Removing Foreign Bodies From the Maxillary Sinus: Sinus Area Classification and Technique Selection
Leon Chen, DMD, MS; and Jennifer Cha, DMD, MS
ABSTRACT
The displacement or invasion of a foreign object (eg, amalgam, dental bur, dental cement, dental implant) into the maxillary sinus can lead to various negative sequelae. Several techniques have been described for the removal of such objects, but although all of them require correct diagnosis and accurate determination of the exact size and location of the foreign object before the removal procedure is performed, high postoperative complication rates often result from these invasive procedures. The authors propose the categorization of two different types of maxillary sinus areas that can be invaded by dental implants and/or foreign objects; diagnosis and treatment are predicated on differentiating and/or identifying these two spaces. The clinical implications of these classifications include the ability to select from and execute appropriate and minimally invasive removal techniques, which are described and demonstrated in three presented case reports.
The maxillary sinus is a paranasal sinus space present in the anatomy of the maxilla. Considered to be the largest paranasal sinus, it is present at birth as rudimentary air cells and continues increasing in size throughout childhood until age 18.1 Throughout its growth and development, the maxillary sinus undergoes changes in vertical, horizontal, and antero-posterior directions.2 Aging and tooth loss during an individual's lifetime influence the maxillary sinus' ultimate dimensions, such as contours and total volume.3 For example, completely and partially edentulous individuals have less total maxillary sinus volume than non-edentulous people. Similarly, older people also have less maxillary sinus volume.3
Over the past 15 years or so, the dental literature has cited various cases involving foreign body displacement or invasion into the maxillary sinus, leading to a variety of negative sequelae (eg, chronic pain, fungal infections, sinusitis, dental treatment failure).4-6 These foreign objects range from amalgam and dental cement to dental burs and implants. Their invasion into the maxillary sinus typically results from inadvertent trauma from dental treatment.4,7-9
During or after implant treatment in particular, an implant may migrate into the upper paranasal sinus and adjacent structures, especially considering the anatomical variations of maxillary bone from one person to the next and the likely absence of sufficient bone height.5,10 When foreign objects migrate into the maxillary sinus, they essentially have perforated the sinus membrane (ie, Schneiderian membrane), the thinness and contours of which may predict the risk for perforation (ie, <1 mm, narrow and tapered contours).11 This is particularly relevant in cases involving sinus lifts12; however, even a thicker Schneiderian membrane (eg, 1.47 mm to 2.92 mm) may perforate under the significant elastic forces associated with sinus lifts and implant placement.12,13
Fortunately, research has demonstrated that cone-beam computed tomography (CBCT) can be a suitable and reliable method for determining the exact location of a foreign object in the maxillary sinus that otherwise might go undetected if panoramic or periapical radiographs are used.6,14 However, when a foreign object is present in the maxillary sinus, depending on its exact location and the type of sinus space it occupies, in some instances it may be mobile, and in other cases it may be immobile.
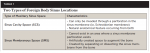
This is significant, because there are two different types of maxillary sinus areas that can be invaded by dental implants and/or foreign objects, and diagnosis and treatment are predicated on differentiating and/or identifying these two spaces.15 Because these two spaces have not been previously differentiated in the literature or classified in the dental anatomy, the authors introduce and explain two descriptive terms-"sinus cavity space" and "sinus membranous space"-that better identify these areas in the maxillary sinus that can be potentially invaded (Table 1).15-17 The authors further propose that by understanding the unique characteristics of these two areas when foreign object invasion occurs, clinicians can then execute one of two removal techniques, each of which is location dependent.
Sinus Cavity Space
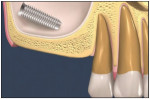
When an object has perforated the Schneiderian membrane and invaded the maxillary sinus, it is now located within the maxillary sinus cavity that is surrounded by the Schneiderian membrane (Figure 1). The authors refer to this area as sinus cavity space (SCS).15-17 The significance of recognizing and differentiating this space is that an extruded implant or invading object can reside in this space only if the Schneiderian membrane has been perforated, thereby providing passageway to this space.15-17 Foreign bodies located in this space are mobile and, therefore, may be removed according to the Chen modified Valsalva sinus clearance technique (described below).
Chen Modified Valsalva Sinus Clearance Technique
Commonly used to describe a forced expiratory effort against a closed airway, mouth, or glottis while in a sitting or supine position, the Valsalva maneuver has multiple diagnostic and clinical applications (eg, arrhythmia treatment) and application in daily life (eg, playing a musical instrument).18,19 In dentistry, the Valsalva maneuver is typically and frequently used during sinus lift procedures to indicate whether or not the sinus membrane has been perforated.
However, a version of the Valsalva maneuver as modified by the authors has application for implant and/or foreign object removal when the SCS has been invaded by enabling objects (eg, implants, dental materials) to be pushed closer to the opening for visibility and easier, less invasive retrieval. Usually when objects are suspected of invading the SCS, clinicians may direct patients to stand and hop up and down to shake the object toward the opening, which is unpredictable and awkward for patients.
According to the Chen modified Valsalva sinus clearance technique, the patient sits upright and slightly forward, using the tongue to close the sinus opening while deeply inhaling. This prevents air from pushing the object further back into the sinus space. When ready, the patient is instructed to exert a forceful expiratory effort and release the tongue from the opening while pinching the nose. This maneuver is repeated five times, after which the clinician verifies that the object is visible through the opening; alternatively, a radiograph is taken while the patient remains in an upright position, which should prevent the object from dropping further back into the sinus.
Note that the Chen modified Valsalva sinus clearance technique is appropriate only when an implant or foreign body has invaded the SCS, since the object is mobile only in this location.
Sinus Membranous Space
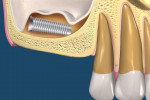
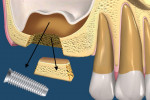
The authors refer to the second space in the maxillary sinus into which a dental implant or foreign object could potentially invade as sinus membranous space (SMS). This term specifically describes the space between the lining of an elevated Schneiderian membrane and the bony maxillary sinus surface (Figure 2). Normally non-existent, this space is only created either by separating the sinus membrane during a surgical procedure or by an endodontic lesion in maxillary teeth; this may explain why it previously has not been described in the literature.15-17
Because objects located in this area are immobile, removal according to the Chen modified Valsalva sinus clearance technique is inappropriate. Over the years, however, a variety of techniques have been described to remove foreign objects from the maxillary sinus, including bone flap, Caldwell-Luc, extraction through the original osteotomy site, transnasal endoscopy, and others.7,16,17,20 These approaches all require correct diagnosis as well as determination of the exact size and location of the foreign object prior to removal procedures being undertaken.7,9,10 Unfortunately, high postoperative complication rates continue to be reported for these more invasive procedures.20
Transmaxillary Trapezoidal Osteotomy
Clinicians, therefore, need to recognize the two distinct areas in the maxillary sinus into which a foreign object or implant can invade (ie, SCS and SMS), undertake radiographic and other diagnostic procedures to determine the exact location of the object, and execute the most appropriate removal procedures in order to prevent or minimize negative outcomes.8,21Upon confirmation that the object is entrapped in the SMS, the transmaxillary trapezoidal osteotomy (TTO) procedure introduced by Chen and Cha can be undertaken.6,15-17
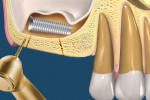
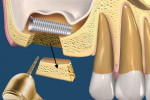
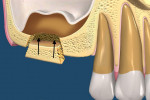
According to the TTO technique, the static location of the implant or object within the SMS is determined based on a CT scan, and a full-thickness flap is made at this site. A block design is then visualized to approximate the location and size of the object. Using a narrow-pointed diamond bur, an osteotomy is performed, with care taken to ensure it is tapered into a trapezoid-shaped cut into the sinus floor, not a straight, parallel, or angled cut (Figure 3). The trapezoidal block is then carefully removed, but not discarded, to expose the implant or object (Figure 4).
Creating and removing the trapezoidal block in this manner facilitates visualization and subsequent removal of the invading implant or object (Figure 5). After the implant or object is removed, the trapezoid block is put back into place. Due to the tapered trapezoidal cut, the block can be stabilized into place without the need for further staple tags or membranes, and primary closure can be sufficiently achieved with only the gingival flap (Figure 6).
Case 1: Bur Removal From Sinus Cavity Space
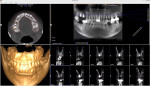
A patient presented for removal of a high-speed bur that the patient's endodontist had accidentally dropped into the sinus cavity while dissecting the tooth root tips. A radiograph was taken to confirm and identify the location of the object (Figure 7). The patient was asked to stand in an upright position and walk around for a few minutes. A second radiograph was then taken (Figure 8), and as anticipated, the bur had moved, confirming its mobility and location within the SCS. This indicated that the Chen modified Valsalva sinus clearance technique would be appropriate for removing the object from the sinus cavity. CBCT analysis was not utilized in this case, because the object was identified to be located in the SCS and could be relocated.
The patient was instructed to use his tongue to close the oro-antral perforation opening while deeply inhaling, then exert a forceful expiratory effort and release the tongue from the opening while pinching the nose. The patient repeated this maneuver five times, after which a radiograph was taken that demonstrated the bur had traveled to the oro-antral opening for easy, nonsurgical removal (Figure 9).
Case 2: Implant Fixture Removal From Sinus Cavity Space
A patient presented after undergoing implant placement 1 week prior at another practice. The implant was inserted without the use of an umbrella cover screw to prevent possible migration into the SCS (Figure 10). Upon taking a radiograph 1-week postoperatively, the implant surgeon discovered the implant fixture had dropped into the SCS (Figure 11). The surgeon then referred the patient to the authors' practice.
The patient was instructed to perform the Chen modified Valsalva sinus clearance technique, as previously described. After this, a radiograph was taken that demonstrated the implant fixture had moved to the osteotomy opening (Figure 12), thus enabling removal without the need for further surgical intervention. Again, CBCT analysis was not necessary since the object was in the SCS and could be relocated.
Case 3: Foreign Body Removal From Sinus Membranous Space
A patient presented with a chief complaint of sinusitis and a desire for implant restorations in the maxillary right posterior area. A complete history was taken, and intraoral examination was performed, including radiographs. A foreign body was observed in the maxillary sinus area.
To confirm which sinus space the foreign body was in (ie, SCS or SMS), three radiographs were taken at different intervals. The first was taken with the patient in a supine position, and two additional radiographs were taken with the patient in an upright position after walking around to determine if the foreign body was in motion. All three radiographs revealed that the aberrant foreign body remained in a static location and was entrapped within the space between the sinus membrane and bony wall of the maxilla.CBCT analysis was used in this case since the object was in the SMS and was immobile.
Therefore, as per the TTO procedure, a full-thickness flap was made at this site, and a block design was visualized to approximate the location and size of the object. Using a narrow-pointed diamond bur, an osteotomy was performed with care taken to ensure it was tapered into a trapezoid-shaped cut into the sinus floor, and not straight, parallel, or angled. The trapezoidal block was carefully removed to expose the foreign body. The foreign body was removed, and the trapezoid block returned to its place. Primary closure was achieved with only the gingival flap. The foreign object was sent for a histology report and determined to be dental cement material.
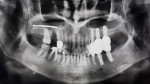
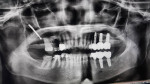
Subsequently, two dental implants (OsseoFuse Sinus, OsseoFuse, osseofuse.com) were immediately placed into the maxillary right posterior arch according to the Hydraulic Sinus Condensing (HSC™) technique (Dental Implant Institute, dentalofficeslasvegas.com). This served to improve implant osseointegration, minimize the invasiveness of the sinus lift protocol, and prevent sinus membrane perforation.15-17,22 A postoperative CBCT was taken to confirm implant placement stability (Figure 13) and ensure that the sinus area was disease-free.
Conclusion
Acknowledging and distinguishing between different spaces within the sinus cavity is essential for diagnosing foreign body invasion into the maxillary sinuses. Proper training and surgical skills are also necessary to perform procedures involving the maxillary sinus and to successfully treat such complications should they arise. The authors have proposed the identification of two different types of maxillary sinus areas (ie, SCS and SMS) that can be invaded by dental implants and/or foreign objects. Various techniques have been described over the years for the removal of foreign objects, such as amalgam, dental burs, dental cement, and dental implants, from maxillary sinus areas, but high postoperative complication rates often result from these invasive procedures. The authors propose that the ideal removal technique is predicated on understanding the nature of both the invasion and the sinus space affected so that appropriate and minimally invasive removal techniques can be implemented (eg, Chen modified Valsalva sinus clearance technique, transmaxillary trapezoidal osteotomy) and negative outcomes minimized.
About the Authors
Leon Chen, DMD, MS
Chairman and Chief Executive Officer, Dental Implant Institute, Las Vegas, Nevada
Jennifer Cha, DMD, MS
President, Dental Implant Institute, Las Vegas, Nevada
References
1. Moore KL, Dalley AF, Agur AMR. Clinically Oriented Anatomy. Philadelphia, PA: Lippincott Williams & Wilkins; 2006:841,963.
2. Lorkiewicz-Muszyńska D, Kociemba W, Rewekant A, et al. Development of the maxillary sinus from birth to age 18. Postnatal growth pattern. Int J Pediatr Otorhinolaryngol. 2015;79(9):1393-1400.
3. Velasco-Torres M, Padial-Molina M, Avila-Ortiz G, et al. Maxillary sinus dimensions decrease as age and tooth loss increase. Implant Dent. 2017;26(2):288-295.
4. Selvi F, Enoz M, Yazgin I, et al. Do asymptomatic foreign bodies in the maxillary sinus always need to be removed? B-ENT. 2008;4(4):243-247.
5. Galindo P, Sánchez-Fernández E, Avila G, et al. Migration of implants into the maxillary sinus: two clinical cases. Int J Oral Maxillofac Implants. 2005;20(2):291-295.
6. da Costa ED, Peyneau PD, Verner FS, et al. Foreign bodies in the interior of the maxillary sinus: diagnosis by cone beam computed tomography. Gen Dent. 2018;66(3):38-40.
7. Smith JL 2nd, Emko P. Management of a maxillary sinus foreign body (dental bur). Ear Nose Throat J. 2007;86(11):677-678.
8. Brescia G, Fusetti S, Apolloni F, et al. Displaced dental materials in the maxillary sinus: an original series. Analysis and definition of a surgical decision-making process. Ann Otol Rhinol Laryngol. 2019;128(3):177-183.
9. Hara Y, Shiratsuchi H, Tamagawa T, et al. A large-scale study of treatment methods for foreign bodies in the maxillary sinus. J Oral Sci. 2018;60(3):321-328.
10. González-García A, González-García J, Diniz-Freitas M, et al. Accidental displacement and migration of endosseous implants into adjacent craniofacial structures: a review and update. Med Oral Patol Oral Cir Bucal. 2012;17(5):e769-e774.
11. Marin S, Kirnbauer B, Rugani P, et al. Potential risk factors for maxillary sinus membrane perforation and treatment outcome analysis. Clin Implant Dent Relat Res. 2019;21(1):66-72.
12. Insua A, Monje-Gil F, García-Caballero L, et al. Mechanical characteristics of the maxillary sinus Schneiderian membrane ex vivo. Clin Oral Investig. 2018;22(3):1139-1145.
13. Ramanauskaite A, Ataman-Duruel ET, Duruel O, et al. Effects of clinical local factors on thickness and morphology of Schneiderian membrane: a retrospective clinical study. Clin Implant Dent Relat Res. 2019;21(4):715-722.
14. Yilmaz B, Ozcelik BT, Sarantopoulos DM, McGlumphy E. Importance of CT scans in diagnosing symptoms from misplaced implants. Implant Dent. 2012;21(2):108-111.
15. Chen L, Cha J. Dental implant migration into two different maxillary sinus cavities. J Implant Advanced Clin Dent. 2012;4(4):21-25.
16. Chen L, Cha J, Chen HC. Sinus perforation: treatment and classifications. J Implant Advanced Clin Dent. 2007;3(1):19-30.
17. Chen L, Cha J. Transmaxillary trapezoidal ostectomy technique. Lecture presented at: Dental Implant Institute of Las Vegas Annual Symposium. March 2004; Las Vegas, NV.
18. Kumar CM, Van Zundert AAJ. Intraoperative Valsalva maneuver: a narrative review. Can J Anaesth. 2018;65(5):578-585.
19. García D, García C. Valsalva: much more than a simple maneuver. Antonio Maria Valsalva (1666-1723) [article in Spanish]. Rev Med Chil. 2006;134(8):1065-1068.
20. Ramotar H, Jaberoo MC, Koo Ng NK, et al. Image-guided, endoscopic removal of migrated titanium dental implants from maxillary sinus: two cases.J Laryngol Otol. 2010;124(4):433-436.
21. Shao L, Qin X, Ma Y. Removal of maxillary sinus metallic foreign body like a hand sewing needle by magnetic iron. Int J Clin Pediatr Dent. 2014;7(1):61-64.
22. Chen L, Cha J. An 8-year retrospective study: 1,100 patients receiving 1,557 implants using the minimally invasive hydraulic sinus condensing technique. J Periodontol. 2005;76(3):482-491.