Immediate Temporization Crown Lengthening
Abstract
Background: The biologic width provides a tight seal around the tooth, protecting the periodontium from microbial injury and promoting periodontal health. However, clinical situations such as subgingival caries and crown-root fracture may compromise the biologic width dimension. Crown lengthening is a surgical technique that can be used to re-establish this important landmark in order to maintain periodontal health and long-term stability of the restorations. Method: A full-thickness mucoperiosteal flap is elevated to expose the bone and root surfaces. Debridement of the bone and root surfaces is completed and the crown preparation finalized, ensuring that at least 3 mm is between the restorative margin and alveolar bone crest. This guarantees preservation of the biologic width. The crown preparation is subsequently provisionalized to protect the tooth structure and promote soft-tissue healing. Results: Using the immediate temporization crown-lengthening (ITCL) technique, the crown preparation is finalized and impressions can be obtained during the surgical phase. This not only shortens the patient visits but also allows for the fabrication of a restoration of a good fit. The patient also receives a provisional restoration, which provides protection of the tooth structure and restores function and esthetics during healing. Conclusion: ITCL is a simple, straightforward, and predictable approach that can be easily incorporated into the daily practice of many dentists.
As dentistry evolves to encompass implant therapy, the number of implants placed in the United States has been increasing.1,2 This implies more teeth are being extracted as more implants are placed. Although implants have reasonably high success rates,3-6 implant failures7,8 can be emotionally devastating to both patients and clinicians. It was recently found that retaining a tooth over time is the most economical option compared to replacing it with an implant prosthesis.9 Hence, the importance of preserving the natural dentition cannot be ignored.
Crown lengthening, as defined by the American Academy of Periodontology, is “a surgical procedure designed to increase the extent of the supragingival tooth structure for restorative or esthetic purposes by apically positioning the gingival margin, removing supporting bone or both.”10 The goal of crown lengthening is to ensure a healthy restorative and periodontal relationship by reestablishing the required biologic width, namely, 1 mm of junctional epithelium and 1 mm of connective tissue attachment apical to the level of pathology.11 Crown lengthening is particularly useful in dealing with clinical situations, such as subgingival caries, crown or root fractures, cervical root resorption, short clinical crown heights, and iatrogenic defects around the cervical region. The procedure can be broadly categorized into esthetic crown lengthening or restorative crown lengthening.
The biologic width, also known as the physiologic dentogingival junction, consists of epithelial and connective tissue attachment.12 A classic study found that the mean biologic width is 2.04 mm.11 Though, the biologic width might differ from tooth to tooth, it is critical in the maintenance of periodontal health. It was shown that gingival inflammation increased when a crown margin was placed near the base of the gingival sulcus, thus impinging on the biologic width.13 In the fabrication of a crown, a ferrule provides resistance against lateral forces. The resistance is supplied by the parallel dentin walls coronal to the crown margins. The ferrule effect, as defined by Sorensen and Engelman,14 is the 360° metal collar of the crown that surrounds the parallel dentin walls coronal to the crown margin. It was found that 1 mm of dentin walls coronal to the crown margin was sufficient to resist failure.14 In general, 3 mm to 4 mm of tooth structure coronal to bone is necessary during crown preparation.
In sequential order, conventional crown lengthening involves flap design and incision, full-thickness mucoperiosteal flap reflection, degranulation, root planing, ostectomy, flap apical repositioning, flap closure with suturing, and placement of a periodontal dressing. However, the potential drawbacks include fracture or crack initiation and propagation in the weakened residual tooth structure; loss of the provisional restorations; and compromised esthetics and function leading to enhanced psychosocial stress for the patient during tissue healing. Re-violating the biologic width during tooth preparation may be possible, especially in areas of limited access, eg, distal line angles of a tooth.
To overcome these potential limitations of the conventional crown-lengthening technique, a new method, which considers the periodontal and restorative aspects of crown lengthening at the time of surgery, has been proposed. This article reviews the immediate temporization crown-lengthening (ITCL) technique. The objectives of this technique are to simplify crown lengthening for daily practice; shorten the overall chair time; provide the patient with esthetics, function, and comfort; protect the weakened tooth structure; and establish an adequate biologic width that is essential in the long-term stability of the periodontium and restorative treatment.
ITCL Technique
Prior to crown-lengthening surgery, clinical and radiographic examinations of the tooth involved and the surrounding structures are mandatory. The factors to note are the apical extension of the caries or fracture, the location of the osseous crest and furcation, restorability of the tooth, short-term and long-term prognoses, crown-to-root ratio, the strategic value of the tooth, and periodontal stability of the tooth in terms of clinical attachment loss.
Some of the key considerations when designing the incision are the probing depths, amount of keratinized tissue available, and the location of the furcation. A minimum of 2 mm of keratinized gingiva15 should be left and the furcation area should not be exposed16 in order to maintain periodontal health. The presence of the mucogingival junction in the facial and lingual flaps enables apical repositioning of the flaps to achieve an increase in crown exposure. As such, the reverse bevel incision design on the facial and lingual flaps is more conservative compared with the palatal flap. A more resective approach is encouraged when designing the incision on the palatal flap because of the tissue thickness and immobility. Therefore, the incision design aims to remove one half to two thirds of the pocket depth16 to achieve crown exposure and apical flap positioning.
A full-thickness mucoperiosteal flap is subsequently elevated atraumatically with either a Buser elevator (Hu-Friedy Mfg Co Inc, www.hu-friedy.com) or a No. 7 wax spatula (Hu-Friedy). A moist gauze can be placed on the bone surface beneath the flap to aid in pushing the flap apically with minimal flap trauma. With the flap elevation, direct access to the bone and root surfaces is achieved. At this stage, removal of all soft tissue is crucial not only to achieve hemostasis but also to accurately determine the cemento-enamel junction (CEJ) or the restorative margin. Degranulation can be performed using curettes, back action chisels, and Neumeyer’s bur (Brasseler USA, www.brasselerusa.com).
A clean field of view is achieved when degranulation is completed. It is strongly recommended to start preparing the tooth for either a crown or restoration because of the easier access and identification of the preparation margins. To preserve the biologic width, a minimum distance of 3 mm between the restorative margin and alveolar bone crest needs to be maintained.17,18 An end-cutting bur with 3-mm demarcation on the bur shank (Brasseler) can be used to create the biologic width with minimal damage to the adjacent structures. In cases in which the tooth has been endodontically treated and a post and core is necessary prior to crown placement, an additional 1.5 mm to 2 mm of crown height is required to create a ferrule effect,14,19 which prevents crown failure by enhancing its resistance form.20,21 The clinician can prepare the post space and take its impression in one visit.
The flap is carefully adapted apically and secured with either a vertical mattress suture or a continuous sling suture. The vertical-releasing incision is frequently closed with simple interrupted positional sutures. The tooth is subsequently temporized with a preformed or customized acrylic crown, which protects the weakened prepared tooth structure, promotes soft-tissue healing, and prevents its rebound. The occlusion on the provisional crown is adjusted to prevent mechanical complications, eg, acrylic fracture and biologic complications such as occlusal trauma. A periodontal dressing such as Coe-Pak™ (GC America, Inc, www.gcamerica.com) may be placed to protect the surgical area and apply positive pressure to apically position the flap.
In this technique, the flaps are secured apically with a vertical mattress suture or a continuous sling suture. Therefore, allowing the temporary crowns to be fabricated to the prepared level provides protection to the preparation margin. The final impression can be taken during the surgical visit or 8 weeks afterward to allow for soft-tissue healing. Determining the emergence profile of the crown restoration depends on the tooth morphology and its relation to the adjacent teeth. It is important to keep the crown contours flat instead of convex to facilitate oral hygiene practices and maintain periodontal health.22,23
The simplicity of the ITCL technique is illustrated here with two clinical cases. The first case features subgingival caries, while the second shows crown preparations.
Case 1
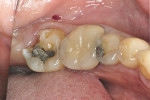
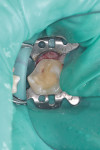
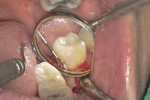
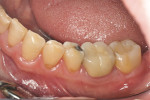
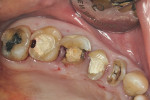
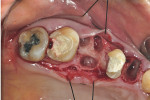
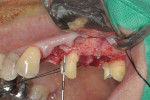
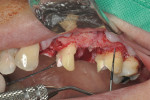
A 56-year-old woman presented with subgingival caries on the distobuccal surface of the mandibular left second molar (Figure 1). Crown lengthening was necessary prior to the placement of a composite resin restoration. After proper local anesthesia was used, a full-thickness mucoperiosteal flap with a mesial vertical releasing incision was elevated. The tooth was isolated using a rubber dam and restored with composite resin (Figure 2). The rubber dam was removed and crown lengthening was performed to create a 3-mm distance between the restoration margin and alveolar bone (Figure 3). The flap was apically repositioned and sutured. After surgery, the patient received written and verbal homecare instructions. The sutures were removed 1 week postsurgery, and the patient was satisfied with the clinical outcome, short dental visits, and improved function and esthetics. At the 8-week re-evaluation, the soft tissue around the tooth was healthy because the biologic width was preserved (Figure 4).
Case 2
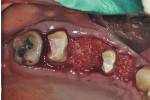
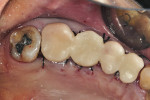
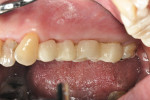
A 53-year-old woman presented with subgingival caries on the maxillary left premolars and molars. The maxillary first premolar and first molar were diagnosed as hopeless due to the extent of the caries (Figure 5). A reverse bevel incisional design was made and a full mucoperiosteal flap subsequently elevated. The hopeless teeth were extracted atraumatically to preserve the alveolar bone (Figure 6). The maxillary second premolar and molar were prepared for provisional crowns (Figure 7). Ostectomy was performed to create the 3-mm biologic width between the crown margins and alveolar bone crest (Figure 8 and Figure 9). Socket preservations were performed using the mineralized bone allograft plug technique24 (Figure 10). Then, the flaps were sutured close, and the provisional bridge was cemented (Figure 11). At the postoperative 8-week re-evaluation, good soft-tissue healing was observed (Figure 12).
Discussion
Violation of the biologic width often induces gingival inflammation and an associated loss of connective tissue attachment with the apical migration of the junctional epithelium.25 This occurs primarily due to a break in the hermetic seal around the tooth; hence, bacteria and their toxic byproducts are able to infiltrate the periodontal tissues. CL has been used to recreate the biologic width in order to maintain periodontal health.
The ITCL proposed here is a simple, straightforward, and predictable method that considers both surgical and restorative aspects, thus encouraging a positive periodontal–restorative relationship. The use of this technique provides the clinician with better access to the alveolar bone and root surfaces so that the biologic width can be preserved. A highly accurate impression also can be obtained due to enhanced visibility of and accessibility to the tooth structure. The mechanically weakened tooth structure will be protected by the provisional restoration from external insults that may damage or fracture it during healing. In addition, the provisional restoration provides function and esthetics, which increase patient satisfaction and comfort. Although ITCL is more technique-sensitive and requires a longer surgical time than conventional crown lengthening, the benefits outweigh the limitations.
Conclusion
As illustrated in the cases presented, the ITCL technique is a simple, straightforward, and predictable approach that can be easily incorporated into the daily practice of many dentists.
References
1. National Institutes of Health Consensus Development Conference statement on dental implants. June 13-15, 1988. J Dent Eucat. 1988;52(12):824-827.
2. Stillman N, Douglass CW. The developing market for dental implants. J Am Dent Assoc. 1993;124(4):51-56.
3. Ekelund JA, Lindquist LW, Carlsson GE, Jemt T. Implant treatment in the edentulous mandible: a prospective study on Brånemark system implants over more than 20 years. Int J Prosthodont. 2003;16(6):602-608.
4. Lindquist LW, Carlsson GE, Jemt T. A prospective 15-year follow-up study of mandibular fixed prostheses supported by osseointegrated implants. Clinical results and marginal bone loss. Clin Oral Implants Res. 1996;7(4):329-336.
5. Esposito M, Coulthard P, Worthington HV, et al. Interventions for replacing missing teeth: different types of dental implants. Cochrane Database Syst Rev. 2002;(4):CD003815.
6. Holm-Pedersen P, Lang NP, Müller F. What are the longevities of teeth and oral implants? Clin Oral Implants Res. 2007;18(suppl 3):15-19.
7. Tomasi C, Wennström JL, Berglundh T. Longevity of teeth and implants - a systematic review. J Oral Rehabil. 2008;35(suppl 1):23-32.
8. Gotfredsen K, Carlsson GE, Jokstad A, et al. Implants and/or teeth: consensus statements and recommendations. J Oral Rehabil. 2008;35(suppl 1):2-8.
9. Pretzl B, Wiedemann D, Cosgarea R, et al. Effort and costs of tooth preservation in supportive periodontal treatment in a German population. J Clin Periodontol. 2009;36(8):669-676.
10. Commonly Used Terms. American Academy of Periodontology’s glossary of definitions for common periodontal terms. American Academy of Periodontology Web site. 2001. Available at: https://www.perio.org/consumer/glossary.htm. Accessed December 18, 2009.
11. Gargiulo AW, Wentz FM, Orban B. Dimensions and relations of the dentogingival junction in humans. J Periodontol. 1961;32(3):261-267.
12. Vacek JS, Gher ME, Assad DA, et al. The dimensions of the human dentogingival junction. Int J Periodontics Restorative Dent. 1994;14(2):154-165.
13. Newcomb GM. The relationship between the location of subgingival crown margins and gingival inflammation. J Periodontol. 1974;45(3):151-154.
14. Sorensen JA, Engelman MJ. Ferrule design and fracture resistance of endodontically treated teeth. J Prosthet Dent. 1990;63(5):529-536.
15. Lang NP, Löe H. The relationship between the width of keratinized gingiva and gingival health. J Periodontol. 1972;43(10):623-627.
16. Ochsenbein C. A primer for osseous surgery. Int J Periodontics Restorative Dent. 1986;6(1):8-47.
17. Ingber JS, Rose LF, Coslet JG. The “biologic width”--a concept in periodontics and restorative dentistry. Alpha Omegan. 1977;70(3):62-65.
18. Lanning SK, Waldrop TC, Gunsolley JC, Maynard JG. Surgical crown lengthening: evaluation of the biological width. J Periodontol. 2003;74(4):468-474.
19. Trabert KC, Cooney JP. The endodontically treated tooth. Restorative concepts and techniques. Dent Clin North Am. 1984;28(4):923-951.
20. Ichim I, Kuzmanovic DV, Love RM. A finite element analysis of ferrule design on restoration resistance and distribution of stress within a root. Int Endod J. 2006;39(6):443-452.
21. Pereira J, de Ornelas F, Conti PC, do Valle AL. Effect of a crown ferrule on the fracture resistance of endodontically treated teeth restored with prefabricated posts. J Prosthet Dent. 2006;95(1):50-54.
22. Kohal RJ, Pelz K, Strub JR. Effect of different crown contours on periodontal health in dogs. Microbiological results. J Dent. 2004;32(2):153-159.
23. Yuodelis RA, Weaver JD, Sapkos S. Facial and lingual contours of artificial complete crown restorations and their effects on the periodontium. J Prosthet Dent. 1973;29(1):61-66.
24. Wang HL, Tsao YP. Mineralized bone allograft-plug socket augmentation: rationale and technique. Implant Dent. 2007;16(1):33-41.
25. Schätzle M, Land NP, Anerud A, et al. The influence of margins of restorations of the periodontal tissues over 26 years. J Clin Periodontol. 2001;28(1):57-64.
About the Authors
Shih-Chang Tseng, DDS
Private Practice
Taipei, Taiwan
Jia Hui Fu, BDS
Resident
Department of Periodontics and Oral Medicine, School of Dentistry
University of Michigan
Ann Arbor, Michigan
Hom-Lay Wang, DDS, MSD, PhD
Professor and Director of Graduate Periodontics
Department of Periodontics and Oral Medicine, School of Dentistry
University of Michigan
Ann Arbor, Michigan