Clinical Case Report: Testing Occlusal Management, Previewing Anterior Esthetics, and Staging Rehabilitation with Direct Composite and Kois Deprogrammer
Treating Dentist:
Jeff H. Bynum, DDS
Private Practice, Valrico, Florida
Background
Age at Initial Presentation: 41
Initial Presentation: November 2008
Active Treatment Completed: November 2009
Medical History
The patient presented with an unremarkable medical history. He was a healthy male taking no medications and had no medical contraindication.
Dental History
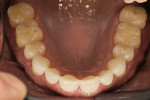
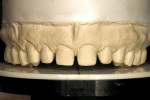
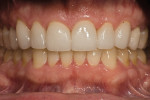
The patient presented with concerns about his smile esthetics and loss of tooth structure. He had noticed his maxillary anterior teeth becoming shorter and the development of erosive lesions on the occlusal, incisal, and cervical surfaces of many teeth. Orthodontic treatment had been performed twice with the latest treatment completed in 1996. He had no complaints related to headaches, muscle tension, or mastication. He had become frustrated with failed attempts to bond the edges of his anterior teeth. He desired the lengthening of his maxillary anterior teeth while minimizing the risks of “chipping” and fracture of any restoration that might be placed (Figure 1, Figure 2, Figure 3, Figure 4 and Figure 5).
Diagnostic Findings
Extraoral: Within normal limits. Cancer screening findings were negative.
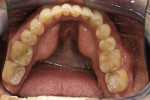
Intraoral: Bilateral mandibular lingual tori were approximately 22 mm x 8 mm (Figure 5). The patient also had bilateral maxillary and mandibular exostosis (Figure 3, Figure 4 and Figure 5).
Temporomandibular Joints: Maximal opening was 51 mm within normal range of movement, and no deviation on opening was observed. No joint sounds were noted. Findings from the load test were negative, as well as the results from the immobilization test.
Diagnosis
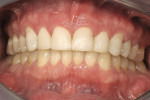
Periodontal: Mild chronic periodontitis, AAP Type II. Probing depths were within normal limits with no bleeding on probing. Bone support was within 2 mm of the cementoenamel junction without any infrabony defects. The gingival architecture was symmetrical (Figure 3).
Biomechanical: No caries was present; minimal erosion on the occlusal surfaces was observed on teeth Nos. 2, 7, 10 to 13, and 15. Moderate erosion on the occlusal surfaces on teeth Nos. 3, 4, 6, 8, 9, 14, 21, and 22 to 28 was noted. Severe erosion was observed on the occlusal surfaces of teeth Nos. 18 to 20 and 29 to 31. Minimal erosion/abrasion lesions were seen on the facial surfaces of teeth Nos. 6, 11, 13, 19 to 21, and 28 to 30. No pulpal pathology or structural compromises were observed (Figure 4 and Figure 5).
Functional: In the presence of such significant active erosion, distinguishing normal and abnormal functional attrition from erosion and friction from normal mastication becomes difficult. In most instances, the erosive component appeared to have outpaced the attrition, except for the moderate attrition on lingual/incisal surfaces of teeth Nos. 7 and 9, the minimal attrition on the facial/incisal surfaces of teeth Nos. 23 and 31, and moderate attrition on facial/incisal surfaces of tooth No. 25. An examination of postorthodontic models from 1996 revealed evidence of erosive lesions already formed in these areas and evidence of mild-to-moderate attrition presumably from the previous condition, leading to the conclusion that the erosion was a more significant and active component of tooth structure loss. No appreciable tooth mobility was evident (Figure 2, Figure 3, Figure 4 and Figure 5).
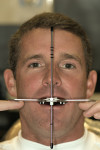
Dentofacial: Medium lip dynamics, normal scallop form, acceptable horizontal symmetry, and acceptable intra-arch tooth position. The maxillary incisal edge position relative to the face and lip position was deficient. Maxillary and mandibular posterior occlusal planes and mandibular incisal edge position were acceptable facially (Figure 2).
Risk Assessment
The risk assessment is determined by the collection of the data in the clinical examination and careful evaluation of the clues gathered from the medical and dental histories. Developing multiple treatment options for a given condition is possible. However, making an accurate diagnosis and determining an individualized risk assessment is important for ascertaining the most appropriate treatment plan for the patient’s needs and desires without unilaterally increasing the risk in that or another category.
Periodontal: Low risk because of slight bone loss and no shared risk factors for bone loss. The patient had resistance to periodontal disease (Figure 3).
Biomechanical: Moderate risk because of the amount of erosion. The patient had no history of carious lesions in adulthood, even in the presence of significant dietary acid consumption. The patient had caries resistance; the risk of caries increases as the enamel decreases in quantity and quality (Figure 4 and Figure 5).
Functional: Low risk because the patient presented with acceptable function. Previous wear, orthodontic treatment, and significant erosion hindered making the diagnosis; however, careful attention to the dental history and evaluation of historical photographs and models led to the understanding that the system was not actively degrading functionally. On the historical models, the attrition and erosion caused by the prior condition were clearly evident. However, based on this assessment, these conditions were determined to have remained stable for more than a decade and the system had not continued to degrade. The dental history revealed that the system had adapted to function effectively with this joint and tooth position without destruction.
Dentofacial: Moderate risk because of medium lip dynamics and incomplete tooth display in full smile. The amount of gingival display and, consequently, the risk increased as the treatment progressed, presumably as the patient became more confident with the appearance of his smile. Exceeding the patient’s expectations was expected to be more difficult. Therefore, the risk would increase as the patient displayed more tooth and gingival architecture. Restoration margin placement, shade matching to the surrounding tooth structure, and adaptation to the surrounding gingiva would require more careful attention as the amount of display increased (Figure 1 and Figure 2).
Concerns
1. How could the patient’s esthetic concerns be achieved without increasing the biomechanical risk? The author was concerned that reducing tooth structure for the restorative materials might lead to removal of tooth structure beyond what the patient may experience in a lifetime even without treatment and therefore increase the biomechanical risks.
2. How could the desired changes in tooth position be achieved without increasing the functional risk? Returning the length to the maxillary anterior teeth without managing the occlusal vertical dimension (OVD) would leave the restorations at risk for fracture and constrict the envelope of function. Of particular concern regarding changes to the tooth length was the contact position of the anterior teeth in centric relation (CR) position and maximum intercuspation (MIP). As determined from the dental history, previous adaptation had occurred to wear the anterior teeth sufficiently to allow the patient to function behind the envelope. Increasing the length of the anterior teeth without producing changes in the OVD would again constrict the envelope of function and raise the functional and biomechanical risk.
3. Which OVD would be the appropriate vertical dimension for this patient? How would this vertical dimension be established? How would this information be maintained throughout the treatment time and communicated accurately to the laboratory technician? Changing the OVD and finding the CR often appear to be shrouded in mystery for restorative dentistry, and communicating this information to the laboratory technician to achieve predictable results can be challenging.
4. How could these changes be managed while segmenting the treatment for time management and financial management? Dentists are often faced with the challenge of not being able to perform all of the treatment simultaneously due to constraints on the patient’s time and financial considerations. Finding a treatment modality that allows the treatment to be staged may make the difference in whether the patient proceeds with treatment. Segmented treatment in this case allowed the patient and treating dentist to preview the esthetics and perform a “trial-run” with the functional component.
Treatment Plan
Treatment options, risks, and goals were discussed with the patient. The patient’s primary objectives were to improve esthetics, manage the continued loss of tooth structure, and minimize the risk for future functional problems. Determining the appropriate size, shape, and length of the anterior teeth would help determine the amount of increase in OVD required to restore the anterior teeth with minimal preparation of both the anterior and posterior tooth structures. Phasing treatment into manageable pieces was also a concern for this patient. Doing this while maintaining the appropriate functional relationships allowed this plan to be completed comfortably even with time and financial restrictions.
Phase I: Transitional Bonding
Because the esthetic desires of the patient were a primary factor in the treatment, it was important to determine the acceptable and appropriate anterior tooth size, shape, and length. The maxillary incisors were lightly abraded with 27 µm of aluminous oxide particles with a PrepStart™, 0.015 tip (Danville Materials, https://www.danvillematerials.com) at 40 psi, etched with 37% phosphoric acid (ETCH-37™, Bisco Dental Products, https://www.bisco.com) for 15 secs, and bonded with an unfilled adhesive resin One-Step® Plus (Bisco Dental Products), and Filtek™ Supreme Plus (3M ESPE, https://www.3MESPE.com), according to the manufacturers’ instructions, to establish size parameters (Figure 6 and Figure 7). The patient approved this. A previously fabricated Kois deprogrammer was then used to establish CR position and the appropriate vertical dimension to allow clearance of the anterior teeth in the chewing envelope. Then, the maxillary canines, premolars, and first molar were built up to that vertical dimension, using the Kois deprogrammer as a guide, with the same bonding protocol as used on the anterior teeth to hold that vertical dimension with bilateral, equal-intensity, and simultaneous contacts. Posterior centric contacts were refined and verified (equilibrated) with TrollDental articulating foil (TrollDental, https://www.trolldental.com, AccuFilm II (Parkell, https://www.parkell.com), and shim stock occlusion foil 8 µm (Almore International, https://www.almore.com) (Figure 6, Figure 7, Figure 8 and Figure 9).
Phase II: Anterior Esthetics
The transitional bonding was allowed to remain in situ for 9 months. No evidence of chipping, cracking, or change in the occlusal relationship was noted after that time in full function. The joint stability did not change, and no new symptoms developed. The patient remained with acceptable function despite the changes in OVD and incisal edge position. At this time, it was appropriate to proceed with the definitive anterior esthetic treatment. Tooth preparation was designed to meet the teeth’s needs by replacing the missing tooth structure for esthetics and strength, not for the requirements of the restorative material. Otherwise, the traditional tooth preparation would have unnecessarily increased the amount of tooth reduction and increased the biomechanical risk. Anterior tooth reduction was limited to 0.3 mm from the facial enamel, maintaining the structural integrity of the teeth. The incisal preparation of 2 mm was almost completely in the transitional bonding (Figure 10). Almost no tooth structure was removed from the incisal edge, and only a small finish line was created on the lingual aspect, incisal to the cingulum, to allow the laboratory technician to create the appropriate occlusal stops on the canines Nos. 6 and 11 and achieve the proper lingual contours required to establish the chewing envelope. The entirety of the preparations was maintained in enamel and supragingivally; therefore, no retraction techniques were required or used for the impressions (Figure 11). Final impressions were made using a monophase, single-stage technique with medium consistency polyether (Impregum™ Penta™ 3M ESPE) according to the manufacturer’s recommendations. Provisional restorations for teeth Nos. 6 to 11 were made chairside directly with a Bis-acrylic composite temporary crown and bridge (Luxatemp®, DMG America, https://www.DMG-america.com). The Kois Dento-Facial Analyzer System (Panadent, https://www.panadent.com) was used to communicate essential functional and esthetic parameters for the mounting of the maxillary provisional cast (Figure 12). Jaw relation records were made in the MIP (which following the additive equilibration, was now coincident with the mandible in CR) using Jet Bite (Coltène Whaledent Inc, https://www.coltene.com). Records, casts, final impressions, and digital photographs were sent to the laboratory technician for the fabrication of the maxillary anterior restorations (Figure 13, Figure 14 and Figure 15). The platform on the articulator served as the natural head posture reference to ensure the symmetry of the incisal edge plane and horizontal and vertical tooth positions. Casts of the transitional bonding served as accurate guides for creating the incisal edge position. The Kois Dento-Facial Analyzer System allowed the preoperative models, transitional bonding models, and preparation models to be cross mounted precisely to ensure the accuracy and predictability of the final result (Figure 13, Figure 14 and Figure 15).
The restorations were luted, using the following adhesively retained protocol. The teeth were microabraded with 27 µm of aluminous oxide with a PrepStart at 40 psi, 0.015 tip. The teeth were etched with 37% phosphoric acid for 15 secs, and three layers of unfilled adhesive resin (One-Step, Bisco Dental Products) were applied and light-cured. The internals of the restorations were etched with hydrofluoric acid, cleaned, silanated (3M Primer, 3M ESPE), and thoroughly dried. All restorations were luted with a photo-activated resin (RelyX™ Veneer, 3M ESPE, shade translucent) and cured with a light-emitting diode light source.
Commentary
The Kois Deprogrammer enabled the treating dentist to diagnostically find the appropriate joint position, establish and maintain an acceptable VDO, equilibrate to the VDO additively, and consequently render phased treatment for the patient who would otherwise not be able to complete the treatment that he desired. Once the VDO was established, direct transitional bonding was created that would hold the joint position and allow for a “test drive” of the occlusal scheme and the esthetics using an inexpensive and easily repairable material. When the esthetics were approved and occlusion verified, the patient could then stage the treatment in a way that suited him, allowing him and the treating dentist to feel confident in the management of this patient’s condition, despite any delays in treatment phases.
The patient continues to have the composite bonding in the posterior region, maintaining the OVD along with the centric stops created on the canine restorations. This will continue until the patient is ready to proceed to the next phase of treatment. The patient is aware that the posterior direct restorations are integral to the success of the entire dentition and may need maintenance depending on the time that elapses before he completes the next phase of treatment. Having restored the CR and sustained an acceptable function, the dentist and patient have achieved some level of safety and consequently, the patient has not had any maintenance needs.
The final result exceeded the patient’s expectations (Figure 16, Figure 17 and Figure 18). The increase in tooth length, by restoring the incisal edge position, has created a natural, esthetic, and more youthful appearance. The high level of esthetics, form, and function achieved to meet the esthetic and functional demands of the patient could not be accomplished without the knowledge, experience, expertise, and artistry of the laboratory technician (Figure 13, Figure 14, Figure 15, Figure 16, Figure 17 and Figure 18). By thoroughly examining the patient’s risk factors and understanding the inherent risks associated with any treatment or no treatment, a plan was designed to minimize any additional risk to the entire dentition and not increase the functional risks at the same time. All the necessary tooth preparation was maintained in the enamel, which reduced the additional biomechanical risks. It could be argued that the biomechanical postoperative risks have decreased as the significantly previously eroded areas of enamel have been restored, covered, and protected from further erosive breakdown, although the patient is likely to continue the erosive dietary habits.
The tooth preparation margin location was also kept supragingivally, which did not contribute to any periodontal risks. The patient is on a 6-month schedule for maintenance, and the periodontal risk has remained low. Using the CR joint position and performing additive occlusal equilibration allowed the VDO to be increased without any increase in functional risk. The postoperative occlusal diagnosis is also in acceptable function. The only anticipated liability is the restorations (ie, chipped porcelain) and not the remaining teeth. The liability has been shifted from the teeth to the restoration.
Acknowledgment
The laboratory support and ceramics were supplied by Wayne Payne, Payne Dental Lab.