Custom Shade Matching: Fine-Tuning and Patient Communication Lead to Success
Luke Kahng, CDT
Abstract
Shade matching is a sometimes difficult process that involves a variety of colors and characteristics. Couple this with a patient base that often encompasses a wide range of ages, and final restorations can frequently require adjustment or repair because they have failed to match the patient's natural teeth. In this article the author relates many of his own custom shade-taking experiences in an effort to help dental technicians improve their color-matching strategies and avoid costly mistakes.
All dental technicians have their own concepts about color matching. Through experience, the author has learned valuable lessons about a variety of dentin and translucency colors.1,2 This article, in which the author relates many of those experiences, is aimed at helping dental professionals avoid color-matching mistakes3,4 and achieve the best results possible.
Technicians have many characteristics to consider when matching a patient's tooth color. However, they often lack the tools to effectively communicate their observations to the patient. After experiencing many frustrating results with the color-matching tools that were available, the author invented his own Chairside Shade Selection Guide™ (LSK121 Oral Prosthetics, www.lsk121.com). This guide has enabled improved communication between the author, his patients, and the clinicians with whom he is associated.
Step-By-Step Process
There are certain step-by-step keys to look for in the shade-matching process. First, the enamel overlay and translucency color should be examined all the way to the gingival area, noting especially how thick the effect is inside the dentin color. The value and chroma must also be noted—how high, low, or different are they? With a traditional shade guide, the technician is not able to accurately account for this information, which means it will need to be recorded separately.
Hydration versus dehydration stages must then be noted. The author’s method of shade-taking dictates that the technician has a strategy in place beforehand for dealing with these stages. Oftentimes, a patient will become dehydrated before the technician is able to accurately note color, translucency, and mamelon.5
The color of the adjacent teeth should be carefully noted, with the patient and the clinician indicating which adjacent teeth to mimic. This is especially true if there is a crown involved or the color of the teeth varies from one to the next. The patient will usually have a preference about which color he or she is interested in matching—and in not matching.
Custom shading is a science, and achieving the delicate balance of enamel overlay, translucency or transparency, and surface texture in the incisal, gingival, or body one third, as well as in the mesial and distal areas, requires a skill and artistry level that even experienced technicians may have a hard time mastering. The technician has only about 2 to 5 minutes to match a patient’s color. Once a patient’s mouth has been opening and closing beyond that period of time, a difference in the color and translucency of the teeth becomes evident due to dehydration.6,7 It is absolutely essential to keep this in mind when making note of the patient’s custom color.
Because of this potential change due to dehydration, technicians must check the patient’s saliva level at all times by opening his or her lips and frequently examining for hydration. Translucency and transparency enamel modifications depend on the colors that are applied. Whether these colors are white, clear, blue, reddish-orange, or pinkish-gray, without saliva the technician will not know which colors to apply or where to apply them.
Keys to Consider
In considering these modifications, the technician should note the following factors:
Tooth area of a particular color. Is the color in the incisal, body, or gingival one third, or distal or mesial area? It is important to note that overlay will be applied with either clear or white enamel effectively toward the body and gingival levels, underneath or over the top, to create different colors. It is also important to consider how thick, dark, and strong the translucency and transparency application should be, bearing in mind that a thicker application will create a grayish hue to the final color.
Mamelon and halo. The next step should be to consider mamelon and halo, which can only be seen with hydration.8
Orange and yellow ochre. If the patient has a lot of translucency, crack lines that are orange and yellow ochre in color will also appear.
Color of the incisal one third. Bright dentin will be covered with clear or enamel color. The differences will be delineated with staining in the gingival, mesial, or distal area, either with orange, ochre, brown-pink, or grey.
After verifying all of these modifications, the next step is to check the patient’s mouth after it is opened for about 20 seconds. Watch the saliva disappear and see subtle white spots develop. Translucency creates a dark crack line effect; but if high-density enamel is observed, white crack lines will be visible instead.9,10
Modifications
Surface texture is crucial. Surface texture lines relate to lobe and tooth contour and will have an effect on the final shade the technician chooses. If surface texture does not match with adjacent teeth, the restoration will not match because the angles and reflection will totally change the color.11,12
The Chairside Shade Selection Guide has six anterior surface textures from which to choose: Dull, Rough, Shiny, Horizontal Wave, Vertical, or Natural. Based on years of research by the author, these are natural-looking textures and can be recreated if the proper porcelain techniques are used.13
With regard to enamel modification, the guide offers five anterior enamel colors from which to choose: Mamelon Clear, Incisal 1/3, Clear Incisal Enamel, White Clear, and five posterior shades of blue ranging from Light to Grey White.
Finally, enamel overlay will be applied in varying degrees of white, clear, or translucent shades with categorical colors, including grey, tan, blue, pink, and clear, all available in light, medium, or dark tones. Enamel overlay will be applied to either the entire crown, the middle (body) area, or the incisal edge of the tooth; but, however it is applied it will change the color of the final restoration.
The cervical color translucency chroma application creates a natural appearance in the restoration, one that is not opacious. Natural teeth do not have high chroma, but they do have mostly translucent chroma. Matching this is a delicate matter. Enamel overlay with translucency and all the other possible combinations contribute to the many basic differences discussed above.14,15
Shade-Matching Strategies
In order to be productive and save time, dental technicians need a plan for custom shading. In Figure 1 through Figure 32 shade-matching process strategies, as suggested by the author, are depicted.
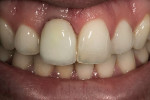
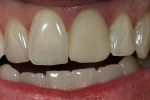
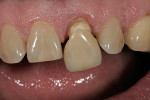
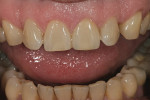
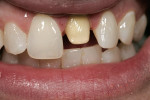
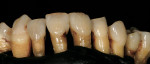
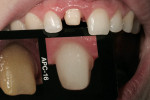
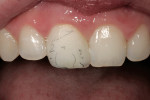
In the hydration stage (Figure 1), translucency, transparency, mamelon, and the amount of enamel overlay is checked. After the mouth is open for more than 10 seconds, dehydration begins to set in (Figure 2). During this stage, with the temporary in the mouth, the color of tooth No. 8 can be seen but not the translucency.
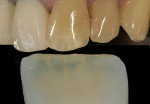
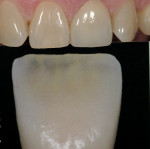
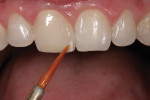
In Figure 3 a mamelon check is performed using the Chairside Shade Selection Guide. The mamelon color for this case is noted to be somewhere between beige and orange, with a blue tint to the incisal one third. The final choice, MA-4 or Clear Orange, is one of eight colors the guide offers (Figure 4).
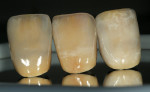
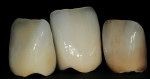
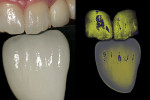
In a lab test to utilize dentin colors, white, light blue, clear, grey, and orange enamel modifications are applied to three sample crowns (Figure 5) in order to create different aspects of mamelon for the Chairside Shade Selection Guide. GC Initial™ Porcelain clear fluorescent (GC America Inc., www.gcamerica.com) is applied with facial glazing to create a different characteristic for each crown (Figure 6). Using different enamel modifications and enamel translucency through porcelain layering techniques, the photographed samples in Figure 7 demonstrate diverse aspects of internal color modifications. These are three of the 150 samples created for the Chairside Shade Selection Guide.
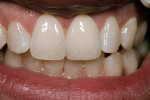
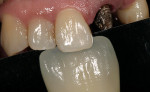
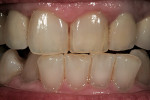
After the crown for central tooth No. 9 is fabricated using GC Initial IQ Press System material (GC America Inc.), the same patient as shown in Figure 4 receives her crown as a try-in, with the same value, translucency, and texture as her natural tooth No. 8 (Figure 8). Post-cementation, the crown is a complete match (Figure 9).
During the hydration stage, a translucency and mamelon enamel overlay check is performed, looking carefully for the degree of color value to apply (Figure 10). After the crown is cemented, with hydration, the restoration’s color value and translucency are a match (Figure 11).
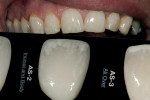
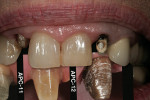
The Chairside Shade Selection Guide is used to check decalcification while the patient is hydrated (Figure 12). The important distinction is where will the color be added? Should it be added to just the incisal, the incisal and body, or all over the tooth? The patient in Figure 12 has decalcification, or anterior stain, in the incisal and body areas, a code of AS-2, or Incisal and Body, in the guide.
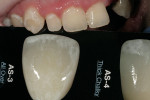
The patient shown in Figure 13 has a similar appearance to the patient shown in Figure 12, but the staining is defined as AS-3, or All Over. This will require a different sort of enamel modification in order to match with the patient’s adjacent teeth. The technician must have a good understanding of custom shading in order to capture the proper amount of staining to apply.
As shown in Figure 14 the Chairside Shade Selection Guide offers four different stages of decalcification, or anterior stain. The stain colors are each different to contrast the internal versus external colors and make them more obvious to the clinician and technician while they decide on the best possible match for the adjacent teeth pictured above the stain samples.
The image in Figure 15 was adjusted in Photoshop® with a gradient map filter as blue/yellow/blue to compare patient texture with shade guide samples. The surface texture of a tooth has the same type of appearance as a fingerprint, with the direction of the surface texture determined by many factors, including brushing techniques and types of food a person consumes. The particular texture shown in Figure 15 is called Horizontal Wave.
In Figure 16, surface texture, which again is clearly delineated through computer graphics, is vertical in appearance, not straight but wavy, with heavy areas of concentration in the pattern. Surface texture can be as individual as the person to whom the teeth belong.
The texture of the patient’s teeth in Figure 17 is heavier in certain areas, creating irregular lobe and reflection. The horizontal lines are light in appearance, while the vertical lines are heavier. Using the Chairside Shade Selection Guide for comparison, the best description for this surface texture is Natural, TE-6.
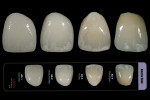
In Figure 18 the crowns created as samples of possible dehydration surface textures are shown above the associated images they would become in the Chairside Selection Guide: Dull (left), Rough (middle), and Shiny (right) are the possible three choices in this group. With six total surface texture possibilities available with the guide, the three remaining textures, shown in Figure 19, are titled Horizontal Wave (left), Vertical (middle), and Natural (right). Each crown was given a surface texture name and used in the Chairside Shade Selection Guide as a communication tool for dentists.
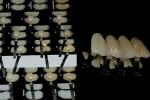
Through the study of maxillary natural, extracted teeth (Figure 20), much can be learned about texture, shape, color variations, and staining. In addition, natural, extracted mandibular teeth (Figure 21) provide a study tool regarding tooth morphology. Based on such research, as well as custom-shading studies, the Chairside Shade Selection Guide zirconia restorations shown in Figure 22 were created and photographed for communication purposes.
Research and development led to the improvement of dentin shade tabs in color selection, as shown in Figure 23. The materials pictured differ in composition: porcelain versus composite.
In another experiment with color, sectioning of various shade tabs (Figure 24) allows technicians to see thickness of enamel layering and apply multiple enamel modifier colors such as blue, white, and pink to the original color. This changes the color of the shade tab from a single color to one of multiple dimensions.
During the dehydration stage (Figure 25), vertical crack lines in the centrals become obvious but it is also important to note that the stump color is variable for this patient. Material selection must effectively cover the dark color. The finished restorations, as shown in Figure 26, proved to be a successful color match and after-prep color cover.
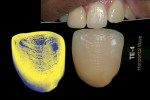
In Figure 27, dehydration/hydration again played a role in the effective matching of the stump shade for central tooth No. 8. The crown was eventually fabricated using the GC Press Initial System (GC America Inc.). As a bisque bake (Figure 28), the crown was tried in the mouth and the technician drew surface texture lines on the crown after the dehydration effect, matching with the adjacent teeth.
Lustre paste samples, such as GC Initial IQ One Body Lustre Paste (GC America Inc.) (Figure 29), offer many possibilities with which to work during the staining process. Lustre paste application (Figure 30) beautifies the restoration by creating variations in color.
The crown in Figure 31 is cemented and the patient dehydrated, highlighting the surface texture of the teeth. With rehydration post-cementation (Figure 32), note that the restoration is slightly shorter than the natural tooth No. 9. The incisal edge is slightly abbreviated due to orthodontics.
Conclusion
To provide effective custom shading, dental technicians must have an education regarding tooth morphology that extends into understanding natural tooth color, shape, and detailed modifications. Knowing the various conditions that may exist in the oral environment and having the proper tools with which to work can lead to satisfying end results. Concurrently, the technician’s expertise level is raised. There is no substitute for experience, and the more a technician studies natural teeth and performs custom shading for patients, the more he or she learns about achieving the best results possible.
This, in turn, leads to a clear understanding of the hydration/dehydration process, which is vital for technicians to succeed with their custom-shading procedures. A strategy must be in place prior to a patient’s appointment in order to produce matching results. Technicians must know the shade-matching process from start to finish. Know when to note the color of the adjacent teeth and when to look for surface texture. Mamelon, crack lines, and translucency are just a few other factors to consider.16
With a good strategy and communication tools in place, dental technicians can offer patients and clinicians a predictable and successful restoration. With all parties cooperating and with a clear understanding of the color-matching process, a technician will be able to provide exceptional work that will improve with experience over the course of time.17
References
1. Rieder CE. The role of operatory and laboratory personnel in patient esthetic consultations. Dent Clin North Am. 1989;33(2):275-284.
2. Goldstein RE. Esthetics in Dentistry. Philadelphia, PA: JB Lippincott; 1976:425-455.
3. Sproull RC. Color matching in dentistry. I. The three-dimensional nature of color. J Prosthet Dent. 1973;29(4):416-424.
4. O’Keefe KL, Strickler ER, Kerrin HK. Color and shade matching: the weak link in esthetic dentistry. Compend Contin Educ Dent. 1990;11(2):116-120.
5. Chu SJ, Devigus A, Mieleszko A. Fundamentals of Color. Carol Stream, IL: Quintessence Publishing; 2004.
6. Terry DA, Leinfelder KF, Geller W. Aesthetic & Restorative Dentistry. Stillwater, MN: Everest Publishing Media; 2009.
7. Kurtzman GM. Improving shade communication. Dent Today. 2008;27(2):132-136.
8. Alwan R, Kahng L. Behind the story: anterior shade-matching mamelon used from bench side. Inside Dentistry. 2009;5(8):84-86.
9. Vanini L, Mangani F. Determination and communication of color using the five color dimensions of teeth. Pract Proced Aesthet Dent. 2001;13(1):19-26.
10. Snyder TC. The importance of shade interpretation when bleaching. Dent Today. 2009;28(6):80-81.
11. Magne P, Belser U. Bonded Porcelain Restorations in the Anterior Dentition: A Biomimetic Approach. Carol Stream, IL: Quintessence Publishing; 2002.
12. Chiche GJ, Pinault A. Artistic and scientific principles applied to esthetic dentistry. In: Chiche GJ, Pinault A, eds. Esthetics of Anterior Fixed Prosthodontics. Chicago, IL: Quintessence Publishing; 1994:13-32.
13. Kahng L. Smile Selection plus CS³ Clinical Cases. Markham, Ontario: Palmeri Publishing; 2009.
14. Sproull RC. Color matching in dentistry. II. Practical applications in the organization of color. J Prosthet Dent. 1973;29(5):556-566.
15. Fradeani M. Esthetic Rehabilitation in Fixed Prosthodontics, Vol. 1. Esthetic Analysis: A Systematic Approach to Prosthetic Treatment. Carol Stream, IL: Quintessence Publishing; 2004.
16. Martignoni M, Schoenberger, AJ. Precision Fixed Prosthodontics: Clinical and Laboratory Aspects. Chicago, IL: Quintessence Publishing; 1990:255-258.
17. Hastings JH. Laboratory communications: Essential keys to exceptional results. Am Acad Cosmetic Dent J. 1998;13(4):22-30.
About the Author
Luke Kahng, CDT
Owner/Founder
LSK121 Oral Prosthetics
Naperville, Illinois