Trap Door: An Alternative Procedure to the Triangular Distal Wedge for the Elimination of Distal Periodontal Pockets Adjacent to Edentulous Areas
Medha Singh, BDS, DMD, MS; Paul C. Stark, MS, ScD; Petros D. Damoulis, DMD, DMSc; Paul Levi, DMD; and Terrence J. Griffin, DMD
Abstract
The study compared a novel trap door (TD) technique with the triangular distal wedge (TW) procedure for the elimination of distal periodontal pockets adjacent to edentulous areas. Thirteen patients with suprabony pockets ≥ 5 mm at the distal surface of terminal molars bilaterally were included in this prospective, single-blinded, randomized clinical trial using a split-mouth design. The authors demonstrated the efficacy of an alternative TD technique in the elimination of the distal pockets adjacent to the terminal molars.
Deep periodontal pockets associated with the distal surfaces of terminal molars in the maxilla and mandible is common; Robinson1 initially described their characteristics in 1963. According to that report, the gingival crest on the distal aspect of terminal molars is frequently 4-mm or more occlusal to the cementoenamel junction. The inaccessibility of the area makes proper cleansing by the patient difficult or impossible and can lead to the development of a pathologically deepened periodontal pocket.1
In both the maxilla and mandible, the presence of thick bone or incomplete fill of bone following the extraction of a third molar contributes to the deep pockets.2 In the past, the management of these distal pockets has been performed by various gingivectomy techniques.3,4 However, the gingivectomy procedure often fails to adequately eliminate pockets if infrabony deformities are present.
Robinson reported the “distal wedge operation” to manage these pockets and described the three distal wedge incisions: triangular, square, and linear. The triangular incision is the most commonly used.1 In addition to providing access to the underlying osseous tissue, the distal wedge procedure permits rapid healing by primary intention, thus overcoming the discomfort of secondary intention healing when a gingivectomy is performed.1 Positioning of the flap tissue at a more apical level leads to exposure of more tooth structure, which makes the site more cleansable by eliminating deep pockets.5
The authors propose an alternative to the triangular distal wedge (TW) for the elimination of pockets present on the distal surface of terminal teeth in the arch, which follows a “trap door” (TD) design. This study compares the primary outcomes of the TD technique with the TW procedure to show changes in probing depth for a 3-month period, and the secondary outcomes to demonstrate changes in clinical attachment level, healing rate, and postoperative pain.
Materials and Methods
This was a prospective, single-blinded, randomized clinical trial using a split-mouth design. The observation period was 3 months. The Tufts New England Medical Center Institutional Review Board approved the protocol and informed consent of the study. A single investigator (TJG) performed the surgeries while another investigator (MS) did the measurements. The TD procedure was performed on the test site; the TW technique was performed at the control site. The test site within a patient was assigned on a random series of numbers generated in a statistical software program (version 12.0, SPSS, www.spss.com).
Participants were included in the study if they presented with bilateral first or second molars that were the terminal teeth in the arch and if they had clinical probing depth ≥ 5 mm only on the distal surface. In addition, the terminal teeth needed to be vital, have no mobility, have no restorations on the distal surface, and have no surgical treatment for at least 2 years previously. Patients excluded from the study were smokers, had local or systemic diseases that contraindicated periodontal surgery, or had sites requiring osseous surgery or bone regeneration. Eligibility was assessed at a screening visit, and a signed informed consent was obtained. Inclusion and exclusion criteria were evaluated through a review of the medical history, as well as radiographic and periodontal examinations. The enrolled participants received oral hygiene instructions and a complete mouth debridement. For each patient, alginate impressions were taken of the maxilla or mandible, including the experimental teeth, and stone models were made. A rigid stent (Press Form™ Sheets, Ellman International, www.ellman.com) was made from the stone model, which had guiding grooves on each experimental tooth angled toward the deepest part of the pocket for accurate clinical pocket measurements.
A periodontal examination was performed using a periodontal probe (UNC-15, Dentsply International, www.dentsply.com) and a customized rigid stent (Press Form Sheets). Measurements were taken from a fixed reference point on the stent and included clinical probing depth and cementoenamel junction position. The deepest probing depth on the distal surface was recorded. Measurements were taken at baseline on the day of surgery, which was 2 weeks after the initial therapy, and again 3 months following surgery. Clinical photographs (35 mm Ektachrome Color Slide Film, Kodak, www.kodak.com) of the surgical site were also taken preoperatively, and at 1 week, 2 weeks, 1 month, and 3 months postoperatively to evaluate healing time.
Surgical Procedure for TW
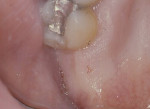
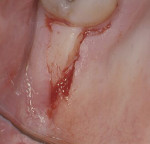
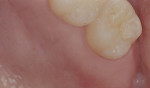
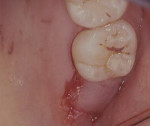
After adequate anesthesia was given, bone sounding was done to determine the soft-tissue thickness on the edentulous ridge (Figure 1). A submarginal incision was performed 1.5-mm apical to the free gingival margin from the mesiopalatal to distopalatal surface of the terminal tooth to allow for apically positioning the flap. An intrasulcular incision was performed on the buccal surface of the terminal tooth from the mesiobuccal to the distobuccal line angle. The incision design continued on the distal surface extending posteriorally in the shape of a triangle coronal to the mucogingival junction to form the TW (Figure 2). The TW length was 10 mm. The TW width was equal to the buccolingual dimension of the distal surface of the terminal tooth.
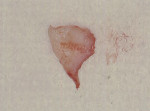
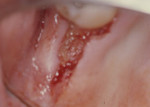
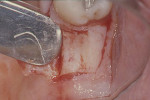
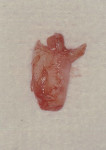
The pocket depth helped determine the amount of tissue excised, with an average of 2-mm thickness of connective tissue removed to thin the flaps. A full-thickness flap was reflected buccally and lingually. Elevation of the buccal flap past the mucogingival junction was performed via sharp dissection in order to allow for the apically positioning of the flap to the crestal bone. The entire distal wedge of tissue was removed, all granulation tissue was curetted, and the roots were carefully scaled and planed (Figure 3 and Figure 4). No osseous surgery was performed.
Surgical Procedure for TD
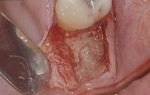
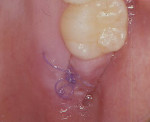
After adequate anesthesia was given, bone sounding was done to determine the soft-tissue thickness on the edentulous ridge (Figure 5). A submarginal incision was performed 1.5-mm apical to the free gingival margin from the mesiopalatal to the distopalatal surface of the terminal tooth to allow for apically positioning the flap. An intrasulcular incision was performed on the buccal surface of the terminal tooth from the mesiobuccal to the distobuccal line angle (Figure 6). A horizontal incision was made, starting from the distobuccal line angle of the terminal tooth directed perpendicularly to the crest of the alveolar ridge and its underlying bony surface and extending posteriorly. The length of the horizontal incision was 10 mm. To facilitate the removal of the distal tissue, a vertical releasing incision was made at the distal termination of the horizontal incision in a buccal direction.
A second mesiodistal split-thickness incision was then placed from the line of the horizontal incision approximately 1 mm beneath the surface of the crestal soft tissue in the edentulous area and directed parallel to the alveolar crest. This incision was made to undermine the flap so that the flap itself was about 1 mm in thickness, while the underlying connective tissue remained attached to the bone. This formed the TD (Figure 7). The connective tissue underneath the TD was then removed to the bony crest (Figure 8 and Figure 9). The TD width was equal to the buccolingual dimension of the distal surface of the terminal tooth. The pocket depth determined the amount of tissue excised, and an average of 2 mm of tissue was removed. The granulation tissue was curetted, and the roots were carefully scaled and planed.
Suturing and Follow-Up Care
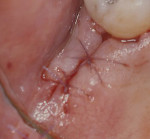
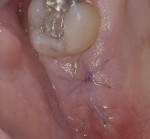
For both TD and TW surgical sites, the distal surface of the terminal tooth was stabilized by “X” sutures using a 5-0 bioabsorbable polygylactic suture material (Vicryl, Ethicon, www.ethicon.com) with a P-3 needle, and the mesial interdental area of the terminal tooth was stabilized by vertical mattress sutures (Figure 10 and Figure 11). Primary wound closure was attempted in all cases. A noneugenol periodontal dressing (Coe-Pak®, GC America Inc.,www.gcamerica.com) was placed over both the test and control surgical sites. There are several reasons for using a periodontal dressing. It protects the surgical site from trauma from masticating food; although a soft diet is recommended, patients are not always compliant. The dressing also covers the sutures, which prevents the patient from feeling them with their tongue. Additionally, the periodontal dressing can provide stability to the wound site and help prevent postsurgical bleeding. Such bleeding could produce a blood clot between the osseous crest and overlying flap; a blood clot could subsequently organize into connective tissue and create thick mucosal tissue, which had just been intentionally thinned.
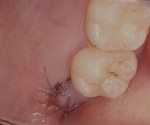
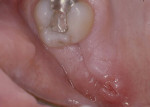
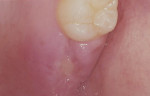
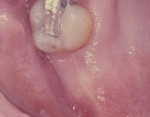
Patients were instructed to use 0.12% chlorhexidine gluconate mouthrinse for 2 weeks. Both the dressing and sutures were removed 1 week after surgery. Patients were seen at 1-week (Figure 12 and Figure 13), 2-week (Figure 14 and Figure 15), 1-month, and 3-month (Figure 16 and Figure 17) appointments for postoperative follow-up. Detailed oral hygiene instructions for plaque control were given at every visit.
The healing was assessed by three periodontists who did not participate in the study. They judged the clinical slides taken at the 1-week, 2-week, 1-month, and 3-month postsurgical visits. These examiners were shown two clinical slides: one from a TD-treated site and the other from a TW-treated site. They were asked to rate the surgical sites for color and contour on a scale of 1 to 3 (1 = good, 2 = acceptable, and 3 = poor). Each examiner was shown the clinical slides twice, at two different times.
Finally, the patients were asked to rate their postsurgical pain level (other than root sensitivity) for each surgical site at their first and second week postoperative appointments using a 10-point visual analog scale (0 to 10), with 0 indicating negligible pain and 10 indicating unbearable pain.
Statistical Methods
Using a split-mouth design, a sample size of 20 pairs (maxilla and mandible) would have excellent power (> 99%) to detect a difference of 2 mm between the pocket depth improvements of the two treatments, assuming a common standard deviation of 1 mm and alpha = 0.05 (nQuery® Advisor 7.0, Statistical Solutions, www.statistical-solutions-software.com). One individual dropped out of the study, resulting in 19 pairs, which still maintained > 99% power. As a result, the data were analyzed using a repeated-measures model. An unrestricted correlation was assumed to account for the correlation between measurements made on the same patients. Because pain scores on the visual analogue scale are ordinal, the median and interquartile range (IQR) was reported. All analyses were performed using the statistical software program SAS (version 9.2, SAS Institute, www.sas.com).
The authors note that while the study was designed to be a comparative study and not an equivalence study, the extremely high power achieved along with the fact that the difference in change between the two groups was almost identical gives the authors confidence that the lack of a significant treatment difference was due to equality in the two treatments rather than insufficient power.
Results
A total of 14 patients were recruited for this study, although one patient withdrew for personal reasons; 13 participants completed the study. The statistical analysis was based on 13 patients; this did not significantly reduce the power of the study.
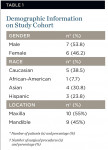
Six participants had four surgeries performed, and the other seven had two surgeries performed for a total of 38 surgeries (19 TD and 19 TW). Ten pairs of surgical procedures were performed in the maxilla (55%) and nine pairs in the mandible (45%). Patients were ages 25 to 65 years. The mean (standard deviation) age was 36.5 (9.2) years (Table 1).
A highly statistically significant reduction was observed in clinical probing depths from baseline to 3 months in both groups (Table 2). In the TD group, the mean probing depths decreased from 5.32 mm (0.48) at baseline to 1.63 mm (0.50) at 3 months (P < .0001). Similar results were found in the TW group, with the respective values being 5.42 mm (0.51) and 1.89 mm (0.32). This difference was also highly statistically significant (P < .0001). However, the difference between the two techniques was not statistically significant (P = .5920).
Changes in clinical attachment levels displayed a similar pattern (Table 2). There was a statistically significant gain in clinical attachment in both groups. Again, the difference between the two techniques was not statistically significant (P = .1071).
Postoperative pain significantly decreased between the first and second week in both groups (Table 3). Although the trend in initial postoperative pain as well as in the rate of improvement clearly favored the TD procedure, the difference between the two groups was not as statistically significant as at week 1 (P = .173) or week 2 (P = .138).
The median (IQR) healing score at week 1 for the TD group was 2.00 (1.67, 2.17); for the TW group it was 2.00 (1.33, 2.33) (Table 4). Comparing these two groups resulted in a P value of .393, suggesting no statistically significant difference between the groups. At 3 months, the median (IQR) healing score for the TD group was 1.17 (1.00, 1.33), and for the TW group it was 1.33 (1.17, 1.50), yielding a P value for the comparison of 0.158.
One of the three periodontists who evaluated healing rate had poor intra-examiner reliability (0.178) and reduced the inter-examiner reliability from 0.873 to 0.462 for the healing data. The other two examiners had good inter- and intra-rater reliability, ranging from 0.54 to 0.813. When examiner number 2 data were removed, the significance of the results did not change.
Discussion
According to Robinson,1 the gingival crest on the distal aspect of terminal molars is frequently 4-mm or more occlusal to the cementoenamel junction. The inaccessibility of the area makes proper cleansing by the patient difficult or impossible and can lead to the development of a pathologically deepened periodontal pocket. The TW or TD procedure allows for elimination of deep periodontal pockets by exposing the underlying osseous tissue and positioning the periodontal flap at a more apical level. This leads to exposure of more tooth structure, which makes the site more cleansable.
Although the TW procedure is routinely performed, it has not been studied extensively in the literature. The existing literature on distal wedge procedures was documented during the 1960s and 1970s, and these studies were mainly personal views or case reports/case series.6-8 Prospective studies related to the outcomes of the distal wedge have not been published. This study was designed as a clinical trial to compare the outcomes of the TW and TD procedures.
The results of the present study demonstrated that both procedures were effective in the reduction of periodontal pockets present on the distal aspect of terminal molars, and statistically significant differences were detected in terms of probing depth reduction, clinical attachment level gain, postoperative pain, and healing rate (Table 2, Table 3, Table 4). This study was the appropriate size to have adequate power to detect a 2-mm difference. However, both interventions showed such marked improvement that a treatment effect was not detected.
Although both procedures eliminated pockets equally, the TD is clinically a better alternative to the TW because the incision designs of the TD procedure offer advantages over the TW. Firstly, the TD does not reduce the amount of masticatory mucosa from the distal of the terminal molars since it uses a single-line incision, which also allows for primary closure. Since there is more inflammation when there is a paucity of attached gingiva—likely because nonkeratinized alveolar mucosal tissue is more sensitive than gingiva during sulcular brushing—patients will tend to avoid this discomfort and thus leave plaque on the tooth. In addition, the horizontal incision in the TD is made from the distobuccal line angle of the terminal tooth and not in the midpoint buccolingually of the alveolar crest. Thus, this incision design of the TD technique is better suited for guided tissue regeneration therapy than the TW technique, as it allows for primary closure buccal to the infrabony defect, lessening the possibility of membrane exposure. Finally, the TD procedure uses an internal beveled incision to thin the flaps, and the underlying connective tissue could be employed as a connective tissue graft to treat a mucogingival deformity on a separate tooth. Complete healing by secondary intention usually requires 30 to 35 days.9 The TD procedure allows for excellent flap approximation; however, secondary intention healing was noted in some cases where mucosal tissue or excessive edema was present. The trap door can swing from the buccal to the lingual if the anatomy suggests that there might be a chance to damage the lingual nerve, thus avoiding a horizontal on the lingual.
A frequent observation after pocket elimination of the retromolar area is pocket recurrence.4 The TD procedure allowed for better exposure of the tooth surface and provided more access for debridement, which could affect long-term stability and prevent recurrence, especially in patients with less-than-optimal oral hygiene. A follow-up study with a larger sample size and longer follow-up period would be desirable to address these issues.
One limitation of the study was a short follow-up period. The length of the study was limited to 3 months, as this is the period of complete soft-tissue healing.9 The study was not designed to assess the long-term stability of the results. Furthermore, because the patients were seen at frequent intervals for evaluation and the importance of oral hygiene was reinforced at every visit, small differences in treatment outcomes between the two groups in this 3-month period may have been masked. In a procedure such as this, if initial pocket reduction is achieved and the patient follows comprehensive plaque control along with professional maintenance therapy, there should be no significant repocketing long-term.
Conclusions
The present study yielded some interesting preliminary findings. The authors demonstrated the efficacy of an alternative TD technique in the elimination of the distal pockets adjacent to terminal molars. The TD technique may provide increased attached gingiva distal to the terminal molar. It avoids a mid-crestal incision, which, if there has been a recent extraction, avoids suturing over a “dead space.” The technique provides complete visualization of the distal of the terminal molar and enables ideal osseous contouring without flap interference. If the soft tissue of the overlying edentulous space is thick and a connective tissue graft is needed, this method provides a means of harvesting a connective tissue graft, thus achieving two procedures with one surgery, and thereby minimizing trauma for the patient. Lastly, this TD technique is technically significantly easier to accomplish than attempting to resect the island of soft tissue distal to the terminal molar and subsequently thinning out any remaining soft tissue.
References
1. Robinson RE. The distal wedge operation. Periodontics. 1966;4(5):256-264.
2. Prichard JF. Advanced Periodontal Disease: Surgical and Prosthetic Management. Philadelphia, PA: W.B. Saunders Co.; 1965:217.
3. Glickman I. Clinical Periodontology. 3rd ed. Philadelphia, PA: W.B. Saunders Co.; 1964:556-557,683.
4. Goldman H, Schluger S, Fox L, et al. Periodontal Therapy. 3rd ed. St. Louis, MO: Mosby Publishing Inc.; 1964:440-448,602.
5. Friedman N. Mucogingival surgery: the apically repositioned flap. J Periodontol. 1962;33:328-340.
6. Kramer GM, Schwartz MS. A technique to obtain primary intention healing in pocket elimination adjacent to an edentulous area. Periodontics. 1964;2:252-257.
7. Pollack RP. Modified distal wedge procedure. J Periodontol. 1980;51(9):513-515.
8. Braden BE. Deep distal pockets adjacent to terminal teeth. Dent Clin North Am. 1969;13(1):161-168.
9. Moss RW. Histopathologic reaction of bone to surgical cutting. Oral Surg Oral Med Oral Pathol. 1964;17:405-414.
About the Authors
Medha Singh, BDS, DMD, MS
Faculty
Department of Oral Medicine
Infection and Immunity
Harvard School of Dental Medicine
Harvard University
Boston, Massachusetts
Paul C. Stark, MS, ScD
Associate Professor
Department of Research Administration
Tufts University School of Dental Medicine
Boston, Massachusetts
Petros D. Damoulis, DMD, DMSc
Private Practice
Athens, Greece
Paul Levi, DMD
Associate Clinical Professor
Department of Periodontology
Tufts University School of Dental Medicine
Boston, Massachusetts
Terrence J. Griffin, DMD
Associate Professor and Chair,
Department of Periodontology
Tufts University School of Dental Medicine
Boston, Massachusetts