A Multipronged Approach to Optimizing Anterior Implant Esthetics
Victor A. Martel, DMD*
When restoring teeth in the esthetic zone by using dental implants, the creation of a natural appearance is paramount. Achieving that goal requires attention to a number of factors. First and most obviously, osseointegration must be achieved.1 Beyond that, treatment planning for esthetic smile rejuvenation depends on both scientific and artistic principles.2-3 The gingiva facial to the restoration and the adjoining papillae are crucial esthetic elements. Assuming that the existing osseous and gingival architecture around the failing tooth is acceptable, preservation of the hard and soft-tissue contours should be the therapeutic goal. Immediate placement of implants followed by immediate provisionalization has been suggested as an effective tool for achieving this result.4-6 After soft-tissue maturation, the choice of material selected for the restoration also can affect the appearance of the final restoration significantly.
It was long assumed that crestal bone remodeling to the first implant thread was a natural consequence of all implant placement.1,7 However, increased understanding of some of the biomechanical sequelae of implant placement has led to a reconsideration of that assumption.8-10 Inflammatory reactions in the peri-implant soft tissues have been identified11 that appear to result from bacterial contamination at the implant-abutment junction on standard implant designs.12 Such designs position the abutment inflammatory cell infiltrate at the outer edge of the implant-abutment junction, in direct approximation to the crestal bone. Modifying that interface by using an abutment smaller in diameter than the implant platform shifts the perimeter of the implant-abutment junction inward toward the implant’s central axis. It has been theorized that such “medialized” designs also shift the inflammatory cell infiltrate inward, limiting crestal bone loss.10 Clinicians placing these “platform-switched” implants have reported significant reductions in peri-implant bone loss.8,13
The following case demonstrates a multipronged restorative approach to optimizing the esthetics of a patient for whom implants replaced bilaterally missing cuspids. The implants placed used a new surface technology to enhance osseointegration. The implant design also incorporated a platform-switching architecture to reduce crestal bone loss during formation of the biologic width and minimize soft-tissue recession. The patient’s occlusion also permitted immediate provisionalization of the implants, another step that aided in maintaining the gingival architecture.
CASE REPORT
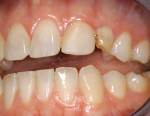
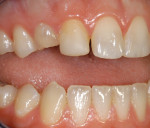
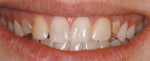
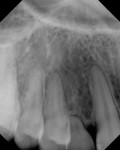
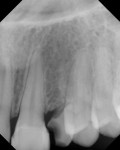
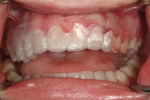
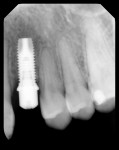
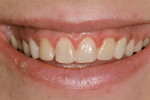
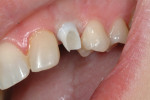
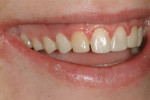
An 18-year-old woman presented with mobile maxillary primary cuspids (Figure 1 through Figure 3). Radiographs revealed bilaterally missing permanent cuspids with sufficient bone to enable placement of 11.5-mm dental implants (Figure 4 and Figure 5). The treatment plan called for placement of two NanoTiteTM PREVAIL® implants (Biomet 3i, Palm Beach Gardens, FL) in site Nos. 6 and 11, to be restored with ZiReal® posts (Biomet 3i) and allceramic crowns.
Materials
The PREVAIL implant configuration incorporates an integrated platform-switching design. The proven OSSEOTITE® surface (Biomet 3i) extends up to the area where the implant platform medialization begins. Numerous multicenter clinical evaluations have documented predictably increased contact osteogenesis, especially in poor-quality bone, associated with this surface treatment.14-21 The NanoTite PREVAIL implant surface builds on this principle by creating an even more complex calcium phosphate (CaP) surface topography on top of the OSSEOTITE surface.22
Traditionally, CaP has been plasma-sprayed on implant surfaces, resulting in a coating thickness ranging from 50 μm to 100 μm.23 However, such plasma-sprayed coatings have proven susceptible to delamination or dissolution of the amorphous content of the coating.23
The CaP on NanoTite implants is applied differently. According to the manufacturer, a patented wet-chemical synthesis process suspends ultrasmall particles of highly crystalline CaP in a solution, into which the dual acid-etched OSSEOTITE-surfaced implants are immersed. Discrete CaP crystals then are deposited on approximately 50% of the titanium oxide surface. According to the manufacturer (Biomet 3i), this discrete crystalline deposition (DCDTM) process results in crystal deposits of only 0.02-μm to 0.1-μm (20 nm to 100 nm) in size. The total amount of material on a NanoTite implant is so small that it weighs less than 20 μg. By contrast, the coating on a typical hydroxylapatite-coated implant has a thickness of 25 μm to 75 μm and weighs 20,000 μg—a one thousand-fold difference.24 In surface characterization studies, results have shown that DCD-treated implants had three orders of magnitude less CaP than plasma-sprayed implants had.25 However, the DCD process increases the implant microsurface by 200%.24 Moreover, the shear strength of the crystal attachment to the OSSEOTITE surface exceeds the minimum shear strength value of 34.5 Mpa set by ASTM standard F1609-03 for attachment of traditional hydroxyapatite coatings on implant surfaces.26 Human histologic studies have shown that the addition of the NanoTite surface topography to dual acid-etched titanium implants increases bone-to-implant contact substantially.27,28
The ZiReal posts planned for this case study are made of tetragonal zirconia polycrystals.29 Because of the translucency of the zirconia, ZiReal posts offer a more natural-looking result than that obtainable with titanium abutments. Furthermore, they incorporate a titanium interface that provides additional strength and reduces the potential for fretting, which may occur in all-ceramic abutments.29
Because the patient in this case was a student enrolled in a college located at some distance from her dental office, she was concerned about the possibility of losing a removable partial denture and not being able to immediately replace it. As her occlusion was an anterior open bite with no canine contact, immediate provisionalization after implant placement was proposed.
Treatment
The patient provided informed consent, and study models were created to fabricate a diagnostic waxup of both cuspids. The waxup was duplicated in a stone model, and two clear plastic matrices (Copyplast, Great Lakes Orthodontics, Ltd, Tonawanda, NY) were created on the stone model. One matrix was sent to the surgeon for use as a template during implant placement (Figure 6), while the second was retained for use in fabricating the temporary restorations.
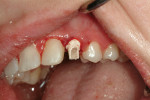
On the day of surgery, after administration of lidocaine 1:100,000, the surgeon extracted the two primary cuspids and created implant osteotomies in the extraction sites following the recommended manufacturer’s protocol. Preparation of the implant osteotomies began with a pointed starter drill (Advanced Cutting Technology® [ACT®], Biomet 3i). The pointed shape on the drill allowed for proper positioning of the osteotomies into the extraction sockets, directed along the palatal wall for proper alignment of the implants. Two 4/5/4-mm x 11.5-mm NanoTite PREVAIL implants (4-mm body, 4.8-mm expanded collar, 4.1-mm restorative platform) were placed in the osteotomies, and healing abutments were connected to them (Figure 7 and Figure 8).
Immediately after the surgery, the patient was seen in the restorative office. The healing abutments were removed, and PreFormance® posts (Biomet 3i) made of polyetheretherketone (PEEK), a biocompatible polymer,30 were selected for use as provisional abutments. These were seated into the internal interface of the implants; an audible click and tactile sensation confirmed that the seating was complete (Figure 9). The interim abutments were retained with GoldTite® abutment screws (Biomet 3i) tightened to 20 Ncm of torque. The abutments then were prepared intraorally to follow the gingival contours and allow for adequate interocclusal clearance and proper arch form.
The Copyplast matrix was filled with bisacryl provisional material and placed in the patient’s mouth over the interim abutments to create the provisional crowns. The crowns then were removed from the abutments, refined extraorally, returned to the mouth, and secured on the abutments with temporary cement (TempBond® ClearTM, Kerr Corp, Orange, CA) (Figure 10). The patient was given instructions for oral hygiene and directed to avoid biting into hard foods directly with her anterior teeth. No other dietary modification was necessary.
Restoration
The patient waited until her first school break to return for restorative treatment, approximately 4 months after implant placement. The surgeon found the implants to be successfully osseointegrated and, when the patient returned to the restorative dentist, the gingiva appeared to be pink and healthy, with no soft-tissue loss evident.
The provisional restorations were removed, and pick-up impression copings (Certain®, Biomet 3i) were placed. Verification radiographs confirmed that the impression copings were fully seated. A polyvinylsiloxane definitive impression was made, along with an impression of the opposing arch. A facebow and centric jaw relation records were made with polyvinylsiloxane material. These were sent to the laboratory, along with instructions to fabricate a softtissue model and prepare two ZiReal posts to 1 mm subgingivally, following the soft-tissue contours. The laboratory was directed to create two all-ceramic crowns (Procera®, Nobel Biocare USA, LLC, Yorba Linda, CA) custom-shaded to match the patient’s natural dentition (Figure 11).
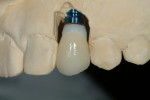
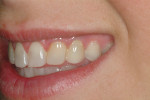
After 3 weeks, the patient returned, and the provisional restorations and abutments were removed. The two prepared ZiReal posts were seated (Figure 12). After the accuracy of the seating was verified radiographically, the abutments were secured with GoldTite screws tightened to 20 Ncm with a torque driver. Cotton pellets were placed over the screw-access openings, and these were sealed with composite resin (Fermit N, Ivoclar Vivadent, Inc, Amherst, NY), which then was light-cured. The Procera crowns were tried in and recontoured with porcelain polishing wheels (DialiteTM, Brasseler USA, Savannah, GA). The definitive crowns were cemented with TempBond Clear. Figure 13 and Figure 14 show the final restorations.
Conclusion
Creating optimal esthetics in the anterior maxilla requires attention to a number of factors. In this case, platform switching and an implant with an innovative surface treatment were used to enhance the implant stability and to prevent crestal bone loss, a prerequisite for maintenance of the soft tissue. The patient’s occlusion made it possible to place the implants, temporary abutments, and provisional restorations immediately after extraction of the cuspids, helping to maintain the gingival architecture during the healing period. The use of zirconia abutments and all-ceramic crowns for the final restorations was the final important element in achieving natural-looking tooth replacements.
Disclosure
The author is a consultant and lecturer for Biomet 3i, but did not receive any financial remuneration for authoring this article.
Acknowledment
Special thanks to surgical colleague Robert L. Holt, DMD, PhD, West Palm Beach, Florida.
References
1. Albrektsson T, Zarb G, Worthington P, et al. The long-term efficacy of currently used dental implants: a review and proposed criteria of success. Int J Oral Maxillofac Implants. 1986; 1(1):11-25.
2. Kois JC. Predictable single-tooth peri-implant esthetics: five diagnostic keys. Compend Contin Educ Dent. 2004;25(11): 895-907.
3. Davis NC. Smile design. Dent Clin North Am. 2007;51(2): 299-318.
4. Wöhrle PS. Single-tooth replacement in the aesthetic zone with immediate provisionalization: fourteen consecutive case reports. Pract Periodontics Aesthet Dent. 1998;10(9): 1107-1116.
5. Saadoun AP. Immediate implant placement and temporization in extraction and healing sites. Compend Contin Educ Dent. 2002;23(4):309-318.
6. Ericsson I, Nilson H, Lindh T, et al. Immediate functional loading of Brånemark single tooth implants. An 18 months’ clinical pilot follow-up study. Clin Oral Implants Res. 2000; 11(1):26-33.
7. Smith DE, Zarb GA. Criteria for success of osseointegrated endosseous implants. J Prosthet Dent. 1989;62(5):567-572.
8. Vela-Nebot X, Rodríguez-Ciurana X, Rodado-Alonso C, et al. Benefits of an implant platform modification technique to reduce crestal bone resorption. Implant Dent. 2006;15(3):313-3120.
9. Baumgarten H, Cochetto R, Testori T, et al. A new implant design for crestal bone preservation: initial observations and case report. Pract Proced Aesthet Dent. 2005;17(10):735-740.
10.Lazzara RJ, Porter SS. Platform switching: a new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent. 2006;26(1):9-17.
11.Ericsson I, Persson LG, Berglundh T, et al. Different types of inflammatory reactions in peri-implant soft tissues. J Clin Periodontol. 1995;22(3):255-261.
12.Berglundh T, Lindhe J, Marinello CP, et al. Soft tissue reactions to de novo plaque formation on implants and teeth. An experimental study in the dog. Clin Oral Implants Res. 1992; 3(1):1-8.
13.Calvo Guirado JL, Sáez Yuguero MR, Pardo Zamora G, et al. Immediate provisionalization on a new implant design for esthetic restoration and preserving crestal bone. Implant Dent. 2007;16(2):155-164.
14.Sullivan DY, Sherwood RL, Porter SS. Long-term performance of Osseotite implants: a 6-year clinical follow-up. Compend Contin Educ Dent. 2001;22(4):326-334.
15.Davarpanah M, Martinez H, Etienne D, et al. A prospective multicenter evaluation of 1,583 3i implants: 1 to 5-year data. Int J Oral Maxillofac Implants. 2002:17(6):820-828.
16.Feldman S, Boitel N, Weng D, et al. Five-year survival distributions of short-length (10 mm or less) machined-surfaced and Osseotite implants. Clin Implant Dent Relat Res. 2004;6(1): 16-23.
17.Sullivan D, Vincenzi G, Feldman S. Early loading of Osseotite implants 2 months after placement in the maxilla and mandible: a 5-year report. Int J Oral Maxillofac Implants. 2005; 20(6):905-912.
18.Stach RM, Kohles SS. A meta-analysis examining the clinical survivability of machined-surfaced and Osseotite implants in poor-quality bone. Implant Dent. 2003;12(1):87-96.
19.Testori T, Wiseman L, Woolfe S, et al. A prospective multicenter clinical study of the Osseotite implant: four-year interim report. Int J Oral Maxillofac Implants. 2001;16(2): 193-200.
20.Gaucher H, Bentley K, Roy S, et al. A multi-centre study of Osseotite implants supporting mandibular restorations: a 3-year report. J Can Dent Assoc. 2001;67(9):528-533.
21.TestoriT,DelFabbroM,FeldmanS,etal.A multicenterprospective evaluation of 2-months loaded Osseotite implants placed in the posterior jaws: 3-year follow-up results. Clin Oral Implants Res. 2002;13(2):154-161.
22.Nishimura I, Huang Y, Butz F, et al. Discrete deposition of hydroxyapatite nanoparticles on a titanium implant with predisposing substrate microtopography accelerated osseointegration. Nanotechnology. 2007;18(24):245101.
23.Ong JL, Chan DC. Hydroxyapatite and their use as coatings in dental implants: a review. Crit Rev Biomed Eng. 2000;28(5-6): 667-707.
24.Suttin Z, Gubbi P. Surface area increase due to discrete-crystalline-deposition of nanometer-scale CaP crystals. Presented at: European Association of Osseointegration 15th Annual Scientific Meeting; October 5-7, 2006; Zurich, Switzerland.
25.Pezeshki P, Lugowski S, Davies JE. Dissolution of discrete calcium phosphate crystals from candidate ti-based implant surfaces. Presented at: Society for Biomaterials 32nd Annual Meeting; April 2007; Chicago, IL.
26.Suttin Z, Gubbi P. Adhesion shear strength of nanometer scale CaP crystals applied by discrete crystalline deposition. Presented at: European Association of Osseointegration 15th Annual Scientific Meeting; October 2006; Zurich, Switzerland.
27.Orsini G, Piatelli M, Scarano A, et al. Randomized, controlled histologic and histomorphometric evaluation of implants with nanometer-scale calcium phosphate added to the dual acid-etched surfaced in the human posterior maxilla. J Periodontol. 2007;78(2):209-218.
28.Goené RJ, Testori T, Trisi P. Influence of a nanometer-scale surface enhancement on de novo bone formation on titanium implants: a histomorphometric study in human maxillae. Int J Periodontics Restorative Dent. 2007;27(3):211-219.
29.Brodbeck U. The ZiReal Post: a new ceramic implant abutment. J Esthetic Restor Dent. 2003;15(1):10-24.
30. Williams D. Polyetheretherketone for long-term implantable devices. Med Device Technol. 2008;19(1):8-11.