Piezocision: A Minimally Invasive, Periodontally Accelerated Orthodontic Tooth Movement Procedure
Abstract:
An increasing number of adult patients have been seeking orthodontic treatment, and a short treatment time has been a recurring request. To meet their expectations, a number of surgical techniques have been developed to accelerate orthodontic tooth movement. However, these have been found to be quite invasive, leading to low acceptance in patients and the dental community. The authors are introducing a new, minimally invasive procedure, combining microincisions with selective tunneling that allows for hard- or soft-tissue grafting and piezoelectric incisions. This novel approach is leading to short orthodontic treatment time, minimal discomfort, and great patient acceptance, as well as enhanced, or stronger, periodontium. Because of the added grafting (bone and/or soft tissue), the periodontium is much thicker buccally.
Significant acceleration in orthodontic tooth movement has been extensively reported following a combination of selective alveolar decortication and bone grafting surgery,1,2 with the latter being responsible for the increased scope of tooth movement and the long-term improvement of the periodontium.1,3-5 This conventional corticotomy approach consists of raising full-thickness flaps and using a bur to create cortical incisions (Figure 1). Then an allograft is placed at the sites needing the bone expansion necessary for proper orthodontic tooth movement. This intentional injury to the cortical bone results in a modification of the bone metabolism, leading to a transient state of osteopenia, described as rapid acceleratory phenomenon (RAP).6-8 RAP was demonstrated at the alveolar bone level following corticotomy and would be responsible for rapid tooth movement.9 Although quite effective, the trauma generated by the necessity to raise large flaps and the extensive nature of the corticotomies have met with some resistance in patients and the dental community. An alternative approach has been recently introduced by Park et al,10 consisting of incisions directly through the gingiva and bone using a combination of blades and a surgical mallet. While decreasing the surgical time (no flaps or sutures; only cortical incisions), this technique did not offer the benefits of bone grafting to increase periodontal support in the areas where expansive tooth movement was desired. In addition, the extensive hammering in office to perform the cortical incisions appears to certain patients to be somewhat aggressive. Moreover, dizziness and benign paroxysmal positional vertigo have been reported, following the use of the hammer and chisels in the maxilla.11
To achieve rapid orthodontic tooth movement without the downside of an extensive and traumatic surgical approach while maintaining the clinical benefit of a concomitant bone graft, the authors developed a minimally invasive procedure combining microincisions, minimal piezoelectric osseous cuts to the buccal cortex only, and bone or soft-tissue grafting concomitant with a tunnel approach.
Case Description
A 26-year-old Caucasian female presented to orthodontic consultation with the chief complaint: “I have an unpleasant smile.” She strongly expressed the demand for a rapid completion of her treatment, citing professional and personal reasons. Her dental history included regular dental visits, an endodontic treatment, and a porcelain fused to metal restoration on tooth No. 14.
Extraoral and Intraoral Examination
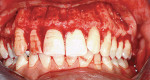
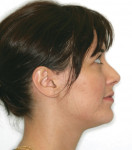
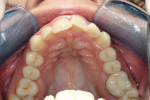
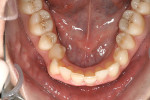
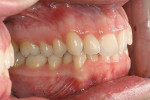
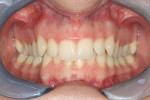
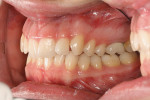
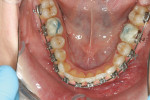
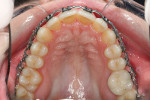
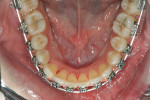
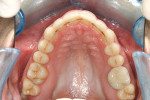
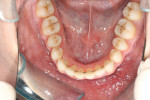
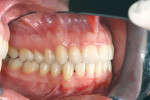
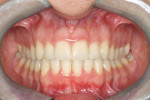
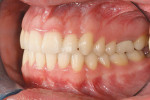
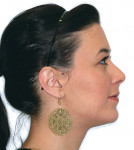
The patient showed a symmetrical face and a normal soft-tissue profile with normal vertical facial height (Figure 2A and Figure 2B). The temporomandibular joints were within normal limits. The lips were competent at rest with adequate vermillion display. When smiling, she exhibited 100% of maxillary incisal display, as well as 1 mm to 2 mm of gingival display. The mandibular dental midline was 2 mm to the right of the facial and maxillary dental midlines, while the maxillary dental midline was coincident with the facial midline. The maxillary and mandibular arch forms were U-shaped, and both presented 6 mm of crowding with few rotated teeth. Tooth No. 28 was lingually positioned (Figure 2C and Figure 2D). The curve of Spee was 3 mm, and the periodontium was healthy.
Dentally, she presented a class II division 2 relationship. (The canines had a 4-mm class II relationship on the right and a 2-mm on the left.) Teeth Nos. 5 and 28 were in cross-bite relationship. The overjet was 3 mm, and the overbite was 65% of lower incisor coverage (Figure 2E through Figure 2G).
From a skeletal standpoint, she had a class I pattern with slightly retruded maxilla and mandible and a normodivergent mandible.
Treatment Objectives
The goal of the treatment was to resolve the crowding in both arches, open the bite, and achieve a class I dental relationship that would be pleasing to the patient and decrease treatment duration. The patient was offered the conventional orthodontic treatment as well as an innovative treatment combining comprehensive orthodontic care with minimally invasive periodontal surgery (termed Piezocision) to accelerate tooth movement. In this procedure, a bone graft was also planned in the area where expansion was needed to expand the bony envelop in the direction of tooth movement and increase periodontal support to improve long-term stability in areas where relapse commonly occurs following orthodontic expansion.4,12 Because the patient sought a short treatment time, the orthodontic treatment coupled with Piezocision was chosen.
Surgical Technique
The surgery was performed 1 week following placement of the fixed orthodontic appliance (second premolar to second premolar brackets and molars bondable tube).
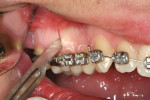
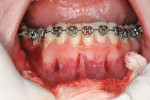
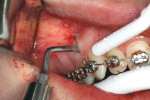
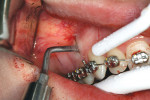
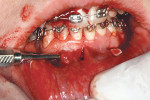
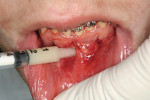
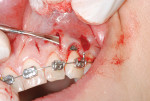
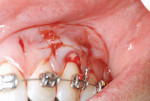
After local anesthesia, 10 vertical interproximal incisions were made, below the interdental papilla, on the buccal aspect of each jaw using a microsurgical blade or a blade No. 15 (Figure 3A). These incisions were kept minimal (microincisions) except when made in the areas of bone grafting (typically between the canines and laterals and between the centrals) (Figure 3B). The incisions went though the periosteum, which allowed the blade to reach he alveolar bone. A Piezo surgical knife (BS 1 insert, PiezotomeTM, Satelec Acteon Group, Merignac, France) was then used to create the cortical alveolar incision through the gingival micro-opening and to a depth of approximately 3 mm (Figure 3C and Figure 3D). When the corticotomies were finished, a small periosteal elevator was inserted in the surgical sites at the areas requiring bone or soft-tissue augmentation. These areas were typically located in the anterior regions where there was very little buccal bone, thin gingiva, or a gingival recession that needed correction. These locations were tunneled to create the necessary space to accommodate a bone or connective tissue graft (Figure 3E).
This tunneling is usually done through the vertical incisions situated between the canines and laterals and between the two central incisors. This is particularly useful for the correction of anterior crowding when the bony envelope needs to be expanded. This allows for a positive modification of the arch that will permit decrowding without extraction. Bone was grafted in the tunneled areas (Figure 3F), and the three vertical incisions between the canines were closed using a resorbable 5-0 suture. A few drops of medicalgrade cyanoacrylate glue could also be used in addition to the suturing (Figure 3G and Figure 3H). The posterior areas that had not been “tunneled” did not need suturing. The patient was sent home with prescriptions for an antibiotic and a non-steroidal antiinflammatory drug (NSAID) and was advised to rinse twice a day with chlorhexidine and use extraoral ice for the first 24 hours.
Treatment Progress
The patient reported using only two tablets of the NSAID after surgery. No swelling, bruising, or severe discomfort was associated with this procedure. The patient could resume oral physiotherapy 24 hours after the surgery. The periodontal healing was optimum with minimal to no scarring at 2 weeks.
It is of paramount importance for the orthodontist and surgeon to understand that the surgically induced high tissue turnover is restricted to the immediate proximity of the surgical cuts,13 creating what might be referred to as a localized spatio-temporal window of opportunity. Attention must be given to perform the bony incisions only around the teeth where tooth movement is planned. As such, the relative anchorage value of the teeth away from the surgical site remains high and anchorage value of teeth adjacent to the surgical site is low. Rapid acceleratory phenomenon6 (RAP) is transient, but continuous mechanical stimulation of the teeth would prolong the osteopenic effect induced by the procedure.14 Hence, it is imperative to see the patient and adjust the orthodontic appliance every 2 weeks.
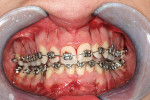
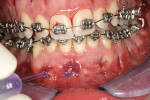
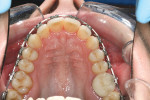
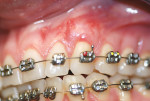
During the first 6 to 10 weeks of orthodontic treatment, both the maxillary and mandibular arches were fully leveled and aligned using increasing size of nickel titanium alloy wires (0.014, 0.016, 0.018, 0.016 x 0.022) (Figure 4A through Figure 4D). The class II dental relationship was then addressed using intermaxillary class II elastics 24 hours a day for 7 weeks on 0.016 x 0.022 stainless steel wires until full class I canine and molar relationship was achieved.
During the course of treatment, a sharp increase in tooth mobility was observed, resulting from the transient osteopenia induced by the surgery. Also important to emphasize is that higher forces are applied to the teeth as compared with conventional orthodontic treatment to maintain mechanical stimulation of the alveolar bone and the osteopenic state, allowing for rapid treatment.
Treatment Results
After 17 weeks of active treatment, the case was debanded and a fixed lingual retainer was inserted from canine to canine on both arches. A mandibular Hawley retainer was also given to the patient for night wear to prevent relapse of tooth No. 28.
The dental arches were fully leveled and aligned (Figure 4E and Figure 4F), class I relationship was achieved on both sides, the overjet was reduced to an ideal 1 mm, and the deep bite was improved from an initial 65% of lower incisor coverage to 8% post treatment (Figure 4G through Figure 4K).
Discussion
Rapid orthodontic tooth movement has recently been the focus of different research studies, with the rationale being that the shorter the overall treatment time, the fewer complications and the more compliant and satisfied the patient. Different approaches ave demonstrated enhanced rate of orthodontic tooth movement after such procedures as local injection of prostaglandins,15 local injection of 1,25 (OH)2 D3,16 local injection of osteocalcin,17 and alterations in alveolar calcium metabolism.18 These therapies are biochemical in nature and have been limited to the animal model. Surgical injury of the cortical bone adjacent to the area of desired tooth movement also has been reported to initiate biochemical changes leading to rapid tooth movement. Surgical injury to the alveolus induces a considerable amount of medullary bone demineralization immediately adjacent to the decortication site.13 This dramatic tissue turnover is expressed both spatially and temporally, and the mechanically induced transient osteopenia enables rapid tooth movement. The teeth move in a bone that has temporarily lost its original density but not its volume.9,19 Adding a bone graft to the technique has allowed for an increase in alveolar volume and enhancement of the existing periodontium.1,4,5 These physical modifications have proven to be beneficial in several ways: increased stability of the clinical outcomes12,20,21 (less orthodontic relapse), increased scope of malocclusion treatment22 (at times, avoiding orthognathic surgery), and reduced active orthodontic treatment time3,23 (by an average of 3-fold).
The initial corticotomies were performed using burs that could potentially damage the teeth (close root proximity) and bone (excessive heat) and could produce marginal osteonecrosis and impair bony regeneration.24 Piezoelectric incisions recently have been reported to be safe and effective in osseous surgeries, such as preprosthetic surgery, alveolar crest expansion, and sinus grafting.25 Because of ts micrometric and selective cut, the piezoelectric knife is said to lead to safe and precise osteotomies without any osteonecrosis damage.26 Furthermore, it works only on mineralized tissues, sparing soft tissues and their blood supply.27 Vercellotti later used it for periodontally accelerated orthodontic tooth movement.23 These authors were still using extensive periodontal flaps and incisions from a buccal and lingual approach, which has great clinical results but also means long hours and patient discomfort.
The technique being proposed here demonstrated similar clinical outcome when compared with the classic decortication approach but has the added advantages of being quick (decreased chairside time), minimally invasive, and less traumatic to the patient. It takes typically 1 hour to complete both arches vs 3 to 4 hours. This technique is quite versatile because it allows for soft-tissue grafting at the time of surgery to correct mucogingival defects if needed (Figure 5A through Figure 5C), as well as bone grafting in selected areas by using localized tunneling.
Conclusion
Piezocision is an innovative, minimally invasive technique to achieve rapid orthodontic tooth movement without the downside of the extensive and traumatic surgical approaches. This novel technique also allows the possibility for hard and/or soft-tissue augmentation, leading to an enhanced periodontium and an increased scope of tooth movement. Piezocision proves to be efficient from both the patients’ and clinicians’ standpoints and offers the advantages that should lead to greater acceptance in the dental community.
References
1. Wilcko WM, Ferguson DJ, Bouquot JE, et al. Rapid orthodontic decrowding with alveolar augmentation: case report. World J Orthod. 2003;4(3):197-205.
2. Sebaoun JD, Surmenian J, Fergusson JD, et al. Acceleration of orthodontic tooth movement following selective alveolar decortication: biological rationale and outcome of an innovative tissue engineering technique. International Orthodontic. 2008;6:235-249.
3. Ferguson DJ, Wilcko TM, Wilcko WM, et al. The contribution of periodontics to orthodontic therapy. In: Dibart S. Practical Advanced Periodontal Surgery. Hoboken, NJ: Wiley-Blackwell Publishing; 2007:23-50.
4. Wilcko WM, Wilcko TM, Bouquot JE, et al. Rapid orthodontics with alveolar reshaping: two case reports of decrowding. Int J Periodontics Restorative Dent. 2001:21(1):9-19.
5. Rothe LE, Bollen AM, Little RM, et al. Trabecular and cortical bone as risk factors for orthodontic relapse. Am J Orthod Dentofacial Orthop. 2006;130(4):476-484.
6. Frost HM. The regional acceleratory phenomena: a review. Henry Ford Hosp Med J. 1983:31(1):3-9.
7. Frost HM. The biology of fracture healing. An overview for clinicians. Part I. Clin Orthop Relat Res. 1989;248:283-293.
8. Frost HM. The biology of fracture healing. An overview for clinicians. Part II. Clin Orthop Relat Res. 1989;248:294-309.
9. Sebaoun JD, Kantarci A, Turner JW, et al. Modeling of trabecular bone and lamina dura following selective alveolar decortication in rats. J Periodontol. 2008;79(9):1679-1688.
10.Park YG, Kang SG, Kim SJ. Accelerated tooth movement by Corticision as an osseous orthodontic paradigm. Kinki Tokai Kyosei Shika Gakkai Gakujyutsu Taikai, Sokai. 2006;48:6.
11.Peñarrocha-Diago M, Rambla-Ferrer J, Perez V, et al. Benign paroxysmal vertigo secondary to placement of maxillary implants using the alveolar expansion technique with osteotomes: a study of 4 cases. Int J Oral Maxillofac Implants. 2008;23(1):129-132.
12.Skountrianos HS. Maxillary Arch Decrowding and Stability With and Without Corticotomy-Facilitated Orthodontics [master’s thesis]. St. Louis, MS: Saint Louis University; 2003.
13.Bogoch E, Gschwend N, Rahn B, et al. Healing of cancellous bone osteotomy in rabbits—part I: regulation of bone volume and the regional acceleratory phenomenon in normal bone. J Orthop Res. 1993;11(2):285-291.
14.Sebaoun JD. Trabecular Bone Modeling and RAP Following Selective Alveolar Decortications [master’s thesis]. Boston, MS: Boston University; 2005.
15.Yamasaki K, Miura F, Suda T. Prostaglandin as a mediator of bone resorption induced by experimental tooth movement in rats. J Dent Res. 1980;59(10):1635-1642.
16.Collins MK, Sinclair PM. The local use of vitamin D to increase the rate of orthodontic tooth movement. Am J Orthod Dentofacial Orthop. 1988;94(4):278-294.
17.Hashimoto F, Kobayashi Y, Mataki S, et al. Administration of osteocalcin accelerates orthodontic tooth movement induced by a closed coil spring in rats. Eur J Orthod. 2001;23(5):535-545.
18.Verna C, Dalstra M, Melsen B. The rate and the type of tooth movement is influenced by bone turnover in a rat model. Eur J Orthod. 2000;22(4):343-352.
19.Pham-Nguyen K. Micro-CT Analysis of Osteopenia Following Selective Alveolar Decortications and Tooth Movement [master’s thesis]. Boston, MA: Boston University; 2006.
20.Nazarov AD. Improved Retention Following Corticotomy Using ABO Objective Grading System [master’s thesis]. St. Louis, MS: Saint Louis University; 2003.
21. O’Hara P. Orthodontic Treatment and Retention Outcomes With or Without PAOO and Fixed Retainers [master’s thesis]. Boston, MA: Boston University.
22. Ferguson DJ, Wilcko WM, TM Wilcko. Selective alveolar decortications for rapid surgical orthodontic resolution of skeletal malocclusion. In: Bell WE, Guerrero CA, eds. Distraction Osteogenesis of the Facial Skeleton. Ontario, Canada: People’s Medical Publishing USA; 2006.
23. Vercellotti T, Podesta A. Orthodontic microsurgery: a new surgically guided technique for dental movement. Int J Periodontics Restorative Dent. 2007;27(4);325-331.
24. Kerawala CJ, Martin IC, Allan W, et al. The effects of operator technique and bur design on temperature during osseous preparation for osteosynthesis self-tapping screws. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999;88(2):145-150.
25.Vercellotti T. Piezoelectric surgery in implantology: a case report—a new piezoelectric ridge expansion technique. Int J Periodontics Restorative Dent. 2000;20(4):358-365.
26.Vercellotti T, Nevins ML, Kim DM, et al. Osseous response following respective therapy with piezosurgery. Int J Periodontics Restorative Dent. 2005;25(6):543-549.
27.Robiony M, Polini F, Costa F, et al. Piezoelectric bone cutting in multipiece maxillary osteotomies. J Oral Maxillofac Surg. 2004; 62(6):759-761.