Re-treating Failed Posterior Amalgam Restorations
Microhybrid composite provides high-strength solution with one shade
Apolinar Madrigal, DDS | Oswaldo Aldaco, DDS
The US Centers for Disease Control and Prevention reported that an impressive percentage of the US population seeks yearly dental treatment, including 84.6% of those aged 2 to 17 years old, 64.4% of those aged 18 to 64 years old, and 64.3% of those aged 65 and older.1 By comparison, only 51% of American adults aged 18 to 64 visit their primary care physician each year.2 These statistics highlight the value that Americans place on oral health and the appearance of their smiles.
Oral healthcare professionals can better align their treatments with the esthetic goals of their patients by utilizing the latest in material developments, such as a microhybrid resin composite that can match the natural tooth structure coloration of any patient with a single shade. The following case report describes the re-treatment of two failed posterior amalgam restorations and outlines how a single-shade microhybrid resin composite solution was the ideal choice for the patient's treatment plan.
Case Report
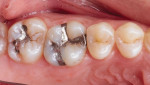
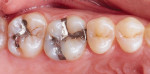
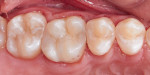
A 27-year-old male patient presented with failed amalgam restorations on teeth Nos. 14 and 15 that were 11 years old (Figure 1). The clinical examination revealed that tooth No. 14 had decay under the distal extension and that tooth No. 15 had broken near the lingual aspect and also exhibited the presence of decay.
Composite dental material fillings were recommended. It was explained to the patient that a light-cured microhybrid resin composite would not only provide a natural "tooth-colored" appearance but also deliver long-term strength and only require minimal preparation of the existing tooth structure.
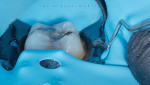
On the day of treatment, the patient was anesthetized using a computer-assisted single tooth anesthesia system (The Wand®, Milestone Scientific). A rubber dam and clamp (Hartzell Upper Molar Rubber Dam Clamp, DenMat) were placed to help achieve complete isolation and ensure a clean and dry working field (Figure 2).
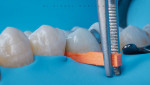
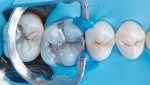
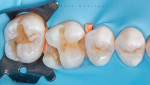
After the area was cleaned and a dental wedge was inserted to create space (Figure 3), a custom ring was created using a matrix ring (Matrix Rings, Garrison Dental Solutions) and block-out resin (LC Block-Out Resin, Ultradent Products, Inc.) (Figure 4). This would give shape to the emergence profile and improve efficiency during the latter stages of the case.
Next, the failed amalgam restorations and the existing decay on teeth Nos. 14 and 15 were removed, and the area was cleaned and prepared for the placement of the composite restorative material (Figure 5). The matrix bands were positioned, and the custom ring made from block-out resin was put into place, which formed the matrix bands to the emergence profile.
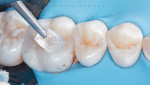
Once the teeth were cleaned and prepared, an etchant (Etch ‘N' Seal®, DenMat) was used to selectively etch all of the uncut enamel. This etchant, which is a special formulation of 25% phosphoric acid and 0.25% aluminum oxalate, etches and desensitizes enamel and dentin simultaneously to maximize bond strength while also protecting dentin from the possibility of over-etching. This step was completed only where bonding to enamel would occur because the bonding agent selected was a self-etch formulation that was able to stand on its own. The etchant was then rinsed away.
After selective etching, the self-etching bonding system (Tenure Uni-Bond®, DenMat) was mixed and applied to the tooth preparation. Next, a light-cured, low viscosity resin composite (Virtuoso® Flowable [shade A2], DenMat) was placed as a fluoride-reinforced base and liner. This composite features a bubble-free, self-leveling viscosity that helps ensure precise placement.
Finally, a light-cured microhybrid resin composite (Nuance® Universal, DenMat) was placed in three small and separate increments: right, left, and middle. This high-strength composite was selected because it can match a patient's natural dentition with a single shade, picking up coloration from the surrounding tooth structure to achieve optimal esthetics for the entire restoration. The material's malleable consistency and excellent handling facilitated ample time for shaping it into the desired, detailed tooth anatomy without any sticking to the composite instrument.
Once the composite had been placed and shaped, the material was light cured in 10- to 20-second increments (Flashlite Magna® 4.0, DenMat). The technique of applying the composite in small increments (ie, less than 2.0 mm), followed by thoughtful shaping of the material, eliminates the need for finishing burs (Figure 6). After curing, a surface penetrating sealant (Gloss 'N' Seal®, DenMat) was applied to the finished composite restorations to serve as a protective barrier to reduce composite wear, marginal staining, and restoration breakdown (Figure 7).
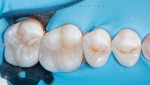
With the composite restorations on teeth Nos. 14 and 15 completed, the dental wedge, clamp, and rubber dam were removed. After verifying the fit and occlusion, the restorations were polished using a 2-step system (Footsie™ Composite Polishers, Komet USA). Once polished, the microhybrid resin composite material appears translucent at the incisal edges but also mimics dentin-like depth, providing multidimensional nuances similar to those of natural tooth structure (Figure 8 and Figure 9). The patient was thrilled with the final result.
Conclusion
The advent of tooth-colored composite restorations gave dentists the ability to deliver lifelike esthetics in any region of the mouth. However, the light-cured microhybrid resin composite used in this case offers multiple benefits, including multifaced fillers that pick up coloration from surrounding tooth structure to deliver lifelike esthetics with a single shade; exceptional handling because of the material's sculptable, nonstick consistency; and a unique composition that provides impressive strength, low shrinkage, and high polishability-all of which provide clinicians with the ability to deliver high-quality restorative care in an anticipatory, fail-proof manner.
References
1. US Centers for Disease Control and Prevention. Health, United States, 2017 - data finder. US Centers for Disease Control and Prevention website. https://www.cdc.gov/nchs/hus/contents2017.htm#078. Reviewed August 9, 2018. Accessed March 24, 2020.
2. US Centers for Disease Control and Prevention. Ambulatory care use and physician office visits. US Centers for Disease Control and Prevention website. https://www.cdc.gov/nchs/fastats/physician-visits.htm. Reviewed January 19, 2017. Accessed March 24, 2020.