Reducing Chronic Massetter and Temporalis Muscular Hyperactivity with Computer-Guided Occlusal Adjustments
Robert B. Kerstein, DMD
Abstract
Muscle hyperactivity is a potential source of symptomatology in patients with temporomandibular disorders. Various occlusal adjustment procedures have been advocated to reduce hyperactivity. A new, measurement-driven, occlusal adjustment procedure, known as immediate complete anterior guidance development (ICAGD), has been shown through nonsimultaneous electromyography to lessen masticatory muscle hyperactivity effectively by reducing posterior disclusion time to < 0.4 sec in all mandibular excursions. This reduction, in turn, lessens the volume of periodontal ligament compressions that create additive and excessive functional muscle contractions via a feedback mechanism involving the trigeminal nerve. This case report describes the treatment of chronic muscular hyperactivity with a computer-guided ICAGD enameloplasty and simultaneously recorded electromyography. Follow-up visits showed that after reduction, the pretreatment levels of excursive muscular hyperactivity were lessened and lasting. This result is caused by the shortened posterior disclusion time resulting in an equally reduced time to muscle shutdown.
Muscle hyperactivity is believed to be a potential source of symptomatology in patients with temporomandibular disorders (TMDs).1,2 Cited causes are bruxism,1,3 clenching habits,4 malocclusion,5 and occlusal interferences.1,2,6 Many treatments for hyperactivity are aimed at the symptoms. Muscle relaxants and other medications,7 physical therapy to the jaw musculature,8 appliance therapy,4 oral deprogramming, and transcutaneous electrical nerve stimulation (TENS)9 also have been advocated as viable treatments to relieve symptoms. Relaxation of the muscles with occlusal splints,4 medications,7 and the other therapies previously described8,9 represent the class of noninvasive methodologies that, when implemented and successful, can limit the need for other more definitive forms of treatment.
However, in cases of chronic myofacial pain dysfunction syndrome (MPDS),10 in which initial attempts to use reversible therapies do not resolve or reverse the symptoms of muscular hyperactivity, the patient undergoes long-term orthotic use in an attempt to lessen the recurrence of frequent symptoms. Appliance therapy does not cause these ongoing symptoms but does not resolve them either. This treatment approach does not offer resolution to patients with chronic, significant symptoms. Usually, these patients self-treat ongoing symptoms with frequent use of anti-inflammatories, muscle relaxants, and pain medications. In addition, they may require ongoing visits to a physical therapist or a chiropractor as adjunctive support.
Patients with chronic MPDS live with a level of symptoms that is life-interfering, while having both the negative systemic sequelae related to long-term medication use (both physical and psychological addictions; liver and kidney problems) and the negative dental sequelae of long-term appliance use (formation of an open occlusion, both anterior and/or posterior depending on splint design, and developing arches that do not relate spatially from a changed occlusal vertical dimension [OVD] that affects condyler position). To avoid these sequelae and attempt to resolve any nonresolving muscular symptoms, the implementation of more definitive therapy can be warranted. Before instituting any nonreversible treatment, assessments of the OVD, temporomandibular joint (TMJ) health (with imaging and joint vibration analysis [BioJVA™, BioResearch Associates, https://www.bioresearchinc.com]), muscular health (with muscle palpation and electromyography measurements of both rest and functional movements [BioEMG™ II, BioResearch Associates]), occlusal relations, and the numbers of missing teeth are all required to make a reliable diagnosis. In patients in whom the diagnostic and biometric assessments reveal that the overriding condition is a muscular-based problem with normal vertical dimension, no internal derangements, and near-normal occlusal relations, the quality of the occlusal contacts often can be a significant contributory factor to the chronic nature of the patients’ condition. Then, occlusal adjustments can be considered as a treatment.
Occlusal adjustment has been advocated to reduce chronic hyperactivity.1,2,11 Multiple studies have shown occlusal adjustment can be an effective treatment for the symptoms of TMD syndrome,11-16 while other research reports no clinical improvements from occlusal adjustments performed on patients with TMD.17
Muscle activity level reductions and the muscle contraction symptoms of chronic MPDS have been shown by one researcher to be treatable physiologically (no adjunctive therapy, no splint therapy, and no medication therapy)11-13,18 by a measurement-driven, computer-guided, occlusal adjustment procedure that has the primary therapeutic goal of measurably decreasing the time required for all molars and premolars to disclude from each other in fractions of seconds during mandibular excursions (disclusion time < 0.4 sec).11 The immediate complete anterior guidance development (ICAGD)11 coronoplasty is performed with the aid of a computer system (T-Scan® III, Tekscan, https://www.tekscan.com) that records real-time measurements of excursive movements as dynamic force movies.
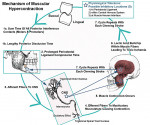
A previously published mechanism for the etiology of masticatory muscular hyperactivity18 described how afferent mechanoreceptors of the molar and premolar periodontal ligaments, when compressed by prolonged excursive tooth contact, activate excess muscle contractions in the masticatory muscles (Figure 1). These afferent fibers synapse with efferent fibers of the trigeminal nerve that emanate in the mesencephalic nucleus of the brain and feed back to the masticatory musculature to instruct the muscles to contract. The longer the time of the excursive interferences, the longer the period that the periodontal ligaments are compressed and the longer the time that the masticatory muscles are activated to contract.18 This cycle repeats with every posterior tooth compression such that prolonged occlusal surface engagement during both functional and parafunctional mandibular movements adds on excessive muscle contractions to the baseline contractions, which are required by the musculature to move the mandible. In patients who are susceptible, this additive effect is a constant source of excessive masticatory muscle contractions resulting in lactic acid accumulation, which often leads to the clinical appearance of muscular hyperactivity.18
The observed reduction in muscular hyperactivity reported from properly performing ICAGD is caused by the decreased time of occlusal surface engagement during excursive movements, which result in an equally decreased time of periodontal ligament compressions. This decrease directly results in muscle activity level reductions posttreatment in the masseter and temporalis (P < .05).11 This physiologic effect is lasting (posttreatment disclusion time has demonstrated permanence19). In a 3-year controlled occlusal adjustment study involving 30 patients with MPDS, ICAGD statistically improved the muscle contraction symptoms of the 17 patients who received treatment without the use of splints or medications to aid in symptom resolution.13 The symptom reductions remained absent in the treated group throughout the duration of the patients’ study participation, as each subject was recalled numerous times in the following year for re-evaluation after receiving the ICAGD enameloplasty. In a separate 9-year recall study of 102 patients who had received ICAGD, statistically significant reductions of masticatory muscle contraction symptomatology were maintained for years after active treatment was completed.12 Lastly, in a study of 62 patients with the condition who underwent ICAGD, posttreatment maximum clench capacity was statistically greater than the pretreatment clench capacity measured in the bilateral massetter and temporalis muscles.20
ICAGD is indicated for use in patients with TMD who exhibit primarily muscular contraction symptomatology and whose anterior teeth couple or near couple. ICAGD is contraindicated in individuals with Class II Division II, patients with severe open occlusion, and people who demonstrate primary internal derangements, such as locking, dislocating, avascular necrosis of the condyle, and/or tumors of the TMJs. Documented complications from using ICAGD are similar to those of other occlusal adjustment/equilibration procedures, including the possibility of developing tooth sensitivity and perforating some occlusal restorations.21 Before receiving any ICAGD corrections, patients are advised that, after treatment, some existing restorations may require replacement from the adjustment process and, if teeth become sensitive, short-term daily fluoride rinsing may be necessary to remineralize occlusal surfaces.
Occlusal equilibration1 is an alternative occlusal adjustment procedure, which has been used to lessen muscular symptomatology. Equilibration differs from ICAGD procedurally. Equilibration’s primary goal is to eliminate the centric relation–centric occlusion discrepancy and remove tooth contacts that interfere with mandibular movement, in and out of a clinician-controlled centric relation position.1 Other procedural differences have been described;18 however, the most significant difference between these two occlusal adjustment procedures is that ICAGD is a computer-guided, measured correction with specific numerical occlusal endpoints that are quantifiably determined by posttreatment computer measurements of tooth contact durations in functional movements. The optimal posttreatment numerical endpoint parameters are: disclusion time ≤ 0.4 sec bilaterally and in protrusion, closure contact time simultaneity in which all teeth occlude in ≤ 0.2 sec, total occlusal force vector summation centered within all contacting teeth resulting in arch half force percentage nearing 50% +/- 2% equality, and quadrant force percentage nearing 25% +/- 2% equality with individual tooth contact near force equality.21,22
Alternatively, occlusal equilibration endpoints are not determined by calculation or measurement, but by feel, sounds, paper-mark size, and color (subjective interpretation), the patient’s subjective occlusal feel assessments, bimanual manipulation, clench testing, and clinician assessment of all these variables.1
Of all these variables for the clinician to interpret, paper-mark size has been advocated in textbooks on occlusion to be an indicator of occlusal load such that equal paper-mark size has been advocated to indicate equal contact load.1,23 These longstanding author-advocated concepts have never been proven accurate in any scientific study, such that no literature supports these advocated paper-mark size concepts. Recently, it has been demonstrated in research analyzing the size of 600 articulating paper marks made at varying human occlusal loads that articulating paper-mark area (size) is not representative of the occlusal force content within a given mark.24 Only 20% of the time did the mark area and the applied load correlate. The study data indicated statistically that equal-size marks on neighboring teeth did not demonstrate equal occlusal load content.24 Additionally, the range of mark areas over a given load was so broad that it would be impossible for a clinician to reliably predict which marks contain the highest loads when trying to select the correct marks to equilibrate.24 These findings confirm the results of other studies performed on articulating paper markings, which also showed that articulating paper-mark size does not reliably describe occlusal forces.25-27
This high variability of paper-mark load content would tend to make occlusal equilibration somewhat unpredictable in its precision, therefore affecting the capacity of the treatment to render highly therapeutic neurophysiologic effects. ICAGD relies on both closure and excursive contact time measurements posttreatment to determine its accuracy. The articulating paper marks are used only as contact locators of the problematic contacts determined by pretreatment computerized force and time measurements. The paper-mark size is never used as an occlusal force indicator, therefore, there is no subjective mark size interpretation used to assess the correctness of the occlusal endpoints.
An additional theoretical difference between ICAGD and equilibration is that equilibration theory describes periodontal ligament mechanoreceptors as excitatory only to the lateral pterygoid when occlusal interferences affect its ability to position the condyle in centric relation, while the other elevator muscles bring the teeth into complete intercuspation.1 ICAGD publications11,18 describe the excitatory nature of the periodontal ligament mechanoreceptors to be a consequence of daily prolonged posterior tooth occlusal surface engagement that repeatedly, through the course of any given day, compresses the ligament fibers multiple times. These ligament compressions are an ongoing and self-perpetuating phenomenon that persists through the life of the occlusion as normal chewing and abnormal parafunction repeatedly occur. The feedback loop (Figure 1) affects all the masticatory muscles innervated by various branches of the trigeminal nerve.
Recently, previously separate dental computer technologies have been synchronized (T-Scan/BioEMG linking software, Tekscan Inc/BioResearch Associates technology partnership), which affords the clinicians the ability to simultaneously record and acquire data from both programs together. When used with ICAGD, the posttreatment impact on the feedback loop by shortening disclusion time can be observed immediately (at the end of Treatment Day 1) within the electromyograph (EMG) traces. This case report describes a patient whose chronic muscular hyperactivity was diagnosed as chronic MPDS that was treated with ICAGD, which was guided by the computerized occlusal analysis/EMG synchronization module. By comparing the pre- and posttreatment EMG tracings, a measurable lessening of excursive contractile muscle activity to near resting-state values and a decreased time to muscle shutdown in the same excursion was observed posttreatment. Recalling the patient at 2 weeks and 4 months from Treatment Day 1 illustrates that, when properly performed, ICAGD maintains a nonhyperactive excursive muscular state.
Case Report
A 48-year-old female presented with chronic muscular hyperactivity symptoms, including facial pain, clenching and bruxism with jaw pain in the morning, regular temporal headaches, fatigue during mastication, and a history of long-term pain medication and appliance use without symptom resolution. As a Class I occlusal scheme, she presented with anterior tooth coupling. Findings from a clinical examination, load test, and BioJVA revealed no internal derangements.
Recording disclusion time has been described previously21 and validated procedurally in scientific studies.12,13,19 With self-adhesive bipolar EMG electrodes placed bilaterally over the bodies of the superficial massetter and the anterior temporalis muscles parallel to the direction of the muscle fibers, a recording was activated in which both the BioEMG II and T-Scan III began data acquisition simultaneously. The patient made a complete intercuspated voluntary closure, held her teeth together for 1 sec to 3 sec, and commenced a right excursion from the completely intercuspated position until only anterior teeth were in contact (canines, lateral incisors, central incisors). The process was repeated for the alternative left lateral and protrusive excursions.
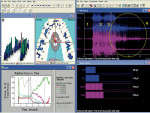
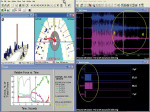
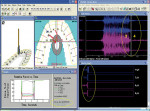
The pretreatment left excursion recording separated into four specific time locations can be seen in Figure 2a, Figure 2b, Figure 2c and Figure 2d. Changing tooth contact sequence, changing occlusal forces, and fluctuating muscle activity levels of the temporalis and massetter muscles were recorded simultaneously and continuously from a nonoccluded position into intercuspation, followed by excursive commencement to the completion of the excursion where muscle shutdown occurred. Pretreatment, after excursive commencement, the working temporalis and the bilateral massetter muscles were still very active well past 0.4 sec because of the prolonged posterior tooth contact (seen in the T-Scan III force plots). The time distance from excursive commencement to the completion of the excursion was 2.5 sec. For brevity, no right lateral or protrusive figures are presented.
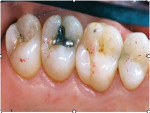
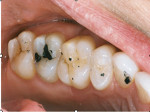
Then, ICAGD was performed, as previously described21 but summarized here. After air-drying opposing maxillary and mandibular quadrants, the patient was instructed to self-close into her maximal intercuspal position (MIP) with articulating paper (AccuFilm®, Parkell, https://www.parkell.com) interposed between the teeth on one side of her mouth, to commence a working mandibular excursion; slide back into MIP; then from MIP, make a balancing mandibular excursion; and again slide into MIP. These movements were not guided or controlled by the clinician in any way. The pretreatment maxillary left posterior quadrant articulating paper marks depicted a long disclusion time (Figure 3).
The computer recordings made of the pretreatment left working excursion guided the clinician to the regions requiring contact labeling. Then, on the side just marked, the clinician removed “by eye” any inclined plane linear contact marks, which represented lengthy disclusion time, with a 0.018-mm round diamond bur (Model No. 6801, Brasseler USA, https://www.brasselerusa.com) leaving the central fossa, cusp tip, and marginal ridge nonlinear contacts only. After the first set of paper markings were adjusted, the patient was instructed to repeat the mandibular excursions to re-mark the same two quadrants and similar adjustments followed. This process was repeated until no linear contact marks remained and visual disclusion was achieved in both the working and balancing movements on that initial side of the mouth. The same process was performed on the opposite side of the mouth until all posterior teeth in the four opposing quadrants had “visual disclusion.” Protrusive corrections followed bilaterally until visual confirmation of disclusion was achieved. Then, the patient made several unguided closures into the new maximum intercuspal position through the articulating paper. The new closure contacts were adjusted selectively until they appeared widespread and uniform. Tooth polishing followed.
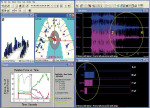
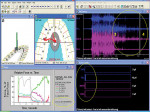
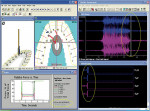
Next, the posttreatment right, left, and protrusive excursive movements and the new intercuspal contacts were measured with the computerized occlusal analysis/EMG synchronization software to determine the quality of the “by eye” paper-only adjusted result. The posttreatment force movies revealed non-ideal disclusion times (> 0.4 sec), occlusal contact nonsimultaneity (all teeth occluding in > 0.2 sec), unequal arch half force percentages (greater than +/- 2%), and poor force summation vector position (noncentered among all occluding teeth); all of which could not be determined visually. Guided by these and successive force movies, further lateral and closure occlusal adjustments were performed until measurable short disclusion time (< 0.4 sec) and all the other precise occlusal force parameters were met.18,21,22 Posttreatment computerized occlusal analysis/EMG recordings of the left excursion can be seen in Figure 4, which shows the muscular changes that resulted from obtaining true and measurable immediate posterior disclusion. Within the EMG tracing, after excursive commencement posttreatment (within 0.3 sec), all muscles reached the resting state and the time distance from excursive commencement to the completion of the excursion was only 0.24 sec.
The second treatment appointment occurred 2 weeks later. A new set of disclusion time measurements were obtained, and further computer-guided occlusal adjustments were performed to improve on all the precision endpoints obtained in the first appointment. This process mimicked the first treatment appointment except that higher precision numerical occlusal endpoints were achieved where possible. This appointment completed the treatment phase. Figure 5 illustrates the paper labeling representative of short disclusion time. Figure 6 shows the computerized occlusal analysis/EMG recordings of the left excursion at the end of Treatment Day 2.
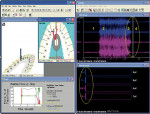
Figure 7 shows the 4-month follow-up computerized occlusal analysis/EMG data for the left excursion. Note the lack of hyperactivity in the excursive period and the very similar time to muscle shutdown as seen in the Treatment Day 1 posttreatment condition (Figure 4). The low level of functional contractile muscle activity demonstrated permanence.
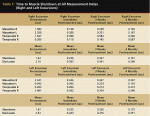
Table 1 contains all recorded mean disclusion times, electromyography microvolt values, and the mean times to muscle shutdown for the pretreatment condition, the treatment session, and the two follow-up visits.
Discussion
In chronic MPDS, patients experience a nonresolving, chronic hyperactive muscular state characterized by persistent facial pain and temporal headaches, chronic splint use, frequent pain medication ingestion, and continuing supportive adjunctive therapy that is ongoing and regular. Precision-measured occlusal adjustments have been shown repeatedly in one researcher’s published occlusal adjustment studies to be effective therapeutically at lessening the chronic symptomatology while simultaneously reducing the need for any ongoing therapies.11-13,17 Long-term data gathered in a 9-year recall study of 102 patients who had undergone ICAGD showed that statistically significant reductions of masticatory muscle contraction symptomotology, medication use, and appliance use were maintained for years after active treatment was completed.12 Additional clinical implementation data of the use on ICAGD on more than 1000 patients with MPDS and TMD performed in a private practice setting from 1986 to the present, as well as in a dental school clinic between 1984 and 1997, have confirmed the clinical efficacy of this computer-guided occlusal adjustment procedure. It is the creation of measured and exact occlusal adjustment endpoints that appears to resolve the chronicity of the symptomatology.
ICAGD shortens posterior disclusion time to < 0.4 sec per excursion, which establishes an occlusal scheme in which the posterior teeth compress each other and their respective periodontal ligament fibers for far less time than during an untreated occlusion or in a treated condition accomplished without measurement of occlusal endpoints. This reduction shortens the contraction time of the masticatory muscles because the feedback loop no longer adds contractions to baseline functional movements. A posttreatment physiologic muscular relaxation is established by precisely altering the timing of functional excursive contacts at the occlusal surface.
Table 1 demonstrates the time to muscle shutdown is directly related to the time of periodontal ligament compression, which is nearly equal in length to the disclusion time. Pretreatment long disclusion time is mirrored by a lengthy time to muscle shutdown in six of eight muscles in both excursions. Only the nonworking temporalis quickly shuts down regardless of the duration of the disclusion. This observation indicates that only the nonworking temporalis is not influenced by excursive tooth contacts regardless of which side of the arch they occur. An examination of this patient’s posttreatment EMG and disclusion time data of the other three muscles involved in any given excursion showed that a rapid time to muscle shutdown was observed with very short disclusion time. Permanence to the time to muscle shutdown was seen in the follow-up appointments. At 4 months, the mean time to muscle shutdown was shorter than at 2 weeks posttreatment. With no more additive muscle contractions present to activate the musculature continually, each muscle shuts off more rapidly, implying healing within the fibers had occurred, which resulted in more efficient functional muscle relaxation.
ICAGD is an occlusal adjustment procedure that requires measurement and calculation to ensure the occlusal changes will lessen the hyperactive pretreatment state measurably by controlling the time that periodontal ligament mechanoreceptors are compressed. “By eye” and “paper-only” adjusting is based on subjective assessments of paper labeling. With those methods, the clinician assumes the paper markings describe occlusal force and time simultaneity, although research has shown this premise to be unsubstantiated.24-27 Therefore, the clinician is not cognizant of whether ideal occlusal endpoints have been obtained and cannot be sure that the occlusion is adjusted precisely. The clinical reality that alternative occlusal adjustment procedures are unmeasured may be partially responsible for the reported lack of effectiveness of occlusal adjustment therapy in the treatment of TMDs.17
Conclusion
This case report demonstrated that physiologic lessening of chronic masticatory muscular hyperactivity in a patient with MPDS can be accomplished with a modern occlusal adjustment procedure that is an alternative to occlusal equilibration. ICAGD is a measurement-driven enameloplasty, such that the performed occlusal changes precisely optimize force and time occlusal endpoints. When properly performed, its clinical effect minimizes periodontal ligament compression time so that the reduced duration of compressions does not add extra muscle activity to the functional baseline. This result translates into a rapid time to muscle shutdown of the bilateral massetter and working temporalis during excursive movements. Since 1990, ICAGD has been shown in research studies and clinical reports to have a positive therapeutic effect on masticatory muscle physiology.
Disclosure
Dr. Kerstein is a consultant for Tekscan.
References
1. Dawson PE. Functional Occlusion: From TMJ to Smile Design. Vol 1. St. Louis, MO: Mosby; 2007:54,266,347,393-399,412.
2. Glickman I. Clinical Periodontics. 5th ed. Philadelphia, PA: Saunders and Co; 1979:948,978.
3. Clayton JA, Kotowicz WE, Zahler JM. Pantographic tracings of mandibular movements and occlusion. J Prosthet Dent. 1971;25(4):389-396.
4. Bertram S, Rudisch A, Bodner G, et al. Effect of stabilization-type splints on the asymmetry of masseter muscle sites during maximal clenching. J Oral Rehabil. 2002;29(5):447-451.
5. Mohlin BO, Derweduwen K, Pilley R, et al. Malocclusion and temporomandibular disorder: a comparison of adolescents with moderate to severe dysfunction with those without signs and symptoms of temporomandibular disorder and their further development to 30 years of age. Angle Orthod. 2004;74(3):319-327.
6. Baba K, Yugami K, Yaka T, et al. Impact of balancing-side tooth contact on clenching induced mandibular displacements in humans. J Oral Rehabil. 2001;28(8):721-727.
7. Herman CR, Schiffman EL, Look JO, et al. The effectiveness of adding pharmacologic treatment with clonazepam or cyclobenzaprine to patient education and self-care for the treatment of jaw pain upon awakening: a randomized clinical trial. J Orofac Pain. 2002;16(1):64-70.
8. McNeely ML, Armijo Olivo S, Magee DJ. A systematic review of the effectiveness of physical therapy interventions for temporomandibular disorders. Phys Ther. 2006;86(5):710-725.
9. Alvarez-Arenal A, Junquera LM, Fernandez JP, et al. Effect of occlusal splint and transcutaneous electric nerve stimulation on the signs and symptoms of temporomandibular disorders in patients with bruxism. J Oral Rehabil. 2002;29(9):858-863.
10. Gavish A, Winocur E, Menashe S, et al. Experimental chewing in myofascial pain patients. J Orofac Pain. 2002;16(1):22-28.
11. Kerstein RB, Wright N. Electromyographic and computer analysis of patients suffering from chronic myofascial pain-dysfunction syndrome; before and after treatment with immediate complete anterior guidance development. J Prosthet Dent. 1991;66(5):677-686
12. Kerstein RB. Treatment of myofascial pain dysfunction syndrome with occlusal therapy to reduce lengthy disclusion time—a recall evaluation. Cranio. 1995;13(2):105-115.
13. Kerstein RB, Chapman R, Klein M. A comparison of ICAGD (immediate complete anterior guidance development) to mock ICAGD for symptom reductions in chronic myofascial pain dysfunction patients. Cranio. 1997;15(1):21-37.
14. Forssell H, Kirveskari P, Kangasniemi P. Effect of occlusal adjustment on mandibular dysfunction. A double-blind study. Acta Odontol Scand. 1986;44(2):63-69.
15. Kirveskari P, Le Bell Y, Salonen M, et al. Effect of elimination of occlusal interferences on signs and symptoms of craniomandibular disorder in young adults. J Oral Rehabil. 1989;16(1):21-26.
16. Vallon D, Ekberg E, Nilner M, et al. Occlusal adjustment in patients with craniomandibular disorders including headaches. A 3- and 6-month follow-up. Acta Odontol Scand. 1995;53(1):55-59.
17. Tsolka P, Morris RW, Preiskel HW. Occlusal adjustment therapy for craniomandibular disorders: a clinical assessment by a double-blind method. J Prosth Dent. 1992;68(6):957-964.
18. Kerstein RB. A comparison of traditional occlusal equilibration and immediate complete anterior guidance development. Cranio. 1993;11(2):126-140.
19. Kerstein RB. Disclusion time measurement studies: stability of disclusion time: a 1-year follow-up. J Prosthet Dent. 1994;72(2): 164-168.
20. Kerstein RB, Radke J. The effect of disclusion time reduction on maximal clench muscle activity levels. Cranio. 2006:24(3);156-165.
21. Kerstein RB. Disclusion time-reduction therapy with immediate complete anterior guidance development to treat chronic myofascial pain-dysfunction syndrome. Quintessence Int. 1992;23(11):735747.
22. Kerstein RB, Grundset K. Obtaining measureable bilateral simultaneous occlusal contacts with computer analyzed and guided occlusal adjustments. Quintessence Int. 2001;32:7-18.
23. Okeson JP. Management of Temporomandibular Disorders and Occlusion. 5th ed. St. Louis, MO: Mosby and Co; 2003:416,418,605.
24. Carey JP, Craig M, Kerstein RB, et al. Determining a relationship between applied occlusal load and articulating paper mark area. The Open Dentistry Journal. 2007;(1):1-7.
25. Carossa S, Lojacono A, Schierano G, et al. Evaluation of occlusal contacts in the dental laboratory: influence of strip thickness and operator experience. Int J Prosthodont. 2000;13(3):201-204.
26. Saad MN, Weiner, Ehrenberg D, et al. Effects of load and indicator type upon occlusal contact markings. J Biomed Mater Res B Appl Biomater. 2008;85(1):18-22.
27. Millstein P, Maya A. An evaluation of occlusal contact marking indicators. A descriptive quantitative method. J Am Dent Assoc. 2001;132(9):1280-1286.
About the Author
Robert B. Kerstein, DMD
Former Assistant Clinical Professor
Department of Restorative Dentistry
Tufts University School of Dental Medicine
Boston, Massachusetts