Periodontal and Restorative Considerations with Clear Aligner Treatment to Establish a More Favorable Restorative Environment
Robert L. Boyd, DDS
Abstract
Although standard fixed appliances are better suited to control difficult tooth movement in three planes of space, clear aligner orthodontic treatment may be requested by patients because of the superior esthetics compared with conventional fixed appliances when clear aligners can be considered. Several clinical trials have shown improved periodontal status during orthodontic treatment with clear aligners while fixed appliances have almost always been associated with increased inflammation and mild periodontal breakdown despite preventive measures performed during treatment. There have been no reports of decalcification and only one reported case of root resorption with clear aligners, whereas with fixed appliances, numerous incidents of both decalcification and root resorption have been reported. In addition, studies have also shown significantly less pain from soft-tissue injuries and muscle soreness from parafunctional habits with computer-aided clear aligners. Restorative advantages include improved esthetics and comfort during treatment for better case acceptance and the ability to bleach teeth throughout treatment. Improving tooth alignment with orthodontic treatment with fixed or clear appliances increases the clinician’s potential capability to perform more conservative restorative procedures, requiring less tooth structure removal and less endodontic involvement because of better tooth positions. In those cases in which clear aligner appliances may be appropriate, less damage may occur to existing porcelain restorations than might transpire from bonding of fixed appliances and their removal, as well as potentially reduced tooth wear during treatment. This article presents three case reports that demonstrate the periodontal and restorative aspects of treatment using the computer-aided clear appliances, which have either eliminated the need for certain restorative procedures or created a better periodontal and tooth position environment for performing these procedures.
Computer-aided successive clear appliances were introduced at an annual orthodontic meeting in 1999 and first reported in the literature in 2000.1,2 (In this article, only the Invisalign® [Align Technology, Inc., Santa Clara, CA] appliance was employed.) Clear aligner appliances have been available for almost 50 years, with the earliest examples made from an individual tooth set-up with a single vacuum-formed appliance made from this appliance to the development of a series of computer-aided, consecutive tooth-moving appliances called Invisalign. Today these computer-aided appliances have been available to clinicians for almost a decade with more than 1 million patients who have received treatment worldwide.
For the first 5 years of use, several studies and case reports showed this appliance was somewhat effective for tipping movements, such as space closure, incisor rotations, and intrusive movements.2-15
Two of these earlier clear aligner longitudinal clinical studies demonstrated plaque control and periodontal health were improved during treatment.12,13 However, a recent systematic review of periodontal damage with fixed appliances indicated that, within the current body of controlled clinical studies in peer-reviewed journals, plaque accumulation and tissue inflammation increased during treatment and gingival recession and mild bone loss may occur in some adolescents (who generally have healthier periodontal tissues than adults).16 Another plaque-related problem commonly encountered in orthodontic treatment with fixed appliances is decalcification.17-19 To date, no studies or case reports of decalcification have been published regarding patients with clear aligners.
Subsequent case reports of clear aligner treatment could be effective for closure of mild-to-moderate open bite without increasing vertical dimension, which is contrary to the mandibular plane usually opening. This is typically seen with closure of open bite with fixed appliances.20-22 Successful correction of deep overbite and class II occlusion; prerestorative treatment to lessen the amount of tooth removal required in restorative dentistry and lower the necessity for endodontic procedures; rotations of canines and premolars; and extrusive movements were all shown to be effectively managed using new forms of composite attachments. Improved protocols for treatment were shown in these reports.20-23
Another likely benefit of clear aligner treatment is the apparent lower risk of root resorption, as only one recent case report has shown moderate root resorption.24 However, root resorption with fixed appliances is common, with an average of 1 mm for every millimeter of total apical displacement of the apex of upper incisors.25 Most studies have reported an average of more than 3-mm root resorption in 10% of patients receiving full-fixed appliances.26
Other recent studies found clear aligners could eliminate or minimize the effects of parafunctional habits that could lead to tooth wear and muscle soreness (myofascial pain). These studies further determined injury to soft tissues, such as lips, tongue, and the roof of mouth, were very minimal compared with fixed appliances.27,28
Significant limitations of clear aligners include the requirement of high patient compliance because the patient can remove the appliance, making treatment totally ineffective. Another significant limitation of tooth movement is bodily movement of roots, such as premolar extraction cases or orthodontic movement of impacted teeth.22 Premolar extraction cases can be done with aurilliaries, such as hooks29,30 or fixed appliances at some point in treatment to parallel the roots.3,22 Another limitation is in patients who are receiving orthognathic surgery and possibly requiring fixed appliances about the time of surgery, especially if multiple osteotomy segments are planned.31
This article presents three case reports that demonstrate the periodontal and restorative aspects of patients who received treatment using clear aligners, which either eliminated the need for certain restorative procedures or created a better environment for these procedures.
Case Reports
Case No. 1
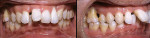
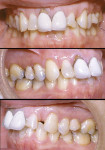
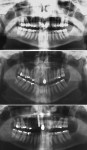
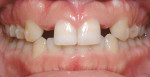
Case No. 1 (Figure 1) shows a 31-year-old male with a negative medical history. His chief complaint was that he “did not want to lose his front teeth.” He had received periodontal treatment previously but was told his upper and lower incisors and maxillary right first molar were hopeless and should be extracted. The initial restorative plan after extraction of these teeth was upper and lower ridge augmentations because of severe bone loss. This was followed by placement of restorative implants.
The examination revealed a severe class II, division I malocclusion with extreme deep overbite and 14 mm of overjet. The upper and lower incisors were excessively flared with spacing between the upper incisors. The profile was extremely convex, with incompetent lips. The patient had severe horizontal bone loss on all upper and lower incisors and a 9-mm pocket with vertical bone loss between No. 7 and No. 8 and 5 mm of root exposed on the distal of No. 8 from gingival recession.
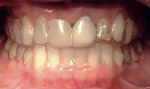
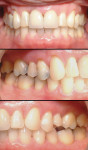
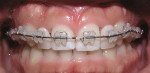
The patient accepted a treatment plan of reshaping and reducing the lengths of his upper and lower incisors, followed by alignment and improvement of the deep bite and large overjet (Figure 1, Figure 2, Figure 3 and Figure 4). Tooth No. 3 was extracted because of its hopeless periodontal prognosis. The patient realized the limitations of this treatment plan because the prognosis for these incisors was extremely guarded and ultimately he would likely lose these teeth. Space was created to intrude and retract the upper and lower incisors through intrusion, using the present space and performing crown-size reduction and interproximal reduction. Treatment time was 33 months, using an initial set of aligners followed by two case refinement series of aligners. The velocity of tooth movement was decreased from the usual 0.25 mm per stage to approximately 0.15 mm per stage by increasing the number of stages by 25% to minimize the applied forces and any increase in mobility of the anterior teeth. Attachments were placed on the first premolars for retention of the aligners.
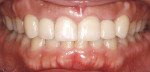
The posttreatment results show a large reduction in both the extreme deep bite and overjet, as well as reduction of the protrusion with lip competence achieved (Figure 5, Figure 6 and Figure 7). The patient was seen for periodontal maintenance at 3-month intervals throughout orthodontic treatment, with reports from his periodontist describing reasonable control of tissue inflammation and excellent plaque removal. Mobility improved in teeth either not being moved or moved only slightly and did not increase on the upper and lower incisors throughout treatment. He also had excellent compliance with aligner wear.
Because the long-term periodontal condition of the upper incisors was guarded, no immediate additional periodontal surgical procedures were done. Although a guided tissue-regeneration procedure was considered for the vertical defect between teeth No. 7 and No. 8, no action was taken because this was a wide, one-walled defect.
Retention was begun, with no additional bone loss. A connective-tissue graft from the palate was placed to improve the esthetics of the area of gingival recession on teeth Nos. 9 and 10. This procedure was done with excellent root coverage. Figure 8 shows the patient more than 4 years after active treatment.
The patient understood lifetime retention would be necessary. He continued to wear clear retainers at night for retention and to minimize the effects of parafunctional habits. No additional tooth wear was noted in the retention period. The patient is considering replacement of tooth No. 3 with an implant, which will require a sinus-lift procedure before placement.
Case No. 2
A 57-year-old female presented with a chief complaint of “spaced upper front teeth” with “spaces that were increasing” (Figure 9). The patient specifically requested that the treatment be done with clear aligners because she was concerned about esthetics with fixed appliances and she wanted more comfort. She had a negative medical history and was in periodontal maintenance for several years because of a previous diagnosis of early-to-moderate periodontitis. She had good oral hygiene and periodontal health and was negative for temporomandibular joint dysfunction and caries. She had been visiting her general dentist regularly and was considering an upper anterior crown to replace tooth No. 9, which had a crown and endodontics from several years earlier.
Her occlusion was class I, with a deep overbite and 8 mm of overjet. A posterior crossbite was present on the left side with tooth No. 13 completely buccal to the lower premolar. Tooth No. 13 also was rotated 180° with the smaller lingual cusp on the buccal. She had 2 mm of crowding on the lower arch and 4 mm of spacing on the upper arch.
The orthodontic treatment plan consisted of 29 months of clear aligner treatment to close all spaces, correct the overbite and overjet, and replace the crown on tooth No. 9 posttreatment. The patient provided excellent cooperation wearing appliances throughout treatment. No fixed appliances were needed because no movements required bodily tooth movements.
Unfortunately, the root of tooth No. 9 developed a vertical fracture and was extracted early in treatment. On the day of the extraction (Figure 10a and Figure 10b), the aligner was filled with a soft, tooth-colored resin at the position of tooth No. 9 to avoid an esthetic problem. This required changing the final restorative treatment plan to include the placement of an implant to replace tooth No. 9. A flipper was constructed with two circumferential clasps around the second molars and cut back from the first molars forward to allow tooth movement when the aligner was removed for eating to avoid an edentulous area (Figure 11). Fortunately, the initial computer-aided treatment plan allowed for the proper size and position of the crown for No. 9 posttreatment.
The implant to replace No. 9 was inserted when the final position of the upper incisors was attained in the last 8 months of treatment. This allowed for healing of the tissue around the implant while orthodontic treatment was being completed.
The final result shows that all goals were achieved. The only remaining problem was that tooth No. 13 had the smaller lingual surface facing buccally, which created the appearance of a smaller crown. Although it was recommended to the patient that she should at least have the buccal surface built up with composites, she declined; she was satisfied with the overall appearance and believed this tooth did not affect her smile.
As shown in 3-year posttreatment photos, excellent esthetics was maintained with good stability of the corrected occlusion because of nighttime wear of clear, removable clear retainers (Figure 12 and Figure 13). No noticeable tooth wear was observed.
Case No. 3
A 28-year-old female presented with the chief complaint of “spaces between her front teeth” (Figure 14 and Figure 15) but did not want fixed orthodontic appliances. The spaces were caused by congenitally missing maxillary lateral incisors. She had a class I occlusion with normal overbite and overjet, with slight crowding on the lower arch. The patient was negative for active periodontal disease and caries. She had a history of occasional myofacial pain related to stress and parafunctional habits. The treatment plan consisted of opening spaces for the lateral incisors, which would be replaced with restorative implants. The patient was told that because of the bodily movement required to parallel the canines and right central incisor, clear aligners could not perform all of this movement and a period of fixed appliances would be necessary for the completion of treatment.
Treatment time was 2 years, with good cooperation throughout treatment (Figure 16a, Figure 16b, Figure 16c and Figure 16d). After approximately 75% of the treatment was accomplished with clear aligners, fixed appliances using clear brackets on the upper arch only were used to complete treatment. The final result and x-ray showed good axial positions of the upper canines and central incisors (Figure 17). The implant was placed (Figure 18) with thin veneers on the upper canines and central incisors for a better overall match in tooth size, shape, and color with the implant crowns.
Retention was not needed for the upper arch but the lower arch, which was initially crowded, needed lifetime nighttime retention with a clear retainer to maintain stability and minimize further tooth wear (Figure 19). Also, patients are instructed to wear their retainers at other times when either myofascial pain returns or if certain daytime activities cause them to clench or grind their teeth.
Discussion
The most significant health benefit of clear aligner treatment is the reduced plaque accumulation that results in improved periodontal health. This is most likely because the patient is more conscientious about removing plaque from the inside of the aligners as a result of decreased clarity from plaque build-up and development of a detectable malodor.32 Two controlled clinical trials have shown this effect,12,13 which makes this benefit more certain because of the ranking of such evidence. A recent study showed fixed appliances, in the presence of active periodontitis, can accelerate periodontal breakdown beyond the level expected from the plaque retention of appliances only.33 Recent studies have shown several general health risks, such as diabetes mellitus, are associated with active periodontitis.34,35 Any appliance that improves periodontal status could be associated with improved overall health.
The presence of severe periodontitis is usually considered a contraindication for receiving orthodontic treatment with fixed appliances.36,37 However, the first patient presented in this report shows even someone with severe periodontitis can be successfully treated with clear aligners with no further progression of periodontal breakdown, provided initial control of active inflammation is achieved and patient compliance with plaque removal and periodontal maintenance is optimum.
Clear appliances also have a unique feature in their ability to move teeth with minimal increases in tooth mobility.32 Mobility can be minimized by reducing the amount of movement per stage (which increases the number of stages) and decreasing the applied force. Mobility also can be reduced by splinting the mobile teeth that are not moving. The teeth that were quite mobile, such as the incisors in Case No. 1, were programmed to receive reduced velocities, which lessened the forces that would cause mobility to increase. This is important for teeth with severely compromised crown-to-root ratios as in Case No. 1 because even light forces can lead to significantly increased mobility.
In all three patients, the long-term follow-up photos and clinical examinations showed no obvious additional wear was detected on the occlusal surfaces or incisal edges of any of the teeth throughout the retention period. No reports of discomfort from appliances or myofascial pain were reported by any of the patients during the entire treatment. The probable reason for the lack of muscle soreness is a disclusion of the teeth because of the smooth plastic material between them. This is similar to other types of splints used for relieving the effects of parafunctional habits, such as clenching and grinding.
In Case No. 2, the posterior crossbite correction was facilitated by the disclusion effect of the appliance and because in the computer-treatment plan tooth No. 13 was initially intruded. This was so that when the lingual cusp (actually the buccal cusp because of the 180° rotation of this tooth) passed over the lower buccal cusp, there was no opposing tooth contact, which would have likely increased trauma and mobility if crossbite elastics had been used. These elastics generally cause teeth being moved to extrude, which would likely increase the traumatic occlusion and potentially add to muscle soreness and mobility because of the increased premature occlusal contacts.
The third case shows one of the primary limitations of computer-aided clear appliances, which is to accomplish significant bodily movement of teeth. In this case, fixed appliances were required to complete treatment of parallel roots adjacent to the implant sites. However, patients will frequently accept orthodontic treatment if most is done with clear aligners and use of fixed appliances is restricted to a smaller portion of the treatment.31
Conclusion
The three cases demonstrate how computer-aided clear aligner appliance systems can be integrated with periodontal and restorative dentistry to obtain better results than if no orthodontic treatment had been performed. These case reports also demonstrate the advantages and disadvantages of computer-aided clear aligner treatment when compared with fixed-appliance treatment. The advantages include reduced plaque accumulation leading to healthier periodontal tissues and less caries, less increase in tooth mobility because of the ability to reduce the velocity of tooth movements (which lowers the forces applied and splinting of teeth not moving), less chance for tooth wear, extremely rare root resorption, potentially more effective correction and stability of mild open-bite correction, less soft-tissue irritation and myofascial pain, easier periodontal maintenance, bleaching of teeth throughout treatment, and better patient acceptance for treatment based on improved esthetics and comfort during treatment. This greater acceptance of the orthodontic treatment by the patients in this report with clear aligners compared with fixed appliances provided an opportunity for creating an improved restorative environment that would lead to less tooth reduction, a much lower probability for endodontic treatment, and fewer compromised teeth positions that would adversely affect the final esthetic restorative results.
Acknowledgment
The author wishes to acknowledge the help of Dr. Joorok Park in the preparation of the photos for this article, Dr. Kurt Pasquinelli for the periodontal treatment of Case 1, and Dr. Joel White for the restorative treatment for Case 2.
Disclosure
The author is a stockholder of Align Technology and serves on its Clinical Advisory Board.
References
1. Boyd RL. 1999 John Valentine Mershon Lecture. Presented at: Annual Meeting of the American Association of Orthodontists. 1999; San Diego, CA.
2. Boyd RL, Miller RJ, Vlaskalic V. The Invisalign system in adult orthodontics: mild crowding and space closure cases. J Clin Orthod. 2000;34(4):203–212.
3. Boyd RL, Vlaskalic V. Three-dimensional diagnosis and orthodontic treatment of complex malocclusions with the Invisalign appliance. Semin Orthod. 2001;7: 274–293.
4. Vlaskalic V, Boyd RL. Orthodontic treatment of a mildly crowded malocclusion using the Invisalign System. Aust Orthod J. 2001;17:41–46.
5. Vlaskalic V, Boyd RL. Clinical evolution of the Invisalign appliance. J Calif Dent Assoc. 2002;30(10):769-776.
6. Chenin D, Trosien AH, Fong PF, et al. Orthodontic treatment with a series of removable appliances. J Am Dent Assoc. 2003;134(9):1232-1239.
7. Womack WR, Ahn JH, Ammari Z, et al. A new approach to correction of crowding. Am J Orthod Dentofacial Orthop. 2002;133(3):310-316.
8. Wong BH. Invisalign A to Z. Am J Orthod Dentofacial Orthop. 2002;121(5):540-541.
9. Millera RJ, Derakhshan M. The Invisalign System: case report of a patient with deep bite, upper incisor flaring, and severe curve of spee. Semin Orthod. 2002;8(1):43-50.
10. Lagravère MO, Flores-Mir C. The treatment effects of Invisalign orthodontic aligners: a systematic review. J Am Dent Assoc. 2005;136(12)1724-1729.
11. Bollen AM, Huang GJ, King G, et al. Activation time and material stiffness of sequential removable orthodontic appliances. Part I: ability to complete treatment. Am J Orthod Dentofacial Orthop. 2003;124(5):496-501.
12. Clements KM, Bollen AM, Huang G, et al. Activation time and material stiffness of sequential removable orthodontic appliances. Part 2: dental improvements. Am J Orthod Dentofacial Orthop. 2003;124(5): 502-508.
13. Taylor MG, McGorray SP, Durrett S, et al. Effect of Invisalign aligners on periodontal tissues [abstract]. J Dent Res. 2003;82(A):1483.
14. Djeu G, Shelton C, Maganzini A. Outcome assessment of Invisalign and traditional orthodontic treatment compared with the American Board of Orthodontics objective grading system. Am J Orthod Dentofacial Orthop. 2005;128(3): 292-298.
15. Norris RA, Brandt DJ, Crawford CH, et al. Restorative and Invisalign: a new approach. J Esthet Restor Dent. 2002;14(4):217-224.
16. Bollen AM, Cunha-Cruz J, Bakko DW, et al. The effects of orthodontic therapy on periodontal health: a systematic review of controlled evidence. J Am Dent Assoc. 2008;139(4):413-422.
17. Boyd RL. Two-year longitudinal study of a peroxide-fluoride rinse on decalcification in adolescent orthodontic patients. J Clin Dent. 1992;3(3):83-87.
18. Boyd, RL. Comparison of three self-applied topical fluoride preparations for control of decalcification. Angle Orthod. 1993;63(1):25-30.
19. Boyd RL, Rose CM. Effect of rotary electric toothbrush versus manual toothbrush on decalcification during orthodontic treatment. Am J Orthod Dentofacial Orthop. 1994;105(5): 450-456.
20. Boyd RL, Oh H, Fallah M, et al. An update on present and future considerations of aligners. J Calif Dent Assoc. 2006;34(10):793-805.
21. Boyd RL. Review of the diagnostic process. In: Tuncay O, ed. Clinical Considerations in Using the Invisalign System. Chicago, IL: Quintessence Publications; 2006:223-250.
22. Boyd RL. Complex orthodontic treatment using a new protocol for the Invisalign appliance. J Clin Orthod. 2007;41(9):525-547.
23. Boyd RL. Esthetic orthodontic treatment using the Invisalign appliance for moderate to complex maloclussions. J Dent Educ. 2008;72(8):948-967.
24. Brezniak N, Wasserstein A. Root resorption following treatment with aligners. Angle Orthod. 2008;78(6): 1119-1125.
25. Baumrind S, Korn EL, Boyd RL. Apical root resorption in orthodontically treated adults. Am J Orthod Dentofacial Orthop. 1996;110(3): 311-320.
26. Vlaskalic V, Boyd RL, Baumrind S. Etiology and sequelae of root resorption. Semin Orthod. 1998;4(2):124-131.
27. Nedwed R, Miethke RR. Motivation, acceptance, and problems of Invisalign patients. J Orofac Orthop. 2005; 66(2):162-173.
28. Miller KB, McGorray SP, Womack R, et al. A comparison of treatment impacts between Invisalign aligner and fixed appliance therapy during the first week of treatment. Am J Orthod Dentofacial Orthop. 2007;131(3):302.
29. Womack WR. Four-premolar extraction treatment with Invisalign. J Clin Orthod. 2006;40(8): 493-500.
30. Hönn M, Göz G. A premolar extraction case using the Invisalign system. J Orofac Orthop. 2006;5(5):385-394.
31. Boyd RL. Surgical-orthodontic treatment of two skeletal Class III patients with Invisalign and fixed appliances. J Clin Orthod. 2005;39(4):245-258.
32. Boyd, RL. Improving periodontal health through Invisalign treatment. Access. 2005:25-26.
33. Wennström, JL, Stokland BL, Nyman S, et al. Periodontal tissue response to orthodontic movement of teeth with infrabony pockets. Am J Orthod Dentofacacial Orthop. 1993;103(4):313-319.
34. Hein C. Scottsdale revisited: the role of dental practitioners in screening for undisclosed diabetes and the medical co-management of patients with diabetes or those at risk for diabetes. Compend Contin Educ Dent. 2008;29(9): 538-553.
35. Mealey BL, Rose LF. Diabetes mellitus and inflammatory periodontal diseases. Compend Contin Educ Dent. 2008;29(7):402-413.
36. Boyd RL, Leggott PJ, Quinn RS, et al. Periodontal implications of orthodontic treatment in adults with reduced or normal periodontal tissues versus those of adolescents. Am J Orthod Dentofacial Orthop. 1989;96(3):191-198.
37. Boyd RL, Baumrind S. Periodontal considerations in the use of bonds or bands on molars in adolescents and adults. Angle Orthod. 1992;62(2):117-126.
About the Author
Robert L. Boyd, DDS
Frederick T. West Professor and Chair
Department of Orthodontics
Arthur A. Dugoni School of Dentistry
University of the Pacific, San Francisco, California