A Conservative Approach to Anterior Esthetics
Treating Dentist:
Michael T. Ricciardi, DDS
Private Practice, Staten Island, New York
Technician:
Peter Pizzi, MDT
Owner, Pizzi Dental Studio Inc, Staten Island, New York
Background
Age at Initial Presentation: 17
Initial Presentation: April 18, 2008
Active Treatment Completed: February 16, 2009
Medical History
The patient had no contributory medical history and took no medications.
Dental History
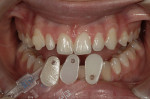
After a referral, the patient presented for a cosmetic consultation. She did not like the interdental spacing following orthodontic treatment and had been advised that she would need eight to 10 veneers to close all spacing. The patient said the orthodontist left the space because her teeth were too small and she would need veneers to fix the discrepancy. She was also concerned about the small “peg” lateral in the No. 7 position and said she wanted this corrected.
The dental history was limited to general 6-month recall appointments and orthodontics. The patient had no history of carious lesions or tooth extractions. She had received orthodontic treatment for approximately 18 months from age 15 to 17. The details of that treatment were based on the patient’s and parents’ recollections—the orthodontist was not available for discussion. The patient and her parents were unhappy and believed that the treatment ended prior to optimum esthetic results.
Diagnostic Findings
Temporomandibular Joints: Right and left joint areas tested normal to loading with no discomfort. The patient had no clicking, popping, or crepitus. She claimed no history of joint discomfort prior to or after orthodontic treatment. No deviation was noticed on opening or closing. She had a normal range of motion on opening and normal left and right lateral excursions.
Extraoral: Normal
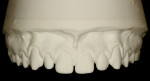
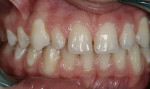
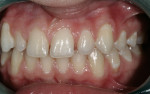
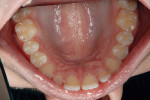
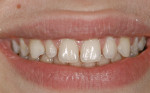
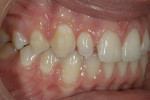
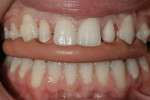
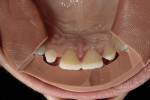
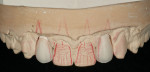
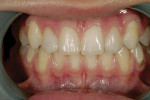
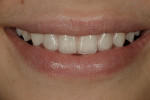
Intraoral: All soft tissue was normal and healthy. The patient presented with mild buccal recession on teeth Nos. 21 and 28. She had postorthodontic spacing of the maxillary anterior teeth (Figure 1). Tooth No. 7 was smaller than No. 10, and the tissue position on tooth No. 7 was more coronal, causing a slight disharmony (Figure 2). The tissue on teeth Nos. 6 and 11 was more apical than desired, but no exposed root surface was observed (Figure 3). Although not ideal, this did not affect the gingival harmony. Periodontal probing did not reveal notable pocket depths.
Occlusal Notes
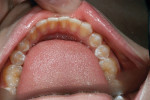
At the initial evaluation, no occlusal issues were seen. There were no signs of wear or apparent occlusal dysfunction or constriction present (Figure 4 and Figure 5). Maintaining a stable occlusion was a concern, especially because the patient had recently completed orthodontic treatment. On checking her function, it was noted that the patient lacked proper canine guidance.
Radiographic Assessment
All radiographic findings were normal. There was no bone loss, no apparent pulpal pathology, and no radiographic decay.
Diagnosis
Periodontal: AAP Type II
Biomechanical: The patient presented with no history of carious lesions and no structurally compromised teeth. The dentition was biomechanically sound.
Functional: Acceptable function. This was determined by the lack of past or present functional signs or symptoms.
Risk Assessment
Dentofacial: Moderate. Managing the space issue of the maxillary anterior teeth would increase the patient’s risk. All treatment options, which included veneers and Invisalign® braces (Align Technology, https://www.invisalign.com), and their risks and benefits, as well as the expected outcomes, were explained to the patient. Tissue augmentation on tooth No. 7 to achieve more harmonious gingival architecture was also discussed. Because of the tooth size, gingival discrepancy, and spacing present, the risks associated with achieving optimal esthetics were explained.
Periodontal: Low. This patient was AAP Type II and had no signs of inflammation or periodontal disease.
Biomechanical: Low.
Functional: Moderate. Although acceptable function was noted, the guidance and future occlusal stability was in question. Not managing the occlusion might have increased the risk and compromised any completed restorations.
Prognosis
Dentofacial: Good. By evaluating the anterior spacing, the ceramist and treating dentist determined the tooth size and shapes needed in the final restoration. It was possible to combine Invisalign, veneers, and gingival augmentation of tooth No. 7 for a good result.
Periodontal: Good. The patient began a 6-month recare program to maintain her AAP Type II status.
Biomechanical: Good. Conservative veneer preparations combined with Invisalign led to a good biomechanical prognosis.
Functional: Good. An Invisalign aligner was used to bring teeth Nos. 6 and 11 into proper position for canine guidance. After the Invisalign treatment, a Kois Dento-Facial Analyzer System (Panadent, https://www.panadent.com) was used for occlusal equilibration to ensure long-term stability of function and occlusion.
Concerns
Performing irreversible restorative procedures in a young patient will always trigger concerns about the long-term risks and benefits. All treatment options must be evaluated and presented to the patient. This patient had desired eight to 10 porcelain veneers to solve the postorthodontic spacing. It was a challenge to suggest more tooth movement to a patient who had recently completed orthodontics. However, the ceramist and treating dentist believed a more conservative approach was the most beneficial. Also, the central incisors had beautiful translucencies that would be challenging to match, but the authors thought they could achieve excellent results.
Her previous dentist provided no follow-up during the orthodontic treatment. The previous orthodontist and dentist had not communicated about the esthetics and functionality in the final treatment goal, which should have been addressed while she was undergoing orthodontic treatment. Consequently, a lack of canine guidance occurred. This made the future stability of the occlusion questionable and in need of attention.
Using Invisalign treatment, the authors planned to close the diastema between Nos. 8 and 9 and leave equal spaces around the lateral incisors. This would have resulted in lateral incisors that were slightly wider than ideal. Managing the ceramics for proper shapes, line angles, and embrasures to achieve natural esthetics was expected to be a challenge.
Treatment Goals
1. Move maxillary anterior teeth using Invisalign braces to close the diastema between Nos. 8 and 9, equalize space around lateral incisors, and bring teeth Nos. 6 and 11 into the guidance position.
2. Provide tissue augmentation for tooth No. 7 to create gingival harmony.
3. Provide natural, esthetic veneers on teeth Nos. 7 and 10 using conservative preparations.
4. Equilibrate to provide a more stable, long-term occlusion.
5. Provide treatment that addresses the risk factors involved and try to decrease the risks whenever possible.
Treatment Plan
The challenge was whether conservative treatment would provide the esthetic result desired by both the patient and clinicians. The evaluation began with taking the proper diagnostic photographs and records. Maxillary and mandibular alginates were taken and transferred to the articulator using a Kois Dento-Facial Analyzer.
Through the use of photographs and mounted casts, the authors were able to take the proper steps toward determining the appropriate treatment. The full-face smile and close-up “E” position and rest position helped determine facially generated tooth positions (Figure 6). The maxillary incisal edge was in an acceptable position (Figure 7), and no alteration was planned except for closing the 1-mm diastema. Tooth No. 7 needed lengthening by approximately 1.5 mm and the diastema closed. Tooth No. 10 required lengthening of 0.5 mm to 1.0 mm and the diastema closed. For teeth Nos. 6 and 11, the incisal edges were in an acceptable position. However, the teeth had a slight buccal flare, removing them from guidance positions. The maxillary posterior occlusal plane was acceptable and no alteration was planned. The mandibular incisal edge position and posterior occlusal plane were in acceptable positions and no alterations were planned.
After determining the end point, the dentist must choose the appropriate treatment to achieve optimum esthetic results while minimizing the risks to the dentition. While evaluating the space with the ceramist, it was determined that moving the teeth orthodontically, combined with tissue augmentation on tooth No. 7, would provide an acceptable esthetic result. The space left after the tooth movement would be wider than ideal; however, the ceramist was confident that manipulating shapes, line angles, and incisal embrasures would achieve optimal results. In the authors’ opinion, one of the best uses for a treatment such as Invisalign is to move teeth into proper position preprosthetically. This provides a conservative and successful approach to anterior esthetics while maintaining low biomechanical risks. The treatment options were presented to the patient with respective limitations, expected outcomes, and approximated time frames.
Phase I: Deprogrammer
Prior to Invisalign treatment, the patient was placed in a Kois Deprogrammer to evaluate the occlusion. This was used only for diagnostic purposes to approximate the movement needed by the anterior teeth, in particular Nos. 6 and 11. The patient was placed in the deprogrammer for 3 weeks, returning weekly for evaluation and adjustment of the platform. A centric relation (CR) bite was taken with the deprogrammer in the mouth. It was mounted on a Panadent articulator (Panadent), and the first tooth contact was verified with what was consistent in the mouth. This was the buccal cusp of tooth No. 21. A trial equilibration was completed on the mounted casts, resulting in equal posterior contacts and light contact on tooth No. 6. There was no contact on tooth No. 11. At this juncture, the original orthodontic treatment had been approximately 5 to 6 months earlier. The patient’s CR and maximum intercuspation positions were very close. It was determined that a slight reduction of the buccal flare of the canines would bring them into proper guidance positions.
Phase II: Invisalign
Invisalign records were taken and sent to the manufacturer with specific instructions on tooth movement. The ClinCheck (Align Technology) was received and manipulated for the desired result. Movement was completed on the maxillary anterior teeth only. The patient visited biweekly for changes of the aligners and evaluation. The authors achieved the desired tooth movement within 5 months of treatment (Figure 8). At this time, new alginate impressions were taken and transferred to a Panadent articulator with a Kois Dento-Facial Analyzer System. A diagnostic wax-up was completed (Figure 9), and a putty index was created to transfer the wax-up to the patient’s mouth. A bisacrylic material was used for the transfer. The esthetics were verified, and the patient was happy with the results (Figure 10). With esthetics verified and teeth Nos. 6 and 11 in a more favorable functional position, Invisalign treatment was complete.
Phase III: Surgical
The periodontist performed tissue augmentation, employing a flapless technique with a scalpel for the gingivectomy and a small bone chisel for alterations in the bony architecture. This technique reduced the patient’s postoperative discomfort and reduced healing time. No sutures were involved, and the results were excellent and predictable. The patient had little discomfort after the procedure (Figure 11).
Phase IV: Equilibration
The patient was given a Kois Deprogrammer for approximately 3 weeks. She was instructed on the use of the appliance and followed weekly for adjustments. The first tooth contact stayed on the buccal cusp of tooth No. 21. With the appliance in the patient’s mouth, equilibration was completed. There were equal simultaneous point contacts from the canines to the posterior teeth. Function was checked to assure canine guidance. Like the trial equilibration prior to Invisalign treatment, the patient’s CR position was very close to MIP. At the time of the equilibration, the patient’s previous orthodontic treatment had ended 12 months earlier and Invisalign treatment had been completed approximately 2 months prior. Only the maxillary anterior teeth were moved during Invisalign treatment.
Phase V: Veneers
Prior to anesthesia, shade communication was performed, using photographs of multiple shade tabs (Figure 12). Several standard and ceramic-manufactured shade guides were used to document color, translucency, and effects. All guides were held in the same plane as the tooth to best communicate color and depth. This provided the authors with an accurate baseline. Teeth Nos. 7 and 10 were prepared with conservative veneers. Incisal and facial indices were used as a guide for proper reduction (Figure 13 and Figure 14). The indices were based on the accepted diagnostic wax-up that had been tried into the patient’s mouth. After tooth preparation, the teeth were rehydrated with a coating of glycerine and more shade photographs were taken of the prepared teeth for further communication.
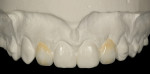
Temporary restorations were fabricated, using a putty matrix of the wax-up. The teeth were spot-etched to hold the bisacrylic temporaries. The impression was poured and mounted opposite the mandibular cast that was positioned against the diagnostic wax-up. The veneers were fabricated using a refractory veneer cast with a refractory veneer technique (Figure 15) and then finished to a solid tissue cast and etched with hydrofluoric acid. The veneers were returned for insertion at the subsequent visit. They were placed, using a translucent cement. The occlusion and function were checked for proper protection of the porcelain restorations. Impressions were taken for fabrication of orthodontic retainers. The retainers were inserted at the next visit, and the patient was instructed on their use.
Commentary
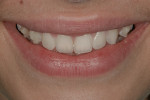
Sometimes in the search for optimal esthetics, dentists may forget that the most esthetic results can be based on the use of the natural dentition. The required time frame should not cause dentists to shy away from offering orthodontics as an option. Nature provides a certain beauty that dentists can approach but never duplicate. This patient’s natural dentition had such ideal shapes, shades, and translucencies that it would have been a disservice not to use this. By moving teeth into the proper position for conservative restorations, the authors were able to achieve a satisfactory esthetic result that was guided by what nature provided. The authors rendered treatment that addressed the desire for esthetics and supplied the patient with a long-term, stable result that reduced the risk factors involved (Figure 16, Figure 17, Figure 18 and Figure 19).