In Complex Restorative Cases, Understanding the Patient’s Expectations is the First Step
Treating Dentist:
Michael T. Ricciardi, DDS
Private Practice, Staten Island, New York
Technician:
Peter Pizzi, MDT
Owner, Pizzi Dental Studio Inc, Staten Island, New York
Background
Age at Initial Presentation: 51
Initial Presentation: August 22, 2007
Active Treatment Completed: October 4, 2008
Medical History
The patient had no contributory medical history and took no medications.
Dental History
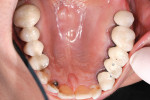
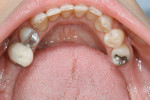
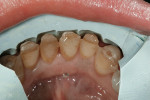
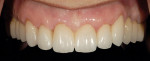
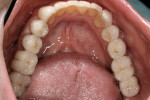
The patient’s dental history was extensive and consisted of multiple extractions (teeth Nos. 1, 3, 4, 12, 15 to 19, and 30 to 32). The patient reported most of these extractions occurred at least 20 years ago. She had a fixed bridge from teeth Nos. 2 to 5 and another from Nos. 11 to 14 with a cantilever on No. 15 (Figure 1). A distal occlusal amalgam was on No. 20, a mesial-occlusal-distal (MOD) amalgam on No. 28, and a porcelain-fused-to-metal (PFM) crown on tooth No. 29 (Figure 2). Teeth Nos. 23 to 26 had mild horizontal bone loss; teeth Nos. 8 and 9 presented with moderate bone loss and were in fremitus. On full-mouth probing, no notable pocketing was observed.
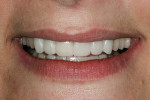
The patient presented with a concern regarding the esthetics of her anterior teeth, in particular, the way tooth No. 11 looked “high up” in comparison to the other anterior teeth. She also complained about the color and shape of her maxillary and mandibular teeth. Another concern was missing mandibular teeth and inability to properly clean under her maxillary posterior bridgework. She stressed she wanted to be able to floss between each tooth.
Diagnostic Findings
Temporomandibular Joints: Right and left areas tested normal to loading, with no discomfort. When evaluated, the patient had no clicking, popping, or crepitus, and she claimed no history of joint noises. There was no deviation on opening or closing. She had a normal range of motion on opening and had left and right lateral excursions.
Extraoral: Normal.
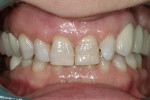
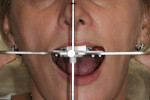
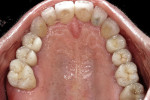
Intraoral: All soft tissue was normal and healthy. The patient presented with mild buccal recession on teeth Nos. 6, 8, 20 to 22, and 27; mild attrition on teeth Nos. 20 to 23, 26, and 27; and moderate attrition on teeth Nos. 24 and 25. Erosion was observed on incisal edges of teeth Nos. 22, 24, 26, and 27 and the buccal cusp tip of No. 28. Slight erosion was also on the incisal edge of tooth No. 9. During periodontal probing, no notable pocket depths were seen. Teeth Nos. 8 and 9 were in fremitus and exhibited +1 degree of mobility (Figure 3).
Occlusal Notes
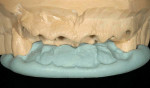
The patient presented with mild-to-moderate wear on the mandibular teeth and a steep anterior guidance causing fremitus in teeth Nos. 8 and 9, with some loss of attachment. Because restoration of the patient’s posterior teeth was planned, it was decided that the occlusal treatment would involve opening the occlusal vertical dimension (OVD) and making occlusal adjustment with a Kois deprogrammer to make the guidance shallower and to reduce forces on the anterior maxillary and mandibular incisors (Figure 4).
Radiographic Assessment
The patient was missing teeth Nos. 1, 3, 4, 12, 15 to 19, and 30 to 32. She had mild-to-moderate bone loss on maxillary anterior teeth Nos. 7 to 10 and mandibular anterior teeth Nos. 23 to 26. Tooth No. 8 showed a mesial vertical bony defect. Decay was present on the mesial of tooth No. 7. No pulpal pathology was noted.
Diagnosis
Periodontal: AAP Type III. This was based on the moderate (2 mm to 4 mm) horizontal pattern of bone loss in maxillary and mandibular anterior teeth. This diagnosis was based on the moderate bone loss observed in the maxillary anterior teeth. Mild horizontal bone loss in the anterior teeth was noted.
Biomechanical: The patient presented with one carious lesion on tooth No. 7 and a large MOD amalgam that structurally compromised tooth No. 28. Tooth No. 29 had a defective crown that needed replacement.
Functional: Occlusal dysfunction.
Risk Assessment
Dentofacial: High risk. This risk assessment was based on the number of alterations planned and the patient’s initial expectations. During the diagnostic process, the patient was asked to bring historical photographs so the restorative team could assess the original facial architecture, tooth color, smile line, and other anatomic features. Instead, the patient presented a magazine cutout of a “model” smile—one that was white, bright, and youthful. The author thought it necessary to educate her about natural tooth contours and transitions of color and translucency with a focus on a more natural “age-appropriate” shade, along with treatment options to achieve more harmonious tissue. They also discussed tooth position and implant placement.
Periodontal: Moderate risk. Teeth Nos. 8 and 9 presented with moderate horizontal bone loss and teeth Nos. 23 to 26 presented with mild horizontal bone loss.
Biomechanical: Moderate risk. The patient presented with one carious lesion on tooth No. 7 and a large MOD amalgam that indicated a structural compromise to tooth No. 28. A defective crown on tooth No. 29 needed replacement.
Functional: Moderate risk. The patient presented with mild-to-moderate wear on the mandibular teeth and a steep anterior guidance causing fremitus in teeth Nos. 8 and 9 with some attachment loss.
Prognosis
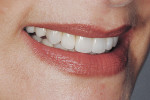
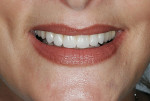
Dentofacial: Fair. The prognosis was based on an initial high-risk diagnosis and thorough patient education. Multiple conversations among the dentist, laboratory technician, and patient resulted in a more realistic vision. The medium maxillary and mandibular lip dynamics made it possible for a promising result because little gingiva would be exposed in a full smile (Figure 5).
Periodontal: Fair. The patient started a 3-month recall schedule after an initial scaling and root planing. The goal was to stabilize the AAP Type III moderate periodontitis.
Biomechanical: Good. After treating the one carious lesion and restoring the structurally compromised tooth No. 28 with a crown and replacing defective crown No. 29, it could be expected that the biomechanical risk would stabilize and the long-term prognosis would be good.
Functional: Good. The use of the Kois deprogrammer to open the OVD along with equilibration was expected to allow the anterior guidance. Canine guidance was achieved after equilibration and copied in the final restorations.
Concerns
The patient desired a short treatment period of 6 months in order to meet the date of her son’s wedding. Such a brief span can be a challenge if the restorative team is not in agreement.
The comprehensive case encompassed tissue augmentation to correct the gingival architecture. The authors told the patient that perfect harmony of the maxillary anterior gingiva could not be achieved without orthodontic extrusion and stabilization of tooth No. 11 (Figure 6).
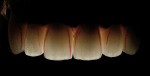
The use of a combination of PFM and all-ceramic (refractory) restorations (Figure 7), as well as the placement of implants to replace bridgework, created a laboratory concern in achieving harmonious esthetics with different materials.
Instead of giving the author historical photos to demonstrate her original smile, she provided a picture from a magazine, which portrayed her expectations. Thus, meeting the patient’s expectations was a concern.
Treatment Goals
1. Replace bridgework with implants and implant restorations.
2. Provide tissue augmentation to better harmonize the gingival architecture.
3. Provide natural and age-appropriate esthetics that exceeds the patient’s expectations.
4. Open the OVD to better control guidance.
5. Provide treatment that addresses the risk factors involved and try to decrease the dentofacial, periodontal, functional, and biomechanical risks.
Treatment plan
When undertaking such a comprehensive case, all professionals involved must have a precise understanding of the variables, a clear vision for the outcome independent of monetary outlay, and agreement on a starting point given all of the parameters. Usually, determining the maxillary incisal edge position is part of the first phase. Evaluating the dentofacial information also plays a critical role in gauging whether the expectations of the patient and dental team can be met.
Photography is key in helping ascertain maxillary incisal edge length. The ideal images are: 1) the rest position; 2) the close-up “E” position or smile shot (Figure 5); and 3) full-face “E” or smile shot. These photographs help determine if the maxillary incisal teeth need lengthening or shortening or if they are appropriately sized. For this patient, tooth No. 9 was in the correct position; No. 8 needed shortening to approximately 0.5 mm; tooth No. 7 required lengthening by 0.5 mm; and teeth Nos. 11 and 12 needed lengthening by 1.0 mm. The maxillary occlusal plane was noted as uneven and would benefit from lengthening to level it with the patient’s right side.
The mandibular lateral incisors and canines exhibited mild wear, and the mandibular central incisors showed moderate wear with compensatory eruption. Overall, the mandibular anterior teeth were in an acceptable position but required leveling. The mandibular posterior occlusal plane extended to the second bicuspid only and would benefit from lengthening on the right. Crown lengthening of the mandibular anterior teeth was proposed to create harmony in the tissue and to compensate for the lost tooth structure caused by the occlusal wear (Figure 3). To fulfill the patient’s wish for more harmonious gingival tissue in the maxillary anterior, the author told her that crown lengthening may help but would not achieve her expectations.
This preliminary case information was transferred to the laboratory with a Kois Dento-Facial Analyzer System (Panadent, https://www.panadent.com) and maxillary and mandibular alginate impressions with a bite registration, as well as a series of diagnostic photographs to facilitate communication. The technician’s role in these first diagnostic stages and discussions is crucial. The technician should be involved in the treatment planning in order to integrate the patient’s desires, the dentist’s vision, and the technician’s skill for a successful outcome.
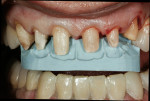
The full-mouth diagnostic wax-up was shown to the patient for a discussion and finalization of the treatment plan (Figure 8 and Figure 9). Also, the treatment limitations and the approximated time frame were discussed.
Phase I: Implant Placement
The patient was sent to the surgeon for consultation and subsequent placement of seven implants in tooth positions Nos. 4, 5, 12, 18, 19, 30, and 31. Surgical guides were used to ensure proper implant placement in the positions desired. Temporary bridges were placed prior to maxillary implant placement.
Phase II: Deprogrammer
Approximately 2 months before the implants were uncovered, the patient was fitted with a Kois deprogrammer to facilitate the bite opening. The deprogrammer platform was reduced to the approximate bite opening needed, and the patient was given instructions on the proper use of the appliance. She was checked weekly to evaluate the progress, and the platform was adjusted at each visit to ensure that she was hitting repeatedly on one small point of contact. After 4 weeks of deprogramming, the patient was ready for an adjustment of the bite opening. Because the platform was already reduced to the position of the desired opening, all that was needed was the addition of a composite on the posterior teeth, which was performed with the deprogrammer in the mouth. The contact was added to the first bicuspids successively, then the second bicuspids, and finally the canines. Then, the deprogrammer was removed and guidance checked to ensure canine guidance during function.
Phase III: Impressions
After the implants were uncovered, impressions were taken for the creation of custom abutments. Maxillary and mandibular posterior temporary bridges were fabricated at the new vertical dimension.
Phase IV: Surgical
Crown lengthening was completed for the mandibular anterior teeth and, at a subsequent appointment, for the maxillary anterior teeth (Figure 10). Tissue recontouring was incorporated into the diagnostic wax-up, which was a guide during the two surgeries. The patient was aware that after healing was completed, the tissue on canine No. 11 would remain apical in comparison to the adjacent tissue and opposite canine No. 6. The tissue architecture of tooth No. 10 was not altered, thus providing a reference for tissue and bony changes.
Phase V: Crowns
While the tissue was healing in the anterior region, the posterior teeth were restored with PFM butt-joint crowns on natural teeth Nos. 3, 12, 14, 20, 28, and 29 and PFM crowns on implants for teeth Nos. 4, 5, 13, 18, 19, 30, and 31. First, the posterior teeth were restored to ensure the opened vertical was maintained. At this point, new maxillary and mandibular alginates were taken and a second diagnostic wax-up was completed for the anterior teeth.
Phase VI: Completion
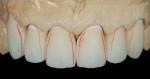
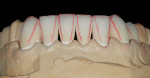
Approximately 6 to 8 weeks after surgery when the tissue was sufficiently healed, the anterior teeth were prepared using facial (Figure 11) and incisal preparatory guides (Figure 12) to aid in proper tooth reduction. Maxillary teeth Nos. 6 to 11 were prepared for all porcelain crowns (Figure 13), and teeth Nos. 21 to 27 were prepared for porcelain veneers (Figure 14). Temporary veneers and crowns were fabricated using putty matrices of the second diagnostic wax-up. The esthetics and incisal edge position were idealized in the temporary restorations (Figure 15) and transferred to the laboratory via an alginate impression and Kois Dento-Facial Analyzer (Figure 16).
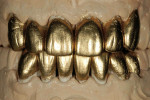
Permanent restorations were fabricated in the den tal laboratory using feldspathic porcelain and a refractory die technique (Figure 17). In dices from the models of the temporary restorations were used as a guide (Figure 18). The permanent restorations were returned and inserted in the subsequent visit. The veneers were placed using a transparent veneer cement. The PFM ceramic shoulders and full-porcelain restorations were placed using a translucent selfadhesive resin cement so as not to negatively influence the dental laboratory’s final ceramic color (Figure 19, Figure 20 and Figure 21).
Commentary
The comprehensive case encompassed tissue augmentation to correct the patient’s gingival architecture, and a combination of PFM and all-ceramic (refractory) restorations, as well as the placement of implants to replace bridgework. Much of the success in this case occurred because the restorative team exceeded the patient’s expectations. Her initial desire for a bright white “model smile” was discussed among the restorative team members. Although her final choice was “brighter” than her natural teeth, the patient and team chose a restoration that would be in the A1 shade (Figure 22 and Figure 23). The completion of treatment by her son’s wedding was not met due to the time constraints of surgical healing, a fact clearly defined to the patient at the treatment initiation. She attended the wedding functionally and esthetically comfortable with the provisional restorations in place. The most important aspect of any restorative treatment is to understand the limitations of the case, present these issues to the patient, and offer viable treatment options. A successful outcome is further ensured by follow-up discussions that clearly outline the treatment process and expected results. Educating the patient allowed the restorative team to give her an excellent outcome (Figure 24 and Figure 25).