors/motor, and light source, which projects 100,000 beams of parallel red laser at focal depth intervals of 50 µm. The reflected light is converted into digital data through the use of analog-to-digital converters; therefore, the entire event takes approximately one-third of a second. The iTero digital impression device does not require opaque powder to provide uniform light distribution, and the surface registration and accuracy are within 15 µm.13
Clinical Evaluation
The case series included 13 patients with single implant sites and two patients with multiple implant sites (two) in both the maxillary and mandibular arches. All patients were healthy and nonsmokers. Cone-beam computerized tomography (CBCT) scans were obtained preoperatively. Prior to surgery, all patients received a loading dose of amoxicillin, 4 mg Medrol Dosepak (methyl prednisone), and 0.12% chlorhexidine mouthrinse. Local anesthesia was delivered using local infiltration and nerve blocks with 2% articaine/lidocaine (1:100,000 epinephrine). Where possible, a flapless surgical procedure was used with a biopsy punch (Ace Surgical Supply, www.acesurgical.com). If guided bone regeneration was anticipated, a full-thickness mucoperiosteal flap was raised for direct visibility and true analysis of hard tissue.
Following ridge exposure, implant osteotomies were prepared according to the manufacturer’s drilling specifications. Seventeen NanoTite™ Certain® implants (Biomet 3i, www.biomet3i.com) were placed in 15 patients using cone-beam analysis and a surgical guide fabricated on study casts from an ideal wax-up or computerized software (Anatomage®, Anatomage, www.anatomage.com). The implant diameters and lengths ranged from 3.25 mm to 5 mm D x 10 mm to 13 mm L. All implant insertion torque values were set at 50 Ncm to achieve adequate primary stability. Primary stability was achieved with all implants and verified with the Osstell™ resonance frequency analysis (RFA) device (Osstell™ Device, Integration Diagnostic AB, www.osstell.com).14,15 Following RFA stability verification, the implants had BellaTek™ Encode® healing abutments (Biomet 3i) placed for single-stage healing. The full-thickness mucoperiosteal flaps were closed using 4-0 and 5-0 Vicryl (Ethicon, www.ethicon.com) interrupted sutures.
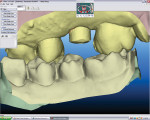
Patients were placed on a 1-week antibiotic regimen (amoxicillin), chlorhexidine 2 times daily, a low-dose steroid, and analgesics as needed. Strict oral hygiene instructions were given in writing and orally, and specific dietary protocols were given. After 14 days, the sutures were removed and each patient’s oral hygiene instructions were modified and the patients reinstructed. The implants were allowed to heal for approximately 3 to 5 months prior to definitive restoration. A digital scan of the BellaTek Encode healing abutment using the iTero intraoral scanner (Figure 1) was taken to include the opposing arch and 90-degree occlusal registration. All scanning data was sent to iTero to be processed and converted to standard triangulation language (STL) files in preparation for definitive abutment fabrication. The data was forwarded to the BellaTek™ Production Center at Biomet 3i, where the virtual BellaTek abutment was designed in preparation for the CAD/CAM milling process. For further modification and approval, a jpeg file can be sent to the restorative dentist to approve the design (eg, margin location) prior to final manufacturing.
The new STL file with the patient-specific abutment (BellaTek™ Abutment, Biomet 3i) in place and the healing abutment removed was sent back to iTero for fabrication of a polyurethane master cast (working model) for completion of the definitive restoration. The crown was then fabricated on the iTero model and delivered to the restoring clinician with model, abutment, and abutment-specific screw in preparation for the final seating. Once seating verification was complete, the BellaTek final abutment was torqued down with a gold screw (Gold-Tite® abutment screw, Biomet 3i) to 20 Ncm with the indicated torque driver. The crowns were then seated using a cement-retained protocol individualized to each clinician. A post-seating radiograph was taken to assess marginal fit and to check for retained cement.
Case
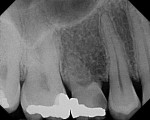
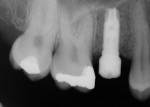
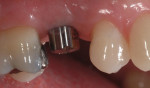
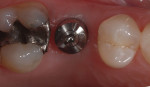
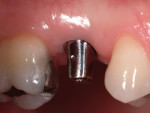
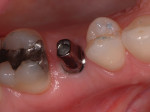
In a sample case among the patients treated in this evaluation that depicts a typical application of the technology, a 28-year-old woman presented with recurrent caries associated with the mesial aspect of tooth No. A in the No. 4 position (Figure 2). The restorative dentist determined this tooth should not be retained and recommended extraction. The tooth was extracted approximately 6 months prior to implant placement. A 4.1/3.25-mm x 13-mm implant (NanoTite Certain, Biomet 3i) was placed in the No. 4 area with the aid of a surgical guide (Figure 3). The implant insertion torque value was set at 50 Ncm to achieve adequate primary stability. Primary stability was achieved and verified with the Osstell™ RFA device prior to the final restorative phase. The BellaTek Encode healing abutment was checked for mobility, and torque was verified at 20 Ncm (Figure 4 and Figure 5). A radiograph was taken for seating verification prior to the digital scan. A digital scan of the healing abutment using the iTero intraoral scanner was taken to include the opposing arch and 90-degree occlusal registration (Figure 6).
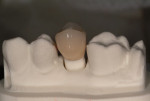
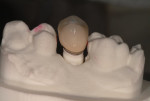
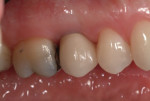
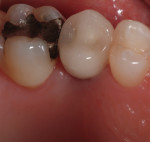
The crown was then fabricated on the iTero model and delivered to the restoring clinician with the model, abutment, and abutment-specific screw in preparation for the final seating (Figure 7 and Figure 8). Once seating verification was complete, the BellaTek abutment was torqued down with the gold screw (Gold-Tite) in place to 20 Ncm with the indicated torque driver (Figure 9 and Figure 10). The crowns were then seated using a cement-retained protocol (Figure 11 and Figure 12).
Conclusions
Digital scanning technology is changing the face of implant dentistry. Compared to elastomeric impression materials digital scanning results in less expense, increased productivity, and more efficient clinical systems. Digital scanning technology has significantly enhanced clinical accuracy and productivity in comparison to conventional impression techniques. A variety of impression materials can be prone to inherent challenges that decrease their overall accuracy. Scanning technology such as that used in this evaluation eliminates these issues and consistently produces highly accurate digital impressions.
Today in dentistry, specific implant abutments can be scanned and the information digitally transferred directly to a five-axis milling center. This technology saves additional time and money for all parties. The introduction of digital impression systems provides clinicians the opportunity for better-fitting restorations and greater general dentistry productivity. These digital systems are now being utilized together to serve clinicians and patients more effectively. The design technician is also given more information, improving the design of the CAD/CAM abutments with the aid of computerized virtual programs.
Undoubtedly, digital impression devices are going to be a significant part of the future of implant dentistry. The industry will see continued development within the digital markets, which will increase market competition, and with more clinicians implementing the technology into their practices, the technology will likely become more affordable.
DISCLOSURE
This project was partially supported by Biomet 3i.
Acknowledgments
The author would like to thank Mrs. Amy Derhalli and Dr. Richard Mounce for their critical review, and Dr. Steven Hopmann for the restoration shown in Figure 11 and Figure 12. In addition, he would like to thank O’Brien Dental Lab, Inc., Corvallis, Oregon.
References
1. Farman AG, Scarfe W, van Genuchten M. Multidimensional imaging: immediate and imminent issues. Compend Contin Educ Dent. 2010;31(8):648-651.
2. Lie A, Jemt T. Photogrammetric measurements of implant positions. Description of a technique to determine the fit between implants and superstructures. Clin Oral Implants Res. 1994;5(1):30-36.
3. Jemt T, Bäck T, Petersson A. Photogrammetry—an alternative to conventional impressions in implant dentistry? A clinical pilot study. Int J Prosthodont. 1999;12(4):363-368.
4. Jemt T, Lie A. Accuracy of implant-supported prostheses in the edentulous jaw: analysis of precision of fit between cast gold-alloy frameworks and master casts by means of a three-dimensional photogrammetric technique. Clin Oral Implants Res. 1995;6(3):172-180.
5. Del Corso M, Giancarlo A, Vazquez L, et al. Optical three-dimensional scanning acquisition of the position of osseointegrated implants: an in vitro study to determine method accuracy and operational feasibility. Clin Implant Dent Relat Res. 2009;11(3):214-221.
6. Christensen GJ. Impressions are changing: deciding on conventional, digital or digital plus in-office milling. J Am Dent Assoc. 2009;140(10):1301-1304.
7. Farah JW, Brown L. Comparison of the fit of crowns based on digital impressions with 3M ESPE Lava Chairside Oral Scanner C.O.S. vs. traditional impressions. The Dental Advisor Research Report. 2009;(22):1-3.
8. Henkel G. A comparison of fixed prostheses generated from conventional vs digitally scanned dental impressions. Compend Contin Educ Dent. 2007;28(8):422-424, 430-431.
9. Garg AK. Cadent iTero’s digital system for dental impressions: The end of trays and putty? Dent Implantol Update. 2008;19(1):1-4.
10. Jones PE. From intraoral scan to final custom implant restoration. Inclusive. 2011;2(4):6-13.
11. Jones PE. Cadent iTero digital impression case study: full-arch fixed provisional bridge. Dentalcompare Web site. July 8, 2009. https://www.dentalcompare.com/Featured-Articles/2082-Cadent-iTero-Digital-Impression-Case-Study-Full-Arch-Fixed-Provisional-Bridge/. Accessed January 29, 2013.
12. Jones PE. Cadent iTero optical scanning digital impressions for restorative and Invisalign. Dental Product Shopper Web site. June 28, 2011. https://www.dentalproductshopper.com/articles/cadent-itero-optical-scanning-digital-impressions-restorative-and-invisalign. Accessed January 29, 2013.
13. Strietzel R, Lahl C. CAD/CAM Systems—Parts 1-4. Procedure: Principles and history. Spectrum Dialogue. 2010;9(4-7).
14. Degidi M, Daprile G, Piatelli A. RFA values of implants placed in sinus grafted and non-grafted sites after 6 and 12 months. Clin Implant Dent Relat Res. 2009;11(3):178-182.
15. Friberg B, Sennerby L, Meridith N, Lekholm U. A comparison between placement torque and resonance frequency measurements of maxillary implants. A 20 month clinical study. Int J Oral Maxillofac Surg. 1999;28(4):297-303.
About the Author
Munib Derhalli, DMD, MS, MBA
Private Practice
Vancouver, Washington