Influence of Implant–Tooth Proximity on Incidence of Caries in Teeth Adjacent to Implants in Molar Sites: A Retrospective Radiographic Analysis of 300 Consecutive Implants
Richard B. Smith, DDS; Samantha B. Rawdin, DMD; and Victor Kagan, DDS
Abstract
Implants used to replace molar teeth present issues of space distribution and crown contours that are unique to these sites. Because the diameter of the implant typically is smaller than that of the tooth being replaced, and the circular shape of the implant does not replicate the anatomy of the tooth, a large gingival embrasure area between the implant platform and adjacent tooth often results. Upon the review of radiographs of molar implants placed over an 11-year period in one private practice, the authors identified an unusually high incidence of approximal, cervical, and root caries on teeth adjacent to these implants. This retrospective radiographic study investigated the incidence of decay as related to: (1) the horizontal distance from the implant to the adjacent tooth (ie, the implant-tooth distance, or ITD) as measured at the alveolar crest, (2) the vertical distance from the apical portion of the prosthetic contact area to the implant platform, and (3) the presence of an existing restoration on the adjacent tooth. Of the three variables examined, both the horizontal distance of the implant to a natural tooth (ITD) and the presence of an existing restoration on an adjacent tooth proved to be significantly correlated with the incidence of decay. Results showed that incidence of decay ranges from 7.4% when the ITD is <2 mm to 40% when the ITD is ≥6 mm. The mean ITD in cases in which decay was found was 4.1 mm, and it was 3.5 mm in cases that showed no decay (P = .005). It is therefore suggested that the horizontal threshold of 4 mm be considered as the "critical ITD." The results also indicated that the presence of a previous restoration on an adjacent tooth increases the incidence of decay to a statistically significant degree with an odds ratio of 2.25 at a 95% confidence level. This information may prove useful in diagnosis and treatment planning for molar implant replacement.
When implants are used to replace molar teeth, issues of space distribution and crown contours may present that are unique to these sites. The diameter of the implant typically is smaller than that of the tooth being replaced, and, moreover, the circular shape of the implant does not replicate the anatomy of the tooth. These circumstances often result in the manifestation of a large gingival embrasure area between the implant platform and adjacent tooth.
After reviewing radiographs of molar implants placed over 11 years in one private practice, the authors identified an unusually high incidence of approximal, cervical, and root caries1 on teeth adjacent to these implants. This retrospective radiographic study investigated the incidence of decay as related to the following three factors: the horizontal distance from the implant to the adjacent teeth as measured at the alveolar crest, the vertical distance from the apical portion of the prosthetic contact area to the implant platform, and the presence of an existing restoration on the adjacent teeth. Of the three variables tested, both the horizontal distance of implants to natural teeth and the presence of an existing restoration on an adjacent tooth proved to be significantly correlated with the incidence of decay. The results showed statistically significant correlation with a positive predictive value, which could prove as useful information in diagnosis and treatment planning for molar implant replacement.
Materials and Methods
Digital radiographs of 300 consecutive single molar implants placed in one private practice were evaluated. The implants placed were from several different manufacturers and ranged in platform diameter from 4 mm to 6.5 mm. Both immediately and non-immediately placed implants were included in the study. All restorations were screw-retained. All radiographs were digitally calibrated using the dental implant dimensions as the known reference.
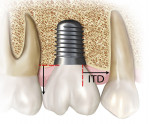
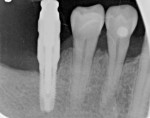
Only implants that were placed adjacent to at least one natural tooth were included. Data collected encompassed the following categories: (1) horizontal distance from the abutment/platform connection to the adjacent tooth root as measured at the alveolar crest; for platform-switched implants the distance from the outer aspect of the abutment connection was used as the measuring point instead of the outer diameter of the implant (Figure 1); (2) vertical distance from the apical portion of the prosthetic contact area to the implant platform (as measured radiographically); and (3) presence or absence of previous restorations on adjacent proximal tooth surface.
The 300 implants yielded 407 "sites" (mesial and/or distal implant-tooth embrasures) to be evaluated for the presence or absence of decay. Sites were evaluated by three examiners, while all final measurements were confirmed by one examiner.
Results
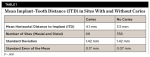
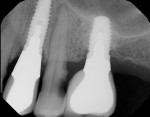
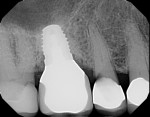
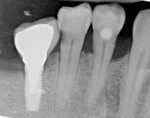
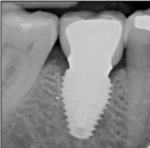
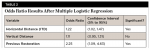
Horizontal distance from the implant platform/abutment connection to the adjacent tooth: The data indicates that as the distance between the natural tooth and the implant increases, the incidence of decay increases precipitously (Figure 2 and Figure 3). Decay occurrences range from 7.4% when the implant-tooth distance (ITD) is <2 mm to 40% when the ITD is ≥6 mm. In the 69 sites that exhibited caries, the mean ITD was 4.1 mm, and in the 338 sites without decay the mean ITD was 3.5 mm (P = .005) (Table 1). A logistic regression was performed with the single binary variable indicating whether or not the "horizontal threshold distance" was greater than 4 mm. The results show a statistically significant odds ratio of 2.00 (95% confidence interval of 1.191599, 3.350288) (Table 2.) Therefore, it is suggested that the horizontal threshold of 4 mm be considered as the "critical ITD."
Vertical distance from the interproximal contact area to the implant platform: This measurement varied greatly among samples and showed not to be a statistically significant contributing factor in decay formation (Table 2).
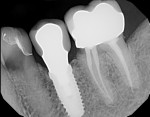
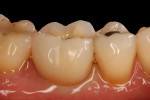
Presence or absence of restorations on the adjacent teeth: A positive correlation between existence of a previous restoration and decay was found (Figure 4, Figure 5, and Table 2).
Discussion
This study strongly suggests that there is a direct correlation between the horizontal ITD and incidence of decay. The 17% incidence (range = 7.4% to 40%) of caries formation on the 407 sites was significantly higher than normal incidence of root caries (1.87% to 2.7%) previously reported in the literature.2,3 It can be inferred from this data set that an ITD of <4 mm is recommended to significantly reduce the likelihood of developing caries in teeth adjacent to molar implants. Additionally, the data suggests a statistically significant correlation between the presence of a previous restoration on the natural tooth and caries formation. However, this data should be considered with caution as not all decay occurred directly at the restorative margin, but rather some decay occurred distant to the margin, further apically on the root surface.
The authors can only speculate as to the underlying cause for this decay pattern. The formation of approximal decay is multifactorial.4 Plaque retention and diet are among a host of risk factors that contribute to caries formation.5 However, in this retrospective radiographic study it was not possible to assess plaque index, caries index, dietary influences, or home care effectiveness. In order to evaluate these factors, a prospective clinical study would be needed. It may be that the increase in decay incidence is due to food/plaque retention beneath molar implant restorations that most often emerge from relatively narrow implant platforms. Such restorations often exhibit contours that are difficult for the patient to maintain. It should be noted, however, that many of the implant crowns studied did exhibit flat and smooth emergence profiles. The variability of the contours was not quantifiable in this retrospective radiographic study, and more research is needed to determine if crown contour is correlated with incidence of decay on neighboring teeth.
Open contact between implant restorations and natural teeth has been reported in the literature and was considered as a potential causative factor.6-8 It is believed that due to continuous growth and migration of teeth, open contacts most commonly occur mesial to the implant restoration.9 However, in the present radiographic retrospective study, contact status could not be determined with confidence. A prospective, combined radiographic and clinical study is needed to more accurately assess contact status and its influence. Perhaps relevant to this phenomenon, it has been reported that both open contacts and marginal fit discrepancies in porcelain-fused-to-metal crowns adjacent to natural teeth are causative factors in increased approximal caries formation.10
In this study the authors were unable to establish a meaningful mean timeframe for caries formation to occur because not all patients in the study were seen on regular recall intervals. Many patients were referred to the practice intermittently for surgical treatment only, and many had years-long intervals between visits. Decay did appear as early as 7 months and as late as 10 years after prosthesis insertion (Figure 6 and Figure 7). Again, a prospective clinical study would be able to more effectively assess time to decay.
In terms of distance between implant and tooth, the literature suggests a minimum distance of 1.5 mm to 2 mm as it pertains to maintenance of interproximal bone.11-13 There has been no mention of a maximum recommended distance between tooth and implant, however.
Further research is needed to more fully understand why the horizontal ITD has such a profound impact on the rate of caries formation on teeth adjacent to molar implants. Why the horizontal ITD of ≥4 mm between the adjacent tooth and the abutment/platform connection seems to be so critical to the increased chance of decay formation needs to be further examined.
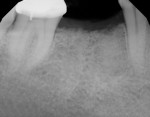
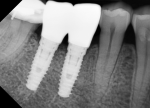
Based on the present findings, treatment protocols for molar sites may need to be altered. A reevaluation of the diameter of implants placed in molar sites may be necessary, with utilization of wider implants wherever possible (Figure 8 and Figure 9). In areas of limited alveolar ridge width, such as healed ridges, it may be advantageous to place two smaller-diameter implants instead of one wide implant to minimize the distance between the implant and adjacent tooth/teeth, ie, the ITD (Figure 10 and Figure 11).14 Alternatively, grafting the ridge, either before or at the time of placing a wider implant, could be considered. Finally, patients with molar implants, especially those with at least one ITD of ≥4 mm, may benefit from being placed on an aggressive caries prevention regimen.15
Conclusion
A high incidence of approximal, cervical, and root caries has been identified in teeth adjacent to implants placed in molar sites. The data in the present study indicates that decay incidence is directly related to the horizontal distance (ITD) between the implant/abutment connection and the adjacent root surface and may be associated with the presence of previous restorations on the adjacent tooth. The decay rate increases as the ITD increases beyond the "critical ITD" of 4 mm. Treatment protocol changes, including the use of wider-diameter implants, horizontal ridge augmentation grafts, or two narrow-diameter implants in one molar position may be necessary to counter the effects of ITD-related decay. More research is needed to definitively explain this phenomenon.
About the Author
Richard B. Smith, DDS
Associate Clinical Professor, Department of Prosthodontics, Columbia University, College of Dental Medicine, New York, New York; Private Practice, New York, New York
Samantha B. Rawdin, DMD
Private Practice, New York, New York
Victor Kagan, DDS
Private Practice, Bronx, New York
References
1. Young DA, Nový BB, Zeller GG, et al. The American Dental Association Caries Classification System for clinical practice: a report of the American Dental Association Council on Scientific Affairs. J Am Dent Assoc. 2015;146(2):79-86.
2. Beck JD, Hunt RJ, Hand JS, Field HM. Prevalence of root and coronal caries in a noninstitutionalized older population. J Am Dent Assoc. 1985;111(6):964-967.
3. Chi DL, Berg JH, Kim AS, Scott J. Correlates of root caries experience in middle-aged and older adults in the Northwest Practice-based REsearch Collaborative in Evidence-based DENTistry research network. J Am Dent Assoc. 2013;144(5):507-516.
4. Grippo JO, Coleman TA, Messina AM, Oh DS. A literature review and hypothesis for the etiologies of cervical and root caries. J Esthet Restor Dent. 2018;30(3):187-192.
5. Ritter AV, Shugars DA, Bader JD. Root caries risk indicators: a systematic review of risk models. Community Dent Oral Epidemiol. 2010;38(5):383-397.
6. Varthis S, Randi A, Tarnow DP. Prevalence of interproximal open contacts between single-implant restorations and adjacent teeth. J Oral Maxillofac Implants. 2016;31(5):1089-1092.
7. Koori H, Morimoto K, Tsukiyama Y, Koyano K. Statistical analysis of the diachronic loss of interproximal contact between fixed implant prostheses and adjacent teeth. Int J Prosthodont. 2010;23(6):535-540.
8. Greenstein G, Carpentieri J, Cavallaro J. Open contacts adjacent to dental implant restorations: etiology, incidence, consequences, and correction. J Am Dent Assoc. 2016;147(1):28-34.
9. Daftary F, Mahallati R, Bahat O, Sullivan RM. Lifelong craniofacial growth and the implications for osseointegrated implants. Int J Oral Maxillifac Implants. 2013;28(1):163-169.
10. Sadaf DE, Ahmad Z. Porcelain fused to metal (PFM) crowns and caries in adjacent teeth. J Coll Physicians Surg Pak. 2011;21(3):134-137.
11. Buser D, Martin W, Belser UC. Optimizing esthetics for implant restorations in the anterior maxilla: anatomic and surgical considerations. Int J Oral Maxillofac Implants. 2004;19 suppl:43-61.
12. Esposito M, Ekestubbe A, Gröndahl K. Radiological evaluation of marginal bone loss at tooth surfaces facing single Brånemark implants. Clin Oral Implants Res. 1993;4(3):151-157.
13. Tarnow DP, Cho SC, Wallace SS. The effect of inter-implant distance on the height of inter-implant bone crest. J Periodontol. 2000;71(4):546-549.
14. Mazor Z, Lorean A, Mijiritsky E, Levin L. Replacement of a molar with 2 narrow diameter dental implants. Implant Dent. 2012;21(1):36-38.
15. Gluzman R, Katz RV, Frey BJ, McGowan R. Prevention of root caries: a literature review of primary and secondary preventive agents. Spec Care Dentist. 2013;33(3):133-140.